Podiatry in Fairmont, MN: Expert Foot & Ankle Care Near You
November 7, 2025
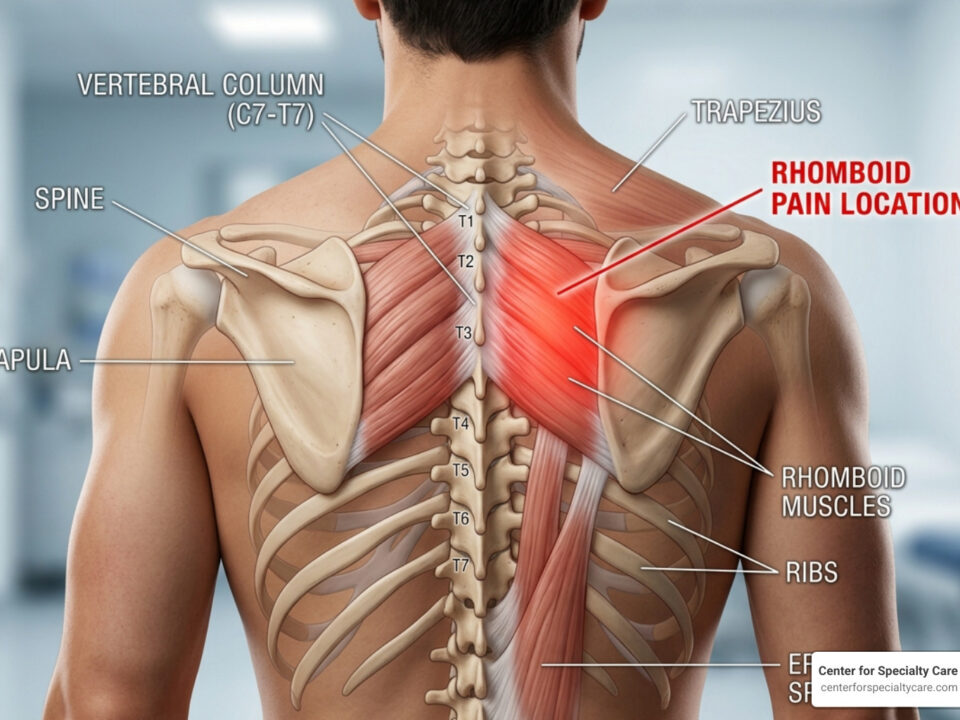
Healing Your Rotator Cuff: From Diagnosis to Relief
November 11, 2025Degenerative disc pain: Ultimate Relief 2025
Understanding Degenerative Disc Pain: What You Need to Know
Degenerative disc pain affects millions of adults, with discomfort ranging from a dull ache to severe episodes. Here’s a quick overview:
Quick Facts:
- What it is: Pain from wear and tear on the spinal discs that cushion your vertebrae.
- Common symptoms: Lower back or neck pain, stiffness, and radiating pain, numbness, or tingling in the arms or legs.
- Primary causes: Aging, disc dehydration, genetics, obesity, smoking, and repetitive strain.
- Pain pattern: Often worse when sitting, bending, or lifting; may improve with walking or changing positions.
- Treatment: Most cases respond well to conservative care like physical therapy, exercise, and lifestyle changes.
- Surgery needed: Only about 10-20% of cases require surgical intervention.
Despite its name, degenerative disc disease isn’t a disease but a wear-and-tear condition that’s a normal part of aging. While nearly everyone shows some disc degeneration after age 40, not everyone develops pain. The discs in your spine act as shock absorbers, but over time they can dry out, thin, and develop small tears. This can lead to pain, stiffness, and nerve-related symptoms.
The condition most commonly affects the lower back (lumbar spine) and the neck (cervical spine). The good news is that most people find relief without surgery. Around 80% of cases improve with conservative treatments. Understanding what’s happening in your spine is the first step toward getting the right care.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon with over 30 years of experience helping patients in southern Minnesota and northern Iowa manage spinal conditions. Using minimally invasive techniques and comprehensive pain management, I’ve helped thousands regain mobility and find relief from degenerative disc pain.

