Cool Down or Warm Up? Deciding on Heat or Ice for Peroneal Tendonitis
September 3, 2025
The Ultimate Guide to Physical Therapy for Rotator Cuff Tears
September 5, 2025Does Medicare Cover Intracept Procedure: Key 2 Relief
Understanding Medicare Coverage for Intracept: What You Need to Know
Does medicare cover intracept procedure? Yes, Medicare covers the Intracept procedure under specific conditions outlined in Local Coverage Determination (LCD) L39644, but only when strict medical necessity criteria are met.
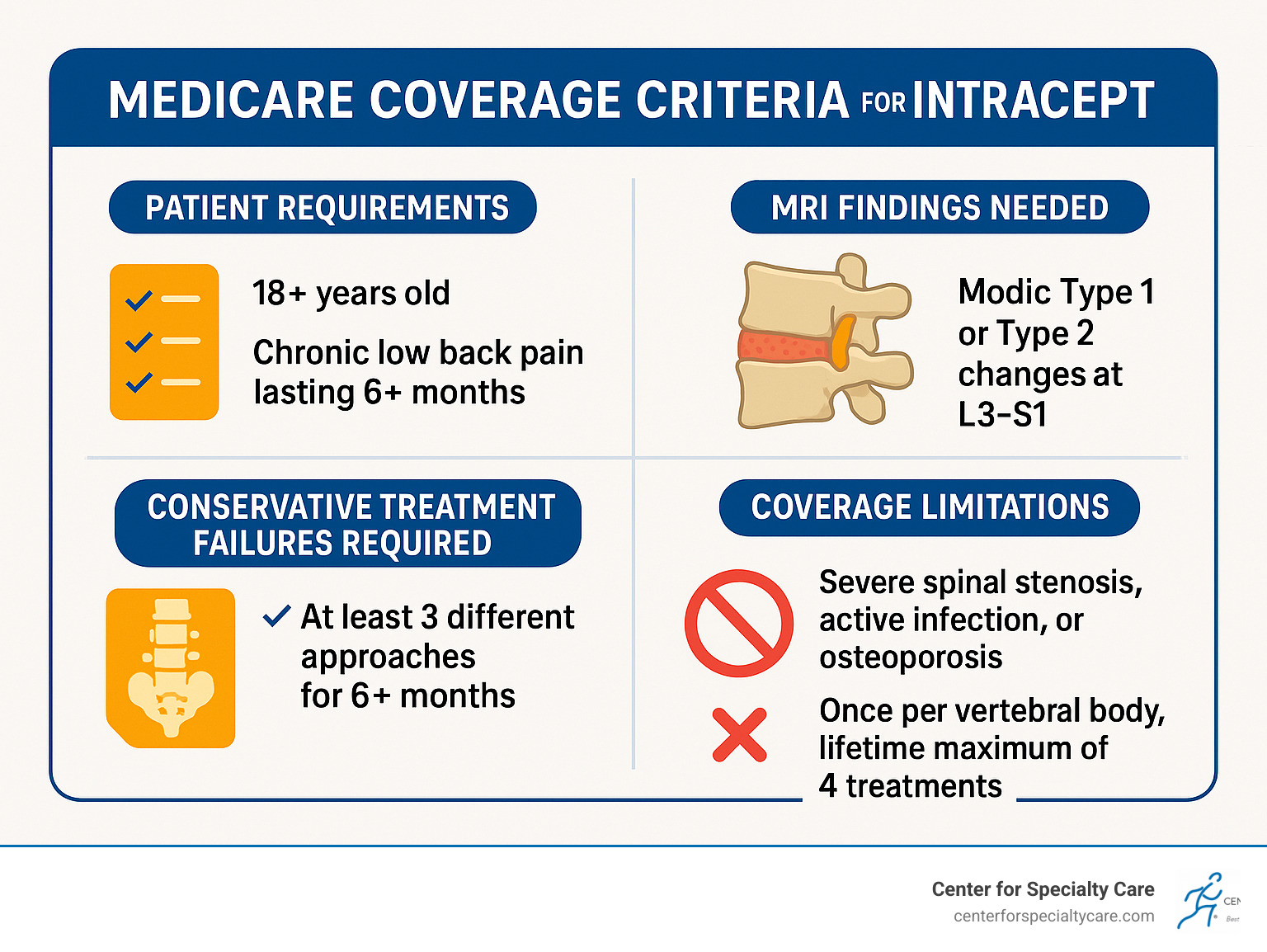
