Your Shoulder’s Best Friend: Choosing an Orthopedic Specialist
March 6, 2026
The Warm Truth: Is Heat Your Tendonitis’ Best Friend?
March 10, 2026Ablation for Back Pain: A Comprehensive Overview
Why Ablation on Back Matters for Chronic Pain Sufferers
Ablation on back is a minimally invasive procedure that uses thermal energy to disrupt nerves transmitting pain signals from the spine to the brain. If chronic lower back pain hasn’t responded to physical therapy or medication, this treatment offers a path to significant relief.
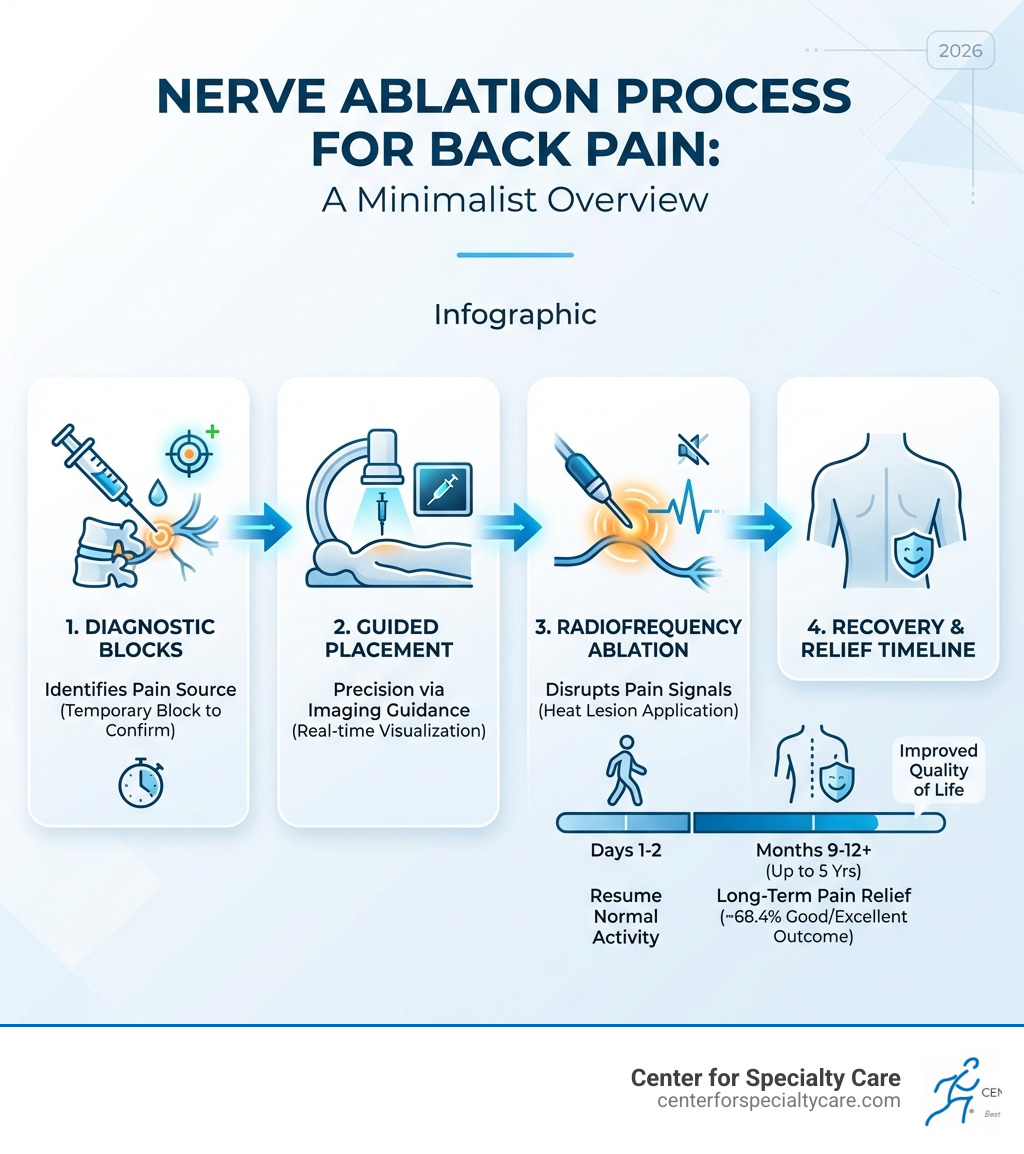
Quick Overview:
- What it is: A procedure disrupting pain signals by targeting specific spinal nerves.