Understanding the Causes and Progression of DDD
Your spinal discs are cushions between each vertebra, with a tough outer layer (annulus fibrosus) and a soft, gel-like center (nucleus pulposus). They act as shock absorbers, allowing you to bend and twist. For a closer look at your spine’s design, see our guide to spinal anatomy.
As we age, our discs, which are about 80% water at birth, naturally lose moisture. This disc dehydration makes them thinner and less flexible. The resulting loss of disc height is a normal part of getting older, but for some, this wear and tear leads to degenerative disc pain.
While aging is the primary cause, several risk factors can accelerate this process:
- Genetics: Research shows that genetics is the most significant predictor of disc degeneration. If your family has a history of disc problems, you may be at higher risk. Learn more about the role of genetics in disc disease.
- Obesity: Extra body weight increases the load on your spinal discs, especially in the lower back, speeding up wear and tear.
- Smoking: Nicotine restricts blood flow, starving discs of the oxygen and nutrients needed to stay healthy.
- Repetitive Strain & Injury: Jobs involving heavy lifting, frequent twisting, or prolonged vibrations can cause cumulative micro-traumas. A single acute injury, like from a fall or car accident, can also trigger degeneration.
The Stages of Disc Degeneration
Degenerative disc pain develops gradually over decades. The process typically unfolds in four stages:
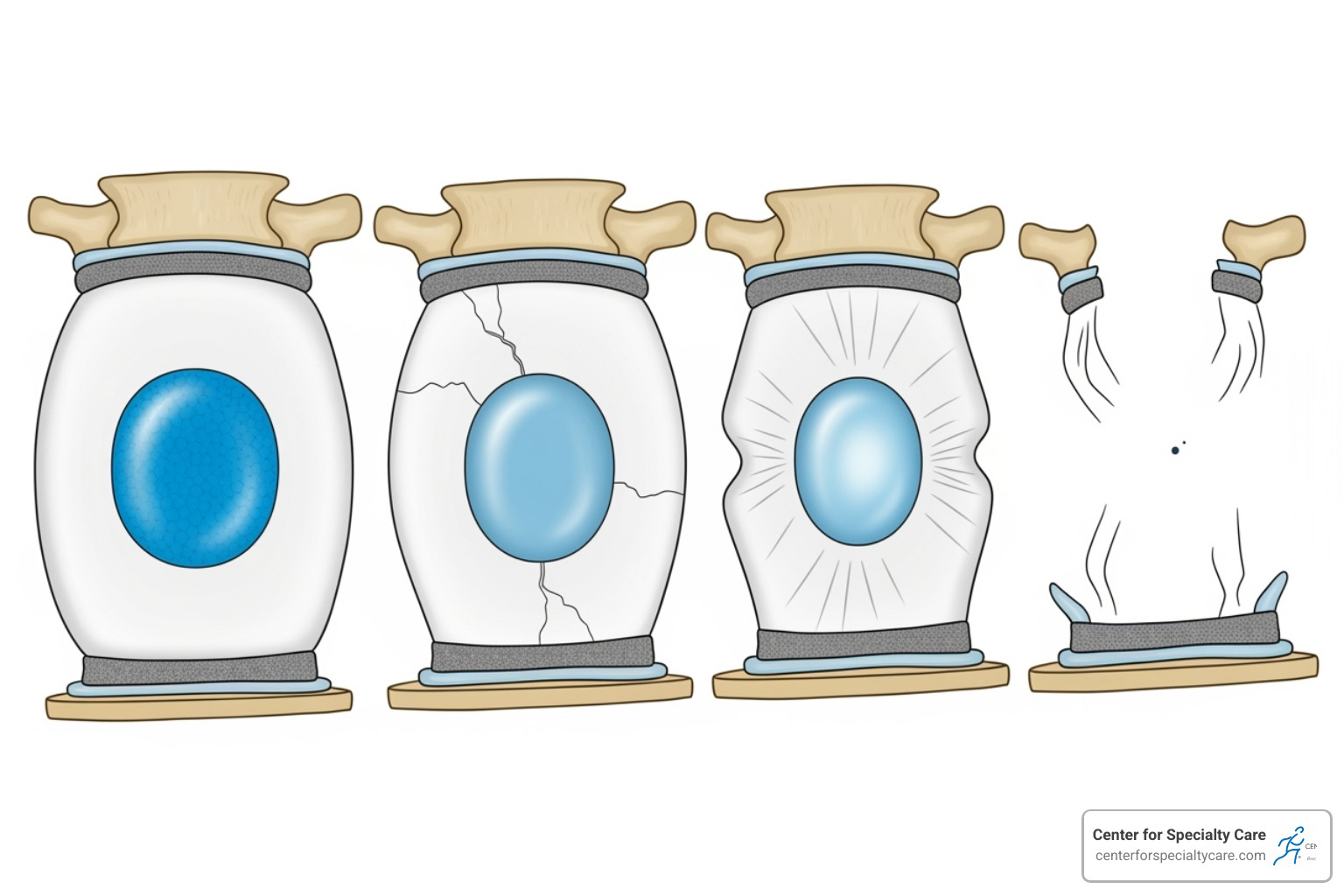
- Dysfunction: Tiny tears develop in the disc’s outer layer, causing mild, occasional pain and inflammation.
- Dehydration: The disc loses water and shrinks, reducing the cushion between vertebrae.