Quick Answer – Medicare Coverage Requirements:
- ✓ Chronic low back pain lasting 6+ months
- ✓ Failed conservative treatment (at least 3 different approaches for 6+ months)
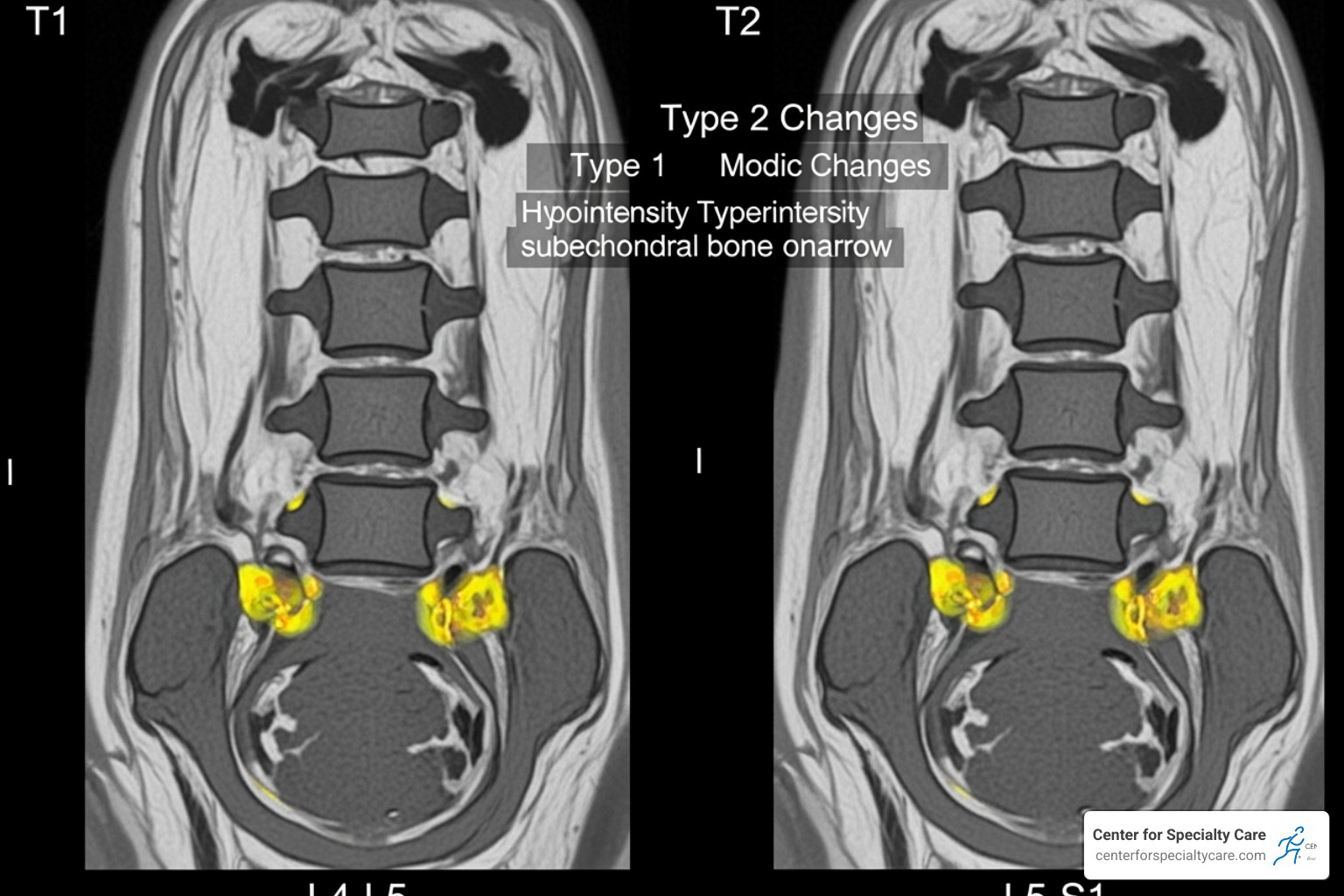
- ✓ MRI showing Modic Type 1 or Type 2 changes in vertebrae L3-S1
- ✓ Patient must be 18+ years old (skeletally mature)
- ✗ Cannot have severe spinal stenosis, active infection, or osteoporosis
- ✗ Limited to once per vertebral body, lifetime maximum of 4 treatments
Chronic low back pain affects nearly 80% of adults at some point in their lives, with about 20% developing chronic