Heat Therapy: Your Guide to a Healthier, Happier You
January 16, 2026
Beyond the Ache: Unpacking What Pain Management Truly Means
January 20, 2026Flat Feet Treatment: Expert Relief 2025
Why Flat Feet Treatment Matters for Your Overall Health
Flat feet treatment aims to relieve pain, improve foot function, and prevent complications in your ankles, knees, hips, and back. Options range from conservative measures like arch supports and stretching to physical therapy and, in rare cases, surgery.
Having flat feet—where the foot’s arch collapses—is common, affecting up to 23% of adults. While many people experience no issues, others suffer from chronic pain in the arch, heel, or ankle. This misalignment can create a domino effect, causing strain in the knees, hips, and lower back. You might also feel fatigued after walking, struggle with balance, or notice uneven shoe wear.
The good news is that most cases of painful flat feet respond well to non-surgical treatment. A combination of exercises, supportive devices, and lifestyle changes can bring significant relief and improved mobility.
I’m Dr. Corey Welchlin, an orthopedic surgeon with over 30 years of experience at the Center for Specialty Care in Fairmont, Minnesota. I specialize in diagnosing and treating foot and ankle conditions, including flat feet treatment. My approach is conservative-first, helping countless patients restore function and eliminate pain while reserving surgery only for the most severe cases.

Understanding Flat Feet: Causes, Types, and Symptoms
Flat feet, or pes planus, occur when the arches flatten, allowing the entire sole to touch the ground. Understanding the cause, type, and symptoms is the first step toward finding the right flat feet treatment.
What Causes Flat Feet?
The reasons for flat feet vary, from genetics to gradual wear and tear.
- Genetics: Many people inherit flat feet from their parents.
- Childhood Development: All babies have flat feet, with arches typically forming by age six. For some, the arches never fully develop. About two in ten children carry flat feet into adulthood.
- Adult-Acquired Flatfoot: This often involves posterior tibial tendon dysfunction (PTTD). The posterior tibial tendon supports the arch, and when it becomes inflamed or torn from overuse, injury, or aging, the arch can collapse. Untreated PTTD can lead to chronic pain.
- Injury: A broken bone, torn ligament, or damaged tendon in the foot or ankle can compromise the arch’s structure.
- Aging: Over time, tendons and ligaments naturally weaken and stretch, which can contribute to arch collapse.
Several risk factors increase your likelihood of developing flat feet:
- Obesity: Extra weight puts significant stress on your arches.
- Diabetes: This condition can affect nerve function and circulation, increasing the risk of foot problems, including Charcot Foot, a severe deformity.
- Pregnancy: Hormonal changes loosen ligaments, and the added weight can cause arches to flatten temporarily or permanently.
- Rheumatoid Arthritis: This autoimmune disease can attack foot joints, leading to inflammation and arch collapse.
(For more on tendon issues, see our guide on Achilles Tendonitis 101: Orthopedic Insights for Managing and Preventing Tendon Pain.)
Types of Flat Feet
Identifying the type of flat foot helps create an effective flat feet treatment plan.
- Flexible Flatfoot: The most common type. An arch is visible when sitting but disappears when standing. It’s often painless but can become uncomfortable over time.
- Rigid Flatfoot: The arch remains flat whether you’re standing or not. This usually signals an underlying structural issue, like fused bones (tarsal coalition) or severe arthritis, and is often more difficult to treat conservatively.
- Adult-Acquired Flatfoot: Also called a fallen arch, this type develops over time, usually due to PTTD. It often starts in one foot and responds well to early intervention.
- Vertical Talus: A rare birth defect where the talus bone is misaligned, creating a “rocker-bottom” foot and preventing an arch from forming.
Common Symptoms
While many people with flat feet have no symptoms, others experience issues that impact daily life.

- Foot Pain: The most common complaint is an ache or sharp pain in the arches, heels, or along the inside of the ankle, often worsening with activity.
