Warm Up to Relief: The Benefits of Heating Pads for Tendonitis
October 30, 2025
Your Guide to Iowa Pain Clinics: Expert Care for Chronic Discomfort
November 3, 2025Intracept Procedure Denied By Insurance: Overturn in 3 Steps!
When Your Intracept Procedure Gets Denied: What You Need to Know Right Now
If your intracept procedure denied by insurance letter just arrived, you’re likely feeling frustrated and confused. But here’s the good news: a denial is not the final word. Many patients successfully overturn their denials by following the right steps.
Quick Answer: What to Do If Your Intracept Procedure Was Denied
- Review your denial letter carefully to understand the specific reason (cost concerns, “experimental” label, missing prior authorization, or incomplete documentation).
- Gather supporting evidence including your medical history, MRI showing Modic changes, and documentation of failed conservative treatments.
- Work with your doctor to obtain a detailed Letter of Medical Necessity.
- File an internal appeal with your insurance company within the specified timeframe.
- Request an external review if your internal appeal is denied.
- Consider legal assistance if you face repeated denials or suspect bad faith.
Chronic low back pain is incredibly common, but for those with pain lasting 12 weeks or more, the Intracept procedure—a minimally invasive treatment targeting the basivertebral nerve—offers real hope when other treatments have failed.
Unfortunately, insurance companies often deny coverage, typically citing cost (the procedure ranges from $10,000 to $15,000) or labeling it “experimental,” despite its FDA approval and strong clinical evidence. The reality is that Medicare and many private insurers do cover Intracept when patients meet specific criteria.
This guide will walk you through exactly how to fight your denial, what documentation you need, and when to escalate your appeal.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon at the Center for Specialty Care. I’ve helped countless patients get their intracept procedure denied by insurance overturned, and I know that proper documentation and persistence can turn a “no” into a “yes.”
Common intracept procedure denied by insurance vocab:
Understanding the Intracept Procedure and Why It’s Recommended
When you’re facing an intracept procedure denied by insurance, you need to know why this specific treatment is right for your condition. The Intracept procedure, or basivertebral nerve ablation, is a minimally invasive outpatient treatment for a specific type of chronic low back pain called vertebrogenic pain. This pain originates from the basivertebral nerve inside your vertebrae. During the procedure, a physician uses radiofrequency energy (heat) to disable this nerve, stopping it from sending pain signals to the brain. Unlike other treatments, it directly targets the source of the pain without spinal implants.

Who is a Good Candidate for Intracept?
