The Great Debate: When to Use Heat or Ice for Tendonitis
January 8, 2026
Beyond the Ache: A Guide to Pain Management Doctors and Their Expertise
January 12, 2026Diabetic foot care: 5 Essential Steps
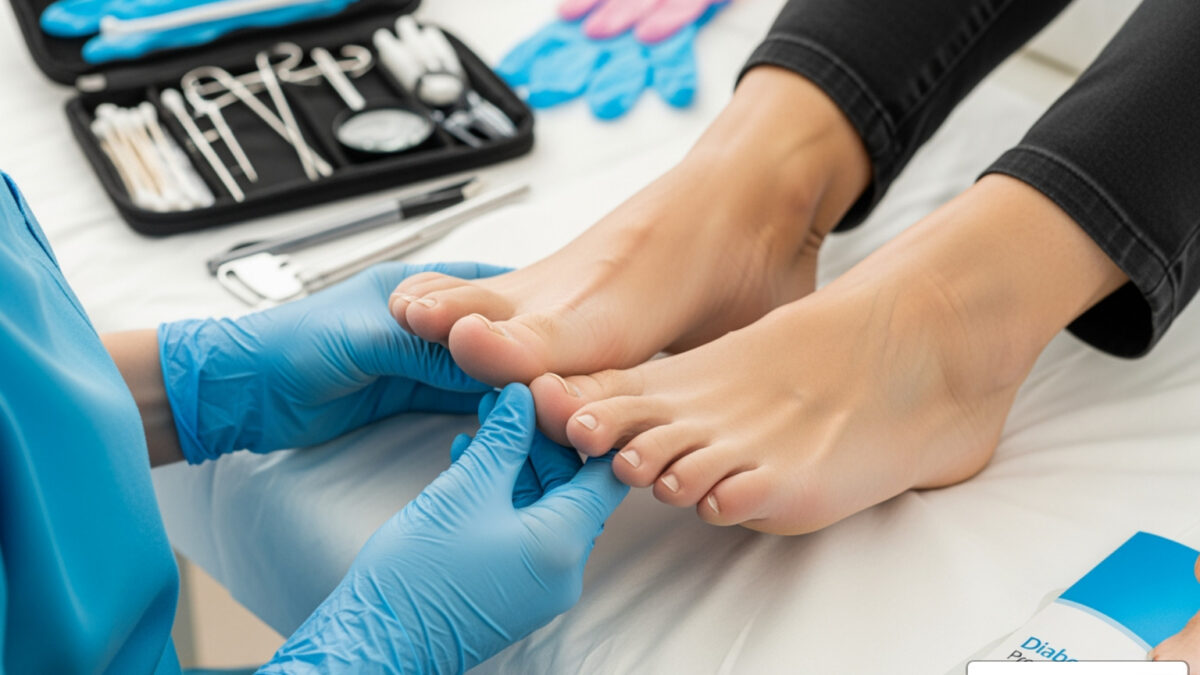
Why Diabetic Foot Care Matters More Than You Think
Diabetic foot care is essential for preventing serious complications like ulcers, infections, and amputation. Here are the key steps to protect your feet:
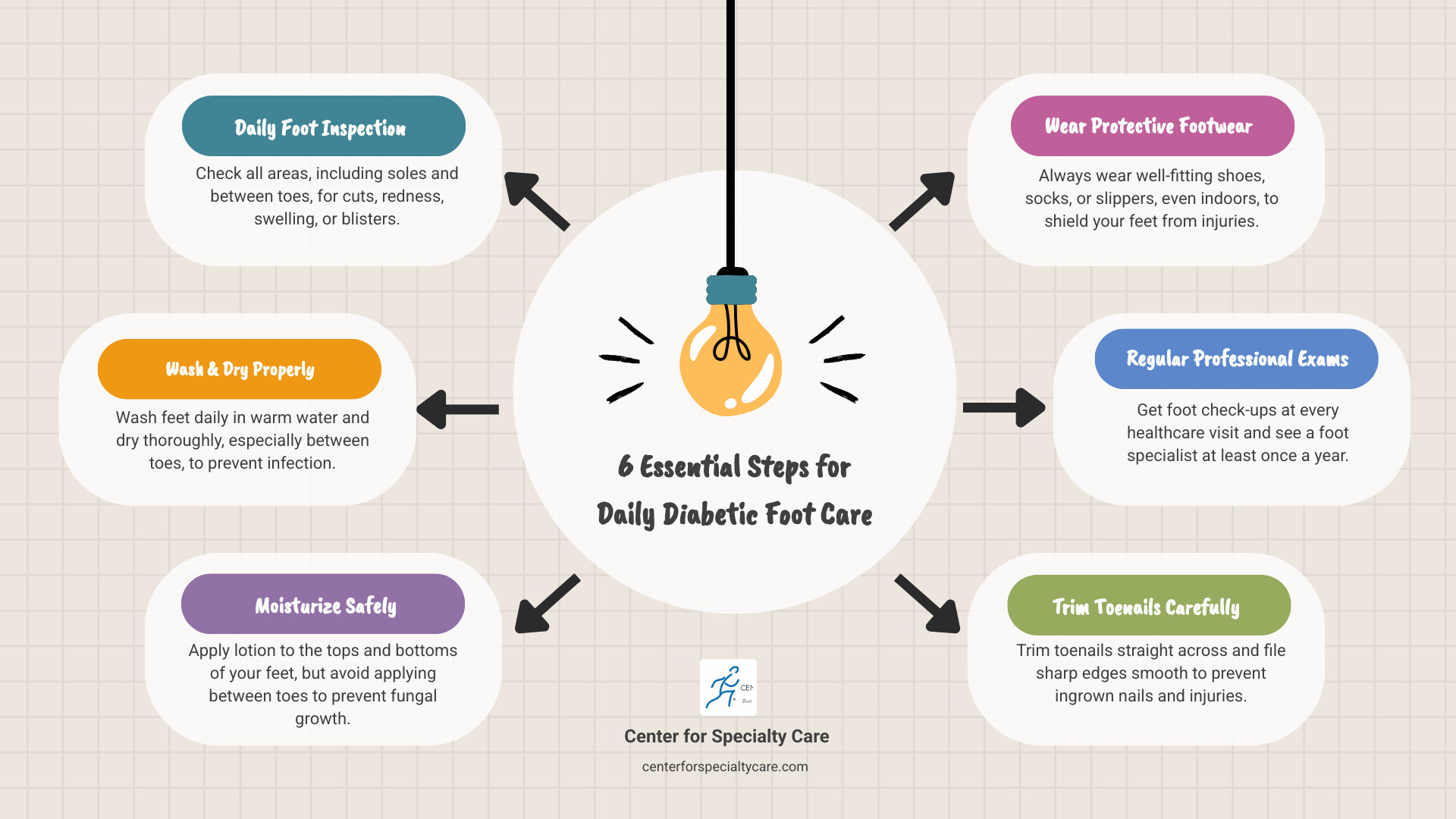
Daily Diabetic Foot Care Essentials:
- Check your feet every day for cuts, redness, swelling, sores, blisters, corns, or calluses
- Wash your feet daily in warm water and dry them thoroughly, especially between toes
- Never go barefoot, even indoors—always wear shoes and socks or slippers
- Trim toenails straight across and file sharp edges smooth
- Wear well-fitting shoes and moisture-wicking socks
- Get professional foot exams at every healthcare visit and see a foot specialist at least once a year
If you have diabetes, your feet face serious risks. High blood sugar damages nerves (neuropathy) and blood vessels, a dangerous combination. Neuropathy, which affects about half of all people with diabetes, can cause a loss of feeling in the feet, meaning you might not notice a cut or blister. At the same time, poor circulation slows healing and increases infection risk.
