The Shoulder Joint’s Secret Support Squad
April 30, 2026Emergency Room Guide for a Dislocated Shoulder
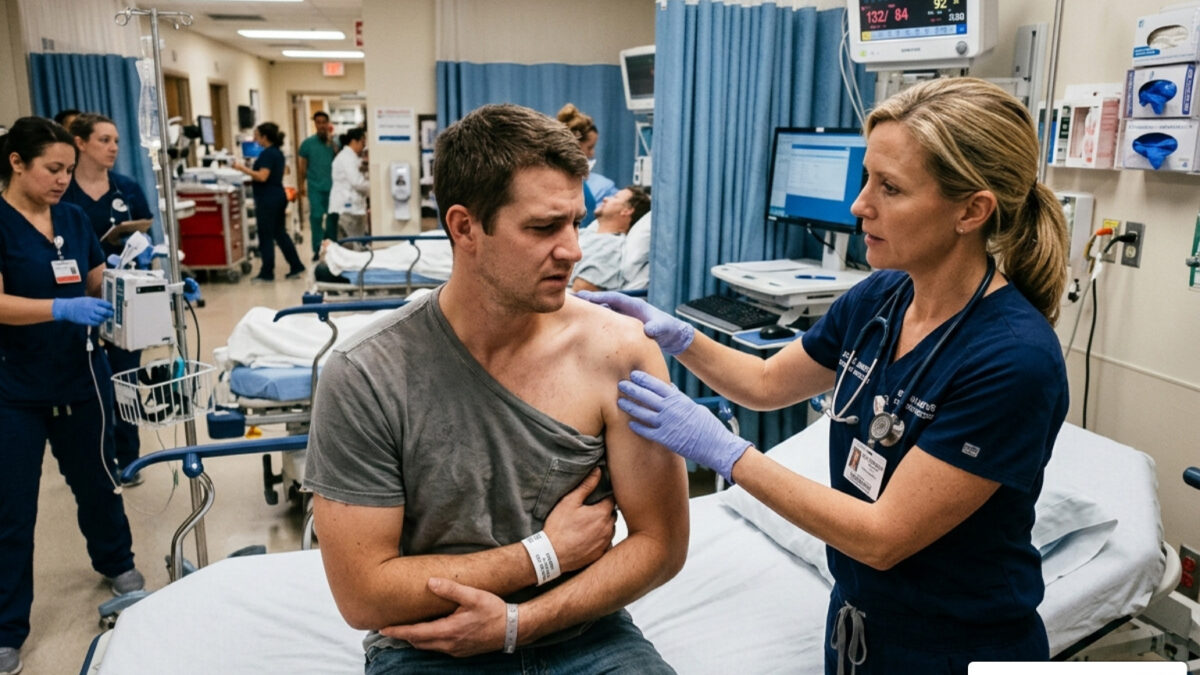
What to Expect at the Shoulder Dislocation Emergency Room
A shoulder dislocation emergency room visit is the right move the moment you suspect your shoulder has popped out of its socket — and knowing what to expect can make a painful situation far less overwhelming.
If you think your shoulder is dislocated, here’s what to do right now:
- Stop moving the arm — immobilize it in whatever position feels most comfortable
- Apply ice wrapped in a cloth to reduce swelling
- Do not try to pop it back in yourself — this can cause serious nerve, blood vessel, or bone damage
- Go to the emergency room immediately — a dislocated shoulder needs professional reduction and imaging
The shoulder is the most frequently dislocated large joint in the body, accounting for roughly 50% of all major joint dislocations. The vast majority — about 95% — are anterior dislocations, meaning the ball of the joint slips forward out of the socket. These injuries are painful, and they almost always require emergency care to safely relocate the joint and rule out fractures or nerve damage.
