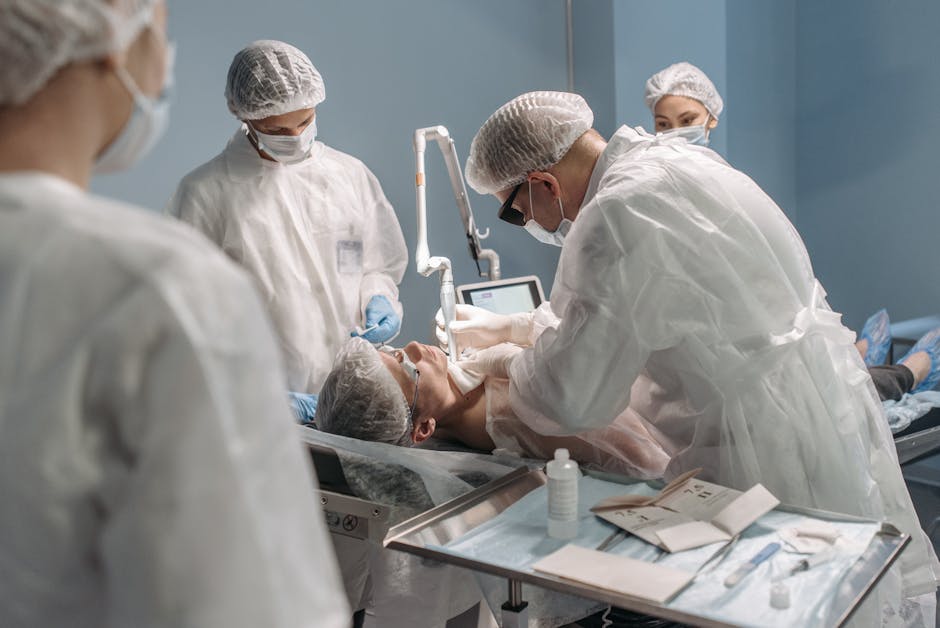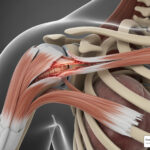
The Rotator Cuff Revealed: Anatomy, Injuries, and What a Tear Really Means
March 23, 2026
The Great Debate: Is Ice or Heat Best for Your Tendons?
March 25, 2026Everything you need to know about the Intracept procedure
Is the Intracept Procedure Right for You? A Quick Look at the Pros and Cons
Understanding the intracept procedure pros and cons is the first step toward deciding if this treatment could end your chronic low back pain. Here’s a fast summary:
Pros:
- Minimally invasive outpatient procedure (no large incisions)
- No implants left in the body
- Less than 0.3% rate of serious complications
- Around 65% of patients report at least 50% pain reduction
- Most people fully recover within 1-2 weeks
- Results can last 5 years or longer
Cons:
- Only works for vertebrogenic back pain (not all back pain types)
- Pain relief may take 2 weeks to 3 months to fully appear
- Insurance coverage varies and isn’t always guaranteed
- Rare risks include infection, nerve damage, or increased pain at the site
- Not suitable for everyone (pregnant individuals, pacemaker users, active infections)
Chronic low back pain affects millions of Americans — and for many, standard treatments like physical therapy, medications, or injections simply stop working. When that happens, a procedure like Intracept can sound like a lifeline. But like any medical treatment, it comes with both real benefits and genuine limitations worth understanding before you decide.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon with over 30 years of experience in minimally invasive spine and joint treatments, including procedures that address the kind of vertebrogenic pain at the heart of the intracept procedure pros and cons conversation. In the sections below, I’ll walk you through everything you need to make a confident, informed decision.

Intracept procedure pros and cons vocab to learn:
- intracept procedure
- intracept procedure recovery
- what is the success rate of the intracept procedure
What is the Intracept Procedure and How Does it Work?
At its core, the Intracept procedure is a minimally invasive treatment specifically designed to tackle “vertebrogenic” pain. This is a very specific type of chronic low back pain that originates from the vertebral bodies (the bones of your spine) rather than the discs or muscles.