Statistics show the seriousness: about 1 in 5 hospital visits for people with diabetes are for foot problems, and about 15% will develop a foot ulcer. The good news is that most serious foot problems are preventable with proper daily care.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon. At the Center for Specialty Care in Fairmont, Minnesota, I emphasize that effective diabetic foot care begins with education and consistent daily habits to prevent serious complications.
Why Diabetes Puts Your Feet at Risk: The Twin Threats
Diabetes puts your feet at risk due to two main threats: nerve damage (neuropathy) and poor circulation (Peripheral Artery Disease, or PAD). High blood sugar quietly damages nerves and blood vessels, creating this dangerous combination. Neuropathy can prevent you from feeling an injury, while poor circulation impairs your body’s ability to heal it.
Research shows that about half of all people with diabetes will develop some form of nerve damage. Your risk increases significantly if your A1C levels stay above 7% for three years or longer. Uncontrolled blood pressure and cholesterol also accelerate nerve damage and restrict blood flow, making blood sugar control the foundation of effective diabetic foot care.
Diabetic Neuropathy: When You Can’t Feel Trouble
Diabetic neuropathy can mean walking with a pebble in your shoe or developing a blister without any pain to warn you. This is the reality for many living with the condition.
Neuropathy occurs when high blood sugar damages the nerves in your feet and legs. Symptoms vary, including tingling, sharp, burning pain (especially at night), or numbness. Some people have no symptoms, which makes daily foot checks vital.
The danger of neuropathy is the loss of protective sensation. Without pain signals, you might not notice stepping on a sharp object, a rubbing blister, or dangerously hot water. These unnoticed injuries can easily become infected.
Over time, nerve damage can also alter the shape of your feet, leading to deformities like hammertoes that create new pressure points and increase ulcer risk. If you’re dealing with nerve pain from neuropathy, you don’t have to suffer. We offer comprehensive pain management solutions that can help.
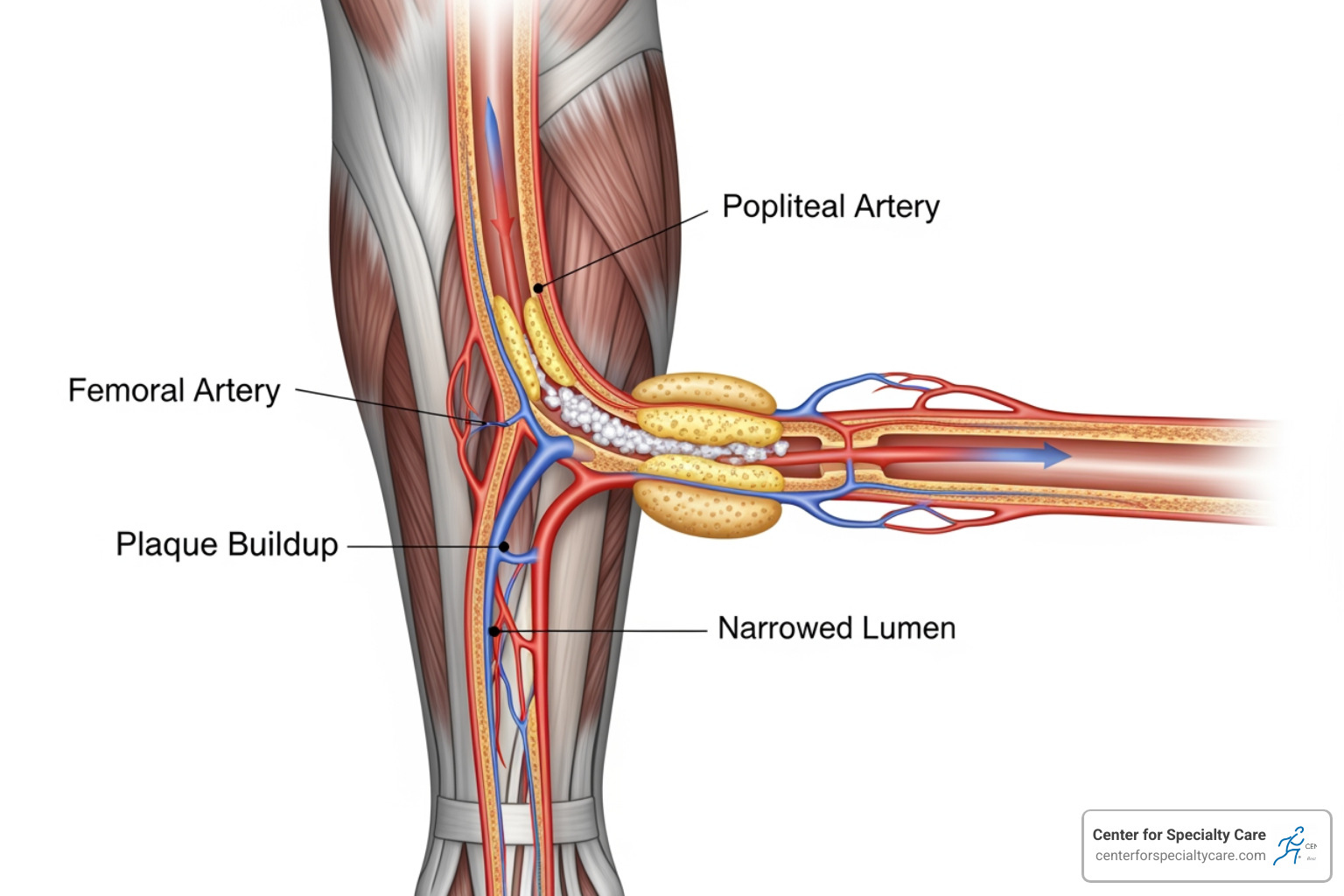
