
Understanding and Treating Flat Feet: A Complete Guide
January 19, 2026
The Ultimate Guide to Foam Rolling Away Shoulder Blade Pain
January 22, 2026What is Pain Management: 1 Proven Path to Relief
Pain Is Your Body’s Warning System—But You Don’t Have to Suffer Through It
What is pain management? It is a medical approach that helps you regulate pain through medications, procedures, exercises, and therapy. Specialists use one or a combination of methods to prevent, reduce, or relieve pain, with the goal of improving your quality of life and restoring daily function.
Quick Answer:
- Purpose: Evaluate, diagnose, and treat different types of pain
- Approach: Often uses a multidisciplinary team (doctors, physical therapists, psychologists)
- Methods: Medications, physical therapy, injections, behavioral therapy, lifestyle changes
- Goal: Reduce pain, improve function, improve quality of life—not always total elimination
Pain is your body’s alarm system, but when it becomes chronic—persisting for months or years—it can take over your life, affecting your body, mood, and relationships. Over 50 million U.S. adults reported chronic pain in 2021, making it a major public health challenge. The good news is that with today’s treatments, you don’t have to tolerate severe pain. Effective pain management can help you heal faster, sleep better, and return to the activities you love.
This guide will walk you through what pain management truly means, from understanding your pain to exploring treatment options and taking an active role in your recovery.
As Dr. Corey Welchlin, a board-certified orthopedic surgeon with over three decades of experience treating musculoskeletal pain in southern Minnesota and northern Iowa, I’ve seen how understanding what is pain management can transform a patient’s journey. My team at the Center for Specialty Care is dedicated to providing comprehensive, personalized pain relief through both surgical and non-surgical approaches.
What is Pain Management and Why is it Important?
What is pain management? It’s a specialized area of medicine focused on helping you live better despite pain. It goes beyond a simple prescription, digging into the cause of your discomfort to build a personalized strategy. This strategy addresses the physical sensation and its impact on your sleep, mood, and daily life.
According to CDC guidelines for pain management, the most effective approach is multidisciplinary, bringing together multiple specialists and treatment methods. With today’s advanced therapies, there’s no reason to tolerate severe, uncontrolled pain. Effective management helps you heal faster and get back to your normal activities sooner.
Defining the Goals of Treatment
Pain management doesn’t always mean pain elimination. For many chronic conditions, the goal is to reduce pain to a manageable level where it no longer controls your life. Successful treatment aims to:
- Reduce pain intensity so you can function comfortably.
- Improve physical abilities like walking, bending, and lifting.
- Restore restful sleep.
- Boost emotional well-being by reducing the anxiety and depression linked to chronic pain.
- Decrease reliance on medication, especially opioids, by finding a balance that provides relief without unnecessary risks.
- Help you return to normal activities, whether it’s a hobby, work, or time with family.
The Multidisciplinary Team Approach
Managing chronic pain is a team effort. A coordinated team ensures you get comprehensive treatment custom to your needs. Your team may include:
- Pain Management Specialist: A physician with fellowship training who leads your team and develops the overall strategy.
- Neurologists: Experts on the nervous system, crucial for nerve-related pain.
- Anesthesiologists: Specialists who often perform interventional procedures like nerve blocks.
- Physical Therapists: Hands-on experts who design exercise programs to rebuild strength and mobility. You can learn more on our Physical Therapy page.
- Psychologists and Counselors: Professionals who help you develop coping strategies to manage the emotional toll of chronic pain.
At Center for Specialty Care, we offer this multidisciplinary approach in Fairmont, Estherville, Buffalo Center, and St. James. Our team includes orthopedic specialists for musculoskeletal pain and rheumatology specialists for autoimmune and inflammatory conditions. Our Rheumatology services provide another layer of specialized care. This team approach means you’re never navigating pain alone.
Decoding Your Pain: Acute vs. Chronic and Other Types
Not all pain is the same. Understanding the type of pain you’re experiencing is essential to finding the right treatment. Pain specialists classify pain by its duration (acute vs. chronic), its cause (nociceptive, neuropathic, or inflammatory), and its origin to create a custom treatment plan.
