Ablation for Back Pain: A Comprehensive Overview
March 7, 2026
The Fairmont Guide to Expert Foot and Ankle Care
March 11, 2026The Warm Truth: Is Heat Your Tendonitis’ Best Friend?
When Tendon Pain Strikes: Understanding Your Treatment Options
Is heat good for tendonitis depends entirely on whether your injury is acute or chronic. Here’s what you need to know:
- For acute tendonitis (first 48-72 hours): Use ice to reduce swelling and inflammation
- For chronic tendon pain (after 72 hours): Use heat to relieve stiffness and increase blood flow
- Never use heat on fresh injuries or when swelling is present
If you’re dealing with tendon pain, you’ve probably received conflicting advice. One friend swears by ice packs. Another insists heat is the answer. Your online search yields equally mixed results.
The confusion is understandable. Tendon pain—whether it’s in your shoulder, elbow, wrist, knee, or heel—can stem from either acute inflammation or chronic degeneration. Each requires a different approach.
The key is timing. Ice works best immediately after injury when inflammation peaks. Heat becomes your ally once that initial swelling subsides and stiffness sets in.
I’m Dr. Corey Welchlin, and over three decades of orthopedic practice in Fairmont, Minnesota, I’ve guided countless patients through this exact question: is heat good for tendonitis in their specific situation? At the Center for Specialty Care, we emphasize proper diagnosis first, then match the treatment to the injury stage.
Quick Is heat good for tendonitis terms:
Understanding Tendonitis: The Source of Your Pain
Before we dive into the nitty-gritty of hot and cold, let’s get acquainted with the star of our show: the tendon.
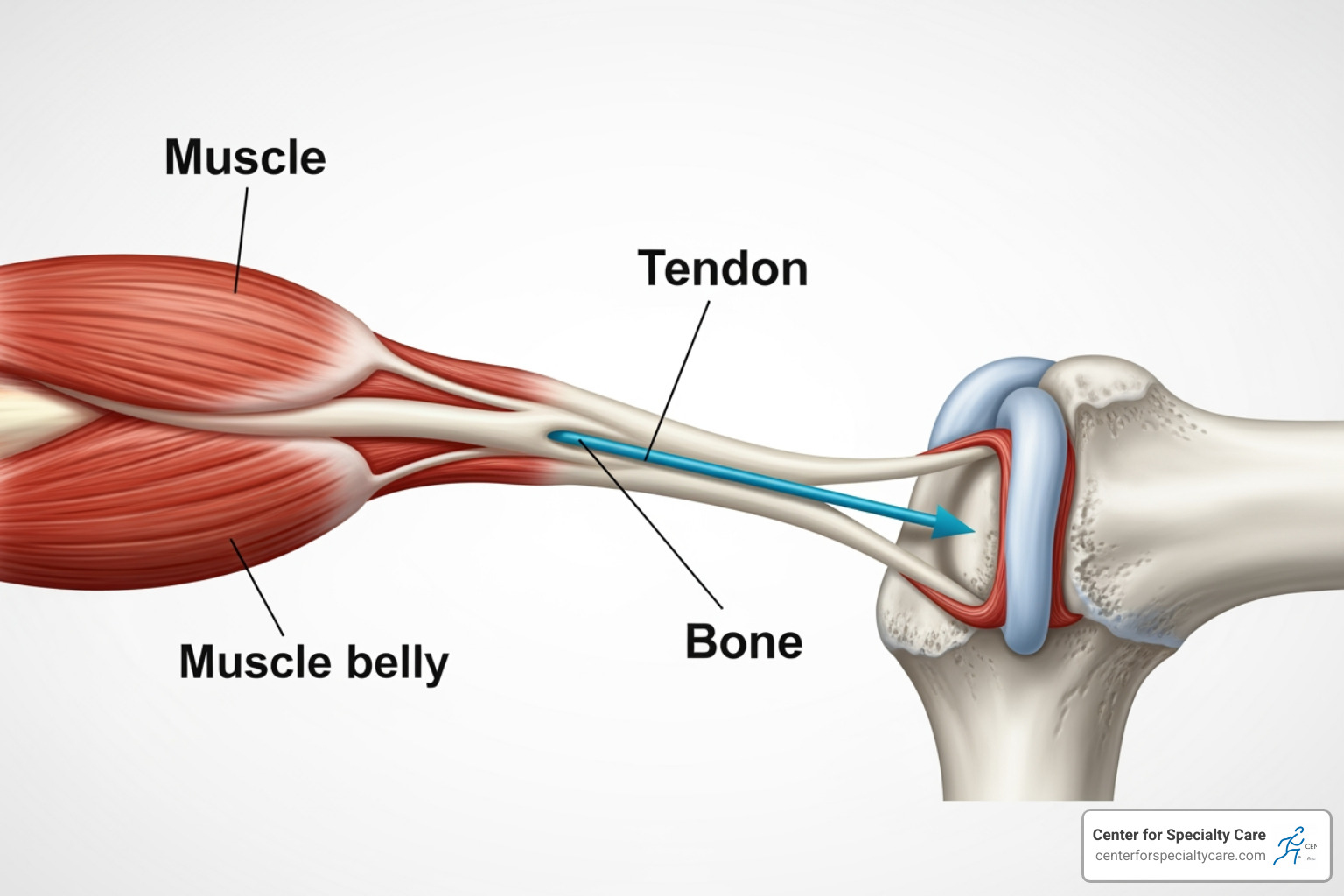
What is a Tendon?
