Signs You Might Have a Torn Rotator Cuff
April 18, 2026
Tendinitis: The Lowdown on Those Pesky Tendon Inflammations
April 21, 2026The sleepy side of Intracept procedure anesthesia
What You Need to Know About Intracept Procedure Anesthesia
Intracept procedure anesthesia is how your care team keeps you comfortable during a minimally invasive treatment for chronic low back pain called basivertebral nerve ablation. Here is a quick snapshot of what to expect:
- Type of anesthesia: General anesthesia or IV sedation with local anesthetic
- Who gives it: An anesthesiologist or Certified Registered Nurse Anesthetist (CRNA)
- How long it lasts: Covers the full 60-90 minute outpatient procedure
- Recovery: Monitored for up to one hour after the procedure before going home
- Key prep steps: Follow fasting guidelines, disclose all medications, and arrange a driver
- Complication rate: Less than 0.3% in clinical trials
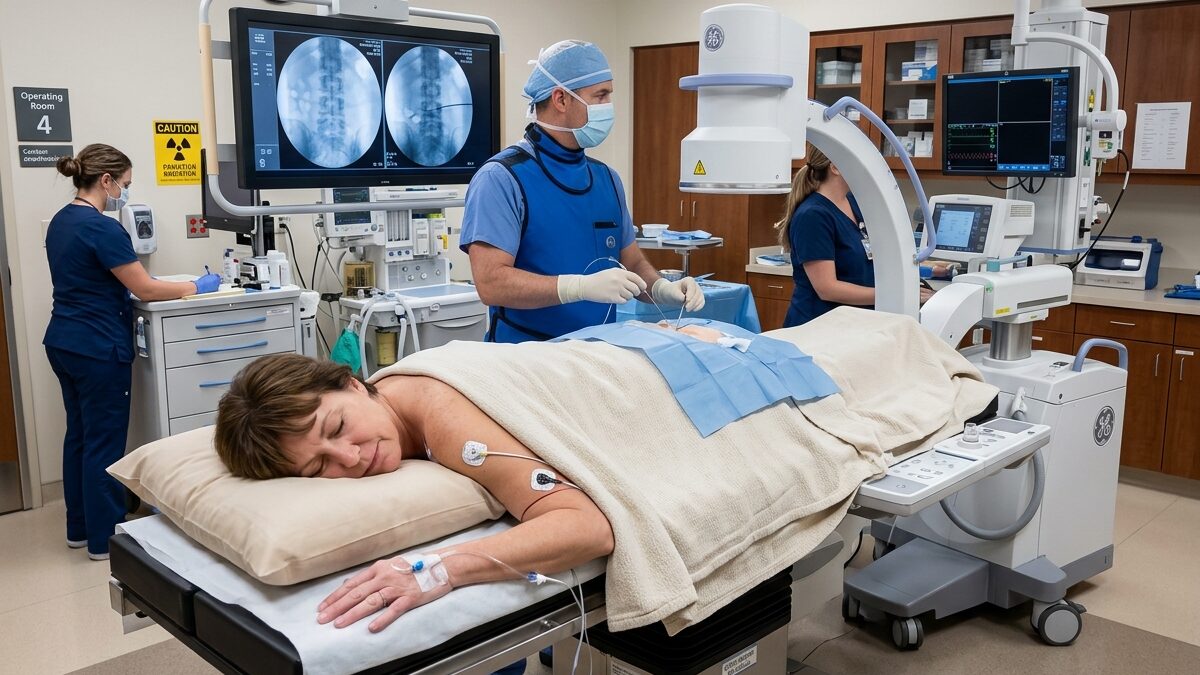
If you have been dealing with chronic low back pain for six months or more — and conservative treatments like physical therapy, injections, or medications haven’t helped — you may be a candidate for the Intracept procedure. It is a one-time, outpatient treatment that uses radiofrequency energy to ablate the basivertebral nerve inside the vertebra, stopping pain signals at their source. Before any of that happens, though, your care team needs to get you safely and comfortably under anesthesia. That part of the process matters more than most patients realize — and it is exactly what this guide covers.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon with over 30 years of experience performing minimally invasive procedures, including spine treatments that require careful anesthesia planning like intracept procedure anesthesia. At the Center for Specialty Care in Fairmont, Minnesota, our team is committed to making sure every patient is fully prepared and at ease before, during, and after their procedure.