Peripheral Artery Disease (PAD): The Circulation Problem
While neuropathy affects your ability to feel, Peripheral Artery Disease (PAD) prevents your body from healing. PAD occurs when arteries in your legs and feet narrow, reducing blood flow. Blood carries oxygen and nutrients needed for healing, along with infection-fighting white blood cells.
Reduced blood flow means even minor cuts heal slowly and are more prone to infection, potentially turning a small scrape into a non-healing ulcer. Wounds may take weeks or months to heal instead of days, and the body’s defenses are weakened.
The most severe consequence is gangrene (tissue death), which appears as black or blue skin and may require amputation to stop its spread. Smoking dramatically worsens PAD by constricting blood vessels further. Quitting is one of the most important steps you can take to protect your feet.
Your Daily Diabetic Foot Care Routine: A Step-by-Step Guide
Daily diabetic foot care takes only a few minutes but is a crucial defense against serious complications. The key is consistency. Make it a daily routine, like brushing your teeth, perhaps after a shower or before bed.
Use a hand mirror to inspect the bottoms of your feet. If you have trouble with flexibility or vision, ask a family member or caregiver for help. A second pair of eyes can be incredibly valuable in spotting something you might miss.

Essential Steps for Daily Diabetic Foot Care
Keep your daily routine straightforward and focused on what matters most.
Wash your feet in warm water daily. Use mild soap and lukewarm water. If you have neuropathy, test the water temperature with your elbow first. Avoid soaking for more than 10 minutes, as this can dry out your skin.
Dry thoroughly, especially between your toes. Damp spaces between toes are a breeding ground for fungal infections like athlete’s foot. Pat your feet gently with a soft towel.
Moisturize the tops and bottoms, but not between your toes. A gentle, unscented moisturizer prevents painful cracks that can let bacteria in. Keep the area between your toes dry, using talcum powder if needed.
Check carefully for cuts, sores, blisters, redness, or swelling. Look for anything unusual, like a new cut, a red area from pressure, or changes in skin color. If something seems off, call your doctor right away.
