Heal & Compete: Discovering Sports Medicine in Fairmont
November 13, 2025
Decoding Rotator Cuff Tears: Everything You Need to Know
November 17, 2025Chronic Pain Treatment: 2025’s Ultimate Path to Relief
Understanding Your Options for Lasting Relief
Chronic pain treatment requires a comprehensive plan that combines lifestyle changes, therapies, and carefully selected procedures or medications to reduce pain and restore function. While completely eliminating chronic pain is rare, evidence shows that a multimodal approach can reduce pain by approximately 30% and significantly improve quality of life.
Quick Overview of Chronic Pain Treatment Options:
- Non-Drug Approaches: Physical therapy, exercise programs, cognitive behavioral therapy, massage therapy
- Medications: NSAIDs, acetaminophen, antidepressants, anti-seizure medications (for nerve pain)
- Interventional Procedures: Epidural steroid injections, nerve blocks, radiofrequency ablation
- Lifestyle Support: Anti-inflammatory nutrition, medical weight loss, stress management
- Team-Based Care: Orthopedic specialists, pain management physicians, physical therapists working together
According to the CDC, over 51 million U.S. adults experienced chronic pain in 2021—that’s one in five people living with pain lasting three months or longer. Unlike acute pain from a new injury, chronic pain involves changes in the nervous system that amplify pain signals, a process called central sensitization. This means your pain is more complex than the original injury.
The path forward involves combining strategies. Some treatments address physical pain sources, while others retrain how your nervous system processes pain. I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon. At the Center for Specialty Care, my team and I have helped thousands of patients in southern Minnesota and northern Iowa move from persistent pain to improved function with personalized treatment plans.
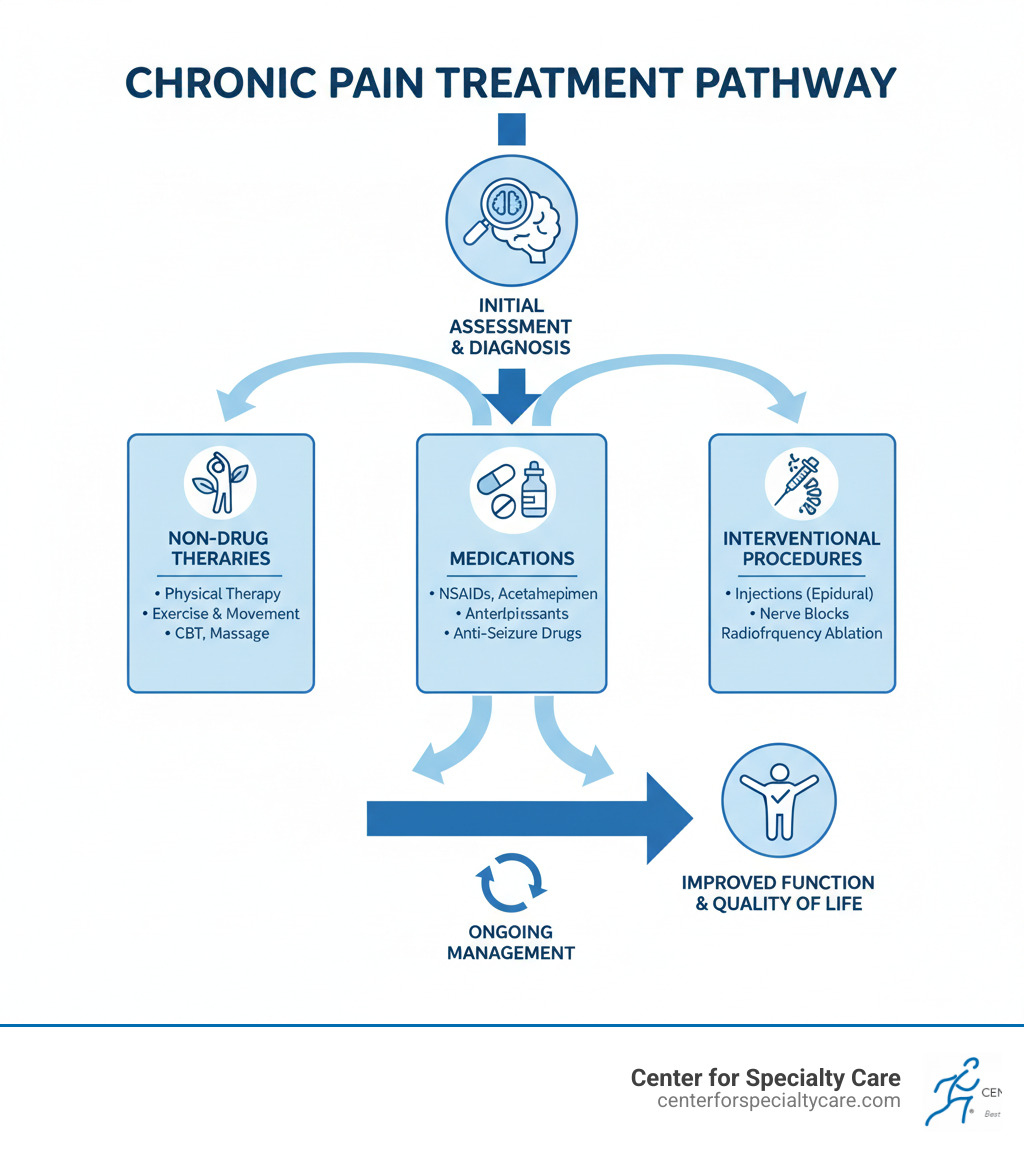
This guide will walk you through each category of treatment—from foundational lifestyle changes to advanced interventional procedures—so you can work with your healthcare team to create a roadmap that works for you.
