Am I a Candidate for Intracept? Unpacking the Criteria for This Minimally Invasive Surgery
February 26, 2026
Finding the Best Foot Care Clinic: Services, Scheduling, and What to Expect
March 3, 2026Stepping Up to Foot Tendonitis: Everything You Need to Know
What You Need to Know About Foot and Ankle Tendon Pain
Foot tendonitis is inflammation or irritation of a tendon in your foot or ankle—the thick, flexible cord that connects muscle to bone. When these tendons are overworked, you’ll typically experience pain, swelling, and stiffness that worsens with activity.
Quick Facts About Foot Tendonitis:
- What it is: Inflammation (tendinitis) or degeneration (tendinosis) of foot or ankle tendons
- Common locations: Achilles tendon, posterior tibial tendon, peroneal tendons, extensor tendons, flexor tendons
- Main symptoms: Pain during activity, morning stiffness, tenderness, swelling, weakness
- Primary causes: Overuse, sudden increase in activity, improper footwear, structural foot issues
- Treatment: Rest, ice, compression, elevation (RICE), physical therapy, orthotics, and in some cases, medical intervention
- Recovery time: Mild cases may improve within a month; severe cases can take several months
That nagging ache in your heel or sharp pain along the top of your foot isn’t something to ignore. Tendons are the workhorses of your feet, transmitting force from muscles to bones with every step. When these fibrous bands become inflamed from overuse, simple activities can become painful.
Most cases respond well to conservative treatment when caught early. However, tendinitis can become a chronic problem, which is much harder to treat than an acute injury. Research shows tendon issues are common, with Achilles tendinopathy affecting nearly a quarter of athletes in their lifetime and running-related injuries having a high prevalence.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon with over three decades of experience treating foot and ankle conditions, including all types of foot tendonitis. At the Center for Specialty Care in Fairmont, Minnesota, I’ve helped hundreds of patients in southern Minnesota and northern Iowa recover from tendon injuries using both conservative treatments and minimally invasive surgical techniques when necessary.

