Podiatrist Near Me: A Quick Guide to Local Foot Care
November 19, 2025
Relieve Rotator Cuff Pain at Night: Tips for a Better Sleep
November 21, 2025Interventional Pain Medicine: Ultimate Relief 2025
Why Interventional Pain Medicine Matters for Your Chronic Pain
Interventional pain medicine is a specialized field using minimally invasive procedures—like nerve blocks and epidural injections—to diagnose and treat chronic pain. Unlike approaches that rely on medication or major surgery, these techniques target the specific source of your pain with precision. This often reduces the need for opioids and helps you return to normal activities.
Key facts about interventional pain medicine:
- Prevalence: More than 20% of American adults live with chronic pain
- Approach: Uses image-guided, minimally invasive procedures instead of surgery
- Goal: Identify and treat the exact source of pain while preserving normal anatomy
- Techniques: Includes injections, nerve blocks, radiofrequency ablation, and spinal cord stimulation
- Outcome: Helps reduce pain, improve pain, improve function, and improve quality of life
Living with chronic pain limits your ability to work, enjoy hobbies, and spend time with loved ones. The good news is that interventional pain medicine offers advanced treatment options that can provide real relief without major surgery. This guide will walk you through what you need to know about these treatments.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon at the Center for Specialty Care in Fairmont, Minnesota. Our team uses interventional pain medicine alongside orthopedic, physical therapy, and rehabilitation services to help patients in southern Minnesota and northern Iowa find lasting relief. We’ll explore how these innovative approaches could help you take control of your pain.
What is Interventional Pain Medicine?
When you’re living with chronic pain, you need answers, not just temporary relief. Interventional pain medicine is a specialty focused on diagnosing and treating pain-related disorders, especially persistent pain that doesn’t respond to conventional treatments.
Instead of simply masking symptoms with medication, we work to identify the exact source of your pain and intervene directly at that spot. We view chronic pain not just as a symptom, but as a disease in itself. This perspective guides our use of minimally invasive techniques—like inserting needles or small catheters—to deliver medication, calm overactive nerves, or repair damaged tissues.
The goal is to alleviate pain, improve function, and improve your quality of life. A significant benefit is reducing reliance on oral medications like opioids, which carry their own risks. Our multidisciplinary approach means we collaborate with physical therapists, orthopedic surgeons, and other specialists to provide comprehensive, personalized care. For more information, please visit our pain management page.