What is Chronic Pain? Causes, Symptoms, and Diagnosis
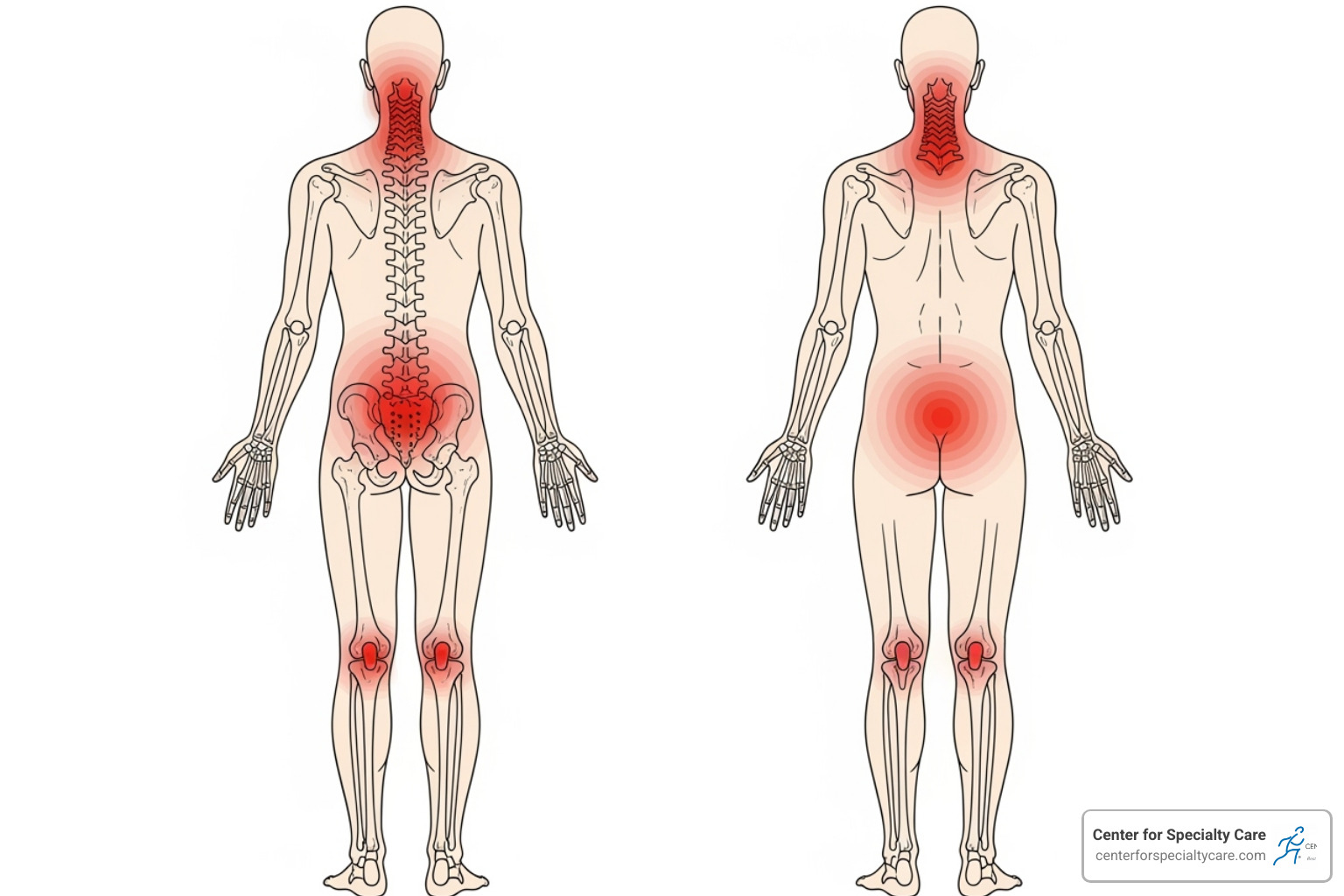
When pain lasts for more than three months, it becomes a chronic condition that affects your entire life. Chronic pain treatment starts with understanding that this is different from acute pain. Your nervous system changes through a process called central sensitization, amplifying pain signals even after an injury has healed. This can lead to different types of pain, including nociceptive (from tissue damage), neuropathic (from nerve damage), and inflammatory pain.