Keep your feet protected at all times. Never go barefoot, even at home. Always wear shoes and socks or comfortable slippers to prevent injury.
How to Trim Toenails Safely
Incorrect toenail trimming can lead to ingrown nails or cuts that become infected.
Trim your toenails straight across after washing, when they are softer. Use clean nail clippers and don’t cut them too short.
File the sharp edges smooth with an emery board. This prevents sharp corners from digging into neighboring toes.
Avoid cutting down into the corners of your toenails. This dramatically increases your risk of painful ingrown toenails.
If your toenails are thick, discolored, or ingrown, or if you have difficulty reaching your feet, schedule an appointment with a podiatrist. They have the specialized tools and expertise to trim your nails safely. For more complex cases, you can learn more about what to expect from podiatric surgery.
The Right Support: Footwear, Socks, and Staying Active
Your shoes and socks are essential protection for your feet. Proper footwear provides a barrier against injury, while staying active improves circulation and keeps your feet healthier. Never go barefoot, even at home, to avoid injuries you might not feel due to neuropathy.
Proper fit is crucial. Therapeutic shoes are designed to reduce pressure points and accommodate deformities like hammertoes. Custom orthotics offer personalized support, distributing pressure evenly across your foot to prevent the hot spots that can lead to ulcers.

Choosing Diabetic-Friendly Shoes and Socks
When selecting footwear, be picky. Smart choices are the start of good diabetic foot care.
Before putting on your shoes, always check the inside for foreign objects, rough seams, or wrinkled linings that could cause a blister.
Choose moisture-wicking, seamless socks without tight elastic bands. This keeps feet dry and avoids restricting circulation. Cotton blends or specialized diabetic materials are good options.
Shop for shoes in the late afternoon or evening when your feet are at their largest. Ensure there’s about a thumb’s width of space between your longest toe and the end of the shoe. Extra-depth shoes can provide more room for custom orthotics or foot deformities.
For more information on addressing common foot issues, explore our helpful resources.
Information on common foot problems
The Role of Exercise in Maintaining Foot Health
Regular exercise is one of the best things you can do for your feet because it improves circulation. Increased blood flow keeps tissues healthy and helps your body fight infections.
Low-impact activities like walking, swimming, and biking are ideal. Always wear well-fitting, supportive shoes for walking and check your feet afterward for irritation. If you have open sores, avoid weight-bearing exercise until they heal completely.
Throughout the day, wiggle your toes and make circles with your ankles, especially if you sit for long periods. When seated, prop your feet up and avoid crossing your legs to promote blood flow.
If you have active foot problems, don’t start a new exercise program without professional guidance. Our physical therapy team can create a safe, effective plan for your specific needs.
More info about physical therapy
Red Flags: Recognizing Complications and When to See a Doctor
Despite a good diabetic foot care routine, complications can arise. Early detection and prompt medical help are critical to preventing serious emergencies. Many hospitalizations for diabetic foot problems—which account for about 1 in 5 such hospital stays—are preventable with early intervention.
Call your doctor immediately if you notice any of the following red flags:
- Non-healing sores: Any cut, blister, or wound that isn’t improving within a day or two.
- Skin color changes: Spreading redness, bluish discoloration, or areas turning darker.
- Temperature changes: One foot feeling significantly warmer or colder than the other.
- Unexplained swelling: Especially if it comes on suddenly.
- Foul odor: A bad smell from a wound or your foot almost always indicates infection.
- New pain or tingling: Even with neuropathy, new sensations need attention.
The CDC advises that when in doubt, get it checked out. Your feet are too precious to risk.