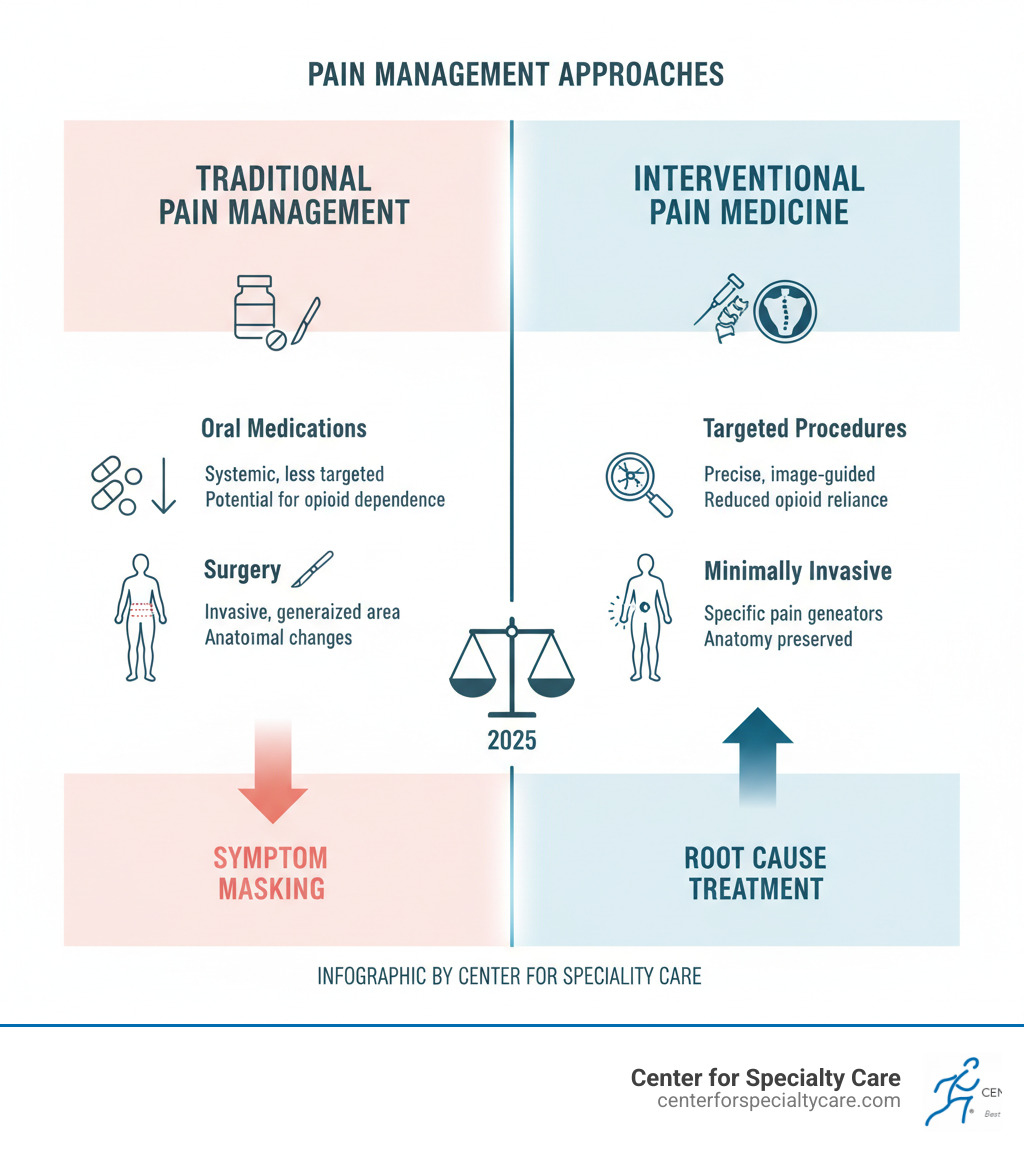
How It Differs from Other Approaches
To appreciate what interventional pain medicine offers, it helps to compare it against traditional options.
| Feature | Oral Medication | Major Surgery | Interventional Pain Medicine |
|---|---|---|---|
| Approach | Systemic (body-wide) | Invasive (open surgical procedures) | Minimally Invasive (targeted procedures) |
| Target | Generalized pain relief | Structural correction (e.g., fusion) | Specific pain generator (nerve, joint, disc) |
| Risk Profile | Systemic side effects, addiction risk | Anesthesia risks, infection, long recovery | Lower risk, often outpatient, faster recovery |
| Diagnostic Capability | Limited | Imaging for structural issues | High (diagnoses and treats simultaneously) |
| Preservation | No impact on anatomy | Often alters anatomy (e.g., removal) | Preserves anatomy, repairs where possible |
| Goal | Symptom management | Cure structural problem | Targeted pain relief, functional improvement |
The key difference is precision. Oral medications affect your entire body, leading to side effects like drowsiness, nausea, and dependency. Major surgery can be necessary but involves significant risks, long recovery times, and permanently alters your anatomy.
Interventional pain medicine offers a targeted middle path. We pinpoint the exact source of your pain and treat it directly, leading to fewer side effects and faster recovery. Many procedures also serve a diagnostic purpose, confirming the pain source before committing to more permanent treatments. This approach prioritizes preserving your natural anatomy, helping you maintain flexibility and future options.
Determining Your Candidacy
Wondering if interventional pain medicine is right for you? We determine this through a thorough, personalized evaluation.
The process begins with a comprehensive review of your medical history, previous injuries, and current medications. A detailed physical examination follows, where we assess your pain, range of motion, and neurological function. Imaging studies like X-rays, MRI, or CT scans help us visualize the underlying problem, such as a herniated disc or spinal stenosis.
Most patients we see have already tried conservative treatments like oral medications or physical therapy without success. If you’re frustrated with a lack of relief, you are the kind of patient we can often help. We’ll also discuss your personal goals—whether it’s playing with grandchildren, returning to work, or simply sleeping through the night.
At the Center for Specialty Care, our specialists in Fairmont, Estherville, Buffalo Center, and St. James provide personalized care with quick appointment availability. We work to assess your needs promptly and develop a treatment plan that makes sense for you. If you’re looking for specialized care, you can find a pain management doctor to explore your options.
