The Stiff Truth About Your Popping Shoulder
December 9, 2025
Shoulder Pain Explained: Causes, Symptoms, and Relief
December 11, 2025Ablation Spine Procedure: Ultimate Pain Relief 2025
Understanding RFA: A Solution for Chronic Spine Pain
Chronic back and neck pain can be debilitating, affecting millions and severely limiting daily life. When conservative treatments fall short, many seek advanced solutions for lasting relief. One such option is the ablation spine procedure.
So, what is an ablation spine procedure?
- It’s a minimally invasive medical treatment.
- It uses controlled heat (radiofrequency energy) to target specific nerves.
- The goal is to temporarily disrupt these nerves from sending pain signals to your brain.
- It’s primarily used for chronic pain stemming from spinal joints.
This procedure offers a way to manage persistent pain, often providing significant relief without major surgery.
As a board-certified orthopedic surgeon and sports medicine physician, I have over three decades of experience with advanced pain management techniques, including the ablation spine procedure, for conditions like chronic back and neck pain. At Center for Specialty Care, my focus is on delivering innovative, minimally invasive solutions that restore function and improve our patients’ quality of life.
Ablation spine procedure terms at a glance:
What is Radiofrequency Ablation and How Does It Work?
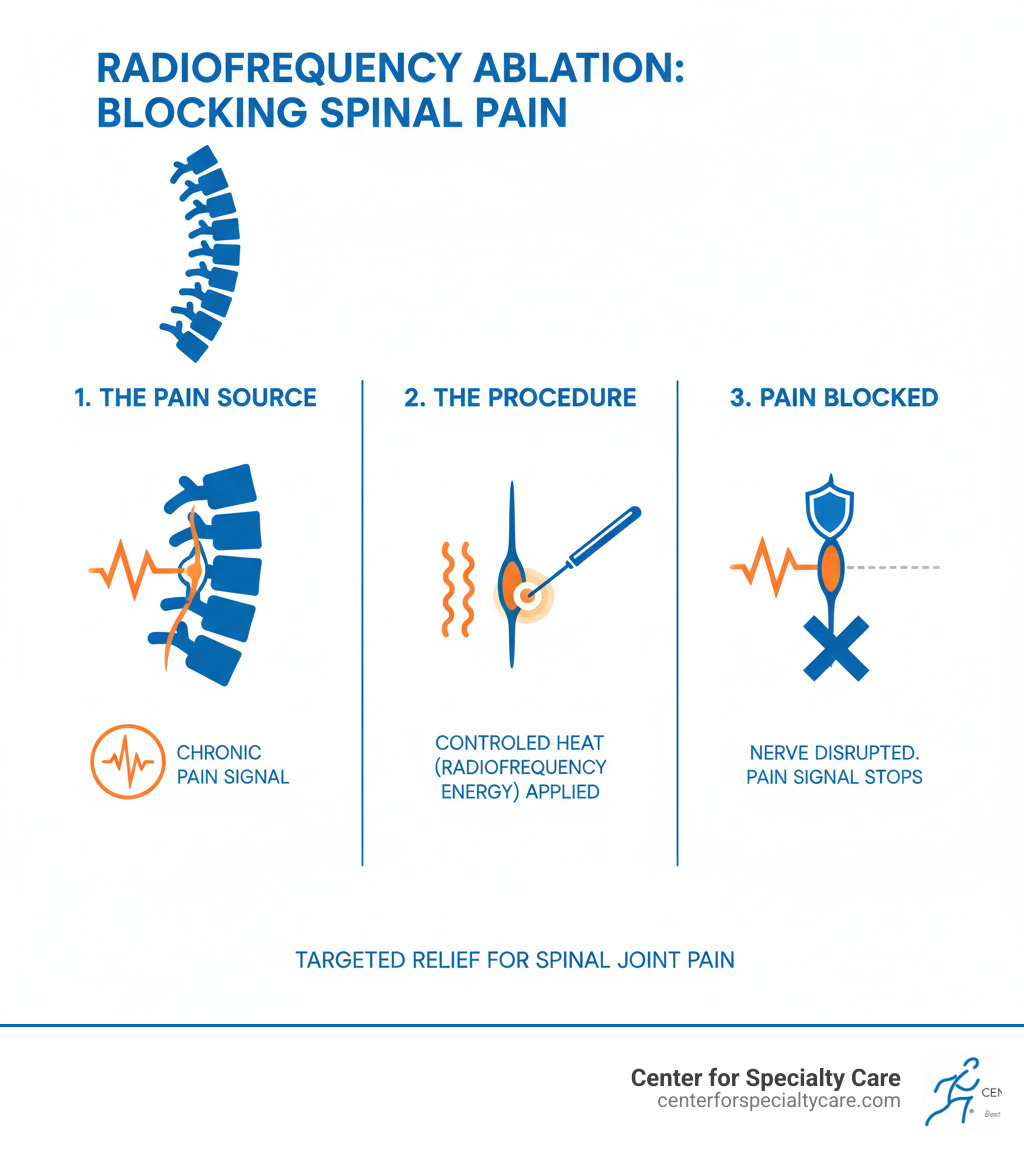
Radiofrequency ablation (RFA), also known as rhizotomy or neurotomy, is a sophisticated, minimally invasive technique designed to alleviate chronic pain. It’s a procedure that uses heat to disable nerves that are transmitting pain signals to the brain. Think of it like this: if a wire is sending an annoying signal, we simply turn off the switch.
The magic behind RFA lies in radiofrequency energy. This energy generates a controlled heat lesion, essentially creating a small burn on the targeted nerve tissue. This heat damages the nerve, preventing it from sending pain messages. The procedure specifically targets the medial branch nerves, which are the small sensory nerves that carry pain signals from the facet joints in your spine. By interrupting these signals, we can provide significant and often long-lasting pain relief.