- Leg Cramps and Swelling: Muscles in the lower legs may cramp from overworking, and swelling can appear around the ankles and arches.
- Difficulty Standing on Toes: Weakened arch-supporting muscles can make this movement challenging.
- Gait Changes: You may notice an awkward walking pattern or excessive inward rolling of the foot (pronation), affecting balance.
- Pain in Knees, Hips, or Lower Back: This is a result of the kinetic chain. Misalignment in the feet creates a ripple effect up the body, potentially leading to bunions, hammertoes, shin splints, and arthritis in various joints.
Understanding your symptoms is the first step toward relief. With a proper diagnosis, most people with painful flat feet can return to an active life.
How a Podiatrist Diagnoses Flat Feet
An accurate diagnosis is the foundation for an effective flat feet treatment plan. At Center for Specialty Care in Fairmont, Minnesota, we conduct a thorough evaluation to understand what is happening with your feet and why.
Physical Examination
Your appointment begins with a comprehensive physical exam to assess both structure and function.
- Visual Inspection: We’ll observe your feet while you stand and sit to check for an arch, look for swelling, and see if your heel tilts inward. This helps determine if you have flexible or rigid flat feet.
- Standing on Toes Test: We’ll ask you to rise onto your tiptoes. If an arch forms, it typically indicates flexible flatfoot. Difficulty with this movement can also signal weakness.
- Shoe Wear Pattern: Bring the shoes you wear most often. The wear patterns on the soles reveal how your feet strike the ground. Excessive wear on the inside edge is a classic sign of overpronation common with flat feet.
- Muscle Strength and Range of Motion: We’ll test the strength of key muscles like the posterior tibial tendon and assess the flexibility of your joints to identify stiffness or looseness contributing to the problem.
- Gait Analysis: We will watch you walk to see how flat feet affect your entire body’s alignment.
For additional information on diagnosis, the Mayo Clinic offers helpful resources.
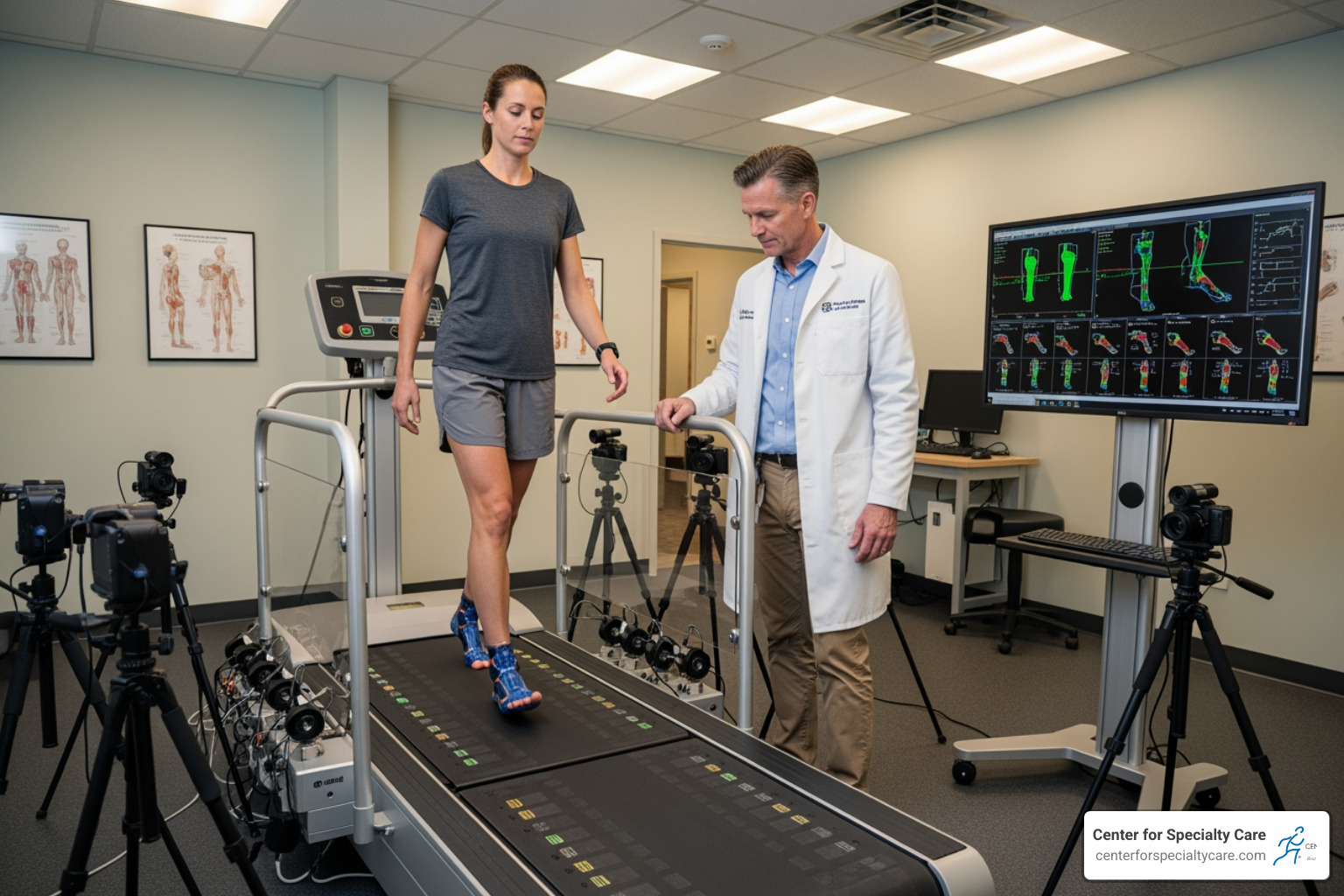
Diagnostic Imaging and Appointment Preparation
If the physical exam isn’t conclusive or you have significant pain, we may use imaging tests for a clearer picture.