Information from the CDC on when to see a doctor
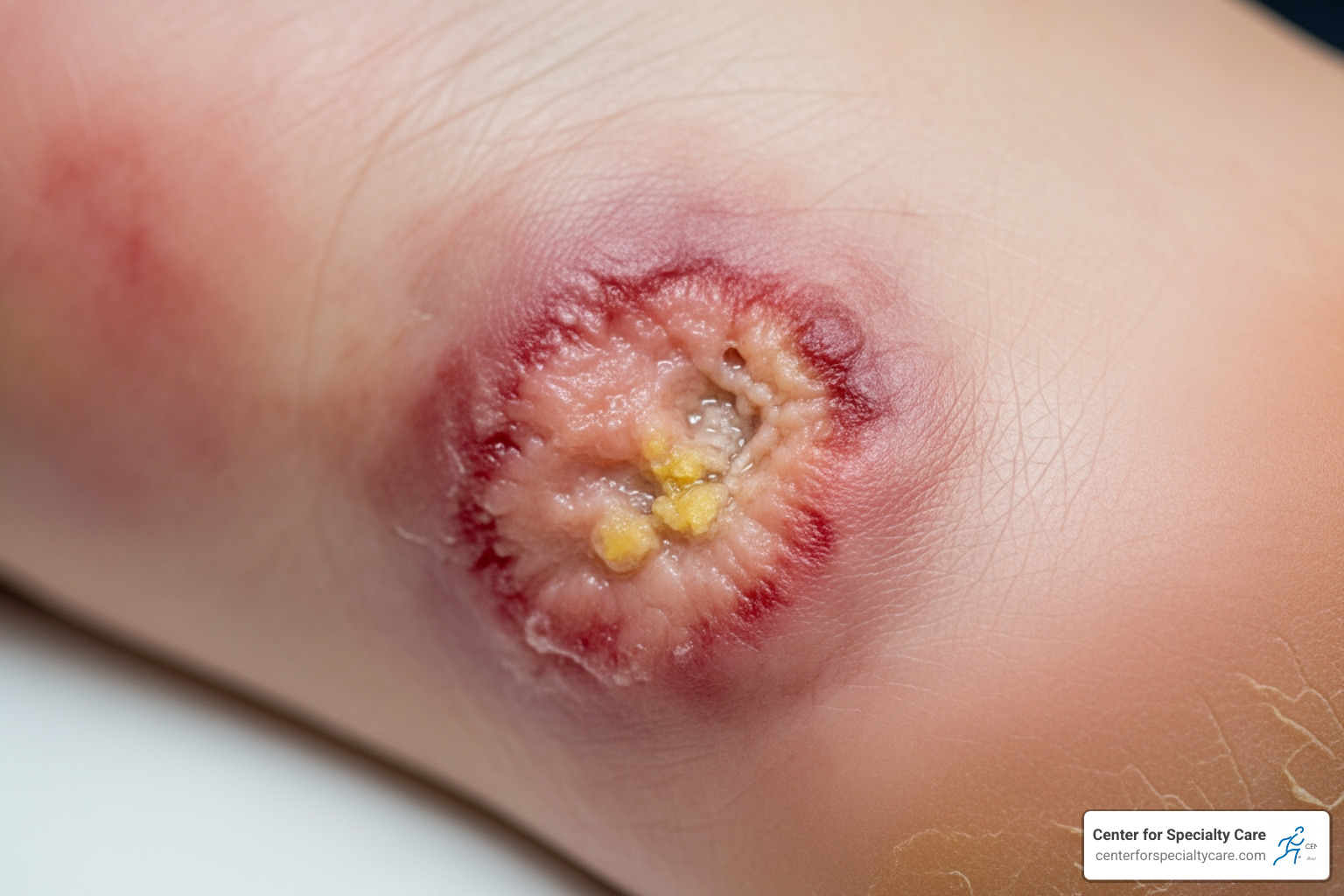
Warning Signs of Ulcers and Infections
Foot ulcers are a common and dangerous complication, affecting about 15% of people with diabetes. They can lead to severe infections and amputation if not treated promptly. Ulcers often appear as open sores on the bottom of the foot, sometimes starting as a simple blister. They require immediate medical attention as they are an entry point for bacteria.
Watch for these signs of infection:
- Drainage or pus coming from any wound.