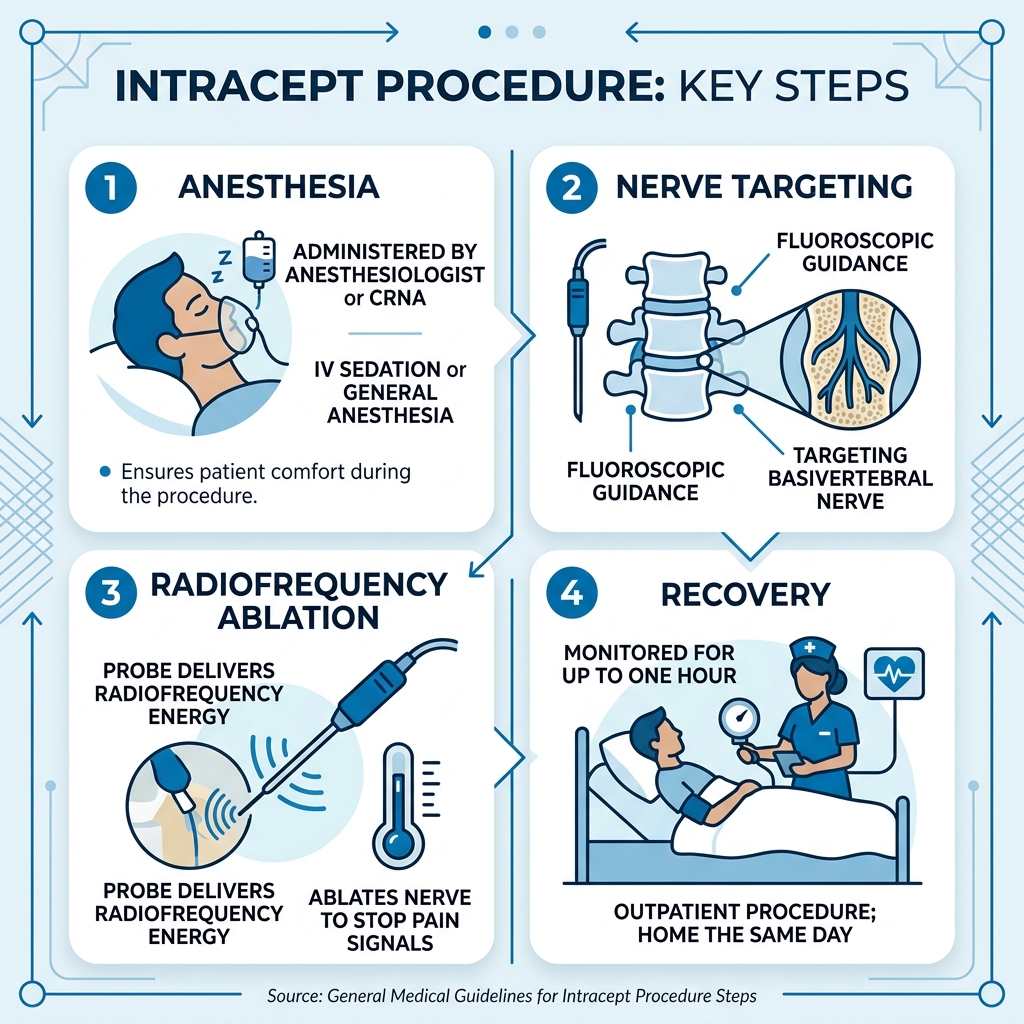
Key terms for intracept procedure anesthesia:
Understanding Intracept Procedure Anesthesia Options
When we talk about the Intracept Procedure, the first question many patients ask is, “Am I going to be awake?” The short answer is that we prioritize your comfort and safety above all else. Because this procedure involves precisely navigating a cannula into the vertebral body (the bone of your spine), it is vital that you remain still and pain-free.
To achieve this, we typically use one of two primary methods: general anesthesia or monitored anesthesia care (IV sedation) combined with a local anesthetic.

- General Anesthesia: This is often the preferred choice. It ensures you are completely asleep and unaware of the procedure. It also allows the medical team to manage your breathing and ensure total muscle relaxation, which is helpful when we are working with millimeter-level precision in the spine.
- IV Sedation: Also known as “twilight sleep,” this involves administering sedative medications through an IV. You are technically “asleep” but may be able to breathe on your own without a ventilator. We combine this with a local anesthetic at the incision site to block pain.
While the Intracept procedure is a minimally invasive outpatient treatment, the choice of anesthesia is a medical decision made by our specialists based on your health history and the complexity of the ablation.
Is General Anesthesia Always Required?
General anesthesia is not “always” required in the strictest sense, but it is the standard for most providers. The goal of intracept procedure anesthesia is to ensure you don’t move. Even a small flinch while the radiofrequency probe is being positioned can affect the accuracy of the treatment.