The process is quite precise. A specialized needle electrode is positioned near the nerve. Once confirmed to be in the correct spot, radiofrequency current is applied, heating the tip of the needle. This heat then cauterizes and destroys the nerve, effectively reducing the pain you feel. It’s a targeted approach, ensuring that healthy nerves and surrounding tissues remain unaffected. This is why RFA is considered a non-surgical technique for pain treatment, offering a less invasive alternative to traditional surgery.
Conditions Treated with an Ablation Spine Procedure
Our ablation spine procedure is primarily intended to treat chronic pain stemming from specific areas of the spine. While it’s often associated with arthritis or joint pain of the spine, its applications are broad, addressing several common and often debilitating conditions.

The most common conditions we treat with RFA include:
- Facet Joint Syndrome: The facet joints are small joints located between the vertebrae that allow for movement and flexibility. When these joints become inflamed or arthritic, they can cause significant chronic low back pain and neck pain. RFA targets the medial branch nerves that innervate these joints, providing relief.
- Sacroiliac (SI) Joint Dysfunction: The sacroiliac joints connect the sacrum (the triangular bone at the base of your spine) to the ilium (the large bones of your pelvis). Inflammation or dysfunction in these joints can lead to pain in the lower back, buttocks, and sometimes the legs. RFA can be particularly helpful for targeting the lateral branch nerves that transmit pain from these joints. The evidence supports RFA as an efficacious treatment for both lumbar facet joint and sacroiliac joint pain, with five of six and both of the RCTs demonstrating statistically significant pain reductions, respectively.
- Spondylosis (Spinal Arthritis): This is a general term for age-related wear and tear of the spine, which often affects the facet joints. As the cartilage wears down, bones can rub together, leading to inflammation and pain. RFA can effectively manage the pain associated with spinal arthritis.