- Stabilization: The body forms bone spurs (osteophytes) to stabilize the spine, but these can sometimes press on nerves.
- Collapse: The disc flattens significantly, potentially leading to bone-on-bone contact, severe pain, and limited movement.
How Lifestyle Factors Impact Your Spine
Daily choices significantly affect your spinal health. Maintaining a healthy weight is crucial, as sitting already places three times more pressure on your lower back discs than standing. Nicotine effects on discs are also severe, as smoking constricts blood vessels and hinders the discs’ ability to repair themselves.
Sedentary lifestyle risks are well-documented; studies show that prolonged sitting weakens supportive muscles and increases disc pressure. Conversely, physically demanding jobs with heavy lifting or constant twisting create cumulative trauma. Finally, poor posture places uneven stress on your discs. Studies confirm a strong link between poor posture, especially while driving, and a higher risk of developing degenerative disc pain. Making small postural adjustments can reduce strain on your spine.
Recognizing Symptoms and Getting an Accurate Diagnosis
Degenerative disc pain can manifest as a chronic, low-level ache or as sudden, intense flare-ups. A telltale sign is pain that worsens with sitting, bending, or lifting, as these activities increase pressure on the discs. Many people find pain relief with movement, such as walking or frequently changing positions.
The pain is most common in the lower back (lumbar spine) and neck (cervical spine), but it can also travel to other areas if nerves are affected. Our guide on Common Spinal Conditions provides more context on various spinal issues.