- X-rays: Show bone structure and alignment, helping us measure arch collapse and identify arthritis.
- Ultrasound: Uses sound waves to create real-time images of soft tissues, ideal for evaluating tendon tears or inflammation.
- CT Scans: Provide detailed 3D views of bones, which is crucial for surgical planning.
- MRI Scans: Offer comprehensive views of both bone and soft tissues to detect ligament, cartilage, or subtle tendon injuries.
To prepare for your appointment, please bring your everyday shoes. Be ready to discuss your medical history, when the pain started, what makes it better or worse, and any home remedies you’ve tried. Sharing this information helps us tailor your flat feet treatment plan to your unique needs.
Comprehensive Flat Feet Treatment Options
At Center for Specialty Care, we create a personalized flat feet treatment plan to relieve your pain, restore function, and help you return to the activities you love. We always start with conservative, non-surgical treatments, as surgery is rarely the first option.
For more insights, see our article on A Walk Towards Healthy Feet: Common Foot Problems and Solutions.
Non-Surgical Flat Feet Treatment and Management
Most people find significant relief without surgery by combining supportive devices, exercises, and lifestyle adjustments.
- Lifestyle Changes: Weight management is highly impactful, as losing even a few pounds can dramatically reduce stress on your feet. Stick to low-impact exercises like swimming or cycling, and rest your feet when they are painful.
- Home Remedies: Applying ice for 15-20 minutes can reduce inflammation. Over-the-counter NSAIDs like ibuprofen can also help manage pain and swelling, but you should consult with us first.
- Orthotics and Supportive Devices: Arch supports are a cornerstone of treatment. They support the arch, realign the foot, and distribute pressure evenly. While over-the-counter options work for mild cases, we may recommend custom orthotics for more severe flat feet. An ankle brace can provide extra stability if needed.
- Proper Footwear: Choose shoes with a stiff sole, good arch support, and excellent shock absorption. Avoid flimsy, overly flexible shoes.
- Physical Therapy: Our physical therapists in Fairmont design custom programs to address muscle imbalances.
