Say Goodbye to Shoulder Blade Knots Your Complete Guide to Lasting Relief
December 26, 2025
The Nerve of It! A Deep Dive into Ablation for Chronic Pain
December 30, 2025Subluxed Joints: Essential 2025 Recovery
What Does “Subluxed” Really Mean?
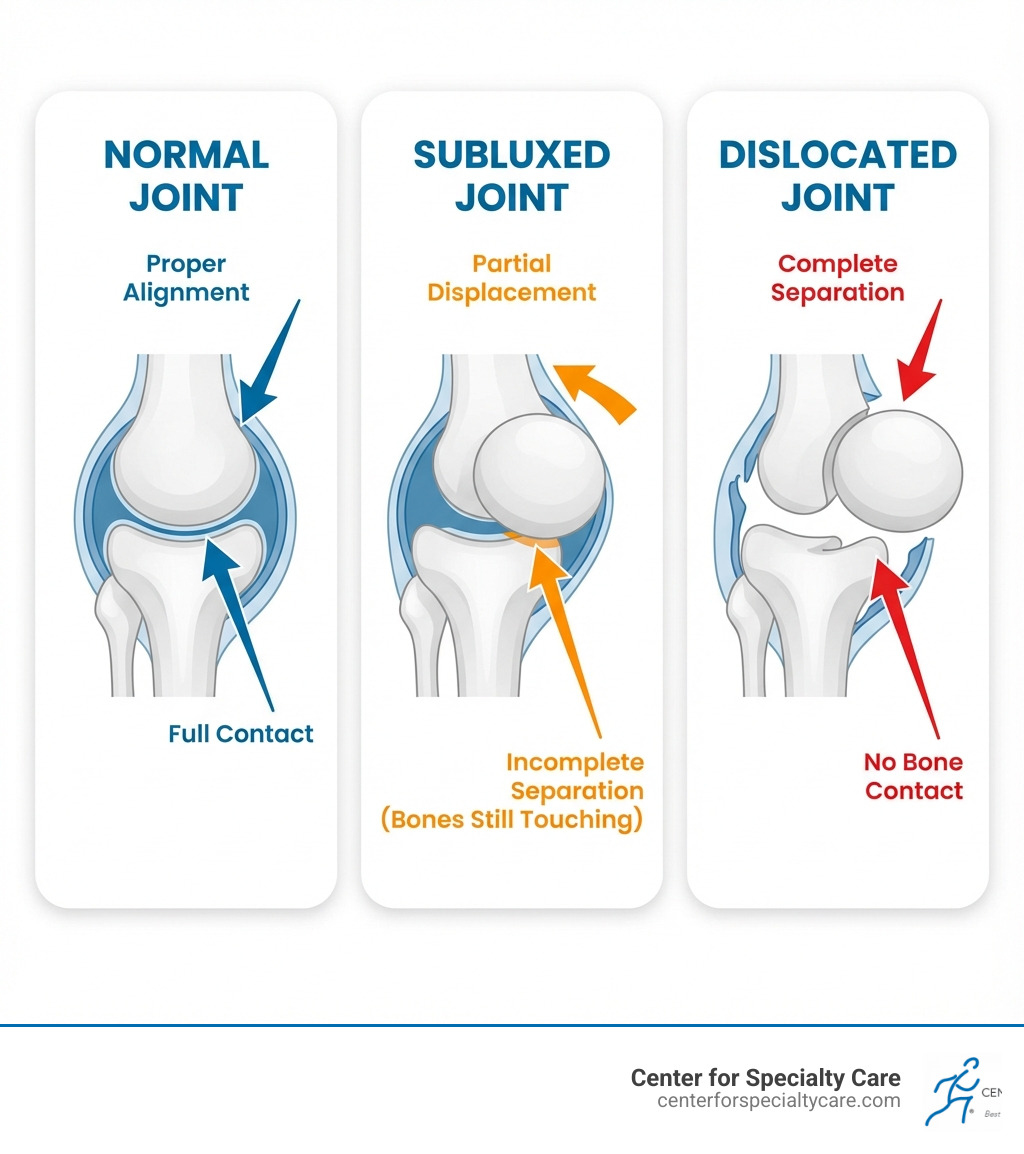
Subluxed refers to a partial dislocation of a joint, where the bones slip out of their normal alignment but remain partially in contact with each other. Unlike a complete dislocation (luxation), where the bones separate entirely, a subluxation is an incomplete separation that can cause pain, instability, and limited movement.