This persistent discomfort can disrupt sleep, make work challenging, and limit activities you enjoy, significantly reducing your quality of life.
Common Causes and Risk Factors
Chronic pain often develops gradually from various sources:
- Previous injuries: Lingering pain from old injuries is a common cause. Our Back and spine conditions specialists often trace chronic pain back to an earlier incident.
- Arthritis: Osteoarthritis (wear and tear) and rheumatoid arthritis (autoimmune) are major culprits. Our Rheumatology team specializes in managing these conditions.
- Nerve damage: Can result from injuries, surgery, or conditions like diabetes.
- Other conditions: Fibromyalgia and autoimmune diseases can cause widespread pain.
- Lifestyle factors: Aging, obesity, and chronic stress all increase the risk of developing chronic pain.
Symptoms and Potential Complications
Chronic pain can feel like a constant ache, burning, shooting pains, or stiffness. Beyond the pain itself, common complications include:
- Fatigue and insomnia: Pain disrupts sleep, leading to constant exhaustion.
- Mood changes: Irritability, anxiety, and depression are very common. Research shows a high comorbidity between chronic pain and mental health conditions.
- Reduced mobility: Pain leads to inactivity, which weakens muscles and stiffens joints, creating a vicious cycle.
- Substance use disorder: The struggle with severe pain can sometimes lead to dependence on pain medication, highlighting the need for safe, effective management.
How a Specialist Diagnoses Chronic Pain
Diagnosing chronic pain is a detailed process that begins with listening to your story. A specialist will use several methods to understand your pain:
- Patient history: A thorough discussion about your pain’s location, feel, and triggers, as well as your medical history and lifestyle.
- Physical examination: To assess range of motion, identify tender spots, and check for muscle weakness.
- Diagnostic imaging: X-rays, MRIs, and CT scans help visualize bones, soft tissues, and nerves. We offer Diagnostic imaging (MRI, X-Ray) services in-house for your convenience.
- Nerve and blood tests: Nerve conduction studies can identify nerve damage, while blood tests can reveal inflammation or other underlying medical issues.
The goal is to identify the root cause of your pain to develop a targeted chronic pain treatment plan that offers the best chance for relief.
Foundational Treatments: Lifestyle, Nutrition, and Mind-Body Therapies
Before turning to procedures or medications, foundational lifestyle strategies can provide significant pain relief. These evidence-based approaches put you in control of your healing journey.
The Role of Exercise and Physical Therapy
It may seem counterintuitive, but appropriate movement is one of the most effective tools against chronic pain. Research confirms that physical activity can improve pain and function with few side effects.
- Improves strength and flexibility: Stronger muscles support painful joints, reducing strain.
- Reduces stiffness: Gentle movement lubricates joints and keeps tissues supple.
- Changes pain perception: Regular exercise can make you less sensitive to pain signals over time, a phenomenon known as exercise-induced hypoalgesia.
There is no one-size-fits-all exercise plan. Our Physical Therapy services focus on creating individualized programs, starting with gentle activities like walking or swimming and progressing as you get stronger.
Nutrition and Supplements for Pain Management
Your diet directly influences inflammation, a key driver of chronic pain. An anti-inflammatory diet, like the Mediterranean diet, emphasizes whole foods such as fruits, vegetables, lean proteins, and healthy fats while minimizing processed foods and sugar.
Weight management is also crucial, as excess weight stresses joints in the hips, knees, and spine. Losing even a small amount of weight can make a big difference. Our Medical Weight Loss programs provide support for this important aspect of pain management.
Certain supplements may also help, but always consult your doctor first:
- Vitamin D: Deficiency has been linked to chronic pain, and supplementation may help.
- Omega-3 fatty acids: Found in fatty fish, these are powerful anti-inflammatory agents.
- Turmeric (curcumin) and Boswellia: Both have been studied for their pain-relieving and anti-inflammatory properties.