Conditions Commonly Treated
More than 20% of U.S. adults struggle with chronic pain. Interventional pain medicine offers effective solutions for a wide range of conditions that may be limiting your daily activities.
Chronic back and neck pain are the most common complaints we address. Caused by issues like degenerative disc disease or facet joint arthritis, this pain can dramatically impact your quality of life. We focus on identifying the specific pain generator to treat it directly.
Sciatica and radiating pain travel down a leg or arm, often with numbness or tingling. This usually occurs when a nerve root is compressed by a herniated disc or bone spur. For more information, explore our guide on common spinal conditions and find tips for managing radiating pain.
Degenerative disc disease occurs as the cushioning discs between your vertebrae lose elasticity with age. Spinal stenosis, a narrowing of the spinal canal, can also put pressure on nerves, causing pain that worsens with activity.
Arthritis and joint pain affect millions, whether it’s osteoarthritis in the knees, hips, or shoulders, or inflammatory arthritis. Our orthopedics services work with interventional pain medicine to provide comprehensive joint care.
Neuropathic pain results from nerve damage, causing burning, tingling, or shooting sensations. Complex Regional Pain Syndrome (CRPS) is a severe form that usually affects a limb after an injury, causing disproportionate pain and sensitivity.
Even chronic headaches and migraines can benefit from interventional approaches when specific nerves are involved.
At Center for Specialty Care, our goal is to help you win the fight against chronic pain through personalized care that addresses the root cause, not just the symptoms.
Types of Interventional Pain Management Procedures
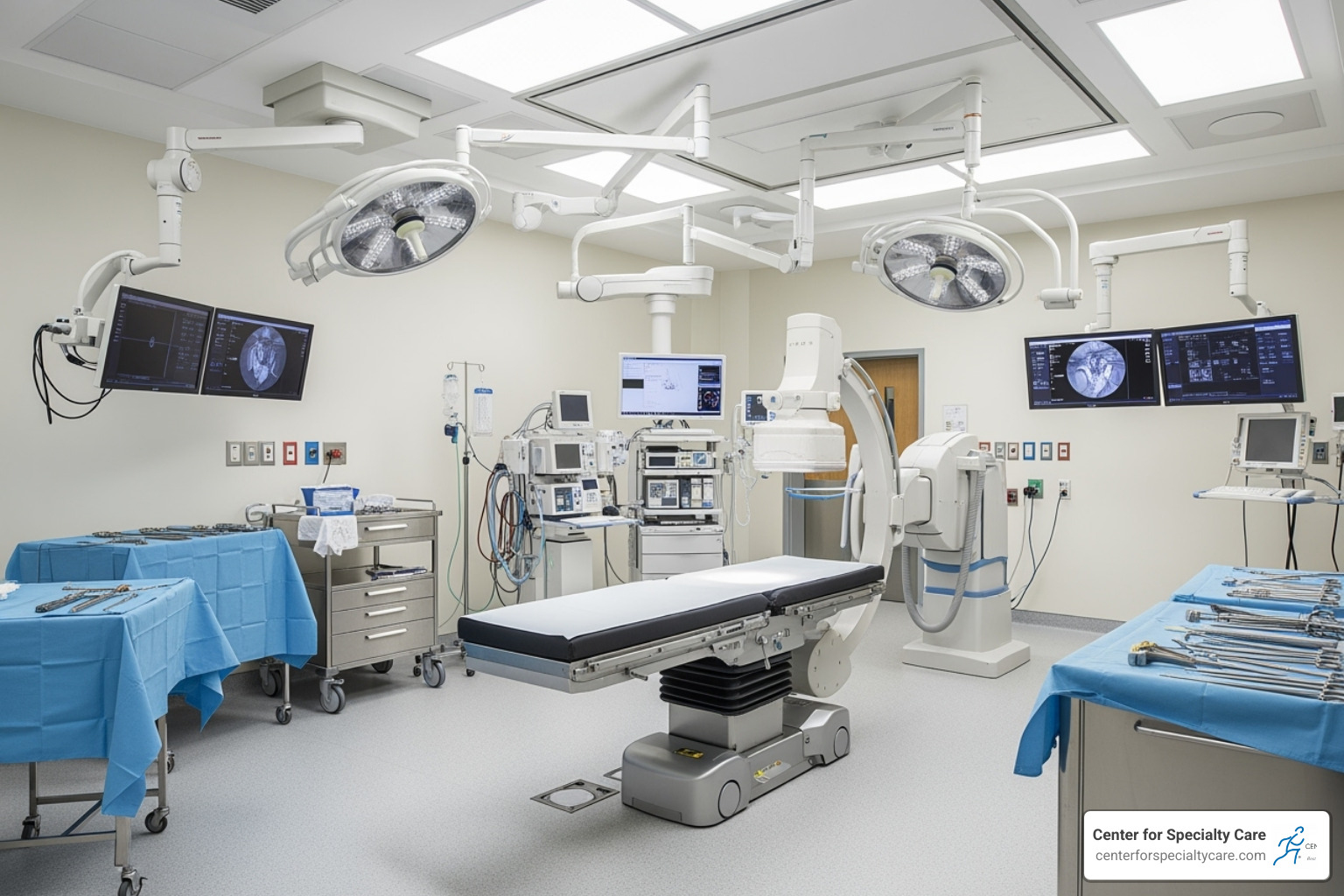
Our procedures use sophisticated imaging like fluoroscopy (real-time X-ray) and ultrasound. This image-guidance allows us to see exactly where we’re working, ensuring precise needle placement for maximum safety and effectiveness. Most procedures are performed in our outpatient facility, and you can typically go home the same day without a hospital stay.