What makes shoulder dislocations tricky is that not all of them look the same — and some types are missed by doctors far more often than you’d expect. Getting the right diagnosis and treatment quickly matters enormously, both for your immediate pain and your long-term shoulder health.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon and sports medicine physician with over 30 years of experience treating acute joint injuries — including shoulder dislocations — at the Center for Specialty Care in Fairmont, Minnesota. My background in arthroscopic surgery and musculoskeletal care gives me a front-row view of what happens when shoulder dislocation emergency room treatment goes well — and what can go wrong when it doesn’t.

When to Visit the Shoulder Dislocation Emergency Room
The shoulder is a marvel of human anatomy—a ball-and-socket joint that allows you to reach overhead, throw a ball, or scratch that annoying itch in the middle of your back. However, that incredible range of motion comes at a price: stability. Because the socket (the glenoid) is quite shallow—think of a golf ball sitting on a tee—it doesn’t take much for the humeral head (the ball) to slip out of place.
When you experience a true dislocation, the symptoms are rarely subtle. You will likely feel:
- Intense, sickening pain: This is often the primary reason for a shoulder dislocation emergency room visit.
- Visible deformity: The shoulder often loses its rounded shape and looks “squared-off.”
- Inability to move the arm: You will find it nearly impossible to move your arm from its fixed position.
- Numbness or tingling: This may radiate down the arm or into the hand, signaling potential nerve involvement.
In the moments following the injury, first aid is critical. We recommend immobilizing the arm with a makeshift sling (using a shirt or towel) and applying ice to control swelling and bleeding. As we discuss in our guide on Will A Torn Rotator Cuff Heal On Its Own Key Recovery Facts, soft tissue injuries often accompany joint trauma, and immediate stabilization is the best way to prevent further damage.
According to the Shoulder Dislocation in Emergency Medicine Overview, prompt medical intervention is necessary to evaluate the joint and ensure no major blood vessels or nerves are trapped.
Initial Assessment and Diagnostic Imaging
Once you arrive at the shoulder dislocation emergency room, the medical team will move quickly. The first priority isn’t the “pop”—it’s the assessment. We need to know if your nerves and blood vessels are intact before any attempt is made to move the bone.
The physician will perform a neurovascular exam, specifically checking:
- The Axillary Nerve: This is the most commonly injured nerve in shoulder dislocations. The doctor will check for sensation on the “regimental badge” area (the outer part of your upper arm) and may ask you to slightly fire your deltoid muscle.
- Distal Pulses: Checking the radial pulse at your wrist ensures that the displaced bone isn’t compressing the axillary artery.
- Motor Function: Can you make a fist? Can you give a “thumbs up”? These simple movements tell us a lot about the health of your brachial plexus.
Research in the Assessment and management of shoulder dislocation emphasizes that a thorough exam is the foundation of safe care.
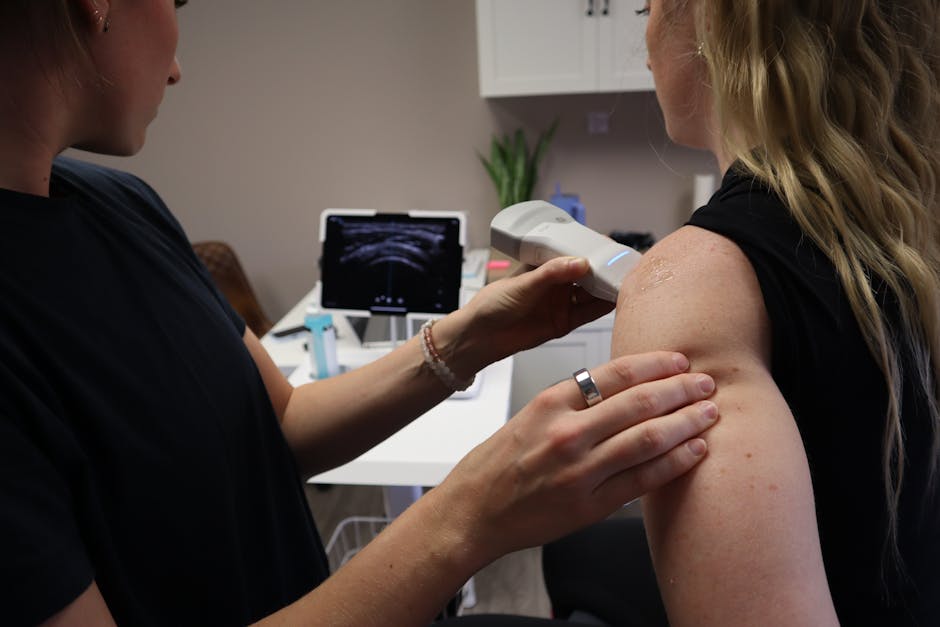
Diagnostic Imaging at the Shoulder Dislocation Emergency Room
“Don’t I just need it popped back in?” is a common question. The answer is yes, but we need pictures first. Statistics show that 13% of fractures are missed simply because X-rays weren’t ordered initially.