Imagine a strong, fibrous rope connecting a powerful engine to a movable lever. In our bodies, that rope is a tendon. Tendons are tough bands of fibrous connective tissue that link your muscles to your bones. They’re essential for movement, allowing you to walk, lift, jump, and perform all sorts of daily activities. Without these unsung heroes, your muscles wouldn’t be able to pull on your bones, and you’d be stuck!
What is Tendonitis?
The suffix “-itis” usually means inflammation. So, tendonitis, simply put, is when a tendon becomes inflamed or irritated. This inflammation can cause joint pain and stiffness, making movement difficult and uncomfortable. It’s often an acute condition, meaning it comes on suddenly, usually after an injury or a period of overuse.
Common Causes of Tendonitis
Tendonitis doesn’t just appear out of nowhere. It’s typically the result of your body telling you it’s had enough! Some common culprits include:
- Repetitive Motion or Overuse: This is perhaps the most frequent cause. Think of activities that involve the same movement over and over, like swinging a tennis racket, typing for hours, or even shoveling snow. Your tendons can only handle so much before they start to protest.
- Sudden Injury or Trauma: A fall, an unexpected twist, or a direct impact can also irritate a tendon, leading to inflammation.
- Overloading the Joint: Pushing your body beyond its current capacity, such as lifting something too heavy or increasing your workout intensity too quickly, can strain tendons.
- Poor Posture or Technique: Incorrect body mechanics during sports, work, or daily tasks can place undue stress on certain tendons.
- Aging: As we age, our tendons can become less elastic and more prone to injury.
- Certain Medications: In some cases, specific medications can contribute to tendon problems.
Common Symptoms of Tendonitis
When a tendon is inflamed, it sends clear signals. You might experience:
- Pain with Movement: This is usually the most prominent symptom. The pain often worsens when you use the affected joint or muscle.
- Stiffness or Tightness: The joint connected to the inflamed tendon might feel stiff, especially after periods of rest, like first thing in the morning.
- Mild Swelling: The affected area might appear slightly swollen, sometimes accompanied by warmth or redness.
- Soreness or Tenderness: The tendon itself might be sore to the touch.
- Grating or Crackling Sensation: In some cases, you might feel or hear a grating or crackling sound when moving the tendon.
Common Locations for Tendonitis
Tendonitis can strike almost any tendon in your body, but some areas are more commonly affected due to their frequent use and susceptibility to repetitive strain. These include:
- Shoulder: Often referred to as rotator cuff tendonitis, causing pain with overhead movements.
- Elbow: Famous examples include “tennis elbow” (lateral epicondylitis) and “golfer’s elbow” (medial epicondylitis).
- Wrist: Common in activities requiring repetitive hand movements, such as typing or crafting.
- Knee: Patellar tendonitis, also known as “jumper’s knee,” is common in athletes.
- Heel: Achilles tendonitis affects the large tendon connecting your calf muscles to your heel bone.
Understanding these basics is the first step toward finding the right relief. Now, let’s tackle the age-old question: ice or heat?
The Great Debate: Is Heat Good for Tendonitis or Should You Use Ice?
This is where the confusion often lies, but the answer isn’t as complicated as it seems. It all boils down to the stage of your injury. Think of it like a fire: you wouldn’t pour oil on a raging blaze, and you wouldn’t use a fire hose to warm up a chilly room.
The Cold Truth: When to Use Ice Therapy
When you first injure a tendon, or when an existing tendon issue flares up suddenly, your body’s natural response is inflammation. This involves increased blood flow to the area, leading to swelling, redness, and pain. In this acute phase, ice is your best friend.
- Ice for Acute Injuries: We recommend using ice immediately after a sudden injury to a tendon or during the first 48-72 hours of a flare-up. This is when inflammation is at its peak.