pain lasting 12 weeks or longer. For many Medicare beneficiaries struggling with this debilitating condition, the Intracept procedure offers hope when traditional treatments have failed.
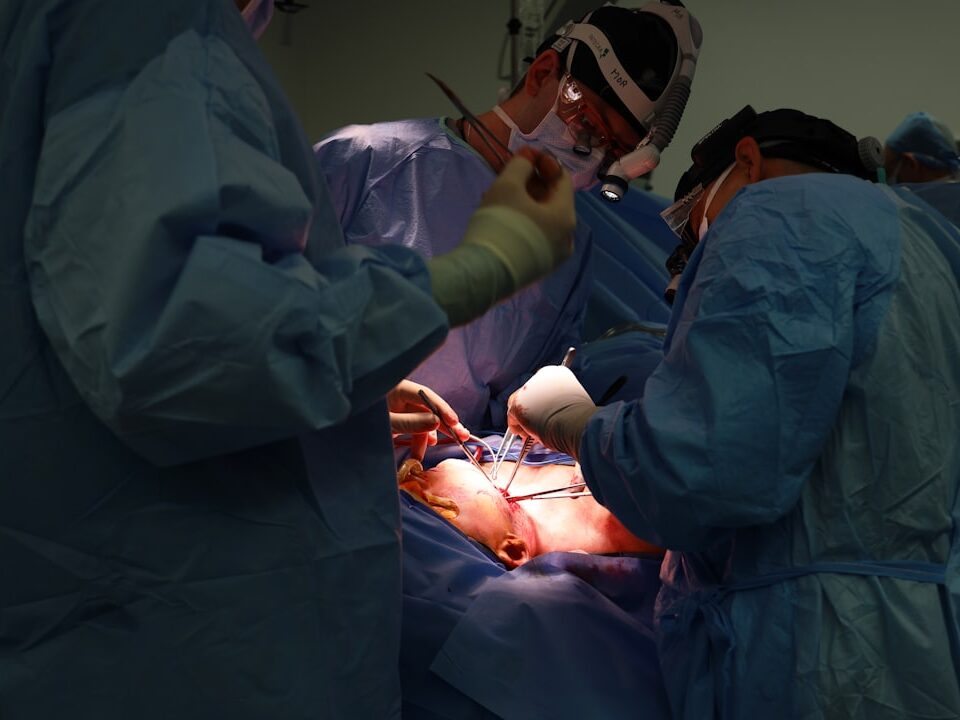
The Intracept procedure targets a specific type of back pain called vertebrogenic pain – pain originating from nerves within the vertebrae themselves, not from discs or other structures. This minimally invasive treatment uses radiofrequency energy to treat the basivertebral nerve, potentially providing lasting relief without spinal implants.
