Is Heat Good for Jumper’s Knee? Understanding Its Benefits
September 17, 2025
Supraspinatus Tear: Your Guide to Understanding This Common Injury
September 19, 2025Nerve ablation procedure for back pain: Maximize Relief 2025
A Modern Solution for Chronic Back Pain
The nerve ablation procedure for back pain uses targeted heat to interrupt pain signals traveling from damaged spinal nerves to your brain. Also known as radiofrequency ablation, this minimally invasive treatment offers lasting relief for chronic back pain that hasn’t responded to medications, physical therapy, or injections. Studies show it can provide significant, lasting relief for pain in the lower back and neck, with many patients experiencing at least a 50% improvement.
Key Facts About Nerve Ablation for Back Pain:
- What it treats: Facet joint arthritis, sacroiliac joint pain, and vertebrogenic pain
- How it works: Heat destroys specific nerves that transmit pain signals
- Pain relief duration: 6-18 months, with the option to repeat
- Procedure time: 30-90 minutes as an outpatient
- Success rate: Over half of patients experience significant improvement
- Recovery: Most return to normal activities within days to weeks
If you’re one of the millions of adults affected by chronic back pain, nerve ablation offers hope when traditional treatments fall short.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon with over three decades of experience treating musculoskeletal conditions in southern Minnesota and northern Iowa. At the Center for Specialty Care, I’ve helped countless patients find relief through advanced nerve ablation procedure for back pain techniques, allowing them to return to activities they love without relying on long-term medications.
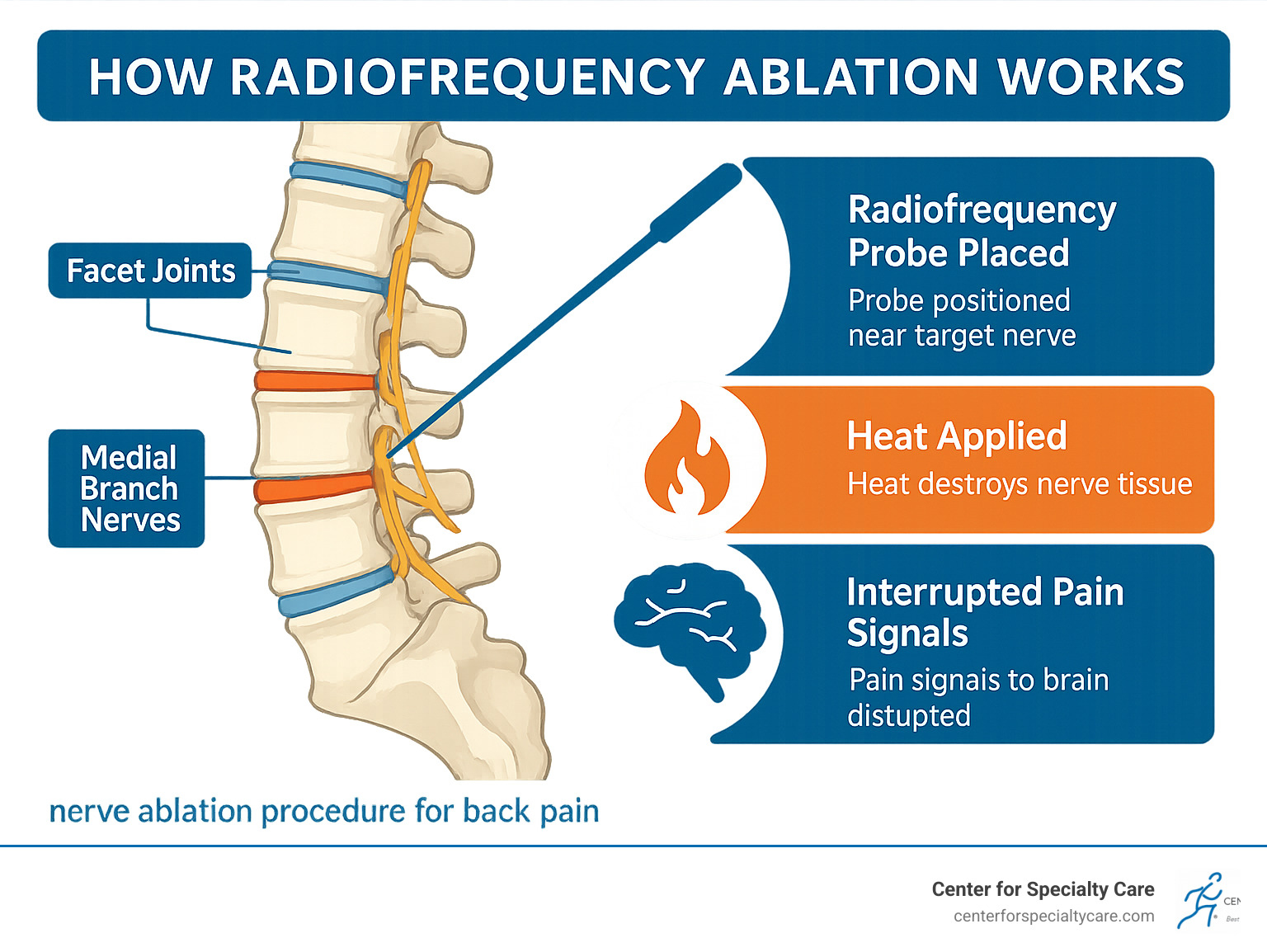
Understanding Nerve Ablation: Who It Helps and How It Works
When traditional treatments haven’t provided adequate relief, the nerve ablation procedure for back pain can be a powerful solution. Also known as radiofrequency neurotomy, this minimally invasive treatment uses precise heat energy to interrupt pain signals at their source, rather than just masking symptoms with medication.