The standard “shoulder series” includes:
- AP (Anteroposterior) View: The standard front-to-back shot.
- Scapular Y-View: This helps determine if the humeral head is sitting in front of (anterior) or behind (posterior) the socket.
- Axillary View: This is the “gold standard” for seeing exactly where the ball is in relation to the socket. It is also where we look for the “light bulb sign” (a sign of posterior dislocation) or the “rim sign.”
While rare, extreme trauma can lead to Fasciotomy A Lifesaving Procedure For Treating Compartment Syndrome if vascular damage occurs, which is why imaging and vascular checks are never skipped at the Center for Specialty Care.
Differentiating Anterior, Posterior, and Inferior Dislocations
Not all dislocations are created equal. Identifying the direction is vital for the reduction technique used in the shoulder dislocation emergency room.
- Anterior Dislocations (95%): The arm is usually held in a position of abduction and external rotation (like you’re about to throw a ball).
- Posterior Dislocations (2-4%): These are the “sneaky” ones. They are missed 50-80% of the time by the first physician who sees them. They often occur during seizures or electric shocks when the muscles contract so violently they pull the ball backward. The arm is usually held tight against the body and internally rotated.
- Inferior Dislocations (Luxatio Erecta, <1%): This is rare and visually striking—the patient’s arm is stuck straight up over their head, and they cannot lower it. This type has the highest risk of vascular and nerve injury.
Detailed clinical signs for each can be found in the Shoulder Dislocation in Emergency Medicine Clinical Presentation guide.
Reduction Techniques and Pain Management
“Reduction” is the medical term for putting the joint back in place. While Hollywood makes it look like a violent “yank,” modern medicine favors “slow and steady.”
Pain Management Options in the Shoulder Dislocation Emergency Room
Muscle spasms are the enemy of a successful reduction. When you’re in pain, your muscles tighten up to protect the joint, which actually locks the humeral head in its dislocated position. To overcome this, we use several methods:
- Procedural Sedation: Often using medications like propofol or etomidate, this puts you in a “twilight” state where your muscles completely relax.
- Intra-articular Lidocaine: We inject numbing medicine directly into the joint space. This is often just as effective as sedation but allows you to leave the ER much faster.
- ERWOSA (External Rotation Without Sedation/Analgesia): This method has a success rate of about 78.7%. It relies on extremely slow, gentle movements to “trick” the muscles into relaxing without drugs.
For more on managing systemic pain and muscle issues, see our resources on Common Spinal Conditions Causes Symptoms And Treatment Options.
Effective Reduction Maneuvers
There are dozens of ways to put a shoulder back, but some are more common in the shoulder dislocation emergency room than others:
| Technique | Success Rate | Description |
|---|---|---|
| Scapular Manipulation | 80-98% | The doctor rotates the shoulder blade to meet the humeral head. |
| External Rotation | 80-90% | Gently rotating the arm outward while the patient is lying down. |
| Cunningham | High | A massage-based technique focusing on the biceps and deltoids. |
| Stimson | Variable | The patient lies face down with a weight (10-15 lbs) hanging from the arm. |
| Milch | 86-100% | Involves reaching the arm over the head with gentle pressure. |
The Shoulder Dislocation in Emergency Medicine Treatment & Management protocols suggest that the best technique is the one the physician is most comfortable with, provided it is performed gently.