The Critical Difference: Acute vs. Chronic Pain
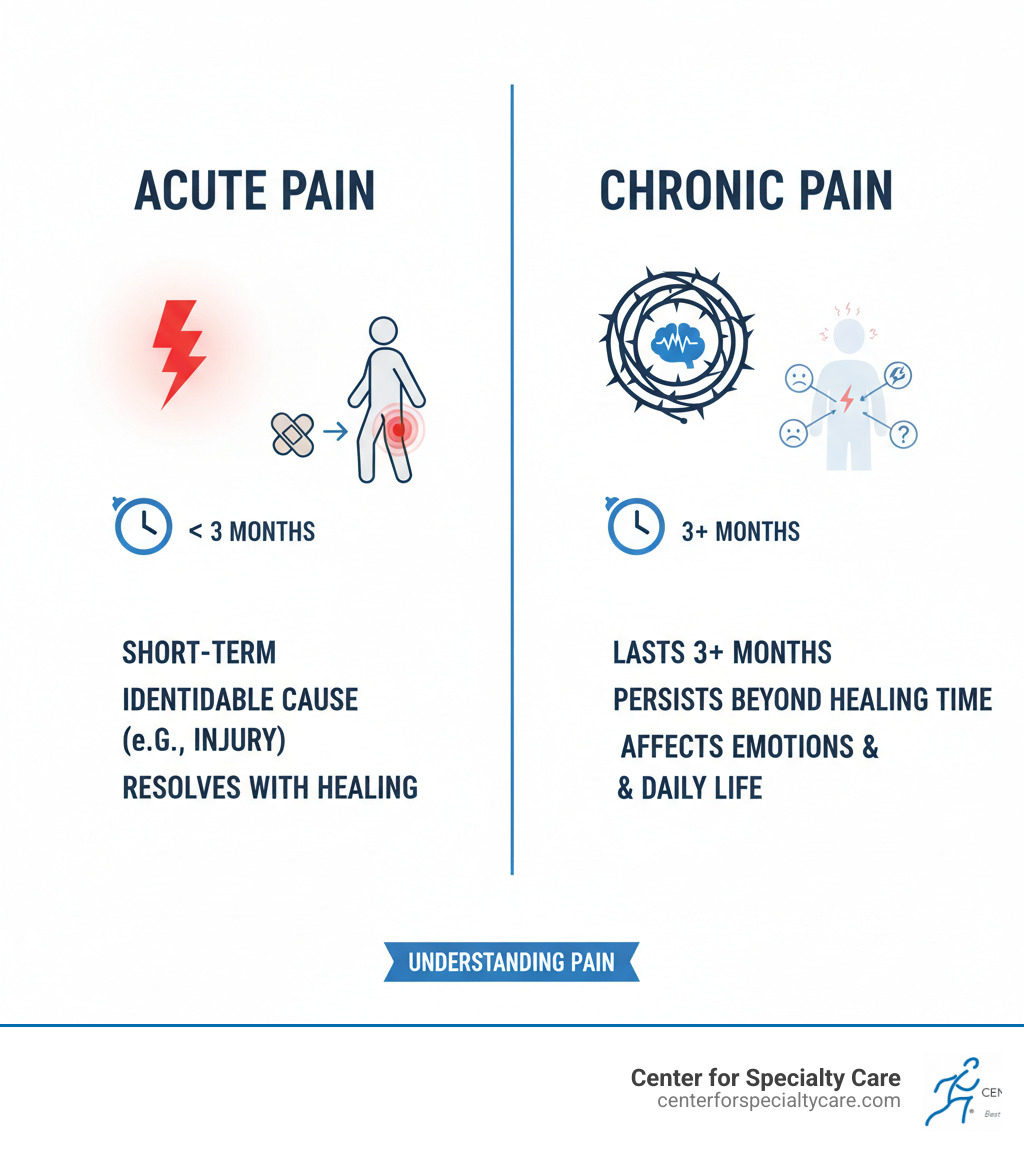
The most important distinction in pain management is between acute and chronic pain.