Common Symptoms of Degenerative Disc Pain
When discs break down, they can press on nerves, causing a range of symptoms:
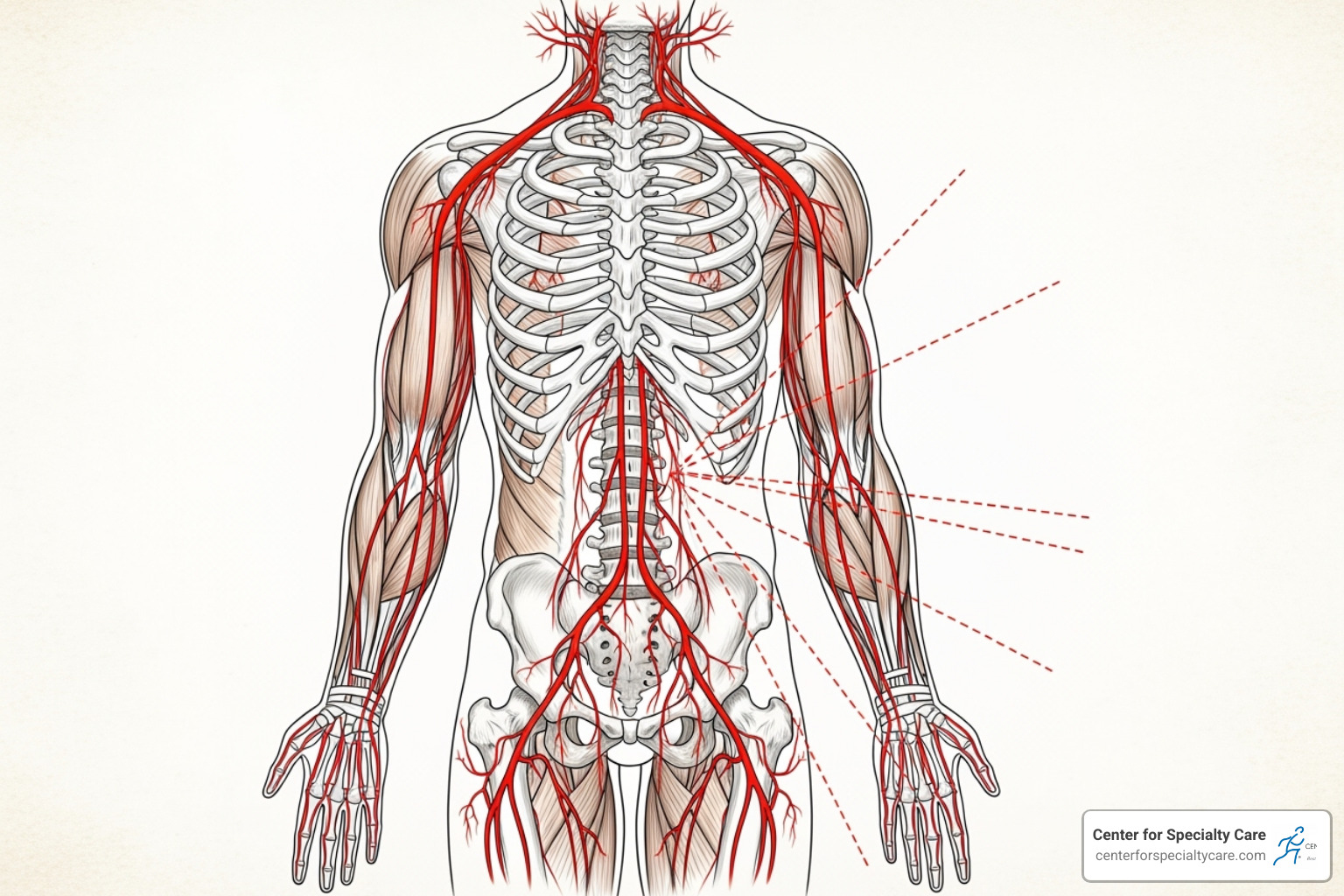
- Neck and Lower Back Pain: This is the most common complaint, often described as a deep, constant ache or stiffness.
- Radiating Pain: Pressure on a spinal nerve can cause pain to shoot down a leg (sciatica) or into an arm or shoulder. Our resource on managing radiating pain offers practical strategies.
- Numbness and Tingling: A pins-and-needles sensation in the arms or legs often accompanies radiating pain, indicating nerve irritation.
- Muscle Weakness: Difficulty with grip strength or lifting your foot can signal more significant nerve compression and requires prompt medical attention.
Disc degeneration on an MRI doesn’t always cause pain. We focus on your symptoms, not just the imaging results.