- First 48-72 Hours: This critical window is where ice shines. It helps to control the initial inflammatory response.
- Vasoconstriction and Reduced Blood Flow: Ice works by causing the blood vessels in the affected area to constrict. This reduces blood flow, which in turn limits swelling and inflammation.
- Decreased Swelling and Numbing Effect: By reducing swelling, ice helps alleviate pressure on nerve endings, thus decreasing pain. It also acts as a natural numbing agent, effectively dulling the intensity of pain signals.
- Pain Relief: The combination of reduced swelling and numbing makes ice incredibly effective for short-term pain relief.
Best Practices for Icing: Our Cool Tips for Safe Application
To get the most out out of ice therapy and avoid any frosty mishaps, follow these guidelines:
- Wrap in a Towel: Never apply ice directly to your skin. Always use a towel or cloth as a barrier to prevent ice burns or frostbite. A bag of frozen vegetables, like peas, can also work well as it conforms to the body.
- 15-20 Minute Sessions: Apply ice for 15 to 20 minutes at a time. Any longer, and you risk damaging your skin or underlying tissues.
- Lift the Area: If possible, lift the injured area above your heart while icing. This further helps to reduce swelling.
- Allow Warm-Up Time: After an icing session, allow at least 30 minutes for the skin and tissue to return to normal temperature before reapplying. We suggest repeating every 4-6 hours initially, or every 2-3 hours for more severe acute pain.
- Move the Ice Around: If you’re using a solid ice pack, gently move it around to prevent prolonged contact with one spot, which can lead to frostbite.
- Listen to Your Body: If the area becomes numb or uncomfortably cold before 15 minutes, remove the ice.
Ice is a helpful solution for controlling pain and swelling, but it does not speed up healing. It simply creates a better environment for healing to begin by managing the initial inflammatory response.
When Is Heat Good for Tendonitis? The Chronic Pain Solution
Once the initial acute inflammation and swelling have subsided—typically after the first 72 hours—or if you’re dealing with persistent stiffness and aching from a long-standing issue, that’s when heat becomes your therapeutic partner. So, is heat good for tendonitis when it’s chronic? Absolutely!
- Heat for Chronic Pain and Stiffness: Heat therapy is particularly beneficial for chronic tendon pain, often referred to as tendinopathy or tendinosis. It’s also great for loosening up stiff tendons before physical activity or stretching.
- After 72 Hours: Generally, we advise waiting at least 72 hours after an acute injury before introducing heat. Applying heat too early can exacerbate inflammation and swelling.
- Vasodilation and Increased Blood Flow: Unlike ice, heat causes blood vessels to dilate (widen). This increases blood circulation to the affected area, bringing in vital nutrients and oxygen, and helping to flush away metabolic waste products. This increased blood flow aids in the healing process of chronic tendon issues.
- Muscle Relaxation and Improved Flexibility: Heat helps to relax tight muscles and tendons, reducing tension and stiffness. This improved flexibility can improve your range of motion and make movements less painful. Research shows that heat is beneficial in increasing muscle and ligament flexibility, reducing the force needed to flex the knee by about 25% compared to cold application. It even increases the extensibility of ligaments like the anterior and posterior cruciate ligaments.
- Pain Relief: The warmth and relaxation provided by heat can also offer significant pain relief, making it easier to move and perform daily activities.
Best Practices for Heating: Our Warm Hugs for Safe Application
To safely and effectively use heat therapy, keep these points in mind:
- Moist Heat is Often Best: Moist heat, such as a warm compress or a warm bath, can penetrate deeper and be more effective than dry heat. However, heating pads, hot water bottles, or heat wraps are also excellent options.
- 15-20 Minute Sessions: Apply heat for 15 to 20 minutes at a time. While heat can be applied for longer than ice, always monitor your skin carefully.
- Protect the Skin: Always use a barrier, like a towel, between your skin and a heating pad or hot water bottle to prevent burns. Ensure the heat is comfortably warm, not painfully hot.
- Never Fall Asleep with Heat: We can’t stress this enough: never fall asleep with a heating pad on, as this can lead to severe burns.
- Consider Warm Baths or Saunas: For broader relief of stiffness, especially in areas like the back or shoulders, a warm bath can be wonderfully relaxing. Infrared saunas can also improve circulation and relieve soreness, offering a comfortable experience.
- Before Activity: Heat is particularly beneficial before gentle stretching or rehabilitative exercises, as it helps prepare the muscles and tendons for movement.
By understanding when to use ice and when to use heat, you’re already taking a huge step towards effective tendon pain management.