- Common types: Radiofrequency ablation (facet joints) and basivertebral nerve ablation (vertebral endplates).
- Success rate: Approximately 68.4% of patients report good to excellent relief.
- Duration: Typically 9-12 months, with some benefits lasting up to 5 years.
- Recovery: Most patients resume normal activities within 1-2 days.
- Ideal for: Those with chronic pain (6+ months) resistant to conservative care.
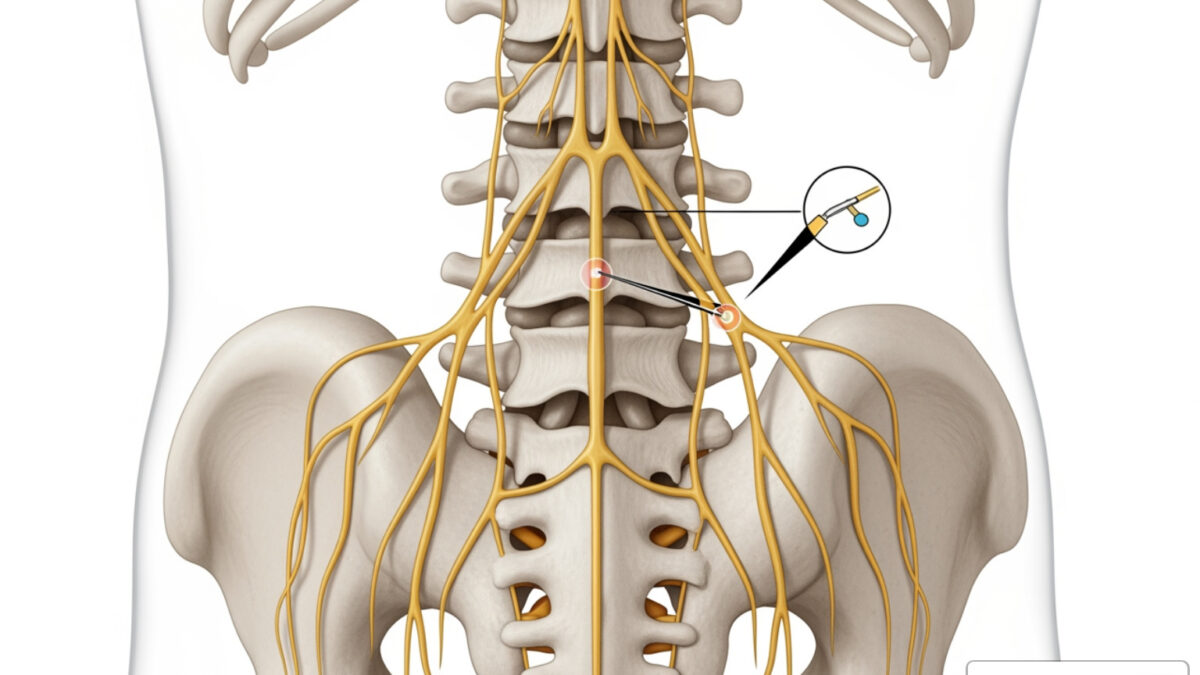
Nerve ablation targets the source of pain signals rather than masking symptoms. By creating a small heat lesion on the nerve, the “phone line” to the brain is cut, reducing pain without fixing the underlying structural condition like arthritis.
It is also important to know what ablation doesn’t do. It does not replace strengthening, mobility work, posture improvements, or other long-term spine health strategies. Instead, it can reduce pain enough to help you move more comfortably, participate in therapy, sleep better, and return to normal routines. Many patients find that when pain is quieter, they can finally make progress with walking programs, core stabilization, weight management, and other steps that support long-term function.
Two main types of ablation are used:
- Radiofrequency ablation (RFA): Targets medial branch nerves for arthritis-related facet joint pain.
- Basivertebral nerve ablation: Targets nerves inside vertebral bodies for vertebrogenic pain (visible as Modic changes on MRI).
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon with over 30 years of experience. At the Center for Specialty Care, I’ve helped hundreds of patients regain their quality of life through ablation on back procedures.