Injections for Targeted Relief
Injection-based treatments deliver medication directly to the source of your pain, avoiding the systemic effects of oral pills.
- Epidural steroid injections place anti-inflammatory medication into the epidural space around the spinal cord to calm irritated nerves from conditions like a herniated disc or spinal stenosis. Learn more in our guide to understanding epidural steroid injections.
- Facet joint injections deliver medication into the small, arthritic joints of the spine to relieve back or neck pain.
- Trigger point injections release tight, knotted muscle bands to interrupt the pain cycle.
- Joint injections for the knee, hip, or shoulder use corticosteroids or hyaluronic acid to reduce arthritis pain and improve function. These injections can banish joint pain for months.
- Nerve blocks are both diagnostic and therapeutic. They help confirm the source of your pain while providing relief by “muting” pain signals from a specific nerve. Learn how nerve blocks work.
Neuromodulation and Nerve Ablation
For longer-lasting relief, we offer more advanced techniques that modify or interrupt nerve signals.
- Radiofrequency ablation (RFA) uses radiofrequency energy to create a lesion on a nerve, stopping it from sending pain signals for months or even years. It is highly effective for chronic pain from facet or sacroiliac joints. Read about the radiofrequency ablation procedure and recovery.
- Spinal cord stimulation (SCS) involves implanting a small device that delivers gentle electrical impulses to the spinal cord, interfering with pain signals before they reach the brain. You control the device with a remote. SCS works well for neuropathic pain, failed back surgery syndrome, and CRPS. Spinal cord stimulators have transformed lives for many patients.
- Intrathecal pain pumps are implanted devices that deliver tiny, continuous doses of medication directly into the spinal fluid. This provides superior pain relief with far fewer side effects than oral medication.
- The Intracept Procedure is a newer technique that targets the basivertebral nerve inside the vertebrae to treat chronic low back pain stemming from vertebral endplate issues. Learn more about the Intracept Procedure and if you are a candidate.
At the Center for Specialty Care, we stay current with these developments to offer you the most effective, evidence-based treatments available.
Benefits, Risks, and Improving Quality of Life
The primary goal of interventional pain medicine is to help you reclaim your life from chronic pain. We’ve seen patients in Fairmont, Estherville, Buffalo Center, and St. James return to activities they love, like gardening or playing with grandchildren.
Key benefits include:
- Significant pain reduction: By targeting the pain source, many patients achieve more relief than with oral medications.
- Improved function and mobility: Less pain means you can move more freely and perform daily tasks with greater ease.
- Minimally invasive nature: Procedures involve small needle punctures and quick recovery times, often helping you avoid major surgery.
- Reduced need for opioids: Direct treatment can decrease or eliminate your reliance on systemic pain medications and their side effects.
While generally safe, these procedures have potential risks, which we will discuss with you in detail. These include a small risk of infection, bleeding or bruising at the injection site, and, rarely, nerve injury or allergic reactions to medication.
This is why the importance of specialist training is critical. Our board-certified pain specialists have extensive training in these intricate procedures. We use advanced imaging guidance (fluoroscopy or ultrasound) to ensure precision, which dramatically improves both safety and effectiveness. Our specialists’ experience minimizes risks and ensures you receive the highest standard of care. A comprehensive review of interventional procedure safety highlights the continuous improvements in this field.