The procedure is not for everyone. It’s specifically for patients who meet strict criteria, which is crucial for proving your case to insurance:
- Chronic Low Back Pain: Lasting at least six months.
- Failed Conservative Care: You must have documented proof that you’ve tried and failed at least six months of other treatments, such as physical therapy, anti-inflammatory medications, injections, and sometimes cognitive behavioral therapy.
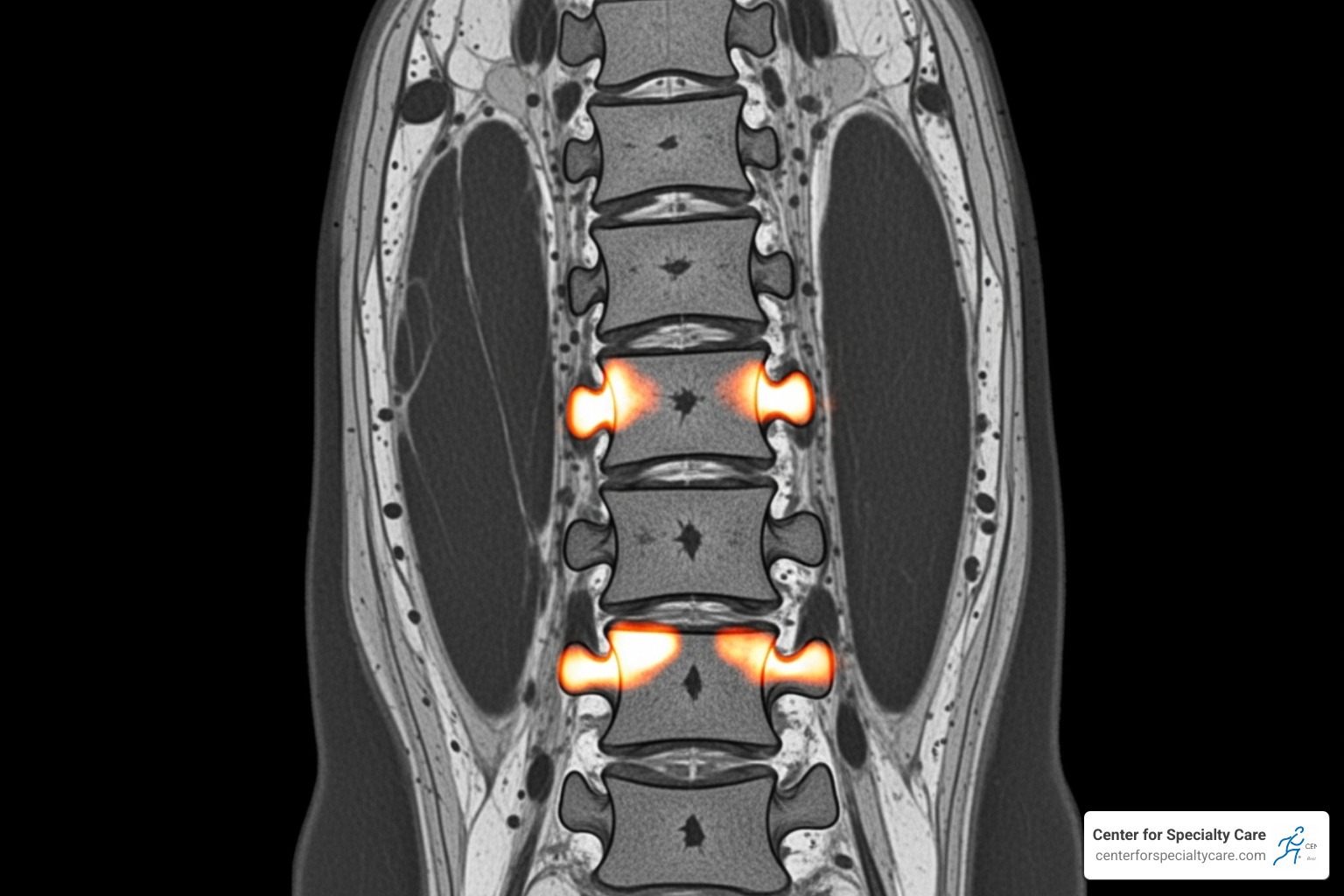
- Specific MRI Findings: Your MRI must show Modic Type I or Type II changes at the vertebral endplates (between L3 and S1). These changes are a key indicator of vertebrogenic pain.
- No Disqualifying Conditions: You generally cannot have severe spinal stenosis, large disc protrusions (>5mm), or significant spondylolisthesis (>2mm).
Why is Intracept Worth Fighting For?
When an intracept procedure denied by insurance happens, it’s important to know the benefits you’re fighting for:
- Proven Success: Clinical studies show 64% of patients report over 50% pain relief, and 30% report complete relief. Long-term data shows these results are sustained for up to five years.
- Minimally Invasive: It’s an outpatient procedure with no spinal implants, leading to a faster recovery than traditional spine surgery.
- FDA-Approved: The procedure is FDA-approved for treating chronic low back pain caused by Modic changes, confirming its safety and effectiveness.
For more details, visit our page on the Intracept Procedure or our Back & Spine section.
Why Your Intracept Procedure Was Denied by Insurance
When that denial letter arrives, it can be confusing. While the reasons can seem complex, they usually fall into a few common categories. Understanding why your intracept procedure denied by insurance claim was rejected is the first step to fighting back.

Common reasons for denial include:
- High Cost: The procedure’s price tag ($10,000-$15,000) makes insurers look for any reason to deny it.
- “Experimental or Investigational” Label: This is a frequent but outdated reason. We counter this by citing the procedure’s FDA approval, Level 1 clinical evidence from major studies, and data showing sustained, long-term pain relief. This is a proven, effective treatment, not an experiment.
- Administrative Errors: Simple mistakes like a lack of prior authorization or incomplete paperwork can trigger an automatic denial.
- “Not Medically Necessary”: The insurer may claim you haven’t tried enough conservative treatments or that your MRI doesn’t meet their specific criteria.
- Exclusion Criteria: Your MRI may show other conditions like severe spinal stenosis or a large disc herniation, which insurers use to deny coverage.
Coverage policies vary. Medicare has specific criteria (Local Coverage Determinations), and while some private insurers like Anthem Blue Cross and Blue Shield, Cigna Healthcare, and Humana have favorable policies, others are more restrictive. Regardless of the insurer, a denial is often based on one of the reasons above, all of which can be addressed in an appeal.