By targeting only the specific nerves responsible for your pain, this procedure can provide significant relief, help you reduce your dependence on pain medications, and maintain normal function. Our Comprehensive Guide to Pain Management explores how this fits into your overall treatment plan, and scientific research on facet joint pain continues to validate its effectiveness.
What Types of Back Pain Can Be Treated?
Nerve ablation is highly effective for pain originating from specific spinal structures.
- Facet joint arthritis (spondylosis): This is a common cause of pain and stiffness from wear and tear on the small joints along your spine. Ablation targets the medial branch nerves that carry pain signals from these joints.
- Sacroiliac (SI) joint pain: When the joints connecting your pelvis and spine become inflamed, it can cause pain in the lower back, buttocks, and legs. Nerve ablation targets the lateral branch nerves that supply these joints.
- Vertebrogenic pain: This newly understood condition involves damage to the vertebral endplates. Ablation of the basivertebral nerve can treat this deep, aching pain that is often resistant to other methods.
- Chronic low back and neck pain: The procedure is an excellent option for pain that has persisted for months or years without relief from conservative treatments, as long as the pain source can be identified and targeted.
To better understand your diagnosis, explore our guide on Common Spinal Conditions: Causes, Symptoms, and Treatment Options.
Are You a Good Candidate for Nerve Ablation?
Determining if you are a good candidate involves a careful evaluation. The ideal candidate typically has:
- Chronic pain lasting at least six months.
- Inadequate relief from conservative treatments like physical therapy, medications, or steroid injections.
- A positive response to a diagnostic nerve block. This “test” injection of numbing medication confirms the source of your pain and predicts the success of the ablation procedure.
Nerve ablation may not be suitable if you have an active infection, are pregnant, or have unmanaged bleeding disorders. Our team performs a thorough evaluation to ensure every patient has the best possible chance of success.
How Effective Is It and How Long Does Relief Last?
The results of nerve ablation are often life-changing. Many patients experience at least a 50% reduction in pain, with some achieving even greater relief.