- Stretching exercises for tight Achilles tendons and calf muscles are essential.
- Strengthening exercises like the short foot exercise and heel raises build up the muscles that support the arch.
- Sensorimotor training improves balance and muscle coordination.
A systematic review from the National Institutes of Health confirms that both exercise and orthotics can reduce pain and improve foot alignment.
When is Surgery Considered for Flat Feet?
We consider surgery only when conservative treatments fail to provide relief, the deformity is severe, or there’s an acute injury like a tendon rupture.
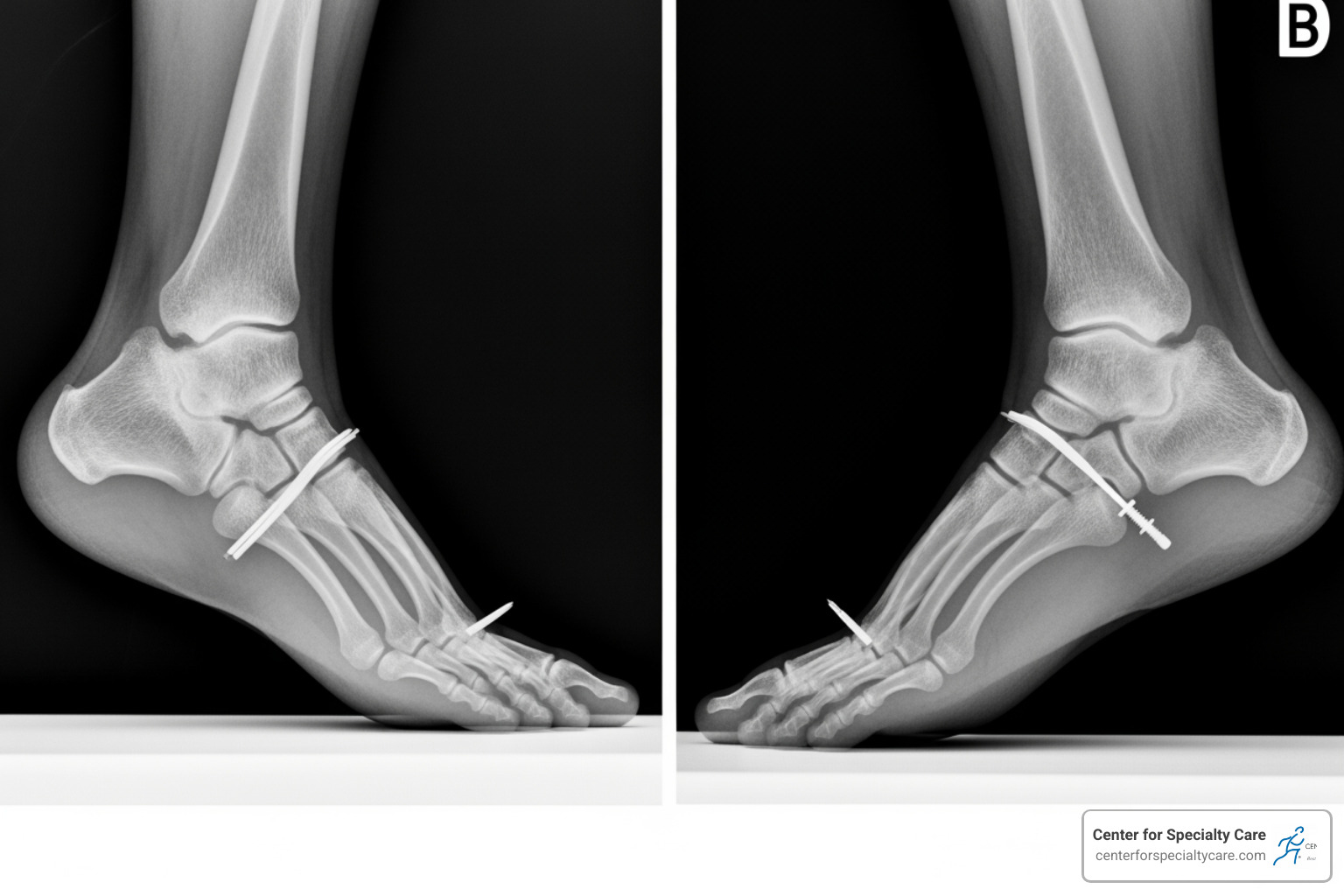
Indications for surgery include persistent pain that limits daily activities, a rigid or worsening arch collapse, or a completely ruptured posterior tibial tendon.