What Insurance Looks For: Proving Medical Necessity
When you appeal a denial, your goal is to prove “medical necessity.” This means showing the insurance company that the Intracept procedure is the right and necessary treatment for you, specifically. It’s not enough for the procedure to be effective in general; you must demonstrate that you meet all the criteria and have exhausted other reasonable options.
This is where your physician becomes your strongest advocate. At Center for Specialty Care, we partner with you to build a compelling case. The cornerstone of a successful appeal is a comprehensive packet of evidence, including:
- A Detailed Letter of Medical Necessity: Written by your doctor, this letter tells your unique story, details your failed treatments, and explains why Intracept is the logical next step.
- Complete Medical Records: This includes consultation notes, physical exam findings, and your MRI reports and images that clearly show Modic changes.
- Documentation of Failed Therapies: We gather proof of every conservative treatment you’ve tried, showing that you’ve done your due diligence.
Our experience in Pain Management means we know exactly what insurers need to see. We don’t just treat your pain; we help you steer the system to get the care you deserve. For more on the conditions we treat, visit our Back & Spine page.
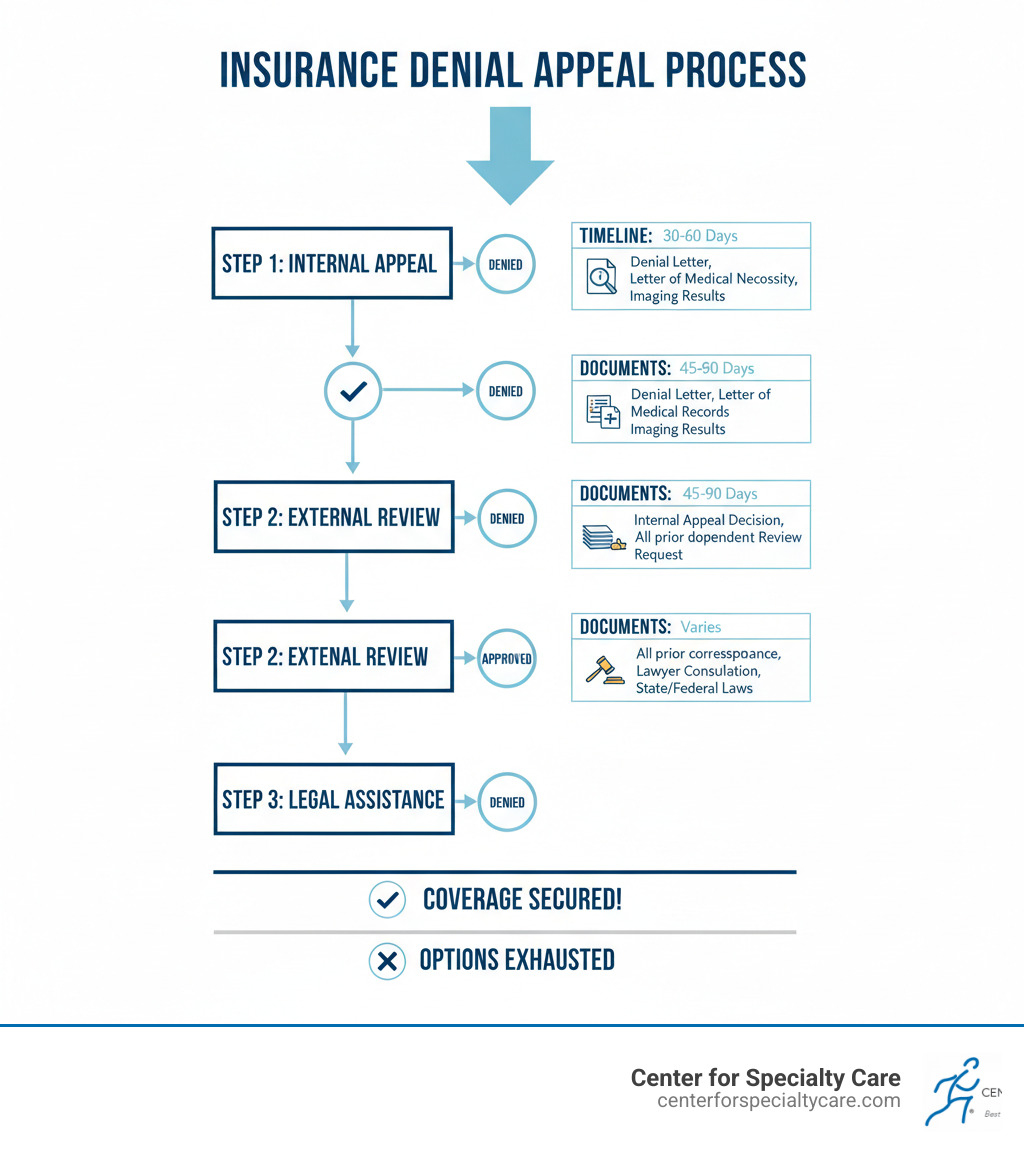
Your Step-by-Step Guide to Appealing an Intracept Procedure Denial
Receiving an intracept procedure denied by insurance letter is frustrating, but it’s not the end of the road. The appeals process is your chance to challenge the decision. It typically involves two stages: an internal appeal with your insurer and an external review by an independent party.

