Step Into Comfort: The Premier Orthopedic Clinic in Fairmont
October 28, 2025
Precision Healing: The Benefits of Specialized Orthopedic Care
October 29, 2025Intracept procedure covered by insurance 2025: Finally!
A New Horizon for Chronic Back Pain Relief
Intracept procedure covered by insurance is a reality for millions of Americans with chronic low back pain. Major insurance providers like Anthem Blue Cross and Blue Shield, Cigna Healthcare, and Humana now have favorable coverage policies for this groundbreaking treatment.
Quick Coverage Overview:
- Medicare: Covers Intracept when specific criteria are met (6+ months chronic pain, failed conservative treatments, MRI showing bone marrow lesions)
- Major Private Insurers: Anthem, Cigna, and Humana now have positive coverage policies
- TRICARE: Provides coverage under specific radiofrequency denervation guidelines
- Workers’ Compensation: May cover the procedure for work-related back injuries
The Intracept Procedure is a breakthrough for treating vertebrogenic pain—chronic low back pain originating from damaged vertebral endplates. This minimally invasive, outpatient treatment uses radiofrequency energy to target the basivertebral nerve (BVN) within the spine, stopping pain signals at the source.
Unlike traditional back surgeries, the Intracept Procedure requires no implants and preserves spinal structure while providing lasting relief. The treatment takes 60-90 minutes, and most patients return home the same day.
As Dr. Corey Welchlin, I’ve seen how expanding intracept procedure covered by insurance policies are changing options for our patients at Center for Specialty Care. With over three decades of orthopedic experience, I help patients steer the clinical and insurance aspects of this innovative treatment.
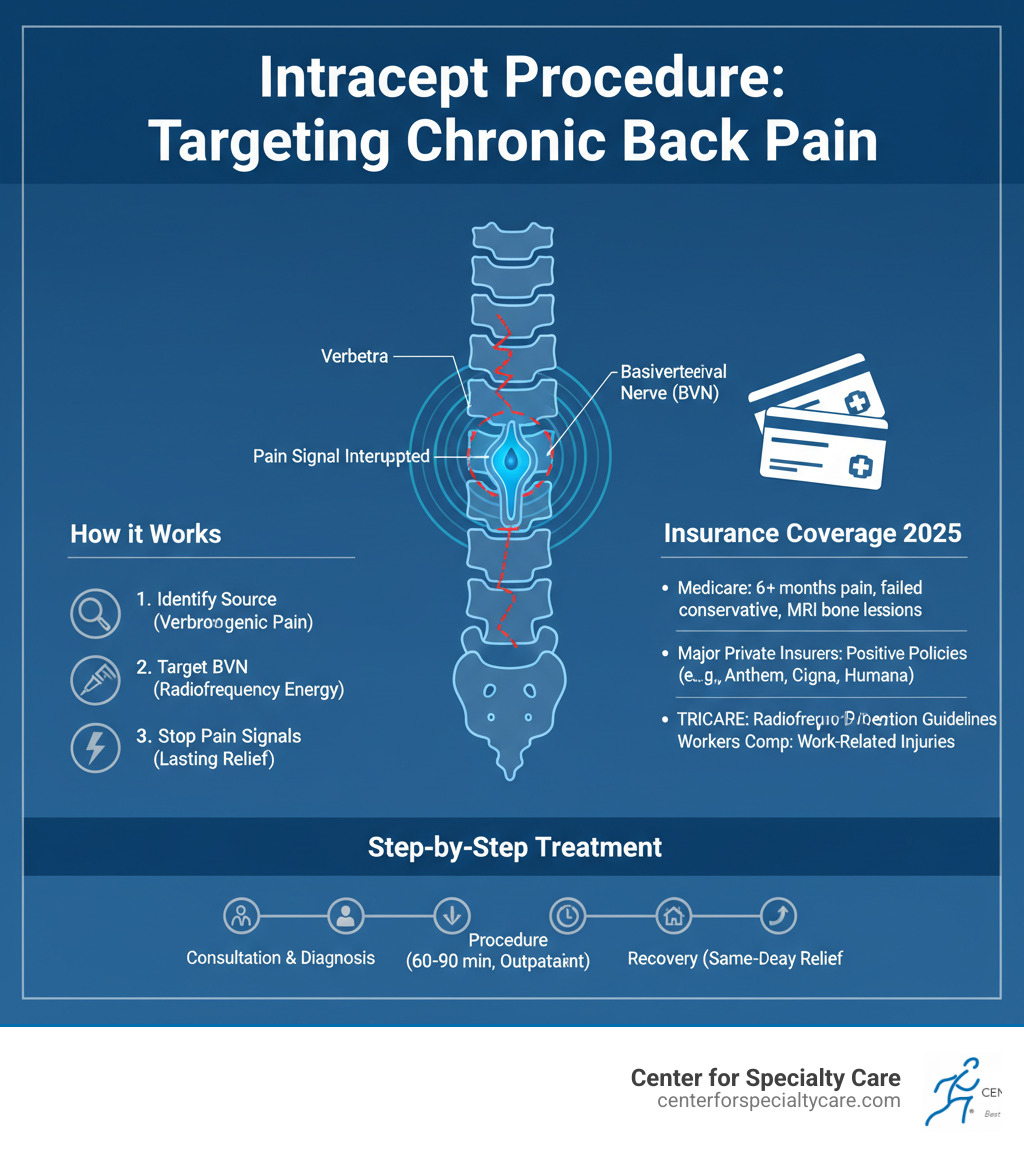