Easy ablation on back glossary:
If you are considering ablation, the biggest first step is an accurate diagnosis. “Low back pain” can come from facet joints, sacroiliac joints, vertebral endplates, discs, muscles, or compressed nerves. The goal of your consultation is to match your symptoms and imaging to a specific pain generator so the treatment is targeted and worthwhile.
Understanding Ablation on Back Procedures
Ablation on back refers to medical procedures that alleviate chronic pain by intentionally disrupting nerve function. This “turns off” pain signals sent to the brain, improving quality of life when structural repairs aren’t the primary goal.
How Nerve Ablation Works
The procedure uses thermal energy (heat or cold) to create a small lesion on the nerve tissue, a process known as coagulation necrosis. This breaks the circuit for nociceptive (pain) signals. We specifically target sensory nerves while preserving motor nerves to ensure pain relief without loss of muscle function.
Nerve ablation is minimally invasive, performed via a hollow needle guided by fluoroscopy or ultrasound. This precision makes it a valuable alternative when conservative treatments like medication or physical therapy fail. For more details, explore scientific research on nerve ablation mechanisms.
Primary Technologies and Types of Nerve Ablation
At the Center for Specialty Care, we primarily use Radiofrequency Ablation (RFA) and Basivertebral Nerve Ablation (BVNA) to address chronic spinal pain.
Radiofrequency Ablation (RFA)
RFA uses radio waves to generate heat (70-80°C), destroying small areas of nerve tissue to block pain signals. It is a mainstay for:
- Facet Joints: Targeting medial branch nerves to treat spinal arthritis.
- Sacroiliac Joints: Targeting lateral branch nerves for pain where the spine meets the sacroiliac joints.
Learn more about How Radiofrequency Ablation Can Help Back Pain.
Basivertebral Nerve Ablation (Intracept Procedure)
BVNA addresses vertebrogenic pain originating from damaged vertebral endplates. A key indicator is the presence of Modic changes on an MRI. By ablating the basivertebral nerve within the vertebral body, we block pain signals from these endplates. Read more at Basivertebral Nerve Ablation for Lower Back Pain.
| Feature | Radiofrequency Ablation (RFA) | Basivertebral Nerve Ablation (BVNA) |
|---|---|---|
| Target Nerves | Medial/Lateral branch nerves | Basivertebral nerve |
| Pain Source | Facet or SI joint arthritis | Vertebrogenic (endplate) pain |
| Diagnostic Aid | Diagnostic nerve blocks | Modic changes on MRI |
| Common Use | Chronic low back/neck pain | Chronic axial low back pain |
| Brand Name | N/A | Intracept® |
Identifying the Ideal Candidate for Treatment
Good candidates for ablation on back typically meet these criteria:
- Chronic Pain: Persistent back pain for at least six months.
- Failed Conservative Care: No relief from physical therapy, medications, or epidural steroid injections.
- Localized Pain: Pain is pinpointed to a specific area rather than generalized.
- Positive Diagnostic Blocks: Temporary relief from a local anesthetic injection confirms the target nerve is the pain source.
Specific Conditions and Exclusions
- RFA is ideal for facet joint arthritis and sacroiliac joint pain.
- BVNA is specifically for vertebrogenic pain with Modic Type 1 or 2 changes on MRI.
Exclusions: Ablation may not be suitable for those with active infections, pregnancy, bleeding disorders, or pain primarily caused by disc herniation (sciatica) or spinal stenosis. A study suggests about 3% of spine clinic patients are candidates for BVNA; see the scientific research on candidate prevalence.
Our team evaluates your history and imaging to ensure functional improvement. If you’re in Fairmont MN, Estherville IA, Buffalo Center IA, or St. James MN, we can help determine if this is right for you.
The Procedure: Preparation, Diagnostic Blocks, and Recovery
Preparation
Before your ablation on back, we review your medications. Blood thinners like aspirin or warfarin must usually be stopped 5-6 days prior. You will fast for 6-8 hours if receiving sedation and should arrange for a driver to take you home.
Diagnostic Nerve Blocks
This “test drive” involves injecting a local anesthetic near the target nerve under fluoroscopy. If you experience significant temporary relief, it confirms the nerve is the pain generator, ensuring a higher success rate for the permanent ablation.
The Procedure Experience
Performed outpatient, the procedure takes less than an hour.
- Numbing: Local anesthetic is applied to the skin.
- Guidance: A needle is guided to the nerve using real-time X-ray (fluoroscopy).
