Warm Up to Wellness: How Heat Therapy Soothes Aches
December 3, 2025
Your Guide to Pain Relief: MN Back and Chronic Pain Clinics
December 5, 2025Achilles tendon pain: Expert Relief 2025
Why Achilles Tendon Pain Demands Your Attention
Achilles tendon pain affects the thick band of tissue connecting your calf muscle to your heel. As one of the most common complaints in active adults, this pain can significantly limit your mobility, whether it’s a sudden “pop” during sports or a gradual ache after morning runs.
Quick Answer: What You Need to Know About Achilles Tendon Pain
- What it is: Inflammation or irritation of the Achilles tendon.
- Common symptoms: Aching pain, morning stiffness, swelling near the heel, and tenderness.
- Main causes: Overuse, sudden increases in activity, tight calf muscles, and improper footwear.
- When to see a doctor: If you have severe pain, cannot move your foot, or suspect a rupture (a popping sound with sudden pain).
- Recovery time: Typically 3-6 months with conservative treatment; 9-12 months if surgery is required.
- Treatment options: Rest, ice, physical therapy, stretching, supportive shoes, and in severe cases, surgery.
The Achilles is your body’s largest tendon, absorbing forces several times your body weight with every step, run, or jump. This constant demand makes it vulnerable to overuse injuries like Achilles tendinitis (also called tendinopathy). While about 24% of athletes experience this, you don’t have to be an elite competitor. Weekend warriors and those starting new exercise routines are also at risk.
The good news is that most cases respond well to conservative treatment when caught early. I’m Dr. Corey Welchlin, an orthopedic surgeon with three decades of experience. At the Center for Specialty Care in Fairmont, Minnesota, I’ve helped countless patients across southern Minnesota and northern Iowa recover from sports injuries affecting this critical tendon. My goal is to help you understand your options and find the most effective path to relief.
Understanding Achilles Tendon Pain: Symptoms and Causes
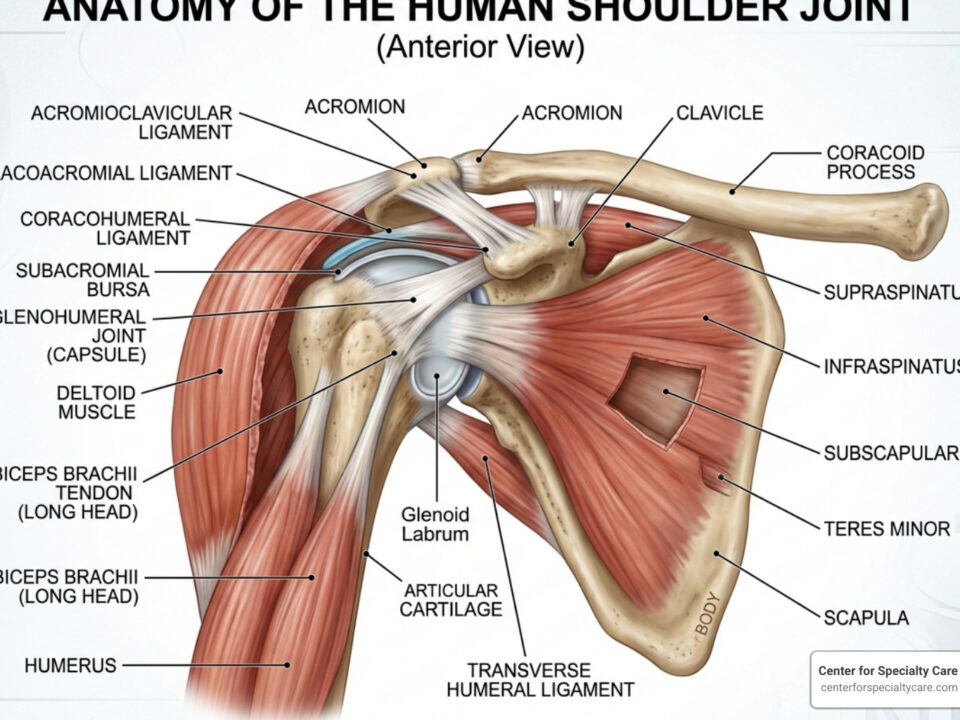
Your Achilles tendon is a thick, fibrous cord connecting your calf muscles to your heel bone, enabling you to walk, run, and jump. When this vital structure becomes irritated or damaged, you experience Achilles tendon pain.