Tendonitis vs. Tendinosis: Why the Diagnosis Changes Everything
Here’s a little secret: many conditions commonly called “tendonitis” are actually something else entirely, especially if they’ve been bothering you for a while. This distinction is crucial because it dictates whether ice or heat, or indeed other treatments, will be most effective.

The “-itis” vs. “-osis” Difference
While often used interchangeably, “tendonitis” and “tendinosis” are two distinct conditions with different underlying pathologies:
- Tendonitis (Acute): As we’ve discussed, tendonitis implies inflammation or irritation of the tendon. It’s an acute condition, typically characterized by sudden onset, swelling, redness, and tenderness. This is your body’s initial response to injury.
- Tendinosis (Chronic): This is a “completely different beast,” as one research source puts it. Tendinosis (sometimes called tendinopathy) is a chronic degenerative condition where the collagen fibers within the tendon break down. Instead of inflammation, you’re dealing with actual structural changes in the tendon tissue. It develops slowly over weeks, months, or even years, often due to repetitive actions over time. There’s typically no significant swelling, just persistent aching and stiffness. When short-term tendonitis goes untreated, it can develop into tendinosis.
Why Common Terms Like “Tennis Elbow” Are Often Misdiagnosed
You’ve probably heard of “tennis elbow” or “swimmer’s shoulder.” Interestingly, these well-known conditions are often incorrectly labeled as tendonitis. In many cases, especially if they’ve been chronic, they are actually forms of tendinosis. This distinction matters because a treatment approach focused solely on reducing inflammation (like extended icing) won’t be effective for a condition that is primarily degenerative.
Here’s a quick comparison to help clarify:
| Feature | Acute Tendonitis | Chronic Tendinosis |
|---|---|---|
| Onset | Sudden (acute) | Slow, gradual (weeks, months, years) |
| Primary Issue | Inflammation, irritation | Degeneration, breakdown of collagen fibers |
| Swelling | Typically present | Typically no significant swelling |
| Symptoms | Soreness, pain, worsens with movement, redness, warmth | Persistent aching, stiffness, restricted movement, tender lump formation |
| Treatment Focus | Reduce inflammation, pain relief | Promote healing, increase blood flow, improve flexibility, rebuild collagen |
| Temp. Therapy | Ice (first 48-72 hours) | Heat |
Understanding this difference empowers you to seek the right treatment. If your pain has been lingering for weeks or months, and stiffness is your main complaint, the question is heat good for tendonitis (or rather, tendinosis) becomes a resounding yes!
Beyond Heat and Ice: A Holistic Approach to Tendon Recovery
While ice and heat are powerful tools in your recovery arsenal, they are often just one part of a comprehensive strategy for overcoming tendon pain. At Center for Specialty Care, we believe in a holistic approach that supports your body’s natural healing processes.
Rest and Activity Modification
One of the most fundamental steps in tendon recovery is giving the affected tendon a break. This doesn’t necessarily mean complete immobilization, which can lead to muscle atrophy and deconditioning. Instead, we advocate for relative rest and activity modification. This means:
- Reducing activities that aggravate your tendon.
- Modifying movements to minimize stress on the injured area.
- For acute tendonitis, resting the affected tendon for 2 to 3 days can significantly aid initial recovery.
- Avoiding heavy lifting, strong gripping, or twisting actions that worsen symptoms.
Contrast Therapy: Alternating Hot and Cold
Sometimes, you don’t have to choose between ice and heat. Contrast therapy, which involves alternating between hot and cold applications, can be beneficial, especially for chronic conditions with occasional flare-ups or when transitioning from the acute to the recovery phase.
- This method helps to stimulate circulation, promoting blood flow while also reducing stiffness.
- One common method is contrast baths, where you alternate immersing the affected area in warm water for 3-4 minutes, followed by cold water for 1 minute, repeating for 20-30 minutes.
- For guidance on the best approach for your specific condition, we recommend consulting with your provider at Center for Specialty Care.
Physical Therapy
Physical therapy is often a cornerstone of tendon recovery, helping to restore strength, flexibility, and function. Our Physical Therapy team can guide you through:
- Eccentric Exercises: These are particularly effective for rebuilding tendon strength and promoting collagen formation in tendinosis. Eccentric exercises involve lengthening a muscle while it’s contracting.
- Gentle Stretching: Once the acute pain subsides, targeted stretching can improve tendon flexibility and range of motion. Applying heat before stretching can further improve flexibility.
- Strengthening Exercises: Building strength in the surrounding muscles helps support the tendon and prevent future injuries.
Pain Management
While heat and ice can provide significant relief, sometimes additional Pain Management strategies are necessary. This might include over-the-counter pain relievers, topical creams, or in some cases, other interventions recommended by our specialists to help you manage discomfort while your tendon heals.