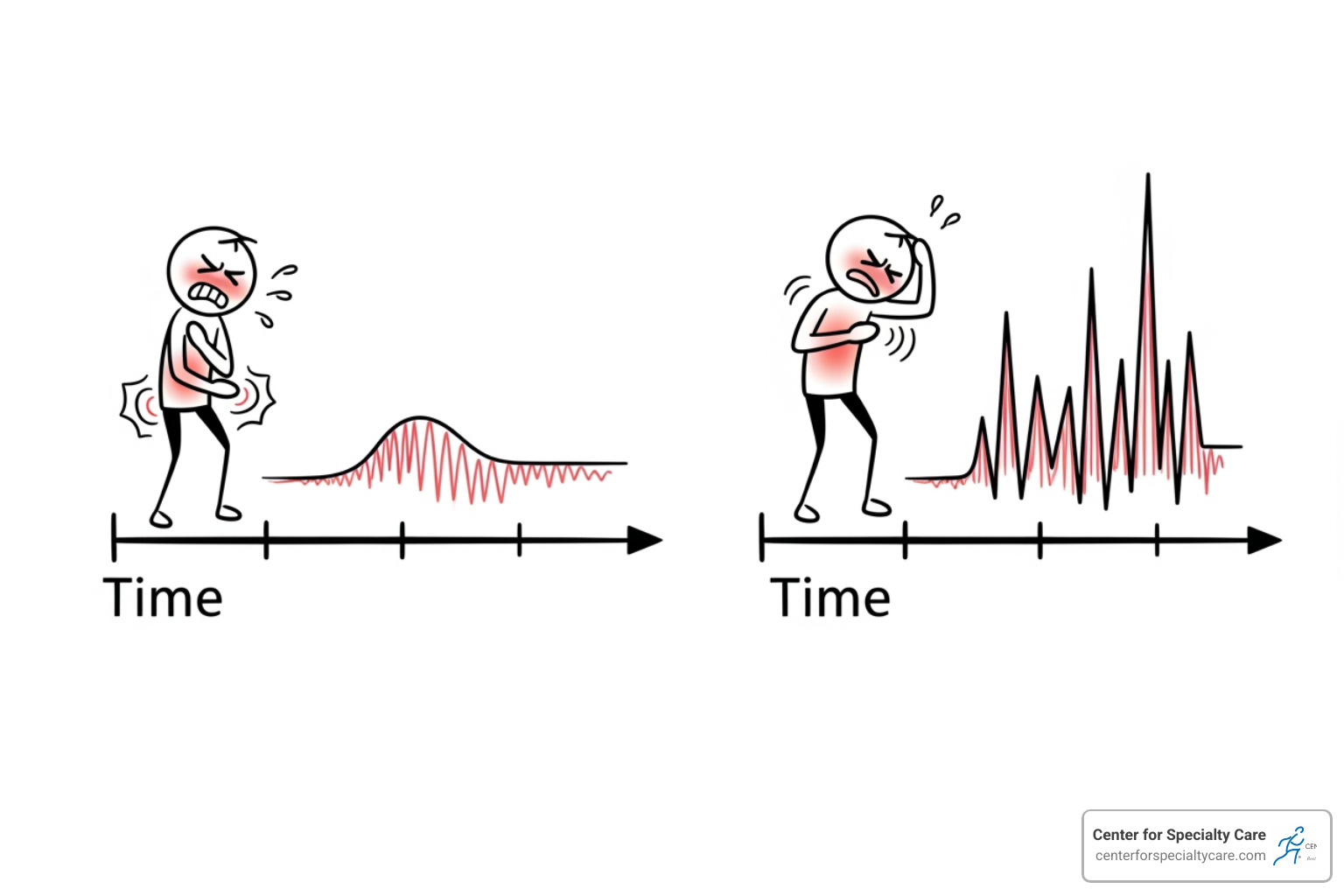
Acute pain is your body’s alarm system. It starts suddenly from a clear cause, like an injury or surgery. It’s a helpful warning signal that resolves as your body heals, typically within days or weeks.
Chronic pain is an alarm that won’t turn off. It’s pain that lasts for more than three months, persisting long after an initial injury has healed, or sometimes with no clear cause at all. It can develop from conditions like arthritis or nerve damage. Unlike acute pain, chronic pain becomes a problem in itself, disrupting sleep, energy, mood, and daily life.
| Characteristic | Acute Pain | Chronic Pain |
|---|---|---|
| Duration | Short-term (days to weeks) | Long-term (months to years) |
| Onset | Sudden, usually clearly defined | Gradual or sudden, persists beyond healing |
| Cause | Identifiable injury, illness, surgery | Ongoing condition, nerve damage, or unknown |
| Purpose | Warning signal, protective | Can be debilitating, no longer protective |
| Impact | Localized, temporary | Widespread, affects emotions, sleep, daily life |
What is pain management for specific conditions?
At Center for Specialty Care, we treat many types of pain, understanding that each patient’s experience is unique. Here are some common conditions we manage:
- Back pain: One of the most common causes of disability, stemming from muscle strains, herniated discs, or spinal stenosis. For pain that shoots down your leg, see our guide on Managing Radiating Pain: Tips for Relief. If you’re unsure about the severity, learn when to seek urgent care for back pain.