- Stimulation (RFA): A brief test ensures the needle is away from motor nerves.
- Ablation: Radiofrequency energy creates the lesion (60-90 seconds). You may feel warmth or pressure.
Recovery
Most patients resume light activities within 1-2 days. Mild soreness at the site is normal and manageable with ice or OTC pain relievers. Full relief typically develops over 1-6 weeks as inflammation subsides. Maximum BVNA benefits are often reached at 3-6 months.
Success Rates and Long-Term Clinical Outcomes
Ablation on back offers encouraging results for chronic sufferers:
- Effectiveness: Studies show 68.4% of RFA patients achieve good to excellent relief. For BVNA, over half experience significant improvement, with 35% reporting complete resolution.
- Duration: RFA relief typically lasts 9-12 months. BVNA offers remarkable longevity, with 50-70% of patients maintaining relief for 2 years, and some up to 5 years. See the scientific research on 5-year outcomes.
Long-Term Benefits:
- Improved Function: Patients return to walking, exercising, and daily tasks.
- Reduced Medication: Significant decrease in opioid use is common, especially after BVNA.
- Repeatability: Nerves can regenerate, but both RFA and BVNA can be safely repeated if pain returns, providing a sustainable long-term management strategy.
Frequently Asked Questions about Back Ablation
How long does the pain relief from back ablation last?
Relief from RFA usually lasts 9 to 12 months. BVNA for vertebrogenic pain often lasts much longer, with studies showing efficacy for 2 to 5 years. While not permanent, this window allows for physical therapy and core strengthening to further support the back.
Is the nerve ablation procedure painful?
Most patients find the procedure comfortable. We use local anesthetics and often mild IV sedation. You may feel a brief tingling during nerve stimulation or warmth during the ablation, but significant pain is rare. Post-procedure soreness is similar to a sunburn and fades quickly.
How often can I repeat a nerve ablation treatment?
Procedures can be repeated if the initial treatment was successful and pain returns due to nerve regeneration. The typical interval for RFA is at least six months. Your specialist will use diagnostic blocks to confirm the nerve is still the pain source before repeating the treatment.
What is the difference between RFA and an epidural steroid injection?
They work in different ways and are used for different pain patterns. RFA is designed to reduce pain coming from specific joints (such as facet joints or the sacroiliac joint) by interrupting the nerve signals from those structures. Epidural steroid injections are typically used to calm inflammation around irritated spinal nerves and are more often considered when leg pain or nerve-related symptoms are present. Your provider will recommend the option that best matches your diagnosis, exam findings, and imaging.
Will ablation on back help sciatica?
In many cases, ablation is not the best match for classic sciatica because sciatica is usually caused by irritation or compression of a spinal nerve root (often from a disc herniation or spinal stenosis). RFA is commonly used for facet or sacroiliac joint pain, and basivertebral nerve ablation is used for vertebrogenic pain with Modic changes on MRI. If your main symptoms include pain traveling down the leg, numbness, or weakness, your evaluation will focus on identifying and treating the nerve root source.
What should I do after the procedure to get the best result?
Plan on a short period of relative rest, then a gradual return to normal activity as advised. Most patients do best when pain relief is paired with a long-term plan such as guided physical therapy, a home exercise program, and core and hip strengthening. Good outcomes are not only about less pain, but also about improving walking tolerance, daily function, and confidence with movement.
What are common side effects and when should I call the clinic?
Temporary soreness at the needle sites, a bruised feeling, or a short flare of pain can happen and usually improves over several days. Rarely, patients may develop signs that need prompt medical attention, such as fever, increasing redness or drainage at the injection site, new or worsening weakness, or severe symptoms that do not improve. Your care team will provide written post-procedure instructions custom to your medications and health history.
Conclusion
Chronic back pain doesn’t have to be permanent. Advanced ablation on back procedures offer a minimally invasive way to block pain signals and restore your lifestyle. At the Center for Specialty Care, led by Dr. Corey Welchlin, we provide expert orthopedic care with a focus on 100% patient satisfaction.
Serving Fairmont MN, Estherville IA, Buffalo Center IA, and St. James MN, we offer quick appointment availability to help you start your recovery journey. Whether you face facet joint arthritis or vertebrogenic pain, our personalized approach ensures you receive the most effective treatment. Contact us today to schedule your consultation and take the first step toward a life with less pain.