For patients who have specific concerns or contraindications for general anesthesia, deep sedation alternatives can be discussed. However, most patients find that general anesthesia provides the most “seamless” experience—you go to sleep, and the next thing you know, you are waking up in recovery with the procedure already finished. Our Pain Management team will walk you through these options during your consultation to find the best fit for your needs.
Who Administers the Anesthesia?
You aren’t just in the hands of your surgeon; you have a dedicated anesthesia provider whose sole job is to monitor your vitals. At the Center for Specialty Care, your anesthesia may be managed by an Anesthesiologist or a highly skilled Richard Kilgore CRNA.
A Certified Registered Nurse Anesthetist (CRNA) is an advanced practice nurse with specialized training in administering anesthesia and monitoring patients during surgery. They stay by your side from the moment you “go under” until you are safely awake. They track your heart rate, blood pressure, and oxygen levels every second of the 60-90 minute procedure. Knowing our experienced providers are focused entirely on your safety allows us to focus on the precision of the nerve ablation.
Preparing for Your Basivertebral Nerve Ablation
Proper preparation is the secret to a smooth anesthesia experience. Think of it like a pre-flight checklist for a pilot; every step ensures a safe “takeoff” and “landing.”
Pre-Procedure Fasting and Medications
Because intracept procedure anesthesia (specifically general anesthesia or deep sedation) can affect your body’s ability to protect your airway, you must follow strict fasting guidelines. This is often referred to as “NPO” status (nothing by mouth).
- Fasting: Typically, you cannot eat or drink anything (including water, gum, or mints) after midnight the night before your surgery.
- Medication Adjustments: We will review your current medications. You may be asked to stop taking blood thinners, certain supplements, or anti-inflammatory drugs several days before the procedure to reduce the risk of bleeding.
- Transportation: You must have a responsible adult driver to take you home. Anesthesia stays in your system for hours, and you will not be legally or physically able to drive yourself after discharge.
For more details on the timeline, you can view the official steps for getting started with Intracept.
Positioning and Patient Preparation
Once you are in the procedure room and the anesthesia begins to take effect, our team will assist in positioning you. For the Intracept procedure, you will be placed in the prone position (lying face down).
This position is necessary because the basivertebral nerve is accessed through the back of the vertebrae. We use specialized pillows and bolsters to protect pressure points and ensure your spine is aligned correctly for the Back & Spine specialists to work. Throughout the procedure, we use fluoroscopic guidance (real-time X-ray) to see exactly where the instruments are moving while you remain comfortably asleep.
Administering intracept procedure anesthesia: Step-by-Step
What actually happens when you “go under”? Here is the typical flow:
- IV Insertion: A small catheter is placed in your arm to deliver fluids and medications.
- Pre-oxygenation: You may breathe oxygen through a mask for a few minutes to saturate your system.
- Induction: The anesthesia provider administers medication through the IV. Within seconds, you drift into a deep sleep.
- Maintenance: During the 60-90 minute procedure, the provider adjusts the levels of anesthesia to keep you at a consistent level of sleep.
- The Procedure: While you sleep, we create a small 1-cm incision, insert the Intracept tools, and use radiofrequency heat to ablate the nerve (usually 7-15 minutes per spinal level).
- Emergence: Once the ablation is complete and the incision is closed with a simple bandage, the anesthesia is tapered off, and you begin to wake up.
Safety, Risks, and Contraindications of intracept procedure anesthesia
Safety is our top priority. One of the most reassuring statistics regarding the Intracept procedure is the exceptionally low complication rate. In clinical trials, the rate of procedure-related complications was less than 0.3%.
Common Side Effects and Risks
Most side effects of intracept procedure anesthesia are mild and temporary. You might experience:
- Drowsiness: Feeling “foggy” for several hours.
- Nausea: Some patients are sensitive to anesthesia; we can often provide anti-nausea meds in your IV to prevent this.
- Sore Throat: If a breathing tube or laryngeal mask was used, your throat might feel scratchy for a day or two.
- Injection Site Soreness: Minor bruising or tenderness where the IV was placed.
While rare, risks specific to the procedure (not just the anesthesia) include infection, bleeding, or temporary nerve irritation. These are similar to the risks associated with other spinal treatments, such as epidural steroid injections.
Contraindications for Anesthesia Candidates
Not everyone is a candidate for the Intracept procedure or the anesthesia required to perform it. We carefully screen for:
- Heart and Lung Conditions: Severe heart failure or advanced COPD may make general anesthesia too risky.
- Active Infection: We cannot perform the procedure if you have a systemic infection.
- Pregnancy: Anesthesia and fluoroscopy are generally avoided during pregnancy.