- Coccydynia (tailbone pain): This pain can make sitting and other daily activities challenging. We identify the cause, whether from a fall or repetitive strain, to create a targeted plan.
- Ankle impingement: Common in active individuals, this occurs when tissue or bone gets pinched in the ankle joint. Early treatment can prevent it from becoming a chronic issue.
- Post-surgical pain: While expected, this pain should be manageable to allow for proper healing and participation in physical therapy. Effective management helps you recover faster.
- Arthritis pain: A long-term challenge from osteoarthritis or autoimmune conditions like rheumatoid arthritis. Our Rheumatology team specializes in managing these conditions to maintain your quality of life.
- Fibromyalgia: This complex condition involves widespread pain, fatigue, and mood changes, requiring a comprehensive, multidisciplinary approach.
A Comprehensive Toolkit for Treating Pain
What is pain management if not a full toolbox of solutions? Your pain is unique, so we create personalized treatment plans that may blend several therapies for the best possible outcome.
Pharmacological (Medication-Based) Treatments
Medications are a valuable tool, often chosen based on the WHO’s “pain ladder” approach, starting with gentler options.
- Over-the-Counter (OTC) Relievers: For mild to moderate pain, we often start with NSAIDs (ibuprofen, naproxen) to reduce pain and inflammation, or acetaminophen (Tylenol) for pain and fever.
- Prescription Medications: When OTCs aren’t enough, we may consider other options. Certain antidepressants and anticonvulsants (like gabapentin) are highly effective for chronic nerve pain. Muscle relaxants can help when spasms are a factor. Opioids are powerful but carry risks of dependence, so we reserve them for severe, acute pain or specific chronic cases where other treatments have failed. The CDC recommends physical therapy and exercise as first-line treatments over opioids for many types of chronic pain, an approach we fully support. You can learn more about our non-surgical orthopedics and pain management.
Non-Pharmacological and Interventional Approaches
Often, the most powerful relief doesn’t come from a bottle. These techniques are central to modern pain management.
- Physical Therapy: One of our most effective tools. Therapists use targeted exercises and hands-on techniques to reduce pain and improve body mechanics. Learn more about our Physical Therapy services.
- Exercise: Appropriate movement strengthens muscles, improves circulation, and releases natural pain-relieving endorphins.
- Injections and Nerve Blocks: For targeted relief, we can inject anesthetic and steroids near specific nerves. An Epidural Steroid Injection can provide significant relief for radiating back and leg pain.
- Spinal Cord Stimulation (SCS): An implanted device sends mild electrical pulses to the spinal cord, changing how the brain perceives pain signals.
- Other Therapies: We also use massage therapy to ease tense muscles, acupuncture to stimulate natural healing, heat and cold therapy for simple relief, and TENS units that use gentle electrical currents to block pain signals.
- Psychological Therapies: The mind is a powerful tool. Cognitive Behavioral Therapy (CBT) helps change negative thought patterns, while mindfulness and relaxation techniques calm the nervous system and reduce pain perception.
What are the risks and side effects?
We believe in honest conversations about treatment. NSAIDs can cause stomach and kidney issues with long-term use. Acetaminophen can harm the liver if taken in excess. Opioids carry significant risks of drowsiness, constipation, and addiction, as documented in studies on “Opioid prescriptions for chronic pain and overdose”. Interventional procedures have small risks of infection, bleeding, or nerve damage. We will always discuss the risks and benefits with you to create the safest, most effective plan.
Working with a Pain Management Specialist
When pain is persistent, a pain management specialist is your expert guide. These are physicians with years of additional fellowship training dedicated to evaluating, diagnosing, and treating complex pain.
What is a pain management specialist and what do they do?
A pain management specialist acts as a detective, uncovering not just where your pain is, but why it’s happening. They take a comprehensive approach, starting with a thorough evaluation, including your medical history, a physical exam, and a review of any diagnostic tests. Based on their findings, they create a personalized treatment plan that might include medications, physical therapy, lifestyle changes, or advanced interventional procedures like nerve blocks or spinal cord stimulation.
Crucially, your specialist acts as the central coordinator of your care team, working with your other doctors and therapists. At Center for Specialty Care, we accept this philosophy, integrating our orthopedic expertise with our Non-Surgical Orthopedics and Pain Management services.