Intracept procedure covered by insurance basics:
What is the Intracept Procedure and How Does It Work?
If you live with chronic low back pain, you may wonder what causes the persistent ache. For many, the cause is vertebrogenic pain, which starts deep inside the vertebrae.
Your vertebrae are connected to spinal discs by endplates. When these endplates are damaged or inflamed from injury or wear, they can irritate the basivertebral nerve (BVN) inside the vertebra. This nerve then sends pain signals to your brain. This is where the Intracept Procedure helps.
The Intracept procedure uses a precise, minimally invasive approach to target this nerve. During the treatment, a physician uses advanced imaging to guide a probe into the vertebra. Once positioned, radiofrequency ablation (controlled heat) quiets the basivertebral nerve, stopping pain signals at their source.
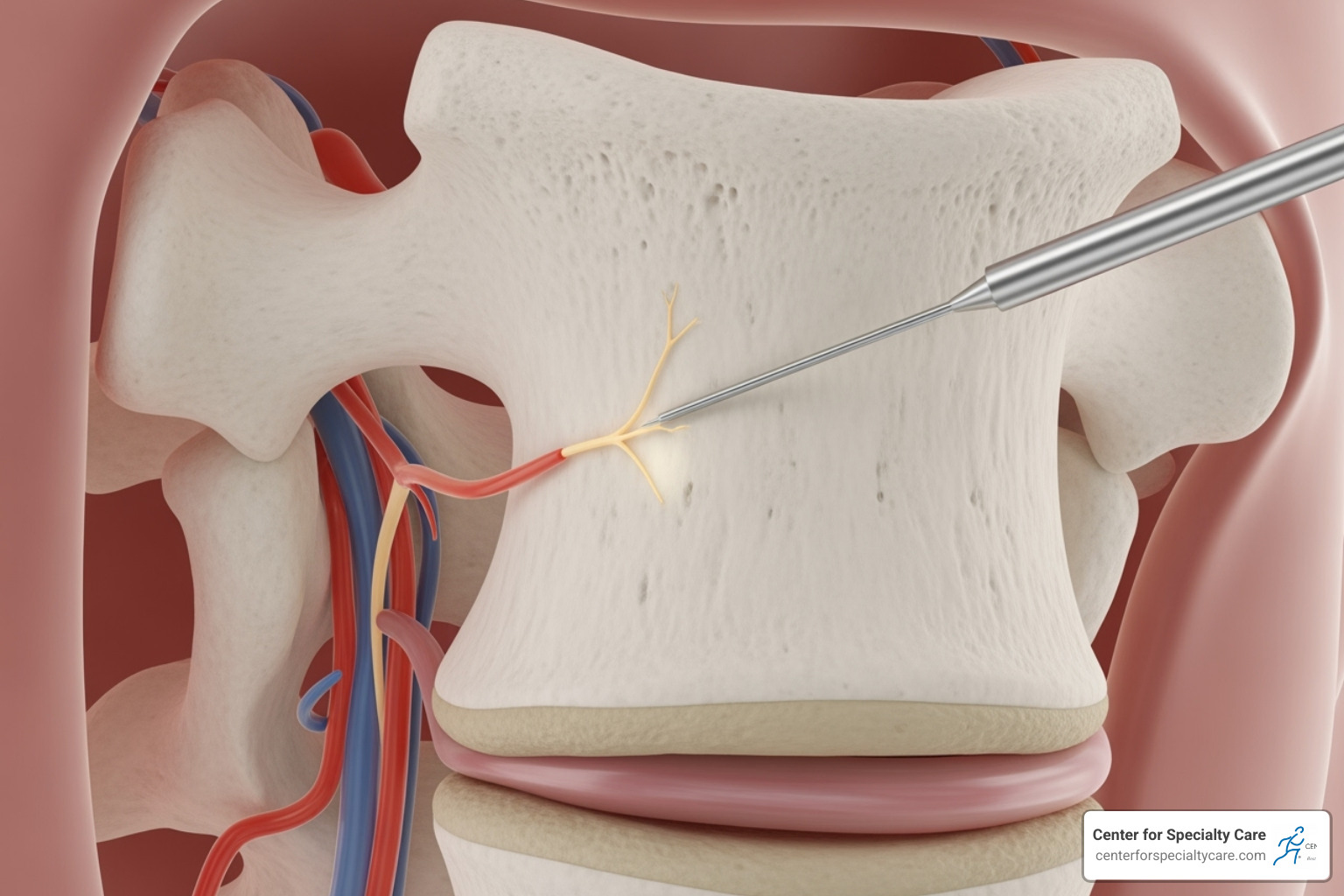
Its minimally invasive nature is a key benefit. It’s an outpatient procedure taking 60-90 minutes, with no implants left behind, and you go home the same day.
The spine-sparing benefits are also significant. Unlike fusion surgery, Intracept doesn’t alter your spinal structure or limit movement. It’s a targeted pain management solution for the spine without the long recovery of traditional surgery.
The Clinical Evidence Behind Intracept
The Intracept Procedure has impressive clinical backing and is proven to work. The procedure earned FDA approval based on robust, long-term studies like the SMART Trial and INTRACEPT Trial.
Results show long-term pain relief, with some studies tracking improvements for up to five years. Patients also saw impressive functional improvement, returning to activities they had given up. Many also significantly reduced opioid use, with one study showing a 73% decrease at five years.