Pain relief typically lasts 6 to 18 months, though some patients enjoy benefits for up to two years. The duration depends on your specific condition and how your body responds. Because nerves can regenerate over time, the pain may gradually return. However, a key benefit of this treatment is that the procedure can be safely repeated, providing a long-term strategy for managing chronic pain.
Many patients find they can return to activities they had given up, reduce their pain medication, and enjoy a better quality of life. For certain conditions like vertebrogenic pain, some studies show lasting benefits for five years or more.
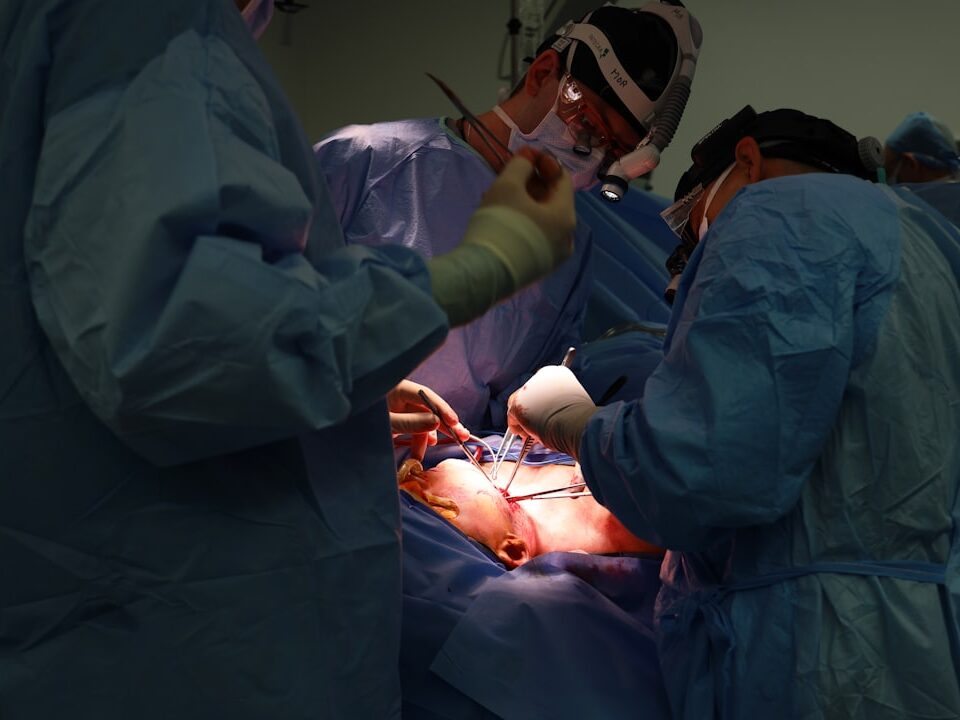
The Nerve Ablation Procedure for Back Pain: A Step-by-Step Guide
Knowing what to expect can ease any concerns about an upcoming medical procedure. The nerve ablation procedure for back pain is a routine, minimally invasive treatment performed in our outpatient facility, allowing you to return home the same day.