Common Achilles injuries include:
- Achilles tendinitis: Acute inflammation from a sudden overload, causing swelling and pain.
- Achilles tendinopathy (or tendinosis): A chronic condition where the tendon’s collagen fibers break down over time from repetitive micro-tears, leading to a thickened, weakened, and chronically painful tendon.
- Achilles rupture: A partial or complete tear of the tendon, often accompanied by a “pop” or snapping sensation. This can happen during explosive movements or even everyday activities if the tendon is already weak.
Most Achilles injuries are overuse injuries from repetitive stress—pushing your body too hard, too fast, without adequate recovery. This is common in athletes who ramp up training too quickly or individuals who suddenly increase their activity levels. With proper care, most of these injuries are preventable. Our Sports Medicine services team can help you return to your favorite activities while minimizing the risk of re-injury.
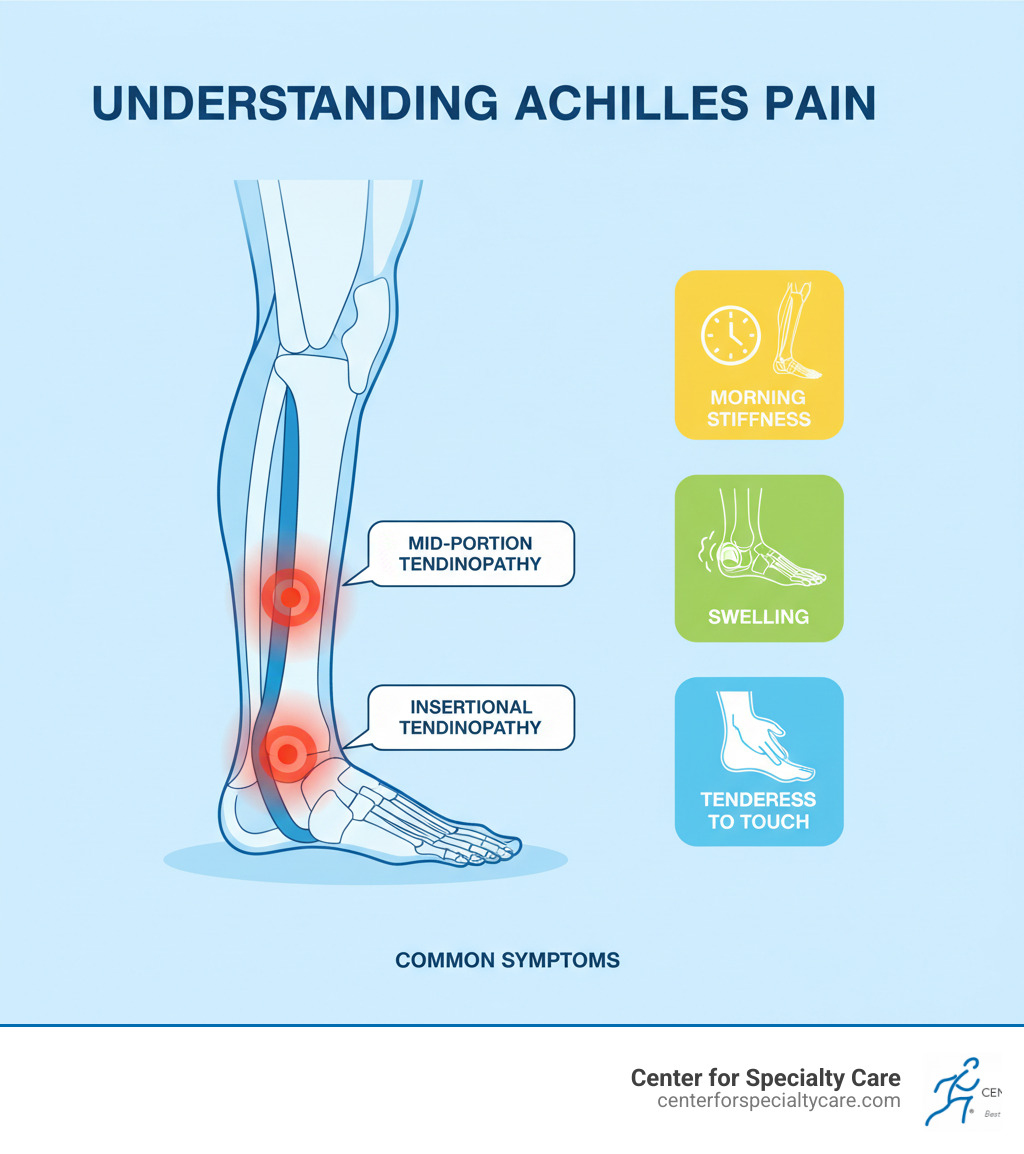
Common Symptoms to Watch For
Recognizing the signs of Achilles tendon pain early can lead to a quicker recovery. Be aware of these warning signals:
- A mild ache in the back of the leg or above the heel, which can progress to severe pain after activity.