The Diagnostic Process
At Center for Specialty Care, we use a thorough process to diagnose degenerative disc pain.
We start with a medical history review and a physical examination to assess your spine’s movement, check your posture, and identify tender areas. A neurological exam helps determine if nerves are involved by testing your reflexes, muscle strength, and sensation.
Imaging tests provide a look inside your spine:
- X-ray: Reveals bone alignment, disc space narrowing, and bone spurs.
- MRI: The best tool for visualizing soft tissues like discs, showing dehydration, herniation, and nerve compression.
- CT scan: Offers detailed images of bone structures.
We always correlate imaging with symptoms to form an accurate diagnosis. If your pain is persistent or worsening, it’s time to seek help. Our article on when to see a doctor for back pain can guide you. We pride ourselves on quick appointment availability, so you don’t have to wait for care.
Conservative Care: Non-Surgical Treatments for Degenerative Disc Pain
Good news: surgery is rarely the first answer for degenerative disc pain. Most people find relief through conservative treatments that support the body’s ability to heal. Our approach at Center for Specialty Care is to help you feel and move better without invasive procedures unless they are truly necessary. We offer comprehensive Pain Management services custom to your specific needs.
For flare-ups, self-care is key. Use heat or ice for relief, perform gentle stretches like cat/cow or bridge pose, and modify activities that worsen pain. Good posture and over-the-counter pain relievers like NSAIDs or acetaminophen can also help manage mild to moderate discomfort.
Physical Therapy and Exercise
Physical therapy is where many patients see real change. Our therapists design a personalized program to help you recover.
A program will focus on:
- Core strengthening: Stronger abdominal and back muscles act as a natural corset for your spine.
- Flexibility and stretching: Reduces stiffness and improves your range of motion.
- Low-impact aerobic exercise: Activities like walking, swimming, or cycling improve blood flow and reduce pain without stressing your discs.
- Posture correction: Learn how to sit, stand, and move in ways that take pressure off your spine.
Many people notice improvement in as little as six weeks with a consistent program. Our Physical Therapy options are designed to help you regain mobility and get back to the activities you love.
Medications and Injections
While you build strength, medications and injections can help manage pain. Over-the-counter NSAIDs (ibuprofen, naproxen) and acetaminophen are effective for mild pain. For more intense pain, we may prescribe muscle relaxants or stronger anti-inflammatory drugs. You can find more details on medicines for back pain.
When inflammation causes significant nerve pain, epidural steroid injections can be a powerful tool. We deliver corticosteroids directly to the source of inflammation, providing a window of relief that allows you to progress in physical therapy. Nerve blocks work similarly by interrupting pain signals.
For some patients with chronic pain, we offer the Intracept Procedure, a minimally invasive treatment that targets the basivertebral nerve to provide lasting relief. Learn more about the IntraDisc Procedure and see if it’s right for you.
When Is Surgery Considered for DDD?
While most people with degenerative disc pain find relief with conservative care, surgery sometimes becomes the right path. We typically discuss surgery after 6 to 12 months of non-surgical treatments have failed to relieve persistent pain that limits your daily life.
Surgery may be considered more urgently if you experience progressive weakness in your arms or legs, as this indicates nerve compression that may not resolve on its own. A rare but critical “red flag” symptom is a loss of bowel or bladder control, which signals a medical emergency (Cauda Equina Syndrome) requiring immediate surgical intervention to prevent permanent nerve damage.
Our Back & Spine specialists will work with you to determine if surgery is the right choice. It is always a shared decision based on your symptoms, imaging, and personal goals.
Surgical Options for Severe Degenerative Disc Pain
When surgery is necessary, our Orthopedics expertise allows us to offer the most advanced techniques. Common options include:
- Discectomy: Removal of the damaged portion of a disc that is pressing on a nerve, often used to relieve radiating pain.
- Laminectomy/Foraminotomy: Creating more space for the spinal cord and nerves by removing a small portion of bone (lamina) or widening the opening where nerve roots exit (foramen).