- Vertebrogenic Pain: This type of pain originates from the vertebral endplates, which are the surfaces of the vertebrae that connect to the intervertebral discs. When these endplates are damaged, often seen as Modic changes (Type 1 or Type 2) on an MRI, the basivertebral nerve (BVN) can transmit chronic pain signals. Basivertebral nerve ablation (BVNA) is a specific type of ablation spine procedure that targets this nerve within the vertebral body, offering relief for this distinct source of chronic low back pain. This is a relatively newer procedure, but studies show significant promise, with over 90% of patients experiencing improvements in pain and functioning in 3 to 12 months, and approximately 60% maintaining improvement for up to 5 years.
While RFA is a powerful tool, understand that it addresses the pain signals, not necessarily the underlying structural issue. However, by reducing pain, it significantly improves quality of life and function.
Who is an Ideal Candidate for RFA?
Determining the ideal candidate for an ablation spine procedure is a meticulous process, as we want to ensure the highest likelihood of success for our patients. This procedure is not a first-line treatment but rather an option for those who haven’t found relief through other means.
We typically consider RFA for individuals who meet several key criteria:
- Chronic Pain (> 6 months): Patients must have been experiencing chronic pain for at least six months. This ensures that the pain is not acute and has persisted despite initial treatment efforts.
- Failed Conservative Therapies: Before considering RFA, patients should have undergone and not found significant relief from a course of conservative treatments. This often includes physical therapy, anti-inflammatory medications, and other non-invasive approaches. We believe in exhausting less invasive options first.
- Positive Diagnostic Block: This is perhaps the most crucial criterion. RFA is considered only after it is confirmed that the cause of back pain lies in the facet joints (or SI joints, or vertebral endplates for BVNA). This confirmation comes from performing a diagnostic facet joint injection or medial branch block. If you experience at least 50% pain relief from this temporary nerve block, it strongly indicates that the targeted nerve is indeed the source of your chronic pain, making you a good candidate for the longer-lasting relief RFA can offer. For basivertebral nerve ablation, an MRI showing Modic Type 1 or Type 2 changes is a key diagnostic step.
- Specific Pain Source Identified: The pain should be localized to specific areas that RFA can effectively target, such as the facet joints or sacroiliac joints. For facet joint pain, an ideal candidate often experiences back pain more than leg pain, with pain worsening with prolonged standing or extension, and improving with sitting.
- Skeletal Maturity (for BVNA): For basivertebral nerve ablation, patients must have confirmed skeletal maturity.
- No Contraindications: We also assess for contraindications such as active infection at the injection site, pregnancy, bleeding disorders, or the presence of certain medical implants like pacemakers or defibrillators.
Our comprehensive evaluation process ensures that we identify patients who will most benefit from this advanced pain management technique. You can learn more about our general Pain Management services.
The Ablation Spine Procedure: A Step-by-Step Guide
I understand that the thought of any medical procedure can feel overwhelming. That’s perfectly normal. But here’s what I’ve learned over three decades: knowing exactly what to expect can transform anxiety into confidence. So let me walk you through our ablation spine procedure from start to finish, just as I would with any patient sitting in my office.
Preparing for Your Procedure
Your journey with the ablation spine procedure actually begins several days before you arrive at our center. Think of this preparation phase as setting the stage for the best possible outcome.
We’ll start with a thorough consultation where we sit down together and really talk. I want to understand your complete medical history, every medication you’re taking, any allergies you have, and what treatments you’ve already tried for your pain. More importantly, I want to hear about how this pain affects your daily life. Can you play with your grandchildren? Are you missing out on activities you love? What would relief mean to you? These conversations matter.
If you’re taking blood thinners like aspirin, warfarin, or newer medications like apixaban or rivaroxaban, we’ll need to make some temporary medication adjustments. This isn’t something to worry about—it’s simply a precaution to minimize any bleeding risk during the procedure. Typically, aspirin needs to stop about six days before your appointment, and warfarin about five days prior. Don’t forget to mention vitamins and supplements too, as some of those can thin your blood as well.
For your safety, we’ll provide specific fasting instructions. If you’ll be receiving sedation, you’ll need to avoid eating or drinking for at least eight hours before the procedure. I know going without your morning coffee can be tough, but it’s an important safety measure that follows guidelines from the American Society of Anesthesiologists.