To understand how it works, we first need to look at the spinal anatomy. Between your spinal discs and the vertebral bone are layers called vertebral endplates. Over time, due to wear and tear, these endplates can become damaged and inflamed. When this happens, the basivertebral nerve—a nerve located inside the bone of the vertebrae—begins to transmit persistent pain signals to your brain.
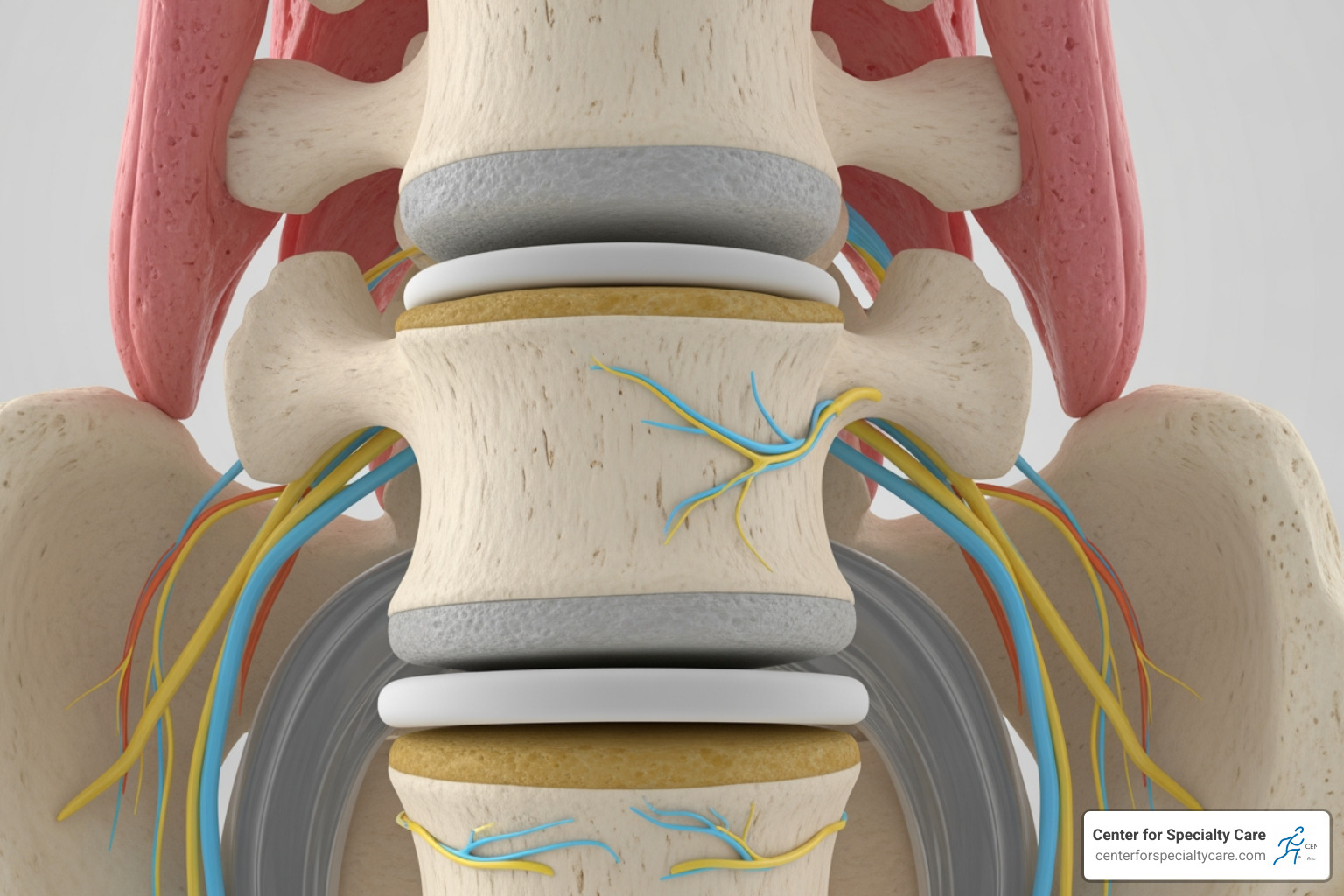
The Intracept procedure uses thermal ablation (heat) to deactivate this specific nerve. Here is the step-by-step breakdown of how we perform it:
- Access: Under local anesthesia and sedation, we make a tiny incision in the back.