- Spinal Fusion: Permanently connecting two or more vertebrae to eliminate painful motion from an unstable or severely degenerated disc segment.
- Artificial Disc Replacement: Replacing the damaged disc with a prosthetic device designed to preserve motion at the spinal segment. This is an excellent option for certain candidates.
| Feature | Spinal Fusion | Artificial Disc Replacement |
|---|---|---|
| Goal | Stabilize the spine, eliminate motion | Preserve motion at the disc level |
| Procedure | Joins vertebrae with bone grafts, screws, rods | Replaces damaged disc with prosthetic device |
| Indications | Instability, severe deformity, failed disc | Single-level disc disease, healthy facet joints |
| Potential Benefit | Reliable pain relief for instability | Maintains spinal flexibility, potentially lower risk of adjacent segment disease |
| Considerations | May increase stress on adjacent segments | Not suitable for all patients, long-term durability still being studied |
The right procedure depends on your age, health, the specifics of your condition, and your lifestyle goals. We will walk you through all options to find the solution that offers the best chance for a pain-free, active life.
Frequently Asked Questions about Degenerative Disc Disease
We’ve gathered the most common questions we hear from patients to provide clear, honest answers about living with degenerative disc pain.
What is the long-term outlook for someone with degenerative disc disease?
The long-term prognosis is positive for most people. The pain is often non-progressive, meaning it stabilizes or improves over time, and the condition is not life-threatening. Most patients successfully manage their symptoms with conservative pain management and lifestyle changes, maintaining an excellent quality of life without surgery. For those who do need surgery, outcomes are generally very positive. You can find more detailed information in these statistics on Lumbar Degenerative Disk Disease.
Can degenerative disc disease be prevented?
While you can’t stop the natural aging process, you can slow disc degeneration and reduce your risk of pain. Key prevention strategies include:
- Maintaining a healthy weight to reduce stress on your spinal discs.
- Regular exercise, focusing on low-impact activities like walking or swimming to strengthen supportive muscles.
- Proper lifting techniques to prevent acute injuries.
- Good ergonomics and posture at work and home to minimize strain.
- Quitting smoking to improve nutrient and oxygen flow to your discs.
What are the potential complications of untreated DDD?
Addressing degenerative disc pain early is important to avoid complications. If left untreated, the condition can lead to:
- Herniated disc: The weakened disc tears, allowing inner material to press on nerves.
- Spinal stenosis: A narrowing of the spinal canal that compresses the spinal cord and nerves.
- Spondylolisthesis: One vertebra slips forward over another, causing instability and nerve compression.
- Radiculopathy: Permanent nerve damage from prolonged compression, resulting in chronic pain, weakness, or numbness.
- Chronic pain: The nervous system can become hypersensitive, making pain harder to treat.
Timely, appropriate care can prevent these issues. If you have persistent pain, our team at Center for Specialty Care is here to help.
Conclusion: Taking Control of Your Spinal Health
Living with degenerative disc pain does not mean accepting a life of discomfort. As we’ve discussed, this condition is a natural part of aging, but its impact can be managed effectively.
Remember the most important takeaway: most people get better without surgery. Around 80% of patients find significant relief through conservative treatments. Physical therapy, targeted exercises, and lifestyle adjustments like maintaining a healthy weight are powerful tools for improving your quality of life. For the small percentage who may need surgery, modern procedures offer excellent outcomes for returning to an active life.
The key is proactive management. Don’t wait for the pain to become debilitating. Early intervention makes a significant difference in your long-term outlook.
At Center for Specialty Care, we partner with you to create a personalized care plan that fits your goals. With our commitment to patient satisfaction and quick appointment availability, you’ll receive compassionate, expert care without a long wait. You’ve taken the first step by educating yourself. Now, let us help you develop your personalized pain management plan and get you back to a more comfortable, active life.