Handy foot tendonitis terms:
Understanding the Types and Locations of Foot Tendonitis
Your feet and ankles contain many tendons—strong, flexible tissues connecting muscle to bone—that are vital for movement and balance. When these tendons become inflamed (tendinitis), it causes pain and impacts mobility. The location of your pain is a key clue to which tendon is affected.
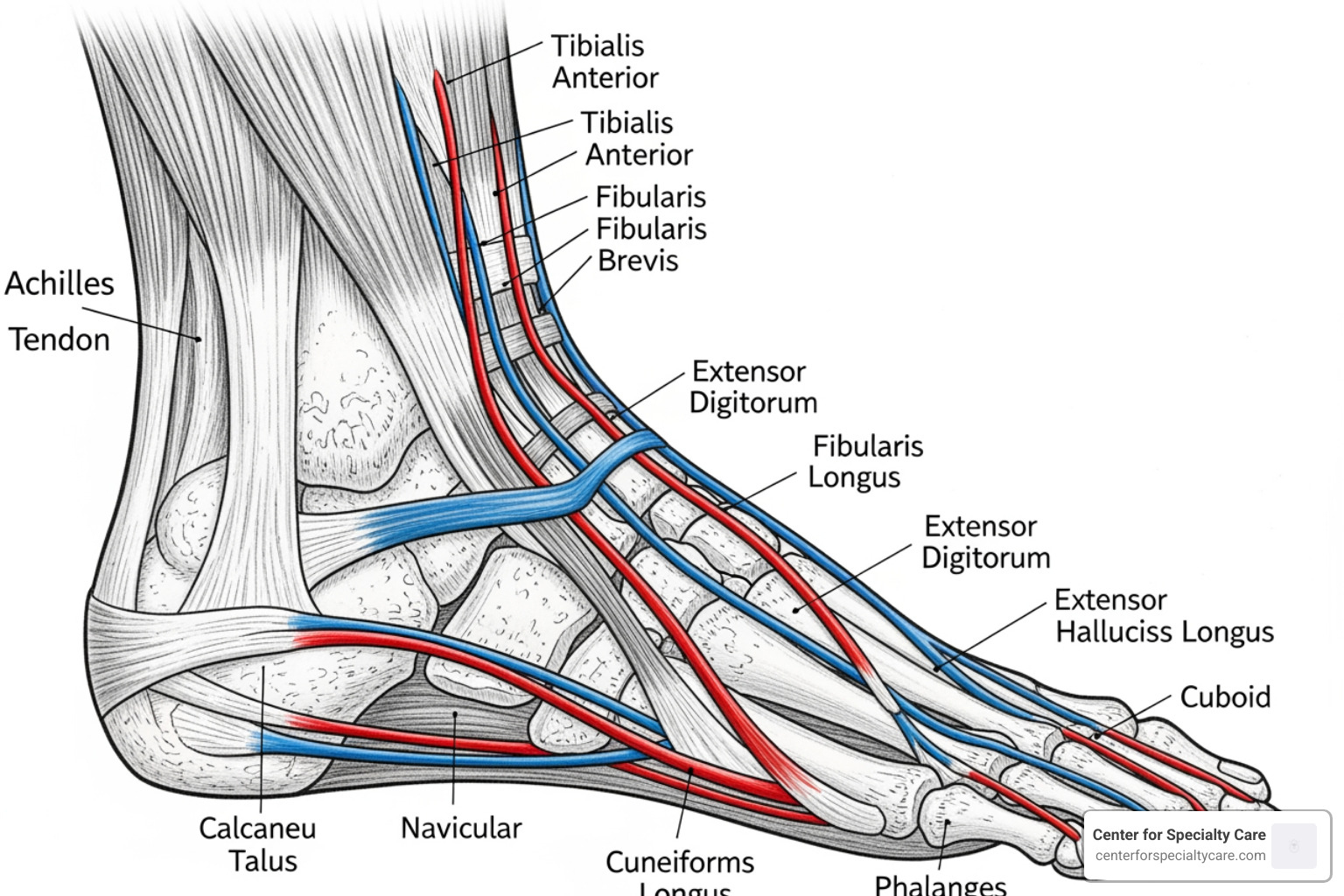
Common Types of Foot Tendonitis
Several tendons in the foot and ankle are particularly susceptible to tendinitis due to the constant stress they endure:
-
Achilles Tendonitis: This common type affects the Achilles tendon, which connects the calf muscles to the heel bone. As the body’s strongest tendon, it’s crucial for walking and running. Pain occurs at the back of the heel and is often caused by overuse or tight calf muscles, making it common in runners. You can learn more about this common condition in our article: More info about Achilles Tendonitis.
-
Posterior Tibial Tendonitis: This affects the tendon supporting your foot’s arch, running along the inside of your ankle. Pain is felt on the inner ankle and arch and is often associated with “flat feet” or overpronation (when the foot rolls inward excessively).
-
Peroneal Tendonitis: The peroneal tendons run along the outside of the ankle, helping to stabilize it. Inflammation causes pain on the outside of the ankle and can be linked to high-arched feet or a history of ankle sprains.
-
Extensor Tendonitis: Located on the top of your foot, these tendons lift your toes. Pain is felt on the top of the foot and can be worsened by tight shoes or repetitive upward flexing of the foot. For more detailed information, see our guide on More info about Extensor Tendonitis.
-
Flexor Tendonitis: Found on the bottom of the foot, these tendons help curl your toes. Pain is often felt under the arch or near the big toe and is common in activities like dancing that require significant toe balancing.
Differentiating Tendonitis from Other Foot Conditions
Foot pain isn’t always foot tendonitis. An accurate diagnosis is crucial, as many conditions have similar symptoms.