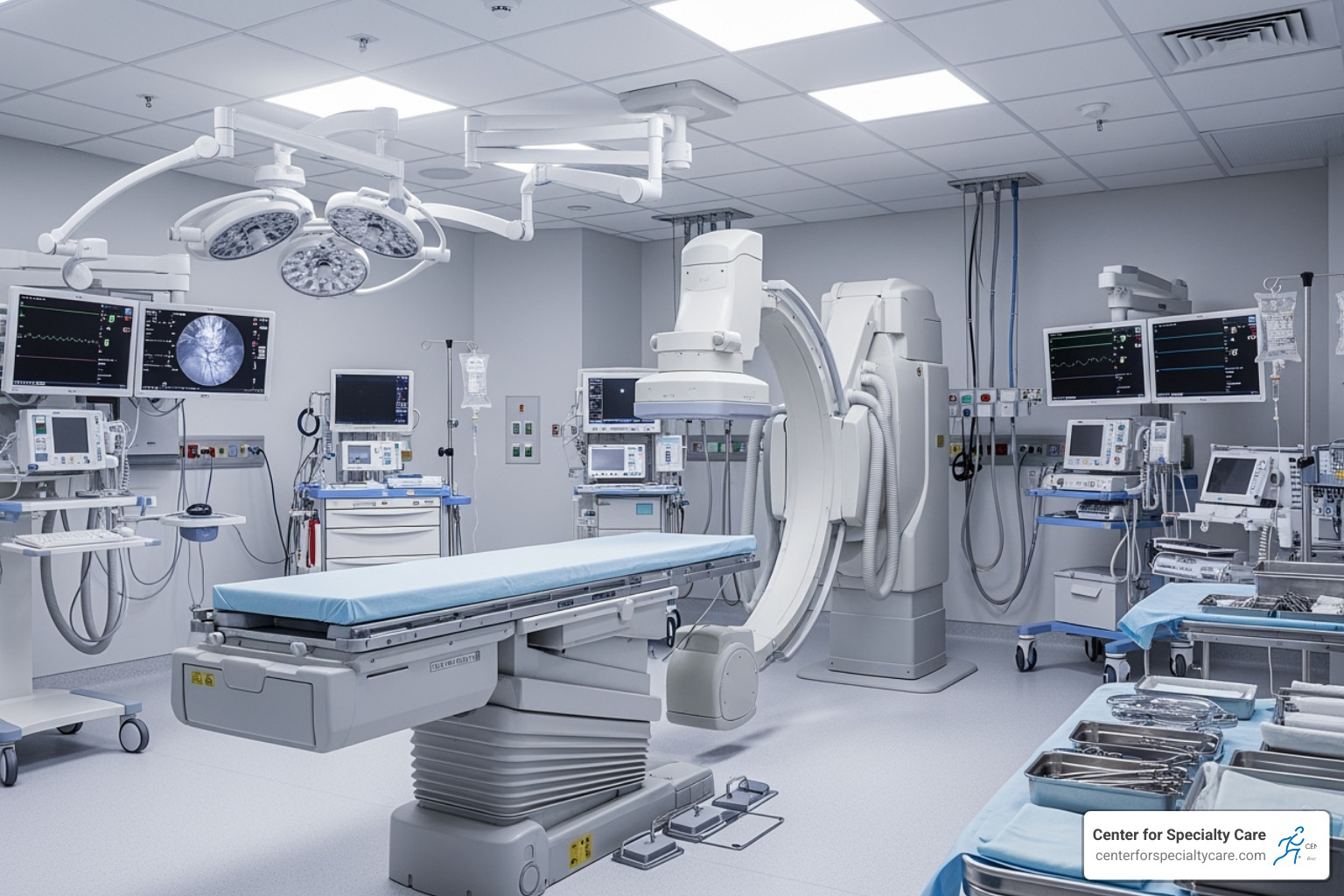
Our team at Center for Specialty Care has extensive experience performing these procedures, ensuring your treatment is as comfortable and stress-free as possible. We tailor the treatment to target the precise source of your pain, whether it affects your Back Spine or other areas.
Preparation for the Procedure
Proper preparation ensures your procedure goes smoothly. This process begins with your initial consultation and the diagnostic nerve blocks that confirm nerve ablation is the right choice for you.
- Medication Adjustments: If you take blood-thinning medications (e.g., aspirin, warfarin) or certain supplements, we will provide specific instructions on when to pause them.
- Transportation: You must arrange for someone to drive you home, as the mild sedation used for comfort will prevent you from driving safely.
- Fasting: You will be asked to avoid eating or drinking for 6-8 hours before your procedure. We will provide clear instructions for any essential medications.
During the Procedure: What to Expect
On the day of your procedure, our team will ensure you are comfortable and well-cared for.
- Positioning and Anesthesia: You will lie on an X-ray table, and we will numb the skin at the treatment site with a local anesthetic.