Here’s something crucial: you’ll need to arrange transportation home. Because we may use sedation to keep you comfortable, driving yourself afterward isn’t an option. Ask a trusted friend or family member to pick you up and ideally stay with you for a few hours. Think of it as a good excuse to spend time together.
We might also ask you to shower with antibacterial soap the morning of your procedure—skip the lotions, creams, or perfumes on the treatment area that day. And if you smoke, this is an excellent time to quit. Stopping all forms of nicotine before the procedure can significantly improve your healing and reduce complications.
Throughout this preparation phase, no question is too small. Our team is here to make sure you feel completely comfortable and confident as your appointment approaches.
What to Expect During the Ablation Spine Procedure
The day has arrived, and I want you to know that our ablation spine procedure is an outpatient procedure—you’ll be going home the same day. While “spine procedure” might sound intimidating, we’ve designed every step with your comfort in mind.
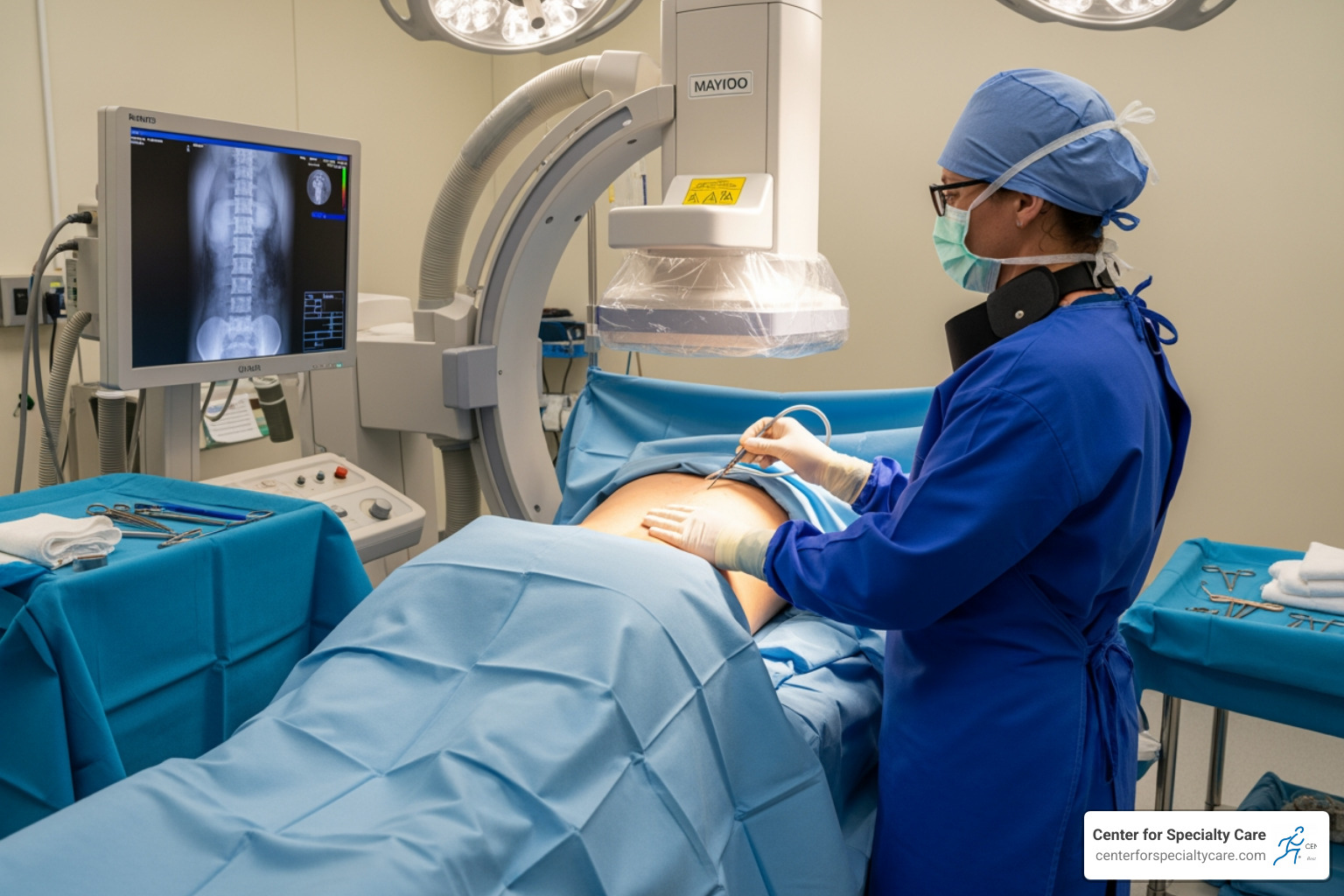
When you arrive at our surgical center, our nursing staff will greet you and help you get comfortable. We’ll position you on your stomach on a specialized X-ray table. Right away, we’ll administer local anesthesia to numb your skin, and we can offer mild sedation to help you relax. You’ll remain conscious throughout—this is actually important because we need to communicate with you during certain steps.
Now comes the precision work. We use fluoroscopy guidance, which is essentially a continuous X-ray that lets us see your spine in real-time. Think of it like having a GPS for your spine—it allows us to guide our instruments with pinpoint accuracy. We might also use a contrast dye to get an even clearer picture of the joints and nerves we’re targeting. This imaging technology ensures we’re placing the needle exactly where it needs to be, nowhere else.
Once your skin is numb, we carefully insert a thin, hollow needle called a cannula. Through this cannula, we advance a radiofrequency electrode. If you’re having basivertebral nerve ablation, this involves a transpedicular approach—we insert the probe directly into the vertebral body itself.