- Implanted Devices: Patients with pacemakers or other electronic implants need special clearance, as the radiofrequency energy can interfere with these devices.
- Skeletal Maturity: The procedure is not for those who are still growing (skeletally immature).
Our Orthopedics and pain specialists perform a thorough medical history review and physical exam to ensure you meet all safety criteria.
Recovery and Post-Anesthesia Care
After the procedure is finished, you aren’t rushed out the door. You will be moved to the Post-Anesthesia Care Unit (PACU), where you will be monitored as you fully wake up.
The First Hour
You will spend about 60 minutes in recovery. Our nursing staff will check your vitals, monitor the incision site, and ensure you can manage small sips of water. Once you are alert, your pain is stable, and you can stand or walk safely, you will be cleared for discharge to your driver.
Many patients are surprised by how quickly they feel “back to normal” after the anesthesia wears off, though you will still need plenty of rest. You can read about others’ experiences in these Intracept patient stories.
The First 48 Hours Post-Procedure
When you get home to Fairmont or your local community, your main job is to relax.
- Rest: Avoid any strenuous activity or heavy lifting for at least 48 hours.
- Incision Care: Keep the small bandage clean and dry.
- Pain Management: It is normal to feel some “procedural soreness” at the incision site. This is different from your chronic back pain and can usually be managed with over-the-counter relievers or ice packs.
- Activity: Light walking is encouraged to keep your blood flowing, but don’t overdo it.
Most of our patients return to light work within 2-3 days, provided their job doesn’t involve heavy manual labor. We provide a personalized recovery plan for every Back patient we treat.
Long-term Outcomes and Pain Relief
The beauty of the Intracept procedure is that the basivertebral nerve does not typically regrow. This means the relief is designed to be durable.
- Onset: Some patients feel better within two weeks, though it may take up to three months to see the full benefit as inflammation subsides.
- Durability: Clinical data shows that improvements in pain and function can last five years or more.
- Success: In a 2023 study, 65% of patients reported at least a 50% reduction in pain at the 6-month mark.
This long-term success makes the 90 minutes of anesthesia well worth the “nap.” It is a much more permanent solution than many other arthroscopic or minimally invasive options.
Frequently Asked Questions about Intracept Procedure Anesthesia
| Feature | Intracept Anesthesia | Standard RFA (Radiofrequency Ablation) |
|---|---|---|
| Primary Method | General Anesthesia / Deep Sedation | Local Anesthetic / Mild Sedation |
| Duration | 60 – 90 Minutes | 30 – 45 Minutes |
| Patient Position | Prone (Face Down) | Prone (Face Down) |
| Recovery Time | 60 Minutes in PACU | 15 – 30 Minutes |
| Incision Size | ~1 cm | Needle Puncture |
How long does the anesthesia last during the procedure?
The intracept procedure anesthesia is designed to cover the entire surgical window, which is usually between 60 and 90 minutes. The anesthesia provider will maintain your level of sleep throughout the entire process. Once the radiofrequency probe is removed and the incision is closed, they stop the medication, and you typically wake up within 5 to 10 minutes.
Does the choice of anesthesia affect the final outcome?
In terms of the nerve being “successfully” ablated, the anesthesia doesn’t change the physics of the radiofrequency energy. However, it does affect the precision. Because we are working inside the vertebral body, having a patient who is completely still allows the surgeon to be as precise as possible. This precision is what leads to those proven results and high patient satisfaction rates.
How intracept procedure anesthesia Compares to Radiofrequency Ablation
You might be familiar with standard Radiofrequency Ablation (RFA) for the medial branch nerves (facet joint pain). Standard RFA is often done with just local numbing or very light sedation.
Intracept procedure anesthesia is generally “deeper” because we are entering the bone rather than just placing a needle near a joint. While standard RFA often needs to be repeated every 6-12 months, Intracept is a one-time procedure. We take the anesthesia a step further to ensure you are comfortable for this more definitive treatment.
Conclusion
At the Center for Specialty Care, we understand that any procedure involving anesthesia can feel a bit daunting. However, intracept procedure anesthesia is a highly controlled, safe, and routine part of providing long-term relief for vertebrogenic pain. Our team in Fairmont is here to provide personalized care, ensuring that from the moment you walk in to the moment your driver takes you home, you feel supported and safe.
If you are tired of living with chronic low back pain and want to see if this “one-and-done” procedure is right for you, we are ready to help. Our commitment to 100% patient satisfaction means we take the time to answer every question about your surgery, your recovery, and your “sleepy side” of the treatment.
Don’t let back pain steal another day. Schedule your Intracept consultation with our specialists today.