- Sedation: Mild sedation is often used to help you relax. You will remain awake and able to communicate with our team.
- Guidance and Placement: We use fluoroscopy (real-time X-ray) to precisely guide a thin needle to the target nerve.
- Confirmation: A nerve stimulation test, which may cause a slight tingling or muscle twitch, confirms the needle is in the correct position.
- Ablation: A radiofrequency current is applied for 60-90 seconds, creating a small heat lesion on the nerve to block pain signals.
The entire nerve ablation procedure for back pain typically takes 30-90 minutes, depending on the number of nerves being treated.
Recovery and Post-Procedure Care
After a brief observation period in our recovery area, you will be ready to go home.

- Initial Soreness: It is normal to experience some soreness at the injection site, similar to a mild sunburn, for a few days. Ice packs applied for 15-20 minutes at a time can help reduce discomfort.
- Activity: Rest for the first 24 hours, then gradually return to your normal activities as you feel comfortable. Avoid strenuous activity for a few days. Warm showers are fine after 24 hours, but avoid baths for a couple of days.
- Physical Therapy: We may recommend physical therapy to help strengthen your back muscles and maximize the procedure’s benefits. Our guide on Managing Radiating Pain: Tips for Relief offers additional strategies.
While some patients feel immediate relief, the full benefits typically develop over 1-3 weeks as the nerves quiet down. Be patient with the healing process, as significant improvement continues for several weeks.
Types of Nerve Ablation and Advanced Options
Not all back pain is the same, which is why we offer different types of the nerve ablation procedure for back pain, each targeting a specific pain source. The most common method is Radiofrequency Ablation (RFA), but for certain conditions, we offer the innovative Basivertebral Nerve (BVN) Ablation, known as the Intracept® procedure. Both are key components of our Pain Management services.
Here’s how these two approaches compare:
| Feature | Radiofrequency Ablation (RFA) | Basivertebral Nerve (BVN) Ablation (Intracept® Procedure) |
|---|---|---|
| Target Nerves | Medial Branch Nerves (Facet Joints), Lateral Branch Nerves (SI Joints) | Basivertebral Nerve (within vertebral bodies) |
| Conditions Treated | Facet joint arthritis, Sacroiliac (SI) joint pain, Neck pain | Vertebrogenic pain (from vertebral endplate damage) |
| Diagnostic Criteria | Positive diagnostic nerve block (medial or lateral branch) | MRI showing Modic Type 1 or Type 2 changes |
| Location of Action | Outside the spinal canal, near the facet/SI joints | Inside the vertebral body (intraosseous) |
| Mechanism | Heat lesion on nerve to block signals | Heat lesion on basivertebral nerve to block signals |
Choosing the right procedure depends on the origin of your pain and diagnostic test results.
Radiofrequency Ablation (RFA) for Facet and SI Joint Pain
RFA is a proven solution for pain from facet joint arthritis or sacroiliac joint dysfunction. This nerve ablation procedure for back pain targets the specific nerves responsible for transmitting pain signals from these joints.
- For facet joint pain, we treat the medial branch nerves. These nerves only sense pain from the joints and do not control muscles or skin sensation.
- For sacroiliac joint pain, we target the lateral branch nerves that supply the joints connecting your pelvis and lower spine.
The precision of RFA is confirmed with a diagnostic nerve block before the procedure. If numbing the nerve temporarily relieves your pain, we know we have identified the correct target. RFA is a distinct treatment but can be part of a comprehensive plan that might also include options like Epidural Steroid Injections. For more technical details, see this overview of ablative nerve blocks.
Basivertebral Nerve (BVN) Ablation: The Intracept® Procedure
The Intracept® procedure is a groundbreaking treatment for vertebrogenic pain, a type of chronic lower back pain originating from within the vertebrae themselves.