Before we proceed with the actual ablation, we perform what I consider the most important safety step: sensory and motor testing. We send a small electrical current through the electrode and ask you what you feel. You might notice a tingling sensation or see a muscle twitch. This feedback tells us we’re positioned correctly on the sensory nerve and safely away from any motor nerves that control your muscles. Your participation in this moment is invaluable.
Once we confirm perfect placement, we inject a bit more local anesthetic to keep you comfortable. Then we begin the ablation cycle. The radiofrequency current flows through the electrode, generating controlled heat at its tip. This creates a small heat lesion on the nerve—essentially interrupting its ability to send pain signals to your brain. Each nerve takes about 60 to 90 seconds to treat, though for basivertebral nerve ablation, the probe stays in place for 7 to 15 minutes.
The entire procedure typically takes about an hour, though it can range from 15 minutes to two hours depending on how many nerves we’re treating. Throughout everything, our team continuously monitors your vital signs and comfort level. We’re right there with you.
Patient Experience and Immediate Aftercare
Once we’ve completed the ablation spine procedure, our focus shifts entirely to your comfort and making sure you’re ready to go home safely.
It’s completely normal to experience some mild soreness at the injection site. Think of it like a sunburn or the feeling after a good workout—tender but manageable. You might also notice some bruising where the needle went in. Some patients experience temporary numbness in the treated area, or even a brief increase in their usual pain. I know that sounds counterintuitive, but it’s actually a sign that the nerve is responding. This typically settles down within a few days to a couple of weeks.
You’ll spend about one to two hours in our recovery room where our nurses will keep a close eye on you. We’re monitoring your vital signs and making sure any sedation has worn off enough for you to safely leave. We don’t rush this—your safety is paramount.
Before you head home, we’ll provide detailed discharge instructions. These cover everything from managing any discomfort to activity restrictions and warning signs to watch for. For the rest of the day, we want you to rest. Take it easy. Avoid strenuous activities, heavy lifting, twisting, or bending your spine for at least 48 hours. If you received sedation, no driving for 24 hours—that’s non-negotiable.