| Condition | Primary Location | Common Symptoms | Key Differentiating Factors |
|---|---|---|---|
| Tendonitis | Specific tendon (Achilles, etc.) | Pain, swelling, tenderness, stiffness, often worse with activity | Pain is localized along the tendon path and often develops gradually from overuse. |
| Plantar Fasciitis | Bottom of heel, arch | Sharp, stabbing pain in the heel, especially with first steps in the morning | Pain is worst after rest (like the first steps in the morning) and improves with initial activity. Often linked to tight calf muscles. You can read more about this in our article: Can Plantar Fasciitis Cause Thigh Pain? |
| Heel Spurs | Bottom of heel (bone growth) | Pain in the heel, especially during weight-bearing | Often occurs with plantar fasciitis. The bony growth (spur) itself may not be the source of pain, which comes from inflamed tissue. Detectable on X-ray. Learn more here: Understanding Heel Spurs: An Orthopedic Guide to Symptoms and Treatment |
| Bursitis | Near joints, retrocalcaneal | Localized pain, swelling, warmth, tenderness | Inflammation of a bursa (fluid-filled sac), not a tendon, often from friction or pressure from ill-fitting shoes. |
| Stress Fractures | Bone (e.g., metatarsals, calcaneus) | Deep, aching pain that worsens with activity and improves with rest | Deep, aching pain within the bone from repetitive impact. Diagnosis may require an X-ray or MRI. |
| Nerve Pain | Various (e.g., Morton’s Neuroma) | Burning, tingling, numbness, sharp shooting pain | Follows a nerve path and is often from nerve compression (e.g., Morton’s Neuroma between toes). May lack visible swelling. |
Accurate diagnosis is the first step toward effective treatment. Our team at Center for Specialty Care will conduct a thorough examination and may use diagnostic imaging to pinpoint the exact cause of your foot or ankle pain.
Causes, Risk Factors, and Symptoms
Understanding why foot tendonitis develops is key to both treating and preventing it. The symptoms can range from a mild ache to debilitating pain, often accompanied by stiffness, weakness, and sometimes a grating sensation known as crepitus.
Primary Causes and Risk Factors
Most cases of foot tendonitis stem from a few core issues:
- Overuse and Repetitive Strain: This is the most common culprit. When tendons are subjected to continuous stress without adequate rest, they can become irritated and inflamed, especially from activities with repetitive foot and ankle motions.
- Sudden Increase in Activity: A sudden spike in exercise intensity or duration can overload tendons that haven’t had time to adapt. For example, running-related injuries have a prevalence between 11% and 85%, with tendon issues being a significant part of this.
- Improper Training or Technique: Incorrect form during sports or exercises can place abnormal stress on certain tendons, such as a poor running stride contributing to Achilles tendonitis.
- Trauma or Injury: While less common than overuse, a direct injury like a fall or awkward landing can strain tendons and lead to tendinitis. This is common for athletes who make quick directional changes.
- Age: As we age, our tendons naturally become less flexible and more susceptible to injury.
For a deeper dive into the scientific understanding of tendon issues, you can explore resources like this Scientific research on Achilles Tendinopathy.
Contributing Structural and Health Factors
Beyond activity-related causes, certain inherent factors can increase your susceptibility to foot tendonitis:
- Structural Foot Issues:
- Flat Feet (Overpronation): If your feet roll inward excessively, it can cause uneven strain on tendons like the posterior tibial and Achilles tendons. Our practitioners evaluate hip strength and ankle mobility to address overpronation.
- High Arches: High arches can also predispose you to certain types of tendinitis, such as peroneal tendinitis, due to altered biomechanics.
- Tight Calf Muscles: This can put increased tension on the Achilles tendon, making it more vulnerable to inflammation.
- Arthritis: Inflammatory conditions like rheumatoid arthritis (RA) or gout can cause inflammation in and around tendons.
- Diabetes: Metabolic diseases like diabetes can affect the structure and strength of collagen in tendons, increasing risk.
- Obesity: Excess weight places additional stress on the tendons in your feet and ankles.
- Cold Weather Impact: Cold weather can worsen tendinitis symptoms. It stiffens tendons and reduces blood flow, making them less flexible and more prone to strain. To protect yourself, warm up thoroughly, wear warm and supportive footwear, and consider staying active indoors during harsh weather.
Many of these contributing factors are discussed in our guide on More info about common foot problems.
Diagnosis and Treatment Options for Foot Tendonitis
If you have persistent foot or ankle pain that you suspect is foot tendonitis, seeking professional medical advice is crucial. Early diagnosis can prevent the condition from becoming chronic.