This solid scientific evidence for basivertebral nerve ablation validates the treatment and is crucial for expanding insurance coverage.
Who is an Ideal Candidate for this Procedure?
The Intracept Procedure isn’t for everyone; we ensure it’s the right treatment for you. Ideal candidates typically meet the following criteria:
- Chronic low back pain lasting more than 6 months.
- Failure of conservative care, meaning at least six months of treatments like physical therapy, medications, or injections without lasting relief.
- MRI findings must show Modic Type 1 or 2 changes in the vertebral endplates (typically between L3 and S1), which indicate the pain is likely vertebrogenic.
- Pain that worsens with sitting or bending forward.
- The primary complaint should be low back pain, not pain radiating down the legs.
If this describes your situation, learn More info about our Intracept Procedure and let our team guide you through the evaluation.
Is the Intracept Procedure Covered by Insurance?
This is a common question, and the good news is that the intracept procedure covered by insurance landscape has expanded dramatically. Major insurers now recognize that the procedure is effective, thanks to robust clinical evidence. This shift means more hope and fewer financial headaches for patients in Minnesota and Iowa with chronic back pain.

Securing coverage requires demonstrating medical necessity through proper documentation for prior authorization. This process ensures you are a good candidate for the procedure. Insurers want to see that you’ve tried other treatments first and that your pain type matches what the procedure treats. At Center for Specialty Care, our team handles the insurance process for you, knowing what each insurer needs to build the strongest case.