However, navigating Medicare coverage can feel overwhelming. While Medicare does cover this innovative procedure, understanding the specific requirements, limitations, and reimbursement details is crucial for patients considering this treatment option.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon. At the Center for Specialty Care, I have extensive experience helping patients steer complex spine treatments and insurance coverage questions, like does medicare cover intracept procedure. We’ve guided countless Medicare patients through the process of accessing innovative pain management solutions like Intracept when they meet the necessary criteria.
What is the Intracept Procedure?
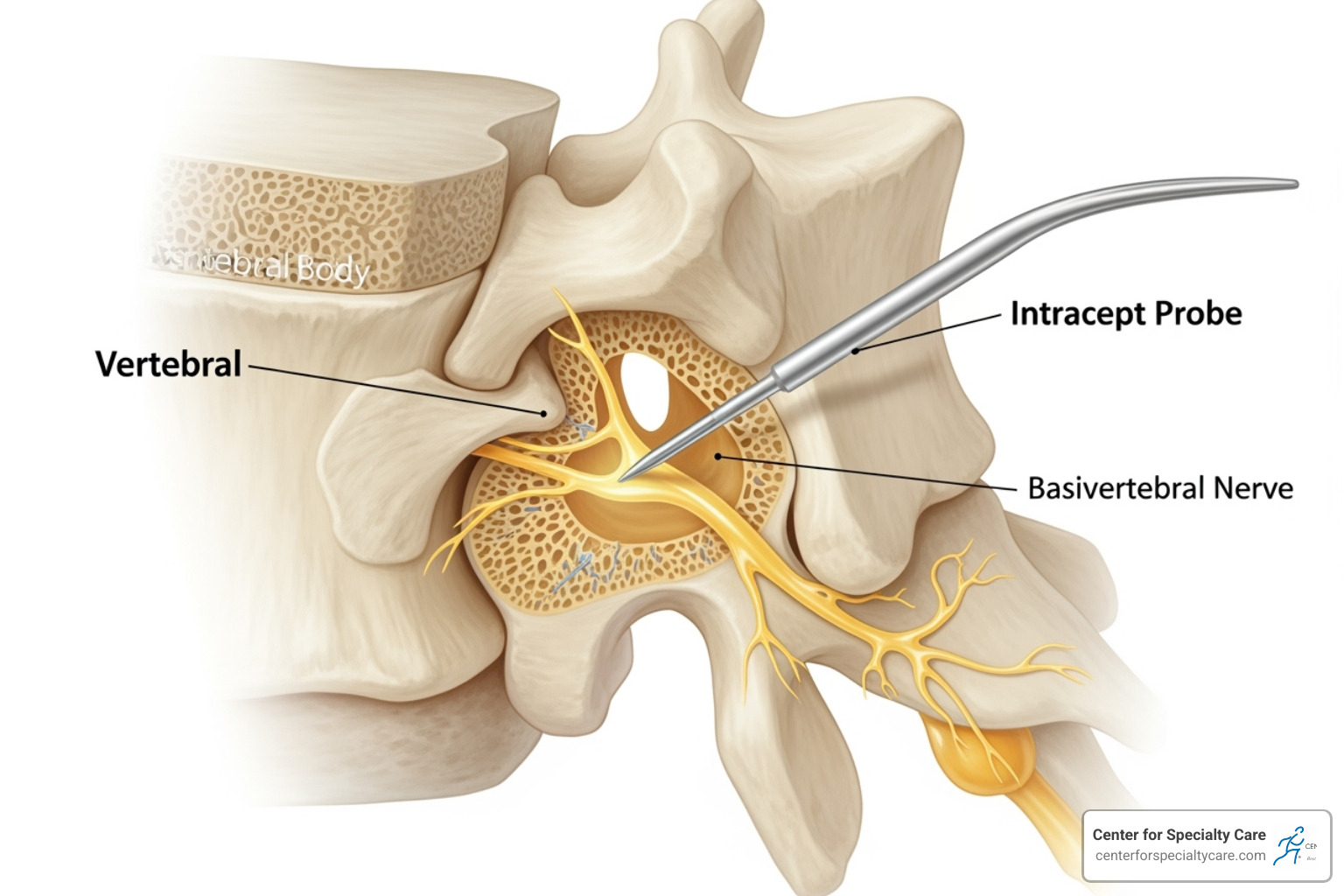
The Intracept procedure is a breakthrough for vertebrogenic pain—a type of chronic low back pain originating from nerves inside the vertebral bones, not from discs or muscles. Unlike treatments that focus on spinal discs, Intracept targets the basivertebral nerve (BVN), which transmits pain signals from the vertebrae to the brain. Using radiofrequency ablation (precisely applied heat), the procedure interrupts these pain signals at their source.