Step 1: The Internal Appeal
This is your first chance to have the decision reversed.
- Review the Denial Letter: It will state the exact reason for the denial and the deadline for your appeal (usually 180 days). Your appeal must directly address their stated reason.
- Gather Your Evidence: Work with our office to collect your complete medical history, MRI reports showing Modic changes, and detailed records of all failed conservative treatments.
- Obtain a Letter of Medical Necessity: This powerful letter from your doctor tells your personal story and directly counters the insurer’s reason for denial, citing clinical evidence and your treatment history.
- Submit Your Appeal: Follow the insurer’s instructions precisely. Send everything via certified mail with a return receipt and keep copies of everything you send.
- Follow Up: Be polite but persistent. Call to confirm receipt and check on the status of your appeal regularly.
Step 2: The External or Independent Review
If the internal appeal is denied, don’t give up. An external review is often where patients succeed.
- What it is: Your case is sent to a neutral, third-party Independent Review Organization (IRO). The reviewer is a medical professional with no financial stake in the decision.
- How to request it: Your second denial letter will contain instructions and a deadline for requesting an external review.
- The Decision: The IRO reviews all the evidence and decides based on accepted medical standards. In many states, the IRO’s decision is legally binding. If they rule in your favor, the insurance company must cover the procedure.
When to Seek Legal Assistance
Most denials can be overturned through the standard appeal process. However, you might consider legal help if:
- Your case is unusually complex.
- You suspect your insurer is acting in “bad faith” (e.g., repeatedly losing documents, ignoring clear evidence).
- You have exhausted all appeals and are still being denied.
An attorney specializing in health insurance denials can help protect your rights and motivate the insurance company to reconsider. At Center for Specialty Care, we are committed to advocating for you throughout this process and will work with you to build the strongest possible case for your treatment.
Frequently Asked Questions about Intracept Insurance Denials
Facing an intracept procedure denied by insurance can be confusing. Here are quick answers to some common questions.
How long does the appeal process usually take?
Timelines vary, but you can generally expect:
- Internal Appeal: 30 to 60 days for a decision.
- External Review: An additional 45 to 60 days.
The entire process can take several months, which is why persistent follow-up is key.
What are my chances of winning an appeal?
Your chances are good if your case is well-documented. Success hinges on having clear evidence that you meet the specific medical criteria, including:
- An MRI clearly showing Modic Type I or Type II changes.
- Thorough records of at least six months of failed conservative treatments.
- A compelling Letter of Medical Necessity from your doctor.
Many patients who persist through the entire appeals process are ultimately successful.
What if my appeal is denied again? Are there other options?
Yes. If your final appeal is denied, we don’t give up. We will:
- Re-evaluate your case to see if a new appeal is possible.
- Explore other effective treatments. Our comprehensive Orthopedics services include many alternatives, from advanced interventional techniques to other surgical options.
- Discuss payment options. We can explore financing or payment plans to make the procedure accessible.
A denial is not the end of your journey to relief. We are committed to finding a solution that works for you.
Take Control of Your Back Pain Journey
Dealing with an intracept procedure denied by insurance is a challenge, but it’s one you can win. You are your own best advocate. With the right documentation—MRI evidence of Modic changes, records of failed conservative care, and a strong Letter of Medical Necessity—many appeals are successful.
You shouldn’t have to live with chronic pain when a proven, FDA-approved treatment is available. At the Center for Specialty Care, we stand beside you through every step of the process. Our physicians are not just providers; we are advocates who craft the detailed documentation needed to overturn denials.
We believe in personalized care and are committed to 100% patient satisfaction. Whether you’re in Fairmont, Minnesota, or our Iowa locations, our team is ready to help you fight for the treatment you deserve.
If your intracept procedure denied by insurance has left you wondering what to do next, we’re here to help. Learn more about the Intracept Procedure and contact us today for a consultation. Let’s work together to get you the relief you deserve.