When you visit us at Center for Specialty Care, our specialists will begin with a physical examination. We’ll ask about your symptoms and medical history, then check for tenderness, swelling, and range of motion. We may ask you to perform certain movements to assess the affected tendon.
To confirm the diagnosis and rule out other conditions, we may order diagnostic imaging tests:
- X-rays: These can help identify bone spurs or rule out stress fractures and arthritis.
- Ultrasound: This technique provides a good view of the tendon, showing inflammation, thickening, or tears.
- MRI (Magnetic Resonance Imaging): An MRI offers a detailed view of soft tissues and bones, providing comprehensive information on tendon damage.
At-Home Management for Foot Tendonitis
For mild cases, several home care strategies can help reduce pain and inflammation:
- R.I.C.E. Method:
- Rest: Stop any activity that causes pain. Staying off your foot is key.
- Ice: Apply ice packs to the area for 15-20 minutes, several times a day, to reduce swelling.
- Compression: Use a compression bandage to help minimize swelling.
- Elevation: Lift your foot above your heart to help reduce swelling.
- Over-the-Counter (OTC) NSAIDs: Drugs like ibuprofen or naproxen can help manage pain and inflammation.
- Activity Modification: Switch to low-impact exercises to avoid aggravating the tendon.
- Gentle Stretching: Once acute pain subsides, gentle stretches can help maintain flexibility.
- Heat Therapy: While ice is best for acute inflammation, heat can be beneficial for persistent aches. You can find more information on this in our article: Does Heat Help Tendonitis? Answers & Tips for Effective Relief.
Professional Medical Interventions
If home care isn’t enough, our specialists can offer a range of professional interventions:
- Physical Therapy: This is a cornerstone of treatment. A therapist will design a personalized program of stretching and strengthening. Eccentric loading exercises are highly effective for many types of tendinitis and can significantly reduce pain.
- Custom Orthotics and Supportive Footwear: We may recommend custom orthotics to correct biomechanical imbalances and reduce stress on the tendon. Proper footwear is also vital.
- Immobilization: In some cases, a walking boot, brace, or soft cast may be used to immobilize the foot and allow the tendon to heal.
- Corticosteroid Injections: These can provide temporary pain relief, but we use them cautiously as they can weaken the tendon over time, increasing the risk of rupture.
- Advanced Treatments:
- Extracorporeal Pulse Activation Therapy (EPAT) / Shockwave Therapy (ESWT): This non-invasive treatment uses acoustic waves to stimulate healing. For Achilles tendinopathy, ESWT can reduce pain by 60% and has high patient satisfaction.
- Iontophoresis: This uses a mild electrical current to deliver anti-inflammatory medication through the skin.
- Ultrasound or Laser Therapy: These can also be used to decrease inflammation and promote healing.
- Surgical Options: Surgery is a last resort for chronic cases that haven’t responded to at least 6 months of conservative treatment or for severe tears. For more general information, consult resources from the American Podiatric Medical Association. Our dedicated Podiatry services offer comprehensive care, from diagnosis to advanced treatment.
Recovery and Prevention Strategies
Recovering from foot tendonitis and preventing its recurrence involves careful rehabilitation and adopting practices that support long-term tendon health.
Healing Timeline and Exercise During Recovery
Healing time for foot tendonitis varies. Mild cases may improve within a month with consistent treatment, while severe or chronic cases can take several months. Chronic tendinitis is much harder to treat than an acute injury, making early intervention key.
Regarding exercise, the general rule is to listen to your body and avoid activities that cause pain.
- Low-impact activities like swimming, cycling, or using an elliptical are often safe and maintain fitness without stressing the tendon.
- High-impact activities like running and jumping should be avoided until your tendon has fully healed.
- Gradual Return to Activity: Once your pain subsides, we will guide you through a gradual return to your normal activities, slowly increasing intensity and duration to allow your tendons to adapt.
Preventing Future Flare-Ups
Prevention is always better than cure. These strategies can significantly reduce your risk of recurrence:
- Proper Warm-up and Cool-down: Always warm up before exercise and cool down with stretches afterward to prepare your tendons for activity and help them recover.
- Strengthening Exercises: Focus on strengthening the muscles that support your foot and ankle, especially your calves, to reduce the burden on your tendons.