A key benefit is that Intracept involves no spinal implants and preserves your spine’s natural structure and movement. The system received FDA approval in 2019, and we are proud to offer this innovative treatment as part of our Back and Spine care services.
Who is a Candidate for Intracept?
Ideal candidates for Intracept meet specific criteria. You must be skeletally mature (18+) with chronic low back pain for at least six months that significantly impacts your daily life. A critical requirement is having failed at least six months of conservative care. This includes documented attempts at treatments like physical therapy, chiropractic care, medications, and injection therapies. Our Pain Management team will carefully review your history to confirm this.
Finally, the diagnosis must be confirmed by MRI findings showing Modic Type 1 or Type 2 changes in your lower back vertebrae (L3 to S1). These changes are specific indicators of vertebrogenic pain. Given the high prevalence of back pain, many people who have not found relief with other treatments may be candidates.
How Intracept Provides Lasting Relief
Intracept is a minimally invasive outpatient procedure that takes about an hour, with no hospital stay or implants. Using imaging guidance, a small probe is placed to target the basivertebral nerve directly with radiofrequency energy. This deadens the pain signals without harming the spine’s structure.
The results can be life-changing, as highlighted in Carson Daly’s Intracept story. The treatment’s long-term effectiveness is a key benefit. Clinical studies show significant pain relief and improved function lasting for five years or more. This advancement in Orthopedics addresses the root cause of vertebrogenic pain, offering hope for a return to an active lifestyle.
Does Medicare Cover the Intracept Procedure? The Official Stance
So, does medicare cover intracept procedure? Yes, but only when specific criteria for medical necessity are met. Medicare acts as a gatekeeper, ensuring this innovative treatment is used for patients who will truly benefit. Coverage is defined by Local Coverage Determinations (LCDs), such as the CMS policy for BVN Ablation (L39644). These policies state that the procedure is covered only for vertebrogenic pain—pain originating from within the vertebrae—and only after conservative treatments have failed. At Center for Specialty Care, we follow these guidelines closely.
Key Criteria: When does Medicare cover the Intracept procedure?
To determine if Medicare will cover the Intracept procedure, we use a comprehensive checklist. Every requirement must be met for approval:
- Age: You must be skeletally mature (18+).
- Pain History: You must have chronic low back pain for at least six months that causes significant functional impairment.
- Conservative Care Failure: You need documented failure of at least three different types of non-surgical management over a six-month period. This can include physical therapy, chiropractic care, medications, or injections.
- MRI Confirmation: An MRI must show Modic Type 1 or Type 2 changes in one or more vertebrae from L3 to S1. These changes are key indicators of vertebrogenic pain.
- Exclusion of Other Conditions: Your pain cannot be explained by other conditions like fractures, tumors, infections, or severe spinal deformities.
- Overall Health: You must pass a physical and psychological assessment to ensure you are a suitable candidate for the procedure.
What Diagnosis and Procedure Codes Does Medicare Recognize?