For managing any soreness, ice is your friend. Apply an ice pack to the treatment site for 15 to 20 minutes every couple of hours during the first day. We may also prescribe mild pain medication if you need it. Keep the small incision sites clean and dry, and avoid submerging them in water—no baths, pools, or hot tubs for at least 48 hours. Warm showers after a day or two are perfectly fine.
Here’s something important to understand: you might not feel immediate relief. Some patients do, but for many, pain relief develops gradually over the next four to six weeks. This is normal and expected. The nerve needs time to fully respond to the treatment.
We’re here to support you through every step of your recovery. If you have any concerns or questions afterward, don’t hesitate to reach out to our team.
After the Procedure: Recovery, Risks, and Results
Our commitment to your well-being extends far beyond the procedure room. We’re dedicated to guiding you through your recovery and helping you achieve the best possible outcomes from your ablation spine procedure.
The RFA Recovery Timeline
After your ablation spine procedure, your road to feeling better often begins quite quickly. Most patients are pleasantly surprised by how swiftly they can return to their daily routines, especially when compared to traditional surgery.
Immediately after, it’s normal to feel a bit of soreness, tenderness, or bruising at the injection site. This is your body’s natural response to the procedure. We recommend resting and taking it easy for the remainder of the day. For those undergoing basivertebral nerve ablation, we suggest a bit more caution in the first 48 hours: limit physical activity, avoid lifting anything over 15 lbs, and try not to twist or bend your spine.
While some individuals might experience pain relief right away, for most, the real magic happens gradually. You’ll likely notice the pain relief becoming more significant over the course of a few weeks. It can take anywhere from three to six weeks to feel the maximum benefit, as the nerve needs time to fully respond to the ablation and for any post-procedure inflammation to settle down.
Soon, you’ll be encouraged to gently ease back into your normal activities. A gradual return to normal activities and exercise is key. Sometimes, we might even recommend physical therapy to help strengthen your back muscles, improve flexibility, and maintain the wonderful benefits of your procedure. This collaborative approach ensures comprehensive care for your Back & Spine health. We’ll also schedule follow-up appointments to monitor your progress, check in on your pain levels, and ensure you’re healing well. We absolutely love hearing about our patients getting back to doing what they love!

Many of our patients find that this gradual return allows them to ease back into their hobbies and daily activities, often with a renewed sense of comfort and mobility they haven’t felt in a long time. Imagine happily returning to gardening, walking, or simply enjoying everyday life with less pain!
Benefits vs. Risks of RFA
Like any medical intervention, the ablation spine procedure comes with both potential benefits and risks. We believe in open and honest communication, so here’s a clear overview:
| Benefits of RFA | Risks of RFA |
|---|---|
| Minimally invasive | Infection (rare) |
| Long-lasting relief | Bleeding (rare) |
| Avoids surgery | Temporary increase in pain or soreness |
| Quick recovery | Temporary numbness or weakness in the treated area |
| Improved quality of life | Nerve damage (very rare, careful technique minimizes) |
| Repeatable | Skin irritation or burn at the injection site (rare) |
Effectiveness and Long-Term Outcomes
So, what kind of lasting relief can you truly expect from an ablation spine procedure? Many patients experience significant pain reduction and improved mobility and function, allowing them to participate in activities they once avoided. This can be truly life-changing!
The duration of relief from RFA is quite impressive, often lasting between 9 to 18 months. This is because the treated nerve eventually regrows. Think of it like a pathway that’s been temporarily blocked; over time, new growth can allow signals to pass again. However, this nerve regeneration doesn’t mean the pain automatically returns with the same intensity. When the pain does start to return, the good news is that the procedure is typically repeatable. Many patients find success with subsequent RFA procedures when needed, continuing to manage their chronic pain effectively.
Research and consensus guidelines for lumbar facet pain (which you can explore further here: https://pubmed.ncbi.nlm.nih.gov/32245841/) consistently support RFA as a safe and effective option for long-term pain management. It’s a powerful tool in our arsenal to help you regain control over your chronic spine pain.