- Guidance: Using real-time X-ray (fluoroscopy), we navigate a small cannula (a hollow tube) into the vertebral body.
- Ablation: We insert a radiofrequency probe through the cannula. Once in place at the trunk of the basivertebral nerve, the probe emits radiofrequency energy to heat and ablate the nerve.
- Disruption: This heat effectively “turns off” the nerve’s ability to send pain signals. Because the basivertebral nerve is a pure sensory nerve inside the bone, deactivating it does not affect your ability to move or feel other sensations.
According to scientific research on the Intracept procedure, this process is highly targeted. Unlike other back surgeries that might involve fusion or large hardware, Intracept leaves the structure of your spine intact.
Analyzing the Intracept Procedure Pros and Cons
When we sit down with patients in our Fairmont or Iowa clinics, we always weigh the clinical benefits against the potential drawbacks. This is not a “magic wand” for every type of back pain, but for the right person, it is often a game-changer.
One of the most significant aspects of the Intracept procedure is that it is an outpatient treatment. You come in, have the procedure (which usually takes about 60 to 90 minutes), and go home the same day. It is entirely implant-free, meaning there are no screws, cages, or plates left behind. This is a major advantage for patients who want to keep their options open for other back and spine treatments in the future.
However, a key “con” is that it is highly specific. It only treats pain coming from the vertebral endplates. If your pain is actually caused by a herniated disc, muscle strain, or sacroiliac (SI) joint issues, Intracept will not help. Furthermore, while some people feel better quickly, it can take several weeks for the inflammation from the procedure itself to subside and for the full pain-relieving effects to kick in.
For more technical details, you can review the scientific research on basivertebral nerve ablation.
The Major Pros of the Intracept Procedure
The list of advantages for Intracept is quite impressive, which is why it has become a preferred choice in our pain management toolkit.
- Durability: Clinical studies have shown that the relief provided by Intracept is not just temporary. Data shows that many patients maintain significant pain reduction for 5 years or longer. This is a “one-and-done” procedure for most.
- High Success Rate: Roughly 65% of patients report at least a 50% reduction in their pain levels within six months. Even more impressive, about one-third of patients in long-term studies reported being 100% pain-free.
- Quick Recovery: Most of our patients return to their normal daily routines within a week or two. You aren’t stuck in a brace or bedridden for months.
- Safety Profile: The serious complication rate is incredibly low—less than 0.3%. Because we aren’t moving major muscles or messing with the spinal canal directly, the risks are significantly lower than traditional open surgery.
Potential Cons of the Intracept Procedure
No medical procedure is without its downsides. When considering the intracept procedure pros and cons, we must be honest about the limitations.
- Narrow Candidacy: You must have “Modic changes” visible on an MRI to qualify. If your MRI doesn’t show this specific type of endplate inflammation, we won’t recommend the procedure because it likely won’t work for you.
- Delayed Relief: This isn’t like a steroid injection that might kick in within 48 hours. It takes time for the body to heal from the thermal ablation. You might even feel a bit more sore for the first few days.
- Insurance Hurdles: While Medicare and many commercial plans now cover Intracept, the authorization process can be rigorous. We spend a lot of time helping our patients navigate these requirements.
- Surgical Risks: Although rare, any procedure involving a needle or incision carries a risk of infection, bleeding, or localized nerve irritation.
Understanding these common spinal conditions is essential to ensuring you are targeting the right source of pain.
Who is an Ideal Candidate for the Intracept Procedure?