- Morning stiffness that makes the first few steps of the day extremely painful but improves with movement.
- Tenderness to touch or a burning sensation along the tendon.
- Swelling around the heel and lower leg, sometimes with noticeable thickening of the tendon.
- Leg weakness, especially when trying to stand on your toes or push off the ground.
- A popping sound with sudden, sharp pain, which is a medical emergency indicating a likely rupture. Seek immediate medical attention.
What Causes Achilles Injuries?
Several factors can contribute to Achilles tendon pain, with overuse being the primary trigger.
- Sudden increase in activity: Dramatically increasing your running mileage or workout intensity without giving your body time to adapt.
- Tight or weak calf muscles: Tight calves put constant strain on the tendon, while weak calves fail to provide adequate support.
- Improper footwear: Worn-out shoes or those lacking proper cushioning and arch support increase stress on the tendon.
- Hill running: Running uphill overworks the tendon, while downhill running increases impact forces.
- Bone spurs: Bony growths on the heel (Haglund’s deformity) can rub against the tendon, causing irritation.
- Age-related weakening: Tendons naturally become less flexible and more prone to injury as we age.
- Medical conditions: Psoriasis, high blood pressure, and high cholesterol have been linked to tendon issues.
- Certain antibiotics: Fluoroquinolones (e.g., Cipro, Levaquin) are associated with a higher risk of tendinitis and rupture. Contact your doctor if you develop tendon pain while taking these medications.
For more in-depth research on Achilles tendinitis causes, the Mayo Clinic provides excellent resources.
Diagnosis: When to See a Doctor for Your Heel Pain
A minor ache might improve with rest, but persistent or severe Achilles tendon pain requires professional evaluation. If self-care measures haven’t helped after a few weeks, or if the pain is interfering with daily activities like walking or climbing stairs, it’s time to see a healthcare provider.
At the Center for Specialty Care, our Orthopedics department is equipped to diagnose and treat a wide range of musculoskeletal issues. We offer quick appointment availability so you can get the help you need without a long wait.
When to Seek Immediate Medical Attention
Some symptoms of Achilles tendon pain require immediate medical care. Head to an urgent care center or call your provider right away if you experience:
- Sudden, severe pain in the back of your ankle during an activity.
- A “pop” or snapping sensation, often described as feeling like you were kicked in the ankle.
- Inability to bear weight on the affected leg or walk normally.
- A visible gap or depression in the tendon area just above your heel.
- Inability to move your foot downward or stand on your tiptoes on that leg.
These are all signs of a potential Achilles tendon rupture and should not be ignored.
How Doctors Diagnose Achilles Tendon Pain
To create an effective treatment plan, we first need an accurate diagnosis. The process begins with a detailed conversation about your medical history, symptoms, activity levels, and footwear.
Next is a physical examination. We will assess your foot, ankle, and lower leg for tenderness, swelling, and any thickening of the tendon. We will also check your range of motion and observe your gait. Simple strength tests, like standing on your toes, help us evaluate the tendon’s function.