Medical billing uses specific codes to communicate with Medicare. Our specialists use these to ensure your claims are processed smoothly, following guidance from resources like the CMS Billing and Coding Article (A59466).
- Diagnosis Code (ICD-10): The primary code is M54.51 (Vertebrogenic low back pain), which specifies the exact condition Intracept treats.
- Procedure Codes (CPT): The procedure is billed using CPT code 64628 for the first two vertebral bodies and the add-on code +64629 for each additional vertebral body.
Understanding Coverage Limitations and Exclusions
Medicare has specific limitations to ensure patient safety and appropriate use. Understanding these helps set realistic expectations.
- Lifetime Limit: The procedure is covered only once per vertebral body per lifetime, with a maximum of four vertebral bodies treated in total.
- Session Limit: No more than two vertebral levels can be treated in a single session.
- Location Limit: Coverage is limited to vertebral bodies from L3 to S1.
Exclusions: Medicare will not cover the procedure if you have:
- Severe heart or lung problems, active infections, bleeding disorders, or osteoporosis.
- Radicular pain (shooting leg pain) as your primary symptom.
- Other causes for your pain, such as severe spinal stenosis, tumors, or large disc herniations.
- A BMI over 40 or active substance abuse (under some policies).
- Previous surgery at the same spinal level (with some exceptions).
Additionally, Intracept cannot be performed during the same session as other spinal injections at the same level.
Navigating the Financials: Reimbursement and Appeals
Understanding the financial side of medical procedures is key. When considering does medicare cover intracept procedure, it’s helpful to know how reimbursement works.
Medicare payment rates vary based on geographic location and where the procedure is performed, such as a Hospital Outpatient Department (HOPD) or an Ambulatory Surgical Center (ASC). These rates, which cover both the physician’s service and the facility fee, are updated annually. Your final out-of-pocket cost will depend on your specific Medicare plan, whether you have supplemental insurance, and if you’ve met your annual deductible.
At Center for Specialty Care, we provide transparent Patient Information regarding potential costs to help you plan and avoid surprises.
How Does Medicare Coverage Compare to Private Insurance?
While Medicare has clear, standardized rules, private insurance policies vary. Many major insurers, like Humana, Anthem, and Cigna, now cover Intracept, but some may still consider it investigational. The key differences are:
- Standardization: Medicare’s criteria are consistent nationwide through its LCDs. Private insurer policies can differ significantly from plan to plan.
- Prior Authorization: Unlike Traditional Medicare, nearly all private plans require prior authorization before the procedure can be performed. This means we must submit documentation and get approval from your insurance company first.
- Reimbursement: Rates are negotiated individually between insurers and providers.
Workers’ Compensation and auto insurance may also cover the procedure if the injury is work- or accident-related, each with its own approval process.
What if Medicare does not cover the Intracept procedure?
A claim denial from Medicare isn’t the end of the road. Denials often result from simple issues like incomplete documentation, coding errors, or not clearly meeting medical necessity criteria. When this happens, there is a formal appeals process.
Our team is experienced in navigating Medicare appeals. The first step is a redetermination, where we resubmit the claim with more detailed information. This often includes a letter of medical necessity from your doctor, which outlines your pain history, failed treatments, and the clinical reasoning for recommending Intracept. Thorough physician documentation is the key to a successful appeal.
If the initial appeal is unsuccessful, there are further levels of review. The process can seem daunting, but you are not alone. We support our patients every step of the way, building a strong case to help you get the coverage you deserve.
The Patient Journey with Intracept
Starting on the Intracept journey is about more than just addressing the question does medicare cover intracept procedure – it’s about taking a meaningful step toward reclaiming your life from chronic pain. Once you’ve discussed the procedure with our team at Center for Specialty Care, and we’ve determined you meet both the clinical criteria and Medicare coverage requirements, we’ll walk alongside you through every step of this process.