Major Insurers with Favorable Coverage Policies
Several major insurers have recognized that covering the Intracept procedure makes both clinical and financial sense.
- Anthem Blue Cross and Blue Shield established a positive coverage policy in September 2023, opening doors for millions of members.
- Cigna Healthcare implemented positive coverage in June 2023, acknowledging the procedure’s benefits.
- Humana published favorable policies in November 2023, impacting over 13 million patients.
- Highmark BCBS established its favorable coverage policy effective March 4, 2024.
The trend is clear: major insurers are embracing the Intracept Procedure as an effective treatment option.
Understanding Medicare and TRICARE Coverage
Medicare and TRICARE also recognize the value of this treatment, though they have unique coverage approaches.
Medicare coverage is determined by regional Local Coverage Determinations (LCDs). Medicare generally requires chronic low back pain for at least six months, failed conservative treatments, and MRI confirmation of Modic Type 1 or 2 changes. Once criteria are met, the approval process is often straightforward.
TRICARE coverage follows specific guidelines for radiofrequency denervation. It has similar requirements: chronic low back pain for at least six months, three months of failed conservative care, and documented Modic changes on MRI. Notably, TRICARE typically excludes patients with prior spinal fusion at the treatment level to ensure the best outcomes.
For detailed information, we recommend checking out: More info about TRICARE West RF Denervation.
Whether you have private insurance, Medicare, or TRICARE, a path to coverage likely exists if you’re a good candidate. Our team can help you steer the system to access the care you need.
Qualifying for Coverage: What Are the Medical Necessity Criteria?
Getting your intracept procedure covered by insurance requires proving it is medically necessary. You must show that this treatment is needed after other options have failed. Insurers follow specific guidelines to ensure they cover evidence-based treatments for the right patients. At Center for Specialty Care, our orthopedics team are experts at gathering the necessary documentation to build a strong case.
The process can seem overwhelming, but we handle the paperwork and insurance communications so you can focus on getting better.
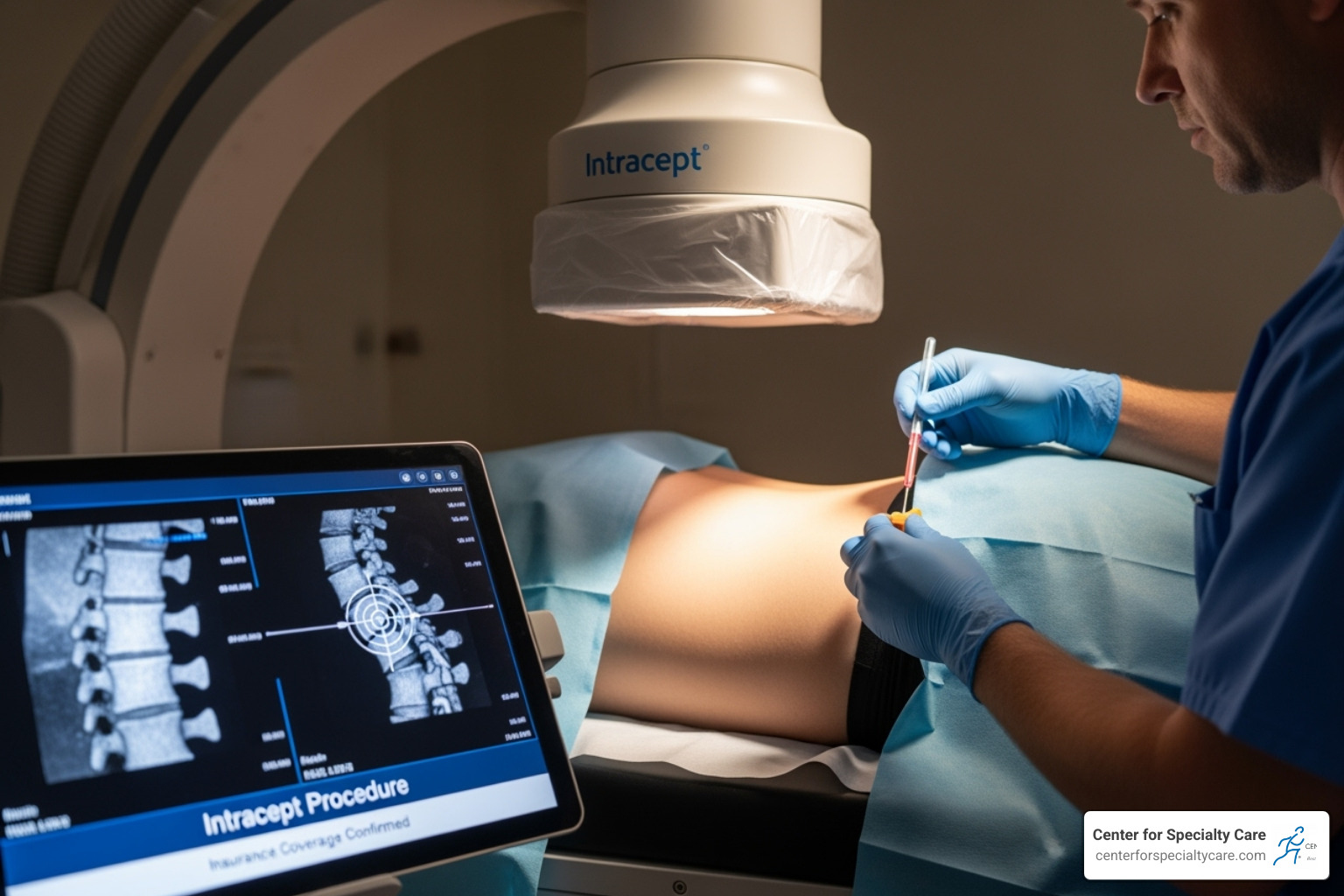
Typical Criteria for the Intracept Procedure Covered by Insurance
While specifics vary, most insurers follow similar guidelines for medical necessity.