Your First Visit: What to Expect
Your first visit at our clinics in Fairmont, Estherville, Buffalo Center, or St. James is a comprehensive conversation. To make the most of it, you should be prepared to:
- Discuss your medical history: Be ready to talk about when the pain started, what it feels like, and what treatments you’ve tried.
- Undergo a physical exam: We’ll assess your movement, posture, reflexes, and areas of tenderness.
- Describe your pain: Use the 1-10 pain scale, but also use descriptive words (sharp, dull, burning, throbbing). Explain what makes it better or worse.
- Set realistic goals: We’ll work with you to define what success looks like, whether it’s sleeping through the night or returning to a favorite hobby.
- Bring previous records: If you have prior imaging (X-rays, MRIs) or test results, bring them with you. You may also be asked to complete an INTAKE QUESTIONNAIRE beforehand.
How to Find and Choose the Right Specialist
Choosing the right specialist is a critical step. Here’s what to look for:
- Start with a referral: Your primary care doctor knows your history and can recommend a trusted specialist.
- Check for board certification: This credential ensures the physician has met rigorous standards in pain management. Dr. Corey Welchlin at Center for Specialty Care brings over three decades of board-certified orthopedic experience.
- Look for a multidisciplinary approach: The best specialists integrate various therapies, not just prescriptions. Our team of providers works collaboratively to create a comprehensive plan.
- Trust your instincts on communication: You need a partner who listens, explains things clearly, and involves you in decisions. Good communication is the foundation of effective care.
Empowering Yourself on Your Pain Journey
You are the most powerful person on your pain management team. Patients who take an active role in their care consistently achieve better outcomes. This means building self-management strategies, communicating effectively, and creating a strong support system.
How to Effectively Communicate Your Pain to Your Doctor
Clear communication is vital. We can’t read your mind, so we rely on your descriptions to guide treatment. Here’s how to help us understand:
- Use the 0-10 pain scale: This helps us track your progress over time.
- Use descriptive words: Is the pain sharp, dull, aching, burning, or tingling? Does it radiate?
- Keep a pain diary: Note when pain flares up, its severity, and what you were doing. This can reveal important patterns.
- Be specific: Tell us what makes your pain better or worse (e.g., movement, rest, heat, ice, specific positions).
The CDC offers more guidance on Working Together With Your Doctor to Manage Your Pain. We are on the same team, working toward the same goal.
When Should You Call a Doctor About Your Pain?
We would rather hear from you too soon than too late. Call us if you experience:
- Sudden, severe, or unexplained pain.
- Pain accompanied by fever, chills, or other concerning symptoms.
- New or spreading numbness, tingling, or weakness.
- Pain that is getting worse or not improving with your current treatment.
- Side effects from medication, such as persistent stomach pain or severe constipation.
- Pain that consistently disrupts your sleep.
- Feelings of anxiety, depression, or being overwhelmed by your pain.
How Can Family and Friends Support Someone with Pain?
Chronic pain can be incredibly isolating. If your loved one is in pain, your support is crucial. Here’s how you can help:
- Listen with empathy. Believe them when they say they’re hurting. Validate their experience without trying to “fix” it.
- Offer practical help. Be specific: “Can I pick up groceries for you on Thursday?” is more helpful than a vague offer.
- Gently encourage them. Be a supportive partner in their treatment plan, perhaps by exercising with them or reminding them of appointments.
- Adapt activities. Suggest things you can do together that accommodate their limitations, like a short walk or a movie night at home.
- Educate yourself. Learning about their condition will help you respond with greater compassion.
Conclusion
Pain is a complex experience, but you don’t have to live with it unmanaged. As we’ve explored what is pain management, the answer is clear: it’s a comprehensive, personalized approach that combines medical expertise with your active participation to help you reclaim your life.
The goal is to reduce pain to manageable levels, improve your daily function, and restore your quality of life. Whether you’re dealing with back pain, arthritis, or post-surgical discomfort, proven strategies can help.
At Center for Specialty Care, our team serving Fairmont, Estherville, Buffalo Center, and St. James is dedicated to providing this kind of compassionate, comprehensive care. We listen first, diagnose thoroughly, and partner with you every step of the way. Our commitment to 100% patient satisfaction means we’re here to support you with personalized plans and quick appointment availability.
Your journey toward better pain management starts with a conversation. To learn more about our solutions, visit our Non-Surgical Orthopedics and Pain Management page. Let’s work together to move you beyond the ache and back to the life you love.