- Flexibility Training: Regular stretching of your calf muscles and tendons improves elasticity and makes them less prone to injury.
- Gradual Progression of Exercise Intensity: Avoid sudden increases in activity. Increase workout intensity or duration by no more than 10% per week.
- Maintaining a Healthy Weight: Excess body weight puts additional strain on your foot and ankle tendons.
The Role of Footwear and Orthotics
Your choice of footwear and the use of orthotics play a critical role in preventing foot tendonitis:
- Supportive Shoes: Wear shoes that provide adequate support and cushioning for your foot type and activity.
- Proper Fit: Ill-fitting shoes can cause friction and abnormal pressure. Ensure your shoes fit well with enough room in the toe box.
- Cushioning: Good cushioning absorbs impact, protecting your tendons from excessive forces.
- Avoiding Worn-Out Shoes: Replace athletic shoes regularly (typically every 300-500 miles for runners) as their support degrades over time.
- Custom Orthotics: For those with structural issues like flat feet or high arches, custom orthotics are highly effective. Molded to your feet, these prescription devices provide personalized support, correct biomechanical imbalances, and reduce stress on tendons to help prevent recurrence.
- Over-the-Counter Orthotics: While not as precise, OTC inserts can offer some support for milder issues. For persistent problems, custom options are often more effective.
For more detailed information on how orthotics can help, you can visit Orthotics information.
Frequently Asked Questions about Foot Tendonitis
We often hear many questions from our patients about foot tendonitis. Here are some of the most common ones:
How long does it take for foot tendonitis to heal?
The healing time for foot tendonitis is highly variable.
- Mild cases: May heal within a month with proper rest and care.
- Severe or chronic cases: Can take several months (up to six or longer), especially if degeneration (tendinosis) has occurred. Chronic issues take longer to heal than acute ones.
Consistency with physical therapy, supportive footwear, and avoiding aggravating activities are crucial for a faster recovery.
Can I still exercise with foot tendonitis?
This depends on the severity of your pain and the type of activity.
- Listen to Your Body: The most important rule is to avoid any activity that causes or increases your pain. Pain is your body’s signal to rest.
- Low-Impact Alternatives: Many people can switch to low-impact activities that don’t stress the affected tendon, such as swimming, cycling, or using an elliptical machine.
- Consult a Professional: We highly recommend consulting with our specialists or a physical therapist. They can identify safe exercises and guide your gradual return to regular activities. Pushing through pain can worsen the injury.
When should I see a podiatrist for my foot pain?
It’s always a good idea to seek professional medical advice for persistent foot or ankle pain. Here are clear indicators that it’s time to schedule an appointment at Center for Specialty Care:
- Pain Persists Beyond a Week: If your pain doesn’t improve with a few days of rest and ice, it’s time for an evaluation.
- Severe Pain Interfering with Walking: If the pain is so intense that it makes walking difficult, you should see a doctor promptly.
- Sudden ‘Pop’ or Tearing Sensation: This could indicate a tendon rupture, which requires immediate medical attention.
- Numbness or Tingling: These symptoms might suggest nerve involvement, which needs professional assessment.
- Signs of Infection: If you notice redness, warmth, or significant swelling, seek immediate medical care.
Don’t wait! Tendinitis can become a chronic problem, and it’s much harder to treat chronic problems than acute injuries. Early intervention makes a significant difference.
Take the Next Step Towards Pain-Free Feet
Foot tendonitis can be debilitating, but it is treatable. Understanding the causes, symptoms, and treatments is the first step toward recovery. The key is to listen to your body, use proper footwear, and seek professional help when needed. Early diagnosis is crucial to prevent the condition from becoming a chronic problem.
At Center for Specialty Care in Fairmont, Minnesota, we provide comprehensive, personalized care for all types of foot and ankle pain, including foot tendonitis. Our team serves patients across southern Minnesota and northern Iowa, and we are committed to your satisfaction and a quick, effective recovery.
Don’t let foot pain hold you back any longer. Take control of your foot health and step towards a pain-free future. Contact our Orthopedics team for a consultation today.