- Duration of Pain: You must have persistent chronic low back pain for at least six to 12 months, depending on your insurer.
- Failed Conservative Treatments: You must show failure of conservative treatments, typically for six consecutive months. This includes structured, physician-supervised care like physical therapy, targeted injections, medication management, and lifestyle modifications. Some insurers also require cognitive behavioral therapy.
- MRI Confirmation: Your MRI must clearly show Modic Type 1 or Type 2 changes in the vertebral endplates, typically between the L3 and S1 levels. These changes are specific signs that your pain originates from the vertebrae.
- Pain Location: Your pain must be primarily axial low back pain (in the lower back, not radiating down the legs) and involve no more than three adjacent vertebral bodies.
Common Contraindications That May Affect Coverage
Certain contraindications, or red flags, may prevent coverage. These are safety measures to protect patients and ensure good outcomes. Common contraindications include:
- Active infections
- Severe heart or lung problems
- Being skeletally immature (under 18)
- Pregnancy
- Severe spinal instability or large disc protrusions
- Active implantable devices like pacemakers
- Previous spine fractures or metabolic bone diseases at the treatment site
Our commitment to 100% patient satisfaction means we carefully evaluate your health history to ensure Intracept is the safest and most effective option for you.
Navigating the Approval and Billing Process
Getting your intracept procedure covered by insurance involves paperwork, but our experienced team at Center for Specialty Care guides you through the process. We know how to present your case for the best chance of approval.
The process involves using specific medical codes. For Intracept, these are CPT codes 64628 (for the first two vertebral bodies) and 64629 (for each additional one). The common diagnosis code is ICD-10 M54.59 for chronic low back pain. Hospitals may also use HCPCS Code C1889 for device costs. These codes are key to coverage.
Our patient advocacy goes beyond forms. We create a comprehensive package with your patient information that tells your unique story, explaining why this procedure is your best path forward. This detail helps secure approval.
The Prior Authorization Process for the Intracept Procedure Covered by Insurance
Prior authorization is your insurer’s request for justification. Our team has perfected this process. We submit a request by gathering your clinical documentation, MRI reports showing Modic changes, and a detailed letter of medical necessity from your doctor.