Your journey begins with hope backed by science. The clinical evidence supporting Intracept isn’t just impressive numbers on a page – it represents real people who’ve found relief when other treatments failed. For Medicare beneficiaries especially, who often have complex health profiles and have tried numerous treatments over the years, having a procedure with proven, long-lasting outcomes makes all the difference.
What Evidence Supports Intracept for Medicare Beneficiaries?
The strong clinical evidence for Intracept is a key reason Medicare provides coverage. For beneficiaries who have struggled with chronic pain, this research offers real hope. Landmark studies, like the INTRACEPT Trial, demonstrate significant benefits:
- Substantial Pain Relief: A large majority of patients experience a 50% or greater reduction in pain, with many achieving complete relief.
- Improved Function: Patients show major improvements in functional ability, allowing them to return to daily activities that were previously impossible.
- Long-Term Results: The benefits are durable, with studies showing sustained pain relief and functional improvement for five years or more.
- Excellent Safety Profile: The procedure has a low rate of complications, and leading medical societies give it their highest recommendation for appropriately selected patients.
Are There Different Rules for Medicare Advantage Plans?
If you have a Medicare Advantage (Part C) plan, the rules can be different. These plans are run by private insurers and, while they must cover everything Original Medicare (Parts A & B) does, they have their own operating procedures.
Key differences include:
- Prior Authorization: Unlike Original Medicare, Medicare Advantage plans almost always require prior authorization. We must get approval from your plan before scheduling the procedure to ensure coverage.
- Network Requirements: You must ensure that Center for Specialty Care is in your plan’s network to get the highest level of coverage. Out-of-network care may cost you more or not be covered at all.
- Plan-Specific Policies: Each plan has its own policy language and may require different documentation, as shown in this example of a Medicare Advantage policy.
Our patient care coordinators are experienced with these plans and will help you verify your coverage and steer the prior authorization process.
Your Next Steps for Chronic Back Pain Relief
Living with chronic low-back pain doesn’t have to be your reality forever. We know how exhausting it can be when every movement reminds you of that constant ache, when getting out of bed feels like climbing a mountain, and when you’ve tried everything but nothing seems to work.
The Intracept procedure represents a targeted solution that goes straight to the source of vertebrogenic pain. Unlike treatments that mask symptoms, this innovative approach actually addresses the basivertebral nerve that’s been sending those relentless pain signals from your vertebral endplates.
So, does medicare cover intracept procedure? Absolutely – but only when you meet their specific requirements. You’ll need MRI-confirmed Modic changes, at least six months of chronic pain, and documented proof that conservative treatments haven’t worked. It sounds like a lot of hoops to jump through, but these criteria exist to ensure the procedure helps the right patients.
At Center for Specialty Care, we’ve guided countless patients through this journey. Our approach is simple: we take the time to properly diagnose your condition, thoroughly document your treatment history, and determine if Intracept is truly the right fit for your unique situation. No rushing, no guesswork – just personalized care custom to your specific needs.
Our Our Providers understand that navigating Medicare coverage can feel overwhelming. That’s why we handle the complex paperwork and work directly with Medicare to ensure your case is presented correctly. We know which documentation Medicare needs, how to demonstrate medical necessity, and what criteria must be met for approval.
Quick appointment availability means you won’t wait months to get answers. We believe that when you’re in pain, time matters. Our commitment to 100% patient satisfaction drives everything we do – from your first consultation through your recovery and beyond.
If you’re tired of living with chronic back pain and think the Intracept procedure might be your path to relief, we’re here to help. Don’t spend another day wondering “what if?” when relief could be within reach.
Contact Us today to schedule your consultation at one of our convenient locations in Fairmont MN, Estherville IA, Buffalo Center IA, or St James MN. Let’s work together to get you back to the life you love.
Learn more about the Intracept Procedure and if you are a candidate
Your journey toward lasting pain relief starts with a single phone call. We’re ready when you are.