Ergonomic Adjustments
For tendon issues caused by repetitive motions, ergonomic adjustments at home or work can be game-changers. Simple changes to your workstation, tools, or sports technique can significantly reduce strain on your tendons and prevent recurrence. Our team can help you identify and implement these crucial modifications.
The Science of Flexibility: How Heat Helps
Research has consistently shown the profound impact of heat on tissue flexibility. According to studies, heat is beneficial in increasing muscle and ligament flexibility, which can significantly reduce the risk of athletic injuries. For instance, heat increases the extensibility of important knee ligaments and can reduce the force needed to flex the knee by about 25% compared to cold application. This is because heat makes collagenous tissues more pliable, allowing them to stretch more easily. Even for women, who naturally show more knee ligament laxness, heat has the same relative beneficial effect on ligament flexibility. This scientific backing reinforces why heat is so valuable for chronic stiffness and preparing tendons for activity.
When to See a Doctor
While self-care with ice and heat is a great starting point, there are times when professional medical advice is essential. We urge you to seek help if:
- Pain Persists Over Two Weeks: If your symptoms don’t improve after two weeks of home treatment, it’s time for an expert evaluation.
- Severe Pain: If the pain is intense, sudden, or significantly impacts your daily life.
- Inability to Move the Joint: If you cannot move the affected joint normally or bear weight on it.
- Suspected Rupture: If you heard a pop or snap at the time of injury, or if there’s a significant deformity, you might have a ruptured tendon, which requires urgent medical attention. If you are in a lot of pain, you can contact Center for Specialty Care for prompt evaluation. You can also get help from 111 online if you’re in a lot of pain or think you have ruptured a tendon.
Frequently Asked Questions About Heat, Ice, and Tendonitis
We know you might still have some burning questions (pun intended!) about managing tendon pain. Here are answers to some of the most common queries we receive.
So, is heat good for tendonitis? A Quick Summary
To recap, is heat good for tendonitis is a nuanced question with a clear answer:
- Yes, heat is excellent for chronic tendon pain (tendinosis) to relieve stiffness, relax muscles, and increase blood flow, which aids in healing and improves flexibility. It’s best used after the initial acute phase (typically 72 hours post-injury).
- No, heat is generally not good for acute tendonitis when there is active inflammation, swelling, and fresh injury. In these cases, ice is preferred to reduce swelling and numb pain.
Can I use heat and ice together?
Yes, absolutely! Alternating between heat and ice, known as contrast therapy, can be very beneficial. This technique works by promoting a “pumping” action in your blood vessels: heat dilates them, increasing blood flow, and cold constricts them, reducing it. This can stimulate circulation, reduce stiffness, and help flush out waste products.
Contrast therapy is often recommended for chronic conditions, especially those with occasional flare-ups or when you’re transitioning from the acute inflammatory stage to the recovery phase. For guidance on the best approach for your specific condition, consult your provider at Center for Specialty Care. They can help you determine if contrast therapy is right for you and teach you the safest way to apply it.
When should I see a doctor for my tendon pain?
While many cases of tendon pain can be managed with rest, ice, and heat, there are definite signs that warrant professional medical attention. We encourage you to contact us at Center for Specialty Care if:
- Your pain is severe or suddenly worsens.
- You experience inability to move the joint or bear weight on the affected limb.
- You suspect a tendon rupture (often indicated by a sudden, sharp pain and a popping sound).
- Your symptoms do not improve within two weeks of consistent self-care using ice, heat, and rest.
- You notice signs of infection, such as increasing redness, warmth, or fever around the affected area.
Early and accurate diagnosis is key to effective treatment and preventing chronic issues. Don’t hesitate to reach out to our team if you have concerns.
Your Path to Pain-Free Movement
Navigating tendon pain can be frustrating, but with the right knowledge and support, you can find relief and get back to your favorite activities. The “warm truth” is that whether is heat good for tendonitis depends on the specific nature and stage of your condition. Ice and heat are powerful allies, but knowing when and how to use them effectively is crucial.
Proper diagnosis is the first and most important step. Listening to your body and understanding the difference between acute inflammation and chronic degeneration will guide you toward the most appropriate care.
For a comprehensive evaluation and a personalized treatment plan from experts who prioritize your recovery, explore the services at Center for Specialty Care. Our team of orthopedic specialists in Fairmont, Minnesota, Estherville, Iowa, Buffalo Center, Iowa, and St. James, Minnesota, is dedicated to helping you achieve 100% patient satisfaction with personalized care and quick appointment availability.