- Black tissue around a sore, which indicates dead tissue.
- Pain and tenderness around the affected area.
- Red streaks spreading from a wound up your leg, which requires immediate intervention.
- Fever or chills, signaling a systemic infection. However, many people with a serious limb infection may not run a fever, making local signs like redness and swelling even more critical to watch for.
Understanding Serious Conditions: Charcot Foot and Gangrene
Charcot foot and gangrene are two of the most serious complications, requiring immediate medical intervention.
Charcot Foot is a rare but devastating complication where bones in the foot weaken and fracture without you feeling it. Continuing to walk on the numb, broken foot causes the arch to collapse, leading to severe deformity. Early signs mimic infection: redness, swelling, and significant warmth in the affected foot. As it progresses, the foot deforms, often into a “rocker-bottom” shape. Immediate immobilization (staying off the foot) is crucial to prevent further damage.
Gangrene is the death of body tissue, often resulting from an untreated infection or ulcer combined with poor circulation. Signs include discoloration (skin turning pale, blue, or black), numbness followed by severe pain, a foul-smelling discharge, and coldness of the affected area. Gangrene is a medical emergency requiring immediate treatment to prevent its spread and save the limb. If you see these signs, go to the emergency room.
Frequently Asked Questions about Diabetic Foot Care
Here are answers to some of the most common questions we hear about diabetic foot care.
Why do my feet get so dry and cracked with diabetes?
Dry, cracked feet are common with diabetes because nerve damage (neuropathy) can impair the function of your skin’s sweat and oil glands. Without this natural moisture, skin becomes dry and prone to cracking. These cracks create entry points for bacteria, making daily moisturizing essential to keep skin soft and prevent infection. Just remember to avoid applying lotion between your toes.
Can I use over-the-counter products for corns and calluses?
No, you should never use over-the-counter corn removers if you have diabetes. These products contain acids that can burn your skin, creating a wound you might not feel. This can lead to a chemical burn or a dangerous infection. While you can gently use a pumice stone on damp skin, never try to cut calluses yourself. For safe removal of bothersome corns or calluses, always consult a podiatrist.
How often should I see a foot doctor?
At a minimum, you should have a comprehensive foot exam by a healthcare provider at least once a year. This includes checking your sensation, circulation, and skin integrity.
More frequent visits—perhaps every few months—are necessary if you have a history of foot ulcers, significant loss of sensation from neuropathy, circulation problems (PAD), foot deformities like bunions or hammertoes, or thick or ingrown toenails that you can’t manage yourself.
These regular check-ups are key to proactive diabetic foot care. Our podiatry specialists at Center for Specialty Care focus on catching problems early to prevent emergencies.
Take the Next Step Toward Healthy Feet
When it comes to diabetic foot care, prevention is the best strategy. The daily habits we’ve discussed are not optional; they are investments in your future mobility and independence. This includes daily foot checks, wearing proper shoes, moisturizing your skin, and managing your blood sugar, blood pressure, and cholesterol. These actions directly protect the nerves and blood vessels in your feet.
Navigating diabetes can be overwhelming, which is why professional oversight is vital for your long-term health.
At Center for Specialty Care, we understand your journey is unique. Our expert podiatrists and orthopedic surgeons create personalized treatment plans for your specific needs. Whether you need a routine check-up, help with a complication, or advanced treatment, we provide the expertise and compassion you deserve.
Serving patients in Fairmont, MN, Estherville, IA, Buffalo Center, IA, and St. James, MN, we are committed to 100% patient satisfaction through personalized, comprehensive care.
Don’t wait for a small problem to become serious. If you have diabetes and haven’t had a recent foot exam, or if you’ve noticed any concerning changes, it’s time to act. Your feet deserve expert care from professionals who understand the unique challenges diabetes presents.
Contact our podiatry specialists today to schedule an appointment and take that next step toward healthier feet. We’re here to walk alongside you, ensuring your feet stay healthy and strong for all the journeys ahead.