The surgical procedure depends on the cause and severity of your flat foot. Options may include:
- Tendon Repair or Transfer: To fix or replace a damaged posterior tibial tendon.
- Osteotomy: Cutting and reshaping bones to realign the foot and restore the arch.
- Arthrodesis (Joint Fusion): Fusing joints to provide stability and correct alignment in cases of rigid flat feet or severe arthritis.
- Arthroereisis: Placing a small implant to limit excessive foot motion.
- Ligament Repair: To restore support from a torn or stretched spring ligament.
Surgery carries risks, such as infection, nerve damage, blood clots, and non-healing of bones, which we will discuss thoroughly with you.
Recovery from flat foot surgery requires patience, typically involving a non-weight-bearing period in a cast followed by extensive physical therapy. Full recovery can take several months to a year. Following post-operative instructions, maintaining a healthy diet, and avoiding smoking are critical for a successful outcome.
For a full overview, read our guide: The Patient’s Guide to Podiatric Surgery: Expectations and Outcomes.
Frequently Asked Questions about Flat Feet
At our Fairmont clinic, certain questions about flat feet come up often. Here are answers to some of the most common concerns.
Can flat feet be permanently corrected without surgery?
For adults, the answer is generally no. Non-surgical treatments like exercises and orthotics are highly effective for managing symptoms, improving foot function, and preventing progression. They relieve pain and improve stability, but they don’t permanently change your foot’s bone structure. The goal of non-surgical flat feet treatment is to help your foot work better with the structure it has.
In children, flexible flat feet often correct themselves naturally as they grow.
What are the long-term complications if painful flat feet are left untreated?
Ignoring painful flat feet can lead to a cascade of problems. The most immediate issue is chronic pain in the foot and ankle. Over time, an altered walking pattern places abnormal stress on other joints, leading to secondary issues like bunions, hammertoes, shin splints, and Achilles tendonitis.
This misalignment can also accelerate arthritis in the foot and ankle. Furthermore, the kinetic chain effect can cause referred pain in the knees, hips, and lower back. Early intervention with proper flat feet treatment is the best way to avoid these complications.
Do children with flat feet need treatment?
Most children do not. It’s normal for babies and young children to have flat feet, with an arch typically developing by age 6 to 10. This painless, flexible flatfoot is a normal part of development and usually requires no intervention.
However, you should seek an evaluation if your child experiences foot or leg pain, has a rigid flatfoot (where the arch never appears), or if the condition significantly impacts their gait. When treatment is needed, it usually involves conservative measures like supportive shoes and exercises. Surgery is very rare for children.
Conclusion: Taking the Next Step Towards Pain-Free Feet
The key takeaway is that flat feet treatment is manageable and highly customizable. For most people, painful flat feet can be successfully treated with conservative, non-surgical approaches like supportive orthotics, targeted exercises, and physical therapy. While surgery is an option for severe cases, it is rarely the first step. You do not have to live with foot pain that limits your life.
Here at Center for Specialty Care in Fairmont, Minnesota, we understand that your feet are your foundation. We take a personalized, conservative-first approach to every patient, listening to your concerns and goals. Our commitment to 100% patient satisfaction and quick appointment availability means we’re ready to help when you need it most.
Taking control of your foot health starts with seeking professional help. You’ve done the research—now it’s time to take action.
Schedule a consultation with our podiatry experts and let’s work together to get you back to pain-free living. Your feet carry you through life, and they deserve expert care.