Mind-Body Approaches for Retraining Your Brain
Because chronic pain changes your nervous system, addressing the mental and emotional components is essential. Mind-body therapies can retrain your brain’s response to pain and reduce stress.
- Cognitive Behavioral Therapy (CBT): Teaches practical strategies to reshape negative thought patterns related to pain and improve your emotional response. It is proven to provide moderate pain relief.
- Mindfulness and meditation: Help you observe pain without judgment, reducing its emotional power.
- Progressive muscle relaxation: Involves tensing and releasing muscle groups to relieve physical tension. It is recommended as a first-line treatment for chronic low-back pain.
- Biofeedback: Uses sensors to help you learn to consciously control bodily responses like muscle tension and heart rate.
These empowering techniques give you active tools to manage your pain and participate in your own healing.
Hands-On and Interventional Chronic Pain Treatment Options
When foundational treatments aren’t enough, hands-on therapies and advanced procedures can target specific pain sources. These interventions are valuable additions to a comprehensive chronic pain treatment plan.
Manual and Complementary Therapies
Manual therapies use skilled touch to reduce pain and restore function.
Massage therapy does more than just relax you. It increases blood flow to tense tissues, helps flush out inflammatory substances, and reduces stress hormones that amplify pain. Regular massage can significantly improve symptoms for conditions like back pain, neck pain, osteoarthritis, and fibromyalgia.
Spinal manipulation, a technique used in physical therapy, applies controlled force to spinal joints to restore proper movement. This can break the cycle of stiffness and discomfort, especially for low back pain. Our Physical Therapy services incorporate these techniques into comprehensive treatment plans to help you regain mobility.
Advanced Chronic Pain Treatment Procedures
For persistent pain, minimally invasive procedures can offer targeted, long-lasting relief.
-
Epidural steroid injections: Deliver powerful anti-inflammatory medication directly to irritated spinal nerves. This provides significant relief for conditions like sciatica, herniated discs, and spinal stenosis. You can learn more about Epidural Steroid Injections and if they are right for you.
-
Nerve blocks: Involve injecting an anesthetic near specific nerves to interrupt pain signals. They can be used to diagnose a pain source or provide therapeutic relief for weeks or months.
-
Radiofrequency ablation: Uses heat to disable small nerve fibers that transmit pain signals. It is highly effective for chronic back and neck pain from facet joints, with relief often lasting six months to a year.
-
IntraCept Procedure: A minimally invasive option for chronic low back pain that targets the basivertebral nerve inside the bone, offering a solution when other treatments have failed.
-
TENS units: Small, portable devices that use mild electrical currents to block pain signals and stimulate the release of natural pain-relieving endorphins.
These advanced procedures are considered carefully as part of your overall plan, offering new possibilities when conservative options haven’t provided sufficient relief.
The Role of Medication in a Comprehensive Plan
Medications can be a key part of a chronic pain treatment plan, but they work best alongside physical therapy and lifestyle changes. The goal is to find the right medication for your specific pain while prioritizing your safety.
Non-Opioid Medications
We always start with the safest effective options first.
-
Nonsteroidal anti-inflammatory drugs (NSAIDs): Over-the-counter (ibuprofen, naproxen) and prescription versions reduce inflammation and are effective for arthritis and back pain. However, long-term use carries risks like stomach problems and kidney issues.
-
Acetaminophen: Eases mild to moderate pain and is gentler on the stomach than NSAIDs. It does not reduce inflammation and must be used carefully to avoid liver damage.
-
COX-2 inhibitors: These prescription NSAIDs are designed to be easier on the stomach but still carry risks, including headaches and potential cardiovascular effects.
We carefully consider your full medical history before recommending any medication.
Adjuvant Medications for Nerve Pain
For neuropathic pain (from nerve damage), traditional pain relievers often aren’t enough. Adjuvant medications, originally developed for other conditions, can be very effective.
-
Antidepressants: Certain types, like tricyclics and SNRIs, adjust neurotransmitters involved in pain processing, which can quiet overactive nerve signals. They also help with the depression and anxiety that often accompany chronic pain.
-
Anti-seizure medications: Drugs like Gabapentin and Pregabalin calm overexcited nerve cells, making them a cornerstone for treating fibromyalgia, diabetic neuropathy, and post-shingles pain.
Side effects like drowsiness and dizziness are possible, so we start with low doses and adjust carefully to find the right balance of relief and tolerability.
A Cautious Approach to Opioids
Opioids are powerful medications that are highly effective for severe acute pain (like after surgery) and cancer-related pain. However, for ongoing, non-cancer chronic pain, their long-term benefits are limited, and the risks are serious.