For a suspected rupture, we perform the Thompson test. While you lie face-down, we squeeze your calf muscle. If the foot doesn’t automatically point downward, it strongly indicates a complete tear.
In many cases, a clinical exam is sufficient for diagnosis. However, we may use imaging tests to confirm the diagnosis, determine the severity of the damage, or plan for surgery.
- X-rays can reveal bone spurs or calcification within the tendon, which is common in insertional tendinopathy.
- MRI scans provide detailed images of soft tissues, allowing us to see the extent of tendon degeneration or identify partial and complete tears.
- Ultrasound offers a real-time view of the tendon, showing thickening, tears, and inflammation, and can be a quicker, less expensive alternative to an MRI.
Your Path to Recovery: Treatment Options
Healing from Achilles tendon pain takes time and dedication. For non-surgical cases of tendinosis, recovery typically takes 3 to 6 months. If surgery is needed for a rupture or chronic condition, the timeline extends to 9 to 12 months or more. Patience is key, but with the right treatment plan, most patients return to their normal activities.
Our Pain Management specialists partner with you throughout your recovery, using comprehensive strategies to manage pain and address the root cause.

Non-Surgical Treatments for Achilles tendon pain
The vast majority of Achilles tendon pain cases respond well to conservative treatment. We always start with these lower-risk, effective methods.
- The RICE Method: Rest from aggravating activities, Ice the area for 15-20 minutes several times a day, use Compression to control swelling, and Elevate your leg to reduce inflammation.
- Activity Modification: We’ll help you switch to low-impact activities like swimming or cycling to maintain fitness without stressing the tendon.
- Physical Therapy: This is crucial for recovery. A therapist will guide you through eccentric strengthening exercises (like heel drops) and calf stretches to rebuild tendon strength and flexibility.
- Supportive Footwear and Orthotics: Shoes with good heel cushioning and arch support are essential. Custom orthotics or heel lifts can correct biomechanical issues and reduce strain on the tendon.
- Night Splints: Wearing a splint at night keeps the tendon gently stretched, which can significantly reduce morning stiffness.
- Pain Relievers: Over-the-counter NSAIDs like ibuprofen can help manage pain and inflammation in the short term, but they are not a long-term solution.
Advanced and Surgical Interventions
If pain persists after six months of conservative treatment, or in the case of a complete rupture, more advanced options may be considered.
We do not recommend cortisone injections into the Achilles tendon, as they can weaken the tissue and increase the risk of rupture.
Surgical options include:
- Gastrocnemius Recession: A procedure to surgically lengthen the calf muscles, reducing tension on the Achilles tendon.
- Debridement and Repair: The damaged portion of the tendon is removed, and the remaining healthy tissue is repaired. Any bone spurs may also be removed. While satisfaction rates are high, 20-30% of patients may experience some continued pain.
- Tendon Transfer: If more than 50% of the tendon is damaged, a healthy tendon (often from the big toe) is transferred to reinforce the Achilles.
- Hydrocision TenJet®: A minimally invasive procedure that uses a high-pressure water stream to remove damaged tissue through a small incision.
Post-surgery rehabilitation is critical and can last up to 12 months. You’ll work closely with our physical therapy team to regain strength and function. For more details, see our Podiatric Surgery Guide.
Sports Medicine Australia also offers helpful resources on this topic.
Preventing Future Achilles Injuries
The best way to deal with Achilles tendon pain is to prevent it. Prevention is about making smart, consistent choices in your training and daily habits to maintain the health of your feet and ankles.
Incorporating cross-training with low-impact activities like swimming or biking gives your Achilles tendon a break from repetitive pounding while maintaining your cardiovascular fitness. This allows the tendon to recover while you stay active.

Key Prevention Strategies
These habits make the biggest difference in preventing Achilles tendon injuries:
- Increase activity gradually. Follow the “10% rule”: increase your training distance, intensity, or frequency by no more than 10% per week to allow your tendons to adapt.
- Warm up properly. Spend 10-15 minutes on light cardio and dynamic stretches before exercise to increase blood flow and make tendons more pliable.