At Center for Specialty Care, we are committed to personalized care and transparent communication. We’ll ensure you feel comfortable and informed, because for many patients, these procedures are the key to managing chronic pain and getting back to the life they want to live.
The Future of Interventional Pain Medicine
The field of interventional pain medicine is rapidly advancing, driven by new technology and a deeper understanding of pain. For our patients at the Center for Specialty Care, this means more effective treatments today and even more promising options on the horizon.
Technology and Innovation
Advanced imaging techniques, like high-resolution ultrasound and real-time fluoroscopy, allow our specialists to see anatomical structures with remarkable clarity. This real-time visualization enables pinpoint accuracy, enhancing both the safety and effectiveness of every procedure.
Regenerative Medicine
Regenerative medicine is an exciting frontier that uses your body’s own healing abilities to repair damaged tissues.
- Platelet-Rich Plasma (PRP) therapy uses a concentration of your own blood platelets, rich in growth factors, to stimulate natural healing in injured tendons, ligaments, and joints.
- Stem cell therapy uses your body’s stem cells to promote tissue repair and regeneration, offering hope for genuine healing in conditions like severe arthritis.
Precision Medicine and AI
The future of pain management is precision medicine, where treatments are custom to an individual’s unique biology. Artificial intelligence (AI) will help us analyze vast amounts of data to create highly personalized treatment plans, predicting which interventions will be most effective for you.
These innovations promise more minimally invasive options, shorter recovery times, and more lasting pain relief. For a deeper look at where the field is headed, this review of future directions in interventional pain management offers valuable insights. At the Center for Specialty Care, we are committed to staying at the forefront of these advances.
Frequently Asked Questions about Interventional Pain Medicine
We know you have questions about interventional pain medicine. Here are answers to the ones we hear most often.
Are the procedures painful?
We take every measure to ensure your comfort. Most procedures begin with a local anesthetic to numb the treatment area, so you should only feel pressure, not sharp pain. We can also offer sedation options to help you relax.
It’s normal to have some post-procedure soreness at the site, similar to muscle tenderness after a workout. This usually resolves in a day or two and can be managed with ice and over-the-counter pain relievers. We will provide detailed instructions to minimize discomfort.
How long does the relief last?
The duration of relief varies depending on the procedure, your condition, and your body’s response.
- Diagnostic procedures, like some nerve blocks, may provide temporary relief for a few hours or days, helping us confirm your pain source.
- Therapeutic procedures offer longer-lasting relief. Epidural injections can last for weeks or months, while treatments like radiofrequency ablation or spinal cord stimulation can provide relief for many months or even years.
We will discuss the goals of your procedure and the potential need for repeat procedures to maintain pain control as part of your long-term treatment plan.
Is interventional pain medicine covered by insurance?
Coverage varies by insurance plan and the specific procedure. Most major insurers, including Medicare, cover many interventional pain medicine procedures when they are deemed medically necessary.
A pre-authorization process is often required, and our team is experienced in handling this paperwork on your behalf. We follow all Medicare guidelines and work to provide a clear picture of any potential out-of-pocket costs during your consultation. We encourage you to also contact your insurance provider to verify your benefits. Our goal is transparency, so you can focus on getting better.
Take Control of Your Chronic Pain
Living with chronic pain is overwhelming, but it is manageable, and you don’t have to face it alone.
Interventional pain medicine offers sophisticated, targeted treatments that address the actual source of your discomfort. Instead of masking pain with medication or facing major surgery, these minimally invasive procedures provide a transformative path for many patients.
Your pain is unique, which is why we provide personalized care. Our team at the Center for Specialty Care is committed to 100% patient satisfaction, and we prioritize quick appointment availability across our locations in Fairmont MN, Estherville IA, Buffalo Center IA, and St James MN because we know you can’t wait for relief.
Imagine regaining your quality of life—playing with grandchildren, sleeping through the night, or returning to your favorite hobbies. Picture reducing your reliance on pain medication or avoiding surgery. These are achievable outcomes.
You’ve been strong for so long. Now, let us help you find a better way forward. We encourage you to learn more about our comprehensive pain management services and find how these advanced treatments could work for you. You deserve to feel better and reclaim the life that chronic pain has been stealing from you.