Your body quickly adapts to opioids, leading to tolerance (needing more for the same effect) and physical dependence. The risk of long-term use increases significantly after just a few days. Opioids are also a leading cause of overdose deaths in the U.S.
For these reasons, our philosophy is to prioritize your safety and long-term well-being. We explore every effective non-opioid option first. When opioids are necessary, we prescribe them at the lowest effective dose for the shortest possible time, as part of a comprehensive chronic pain treatment plan. Your medication strategy is a personal decision we make with you, based on your health, goals, and response to therapy.
Creating Your Personalized Roadmap with a Healthcare Team

You don’t have to face chronic pain alone. The most successful chronic pain treatment plans are built on a partnership between you and a dedicated healthcare team. At Center for Specialty Care, this collaborative approach is central to how we help our patients.
When to Seek Professional Help
It’s time to take control and seek professional care if:
- Your pain has lasted more than three months.
- Pain is interfering with your daily life, work, or sleep.
- Over-the-counter medications are no longer effective.
- Your pain is getting worse despite your efforts.
Waiting too long can make pain harder to treat. A pain management specialist can offer solutions you haven’t tried.
Developing a Personalized Chronic Pain Treatment Plan
Your pain is unique, so your treatment plan should be too. Our multidisciplinary team—including pain management specialists, orthopedic doctors, and physical therapists—works together to address your condition from every angle.
One of the most important steps is setting realistic goals. We focus on meaningful improvements that improve your function and quality of life. This might mean reducing your pain by 30%—a common and achievable goal that can translate into sleeping through the night, returning to hobbies, or playing with your grandkids.
Outlook and Goals of Treatment
For most people, chronic pain treatment is about management, not a complete cure. Like other chronic conditions such as diabetes, effective management can give you your life back. With the right strategies, you can thrive.
Our goal is to help you return to the activities you love. Your plan will include long-term management strategies, such as exercises and tools to handle flare-ups. There is genuine hope. Our team in Fairmont, Estherville, Buffalo Center, and St. James has helped thousands of patients live full, active lives. With personalized care and your active participation, an improved quality of life is within reach.
Frequently Asked Questions about Chronic Pain Treatment
Living with persistent pain raises many questions. Here are answers to some of the most common concerns we hear at the Center for Specialty Care.
Does chronic pain ever go away completely?
For most, chronic pain is managed rather than cured. However, “management” means significantly reducing pain to a level where it no longer controls your life. If a specific underlying cause can be treated—like repairing a joint—the pain may resolve completely. More often, the goal is a 30% to 50% reduction in pain, which can be transformative for your ability to work, sleep, and enjoy life.
Are non-drug treatments really effective?
Yes, absolutely. Non-drug treatments like exercise, physical therapy, and cognitive behavioral therapy (CBT) are often the most powerful tools in your chronic pain treatment plan. Strong evidence supports their effectiveness in improving pain and function. They do more than mask symptoms—they strengthen your body and retrain how your nervous system processes pain. These approaches empower you with skills to manage your health, often reducing the need for medication.
What is a pain management specialist?
A pain management specialist is a medical doctor with advanced training in diagnosing and treating complex pain conditions. They use a multidisciplinary approach, coordinating with physical therapists, orthopedic surgeons, and other specialists to create a comprehensive plan. They are skilled in a wide range of treatments, from medication management to advanced interventional procedures like epidural steroid injections and nerve blocks. Their focus is not just on treating symptoms, but on improving your overall function and quality of life.
Take the First Step on Your Road to Relief
You’ve taken an important step by learning about your options. Living with chronic pain is exhausting, but you don’t have to keep living this way. A better quality of life is possible.
Effective chronic pain treatment combines multiple approaches: a foundation of lifestyle changes and physical therapy, supported by appropriate medications and advanced procedures when needed. There is no single solution, which is why a personalized plan is so critical.
Knowledge is powerful, but action creates change.
At the Center for Specialty Care, our team is committed to creating a personalized roadmap to help you manage pain and regain your life. We bring together orthopedic specialists, pain management physicians, and physical therapists—all focused on your unique goals. We’re not interested in one-size-fits-all solutions; we’re dedicated to walking alongside you on your journey to relief.
We serve communities throughout southern Minnesota and northern Iowa, with locations in Fairmont, Estherville, Buffalo Center, and St. James. We pride ourselves on quick appointment availability because we know you can’t wait for help. Our commitment to 100% patient satisfaction means we will explore every option to help you feel better.
You’ve lived with pain long enough. It’s time to start your journey toward relief.
Contact us to learn more about our comprehensive Pain Management services.