Determining if you are the “ideal” candidate is the most important part of our consultation process. We look for a very specific “triad” of symptoms and clinical findings:
- Chronic Pain: You must have suffered from low back pain for at least six months.
- Conservative Care Failure: You have tried other pain management options—such as physical therapy, chiropractic care, or medications—for at least six months without success.
- MRI Evidence: This is the deal-breaker. Your MRI must show “Modic changes” (Type 1 or Type 2) at the L3 to S1 levels of your spine. These changes are the “smoking gun” that proves your pain is coming from the vertebral endplates.
Who should NOT get the Intracept procedure? There are certain contraindications where we would advise against this treatment. These include:
- Pregnancy (due to the use of X-ray guidance).
- Active systemic infections or infections at the site of the procedure.
- Patients with pacemakers or other electronic implants (the radiofrequency energy can interfere with them).
- Severe heart or lung disease that makes sedation unsafe.
- Pain clearly coming from other sources, like the facet joints or a fresh disc herniation.
If you meet the criteria, the Intracept procedure can be life-changing.
Recovery Timeline and Long-Term Success Rates
One of the most common questions we hear is: “When can I get back to my life?”
The recovery timeline for Intracept is remarkably short compared to traditional surgery.
- Days 1-2: You should rest and avoid any heavy lifting or strenuous activity. You might feel some soreness at the incision site, which can be managed with over-the-counter pain relievers or ice packs.
- Days 3-7: Most patients return to light work (desk jobs) and basic daily activities. Walking is encouraged!
- Weeks 1-2: Full recovery for most. You can typically resume the activity levels you enjoyed before the onset of your back pain.
Regarding long-term success, the data is very encouraging. In a 5-year follow-up study of 249 patients, roughly 70% were able to resume their prior activity levels. Furthermore, 65% of people reported at least a 50% reduction in back pain, and 22.4% reported being completely pain-free. These results are far superior to what we typically see with continued “conservative” management for chronic sufferers.
Our pain management specialists will monitor you closely during this window to ensure the inflammatory relief is progressing as expected.
Frequently Asked Questions about the Intracept Procedure
Does insurance cover the Intracept procedure?
Yes, in many cases. Medicare has established coverage for the Intracept procedure when specific medical necessity criteria are met (the 6-month rules mentioned above). Many commercial insurance providers have also followed suit. However, “prior authorization” is almost always required. We work closely with our patients to submit the necessary MRI findings and treatment history to help secure coverage.
How does Intracept compare to traditional radiofrequency ablation (RFA)?
While both use heat to disrupt nerves, they target completely different things.
- Traditional RFA: Targets the “medial branch” nerves. These nerves carry pain signals from the facet joints (the small joints on the back of the spine). This often needs to be repeated every 6-12 months because those nerves can regrow.
- Intracept: Targets the “basivertebral nerve” inside the bone. This treats vertebrogenic pain from the endplates. Because of the way this nerve is positioned inside the bone, it generally does not regrow, making Intracept a one-time procedure for most.
What are the most common side effects?
The most common side effects are mild and temporary. They include:
- Soreness or “heaviness” at the site of the incision.
- Minor bruising or swelling.
- Temporary numbness or tingling in the legs (usually resolving within days).
- A brief “flare” of your typical back pain before it begins to subside.
Conclusion
At the Center for Specialty Care, we understand that chronic back pain isn’t just a physical sensation—it’s a barrier to living your life. Whether you are in Fairmont, MN, or one of our Iowa locations, our goal is 100% patient satisfaction through personalized, expert care.
The intracept procedure pros and cons show that while this isn’t the right choice for every patient, it is a breakthrough for those suffering from vertebrogenic pain. If you’ve been told you “just have to live with it” or that “major surgery” is your only option, it’s time for a second opinion.
We offer quick appointment availability so you don’t have to wait months for relief. Our team will walk you through the MRI review, the insurance process, and every step of the recovery.
Are you ready to stop managing pain and start treating it? Schedule your Intracept procedure consultation today and let us help you get back to the activities you love.