The insurance review timeline is typically two to three weeks. We stay in contact with your insurer during this time to answer any questions. The Boston Scientific Patient Access Program is another valuable resource. The company’s staff works with insurers to educate them and help patients with coverage challenges. We can connect you with this program for extra support.
What to Do If Your Intracept Claim is Denied
A denial can be disheartening, but it’s not the final word. Denials are often overturned on appeal. We first review the denial letter to understand the reason, which is often incomplete documentation or a claim that the procedure is experimental (it is FDA-approved).
For the internal appeal, we build a stronger case. A detailed letter from your physician is crucial and can be very powerful. If needed, an external review (IRO) brings in independent medical experts who often side with patients when the medical evidence is clear.
Your doctor’s support is critical throughout this process. Persistence pays off, as many initial denials are overturned on appeal. We’re here to guide you through every step. For complex cases, you may want to explore Legal guidance on insurance denials to understand all your options.
Frequently Asked Questions about Intracept Insurance Coverage
Patients often have questions about getting their intracept procedure covered by insurance. Understanding coverage can be overwhelming, so let’s address the most common concerns.
How do I know if my specific insurance plan covers the Intracept Procedure?
Insurance plans vary, even within the same company. The best first step is to schedule a consultation at Center for Specialty Care. Our team will perform a comprehensive benefits investigation. We work directly with your insurer to verify coverage, estimate out-of-pocket costs, and start the prior authorization process. This personalized verification saves you time and stress, as we know what each insurer requires.
What are “conservative treatments” that I must try before getting approved?
Insurers require you to try less invasive treatments for at least six months before approving a procedure like Intracept. The goal is to demonstrate that conventional methods have failed to provide lasting relief. A comprehensive conservative care plan typically includes a combination of:
- Physical therapy with a structured exercise plan and a committed home exercise program.
- Medication management using NSAIDs, muscle relaxants, or other pain relievers.
- Targeted injections like epidural or facet joint injections.
- Activity and lifestyle modifications.
- Chiropractic care.
- Sometimes, cognitive behavioral therapy (CBT).
Does coverage differ for Workers’ Compensation or car accident injuries?
Yes. Workers’ Compensation and Motor Vehicle Accident (MVA) insurance may cover the procedure, but their requirements differ from standard health insurance.
For Workers’ Compensation, you must prove your chronic low back pain is a direct result of a work-related injury. This requires specific documentation to establish medical necessity and a causal link. Our team is experienced with these claims.
MVA insurance, like Personal Injury Protection (PIP), may also provide coverage if the pain stems from an accident. This requires establishing a clear link with medical records, proof of failed conservative care, and a physician’s report.
Both scenarios require thorough documentation. Our team will work with you and the insurer to manage the paperwork and support your claim.
Your Path to a Pain-Free Life Starts Here
If you struggle with chronic low back pain, there is hope for lasting relief. The growing acceptance of the intracept procedure covered by insurance is opening doors to a life free from pain.
Major insurers like Anthem, Cigna, and Humana, along with Medicare and TRICARE, now have favorable coverage policies. This signals a fundamental shift in treating chronic back pain. At Center for Specialty Care, we see this expanding coverage changing lives across Minnesota and Iowa. Patients who felt trapped by pain now have a path forward.
This is an exciting time because of the combination of proven clinical results and accessible coverage. Intracept is a unique, minimally invasive treatment that targets the source of vertebrogenic pain.
Our commitment to 100% patient satisfaction means we guide you through every step, from the initial consultation and insurance verification to your procedure and beyond. Our quick appointment availability means we can move swiftly once insurance is approved, minimizing your wait time.
Expert guidance is key. Our experienced team steers insurance requirements and advocates for your coverage. Your chronic back pain doesn’t have to define your future. Advancing technology, growing insurance acceptance, and our personalized care create new opportunities for relief.
The next step is simple: let us evaluate if the Intracept Procedure is your solution. Candidacy requires a thorough assessment of your pain, medical history, and insurance.
Don’t wait. Schedule your consultation to see if the Intracept Procedure is right for you and take the first step toward reclaiming your life from chronic pain.