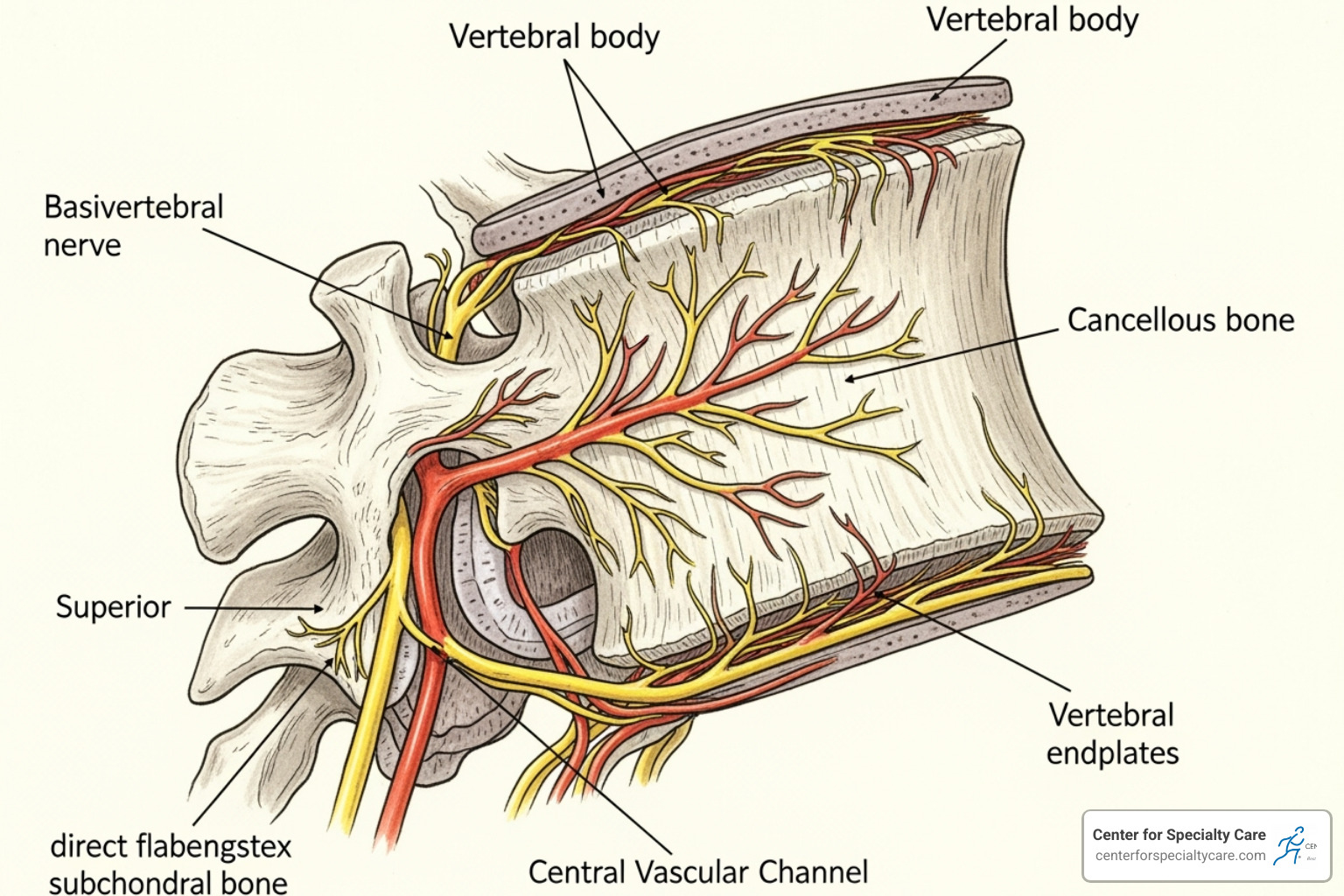
The basivertebral nerve is located inside the vertebral bones and sends pain signals from damaged vertebral endplates (the area between your vertebrae and discs). The Intracept procedure is like a “root canal for your spine,” as it treats the pain at its source from within the bone. During this procedure, we use radiofrequency energy to ablate the basivertebral nerve, stopping the pain signals and providing long-lasting relief.