- Stretch daily. Focus on your calf muscles and Achilles tendon, especially in the morning and before and after activity. Hold stretches like the wall stretch for 30 seconds.
- Strengthen your calf muscles. Perform calf raises (with both straight and bent knees) to build support for the tendon and reduce its workload.
- Choose correct footwear. Wear supportive shoes appropriate for your activity. Replace worn-out athletic shoes every 300-500 miles, as they lose their ability to absorb shock.
- Vary your running surfaces. Avoid constantly running on hard or uneven surfaces. Softer surfaces like tracks or grass are gentler on your tendons.
- Listen to your body. Pain is a signal to stop. If you feel pain in your Achilles, back off or rest. Ignoring it can turn a minor issue into a serious injury.
Frequently Asked Questions about Achilles Tendon Issues
When you’re dealing with Achilles tendon pain, it’s natural to have questions. Here are answers to some of the most common concerns we hear from our patients at the Center for Specialty Care.
How long does Achilles tendinitis take to heal?
Recovery time varies based on the injury’s severity, the treatment approach, and your personal health.
- Non-surgical treatment: For mild to moderate tendinitis, expect a recovery period of 3 to 6 months. Tendons heal slowly due to limited blood supply, so consistency with your rehabilitation is key.
- Surgical intervention: After surgery for a rupture or chronic tendinopathy, a full recovery can take 9 to 12 months or longer. This includes immobilization followed by intensive physical therapy.
Patience is essential. Your Achilles tendon pain didn’t develop overnight, and it won’t disappear overnight either. With proper care, most patients make a full return to their activities.
Should I stop running if my Achilles hurts?
Yes, if the pain is sharp, persistent during your run, or worse afterward, you need to stop running immediately. Trying to “run through” significant Achilles tendon pain can turn a manageable injury into a severe one, potentially leading to a rupture and a much longer recovery.
However, stopping running doesn’t mean stopping all exercise. This is a perfect time for activity modification. Switch to low-impact cross-training like swimming, cycling, or using an elliptical to maintain your fitness without stressing the tendon.
If you’re unsure, consult with one of our specialists. We can assess your injury and provide clear guidance on safe activity levels to prevent further damage.
What are the potential complications of an Achilles injury?
If an Achilles injury is ignored or not managed properly, several complications can arise. While most patients heal well with treatment, it’s important to be aware of the risks:
- Tendon rupture: Chronic tendinitis weakens the tendon, making it vulnerable to a complete tear. This is a serious injury that often requires surgery and a lengthy rehabilitation.
- Chronic pain: Some patients, particularly after surgery for severe tendinopathy, may experience persistent discomfort. Studies show this affects 20-30% of surgical patients.
- Deep Vein Thrombosis (DVT): A blood clot can form in the leg, especially after being immobilized in a cast or boot. This is a serious condition requiring immediate medical attention.
- Re-injury: Returning to sport too soon without completing a full rehabilitation program increases the risk of injuring the tendon again.
- Surgical risks: As with any surgery, there are risks of infection, wound healing problems, or nerve damage. We take every precaution to minimize these risks.
Conclusion: Take the Next Step Towards Pain-Free Movement
You now have a solid understanding of Achilles tendon pain, from its early warning signs to its treatment options. The most important takeaways are to listen to your body, start treatment early, and seek professional guidance.
The sooner you address Achilles tendon pain, the better your chances of a quick, non-surgical recovery. You don’t have to steer this journey alone.
At Center for Specialty Care, our philosophy is that your recovery is personal, and your care should be too. Whether you visit us in Fairmont, MN, Estherville, IA, Buffalo Center, IA, or St. James, MN, you’ll receive personalized attention from a team that understands your goals. We know that heel pain isn’t just a symptom—it’s what keeps you from living your life to the fullest.
Our orthopedic surgeons, podiatry specialists, and pain management experts collaborate to create a treatment plan that fits your life. We stand by our 100% patient satisfaction commitment and offer quick appointment availability because when you’re in pain, you shouldn’t have to wait for help.
You’ve taken the first step by educating yourself. Now, let us help you with the next one.
Contact our Podiatry specialists for a consultation today. Let’s work together to get you back to pain-free movement.