Identifying Associated Injuries and Complications
A dislocation is rarely just a “bone out of place” issue. Because the shoulder is held together by a complex web of ligaments and tendons, damage to these structures is common.
- Hill-Sachs Lesion: A dent in the back of the humeral head caused by it hitting the edge of the socket. This occurs in 54-76% of dislocations.
- Bankart Lesion: A tear in the labrum (the rubbery bumper around the socket). This is a major cause of future instability.
- Greater Tuberosity Fracture: In about 30% of cases, a piece of bone actually breaks off where the rotator cuff attaches.
- Axillary Nerve Injury: Seen in about 3% of cases, usually resulting in temporary weakness or numbness.
If you have underlying inflammatory conditions, recovery can be more complex. We invite you to explore Rheumatology Resources And Care At Center For Specialty Care Mankato Mn if you suspect your joint health is impacted by more than just trauma.
Post-Reduction Recovery and Recurrence Prevention
Once the shoulder is back in place, the relief is usually instant and profound. However, the work is just beginning.
Immobilization: You will likely be placed in a sling or a “sling and swathe.” For patients under 40, we typically recommend about 10 days of immobilization. For those over 40, we shorten this to 5-7 days to prevent “frozen shoulder” (adhesive capsulitis).
The Risk of Recurrence: This is the most significant long-term concern.
- Patients <30 years old: Have a 50-64% risk of another dislocation.
- Older adolescents: Can face up to a 90% risk of recurrence.
This is why physical therapy is non-negotiable. Strengthening the rotator cuff and scapular stabilizers is the only way to “tighten” the joint without surgery. If you are also dealing with other joint issues, our Doctor For Elbow Pain Specialized Orthopedic Treatment guide highlights how we approach comprehensive upper extremity care.
Frequently Asked Questions about Shoulder Dislocations
Why are posterior shoulder dislocations frequently missed?
They are missed because they don’t look like the classic “deformed” shoulder. On a standard front-facing X-ray, the ball can look like it’s in the socket when it’s actually behind it. This is why we insist on multiple X-ray angles. A history of seizures or electric shock should always make a doctor suspect a posterior dislocation.
When is surgery required for a dislocated shoulder?
Surgery is usually considered if:
- The dislocation is “irreducible” (it won’t go back in).
- There is a significant fracture (like a large Bankart or Hill-Sachs lesion).
- The patient is a young athlete with a very high risk of future dislocations.
- There is a complete rotator cuff tear (common in patients over 40).
Can I relocate my own shoulder like on TV?
Please, don’t. While it looks heroic in action movies, in the real world, you are more likely to tear a labrum, break the glenoid rim, or pinch a major nerve. Professional reduction in a shoulder dislocation emergency room ensures the bone goes back in the right way without creating a new injury.
Conclusion
A dislocated shoulder is a major event, but with the right care, you can get back to the activities you love. At the Center for Specialty Care, we pride ourselves on providing Fairmont and the surrounding Minnesota and Iowa communities with personalized, expert orthopedic care. Whether it’s your first dislocation or a recurring issue, our goal is 100% patient satisfaction through both surgical and non-surgical pathways.
If your injury was the result of an accident, be sure to check out our Shoulder Pain After Car Accident Recovery Tips for specialized advice on navigating that recovery process.
Don’t let a shoulder injury keep you on the sidelines in 2026. Contact us today at our Fairmont, MN office or our locations in Estherville and Buffalo Center, IA, to schedule a follow-up and ensure your shoulder is stable, strong, and ready for whatever comes next.