What are ‘Modic Changes’ and How Do They Relate to BVN Ablation?
Modic changes are specific findings on an MRI scan that identify you as a good candidate for the Intracept procedure. They indicate damage to the bone marrow near the vertebral endplates.
- Modic Type 1 changes show active inflammation and often cause more severe pain.
- Modic Type 2 changes show that bone marrow has been replaced by fat, indicating chronic degeneration.
Research shows that up to 43% of patients with chronic lower back pain have this type of endplate damage. Identifying Modic changes on your MRI confirms a vertebrogenic source of pain, giving us confidence that the Intracept procedure will be effective. Our guide on Spinal Anatomy offers more insight into how these structures work together.
Frequently Asked Questions about Nerve Ablation
It’s natural to have questions when considering a medical procedure. We believe clear, honest answers make all the difference. Here are our responses to the most common questions about the nerve ablation procedure for back pain.
What are the risks and benefits of the nerve ablation procedure for back pain?
Like any medical procedure, nerve ablation has both benefits and risks, which we will discuss with you thoroughly.
The benefits are often life-changing. Most patients experience significant pain relief, improved function, and a reduced need for pain medication. Because the procedure is minimally invasive, you can go home the same day and return to light activities quickly, allowing you to get back to the life you enjoy.
The risks are generally minimal. The most common side effects are temporary soreness or numbness at the injection site. There is a small risk of infection or minor bleeding. Serious complications are extremely rare, occurring in less than 0.3% of cases according to clinical trials, making this a very safe procedure.
How is the nerve ablation procedure for back pain different from spine surgery?
This is a key distinction. Nerve ablation is fundamentally different from major spine surgery.
- It is non-surgical: Spine surgery involves incisions, moving muscle, and often placing hardware like screws or rods. Nerve ablation uses only a small needle guided by X-ray, preserving your spine’s natural structure.
- Recovery is faster: Spine surgery can require a hospital stay and months of rehabilitation. Nerve ablation patients go home the same day and typically resume normal activities within days to weeks.
- It preserves future options: Because nerve ablation does not permanently alter your spine’s anatomy, it keeps future treatment options open in a way that major surgery might not.
Think of it as fixing a faulty electrical circuit instead of renovating the entire house. You can learn more about the contrast by reading about surgical options like laminectomy procedures.
Will my nerve grow back after the procedure?
Yes, the treated nerves will eventually regenerate. This is a natural process and part of what makes nerve ablation a practical, long-term pain management strategy.
Nerve regeneration typically occurs over 6 to 18 months. When the nerve grows back, the pain may return. This does not mean the procedure failed; it means you’ve enjoyed a long period of relief that allowed you to live more fully and perhaps strengthen your body with physical therapy.
Because the nerve grows back, the procedure can be safely repeated. Many of our patients find that periodic nerve ablation treatments allow them to maintain an active, fulfilling life without relying on daily medications or considering more invasive surgery.
Take the Next Step Towards a Pain-Free Life
Living with chronic back pain doesn’t have to be your reality. If persistent discomfort is limiting your life, the nerve ablation procedure for back pain could be the turning point you’ve been searching for. This minimally invasive treatment offers lasting relief by targeting pain at its source, allowing many of our patients to return to the hobbies and activities they love.
At Center for Specialty Care, we provide personalized care custom to your unique condition and goals. We offer advanced options like the Intracept® procedure for vertebrogenic pain, a treatment for patients with specific MRI findings. You can Learn more about the Intracept® Procedure to see if it’s right for you.
We are proud of our commitment to 100% patient satisfaction and quick appointment availability. With convenient locations in Fairmont, MN, Estherville, IA, Buffalo Center, IA, and St. James, MN, our experienced team is ready to help you regain mobility and reclaim your life.
Don’t let another day go by in pain. Reach out to explore your options and take the first step toward relief.