Key Facts About Subluxation:
- Definition: A partial or incomplete dislocation where joint surfaces maintain some contact
- Common Locations: Shoulder, kneecap (patella), elbow, spine, and fingers
- Main Causes: Trauma, falls, repetitive motion, sports injuries, joint laxity, or underlying conditions like arthritis
- Symptoms: Pain, swelling, popping sensation, feeling of joint “giving way,” limited range of motion
- Treatment: Ranges from conservative care (rest, ice, physical therapy) to surgical repair for severe or recurrent cases
A subluxation occurs when the ligaments, tendons, or capsule surrounding a joint become stretched, torn, or weakened, allowing the bones to shift out of position. While some subluxations resolve quickly, others can lead to chronic instability and repeated episodes if left untreated.
The term “subluxed” is most commonly used in orthopedic medicine to describe joint injuries, though you may also hear it in dental or chiropractic contexts. In this guide, we focus on the medical understanding of joint subluxations—what causes them, how they’re diagnosed, and the most effective treatment approaches.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon with over 30 years of experience treating joint instability and subluxed joints in southern Minnesota and northern Iowa. As the founder of the Center for Specialty Care in Fairmont, I’ve helped countless patients recover from shoulder, knee, and elbow subluxations through both conservative and surgical treatments.
What is a Subluxation? Causes, Symptoms, and Key Differences
Understanding what it means for a joint to be subluxed is the first step toward effective treatment. It’s a common injury that can affect various joints, leading to discomfort and limiting your daily activities.
Subluxation vs. Dislocation: A Crucial Distinction
When a joint is subluxed, it is partially dislocated. The bones have moved out of their normal alignment but still maintain some contact. In contrast, a complete dislocation (luxation) means the bones are entirely separated. While both cause joint instability, a subluxation is less severe than a complete dislocation, which often involves significant pain and a visible deformity.
To help illustrate the differences, here’s a quick comparison:
| Feature | Subluxation (Partial Dislocation) | Dislocation (Complete Dislocation) |
|---|---|---|
| Definition | Bones partially out of alignment, but still maintain some contact | Bones completely separated, no contact between joint surfaces |
| Severity | Less severe, but still requires medical attention | More severe, often with obvious deformity |
| Symptoms | Pain, swelling, instability, popping/clicking, limited motion | Severe pain, significant swelling, complete loss of function, obvious deformity |
| Joint Contact | Partial contact maintained | No contact maintained |
| Treatment | Often conservative (RICE, physical therapy, reduction) | Requires reduction, often more intensive rehabilitation, sometimes surgery |
Common Causes of Joint Instability
Joint instability, which often leads to a subluxed joint, can stem from several factors:
- Trauma: Acute injuries like falls, direct blows, or sports injuries can force a joint beyond its normal range, stretching or tearing ligaments.
- Repetitive Motion: Overuse can weaken a joint’s supporting structures over time, common in athletes like baseball pitchers or swimmers.
- Joint Laxity: Some individuals have naturally loose ligaments (hypermobility). This can be genetic, related to connective tissue disorders like Ehlers-Danlos syndrome, or temporary, such as during pregnancy.
- Underlying Conditions: Arthritis can damage joint cartilage, while neuromuscular conditions like stroke can cause muscle weakness, both compromising joint stability.
Recognizing the Symptoms
A subluxed joint often presents with a distinct set of symptoms. Recognizing these signs early is key to seeking timely medical attention.
The most common symptom is pain, which can be a dull ache or a sharp sensation. You may also notice swelling and bruising around the joint. Many people report a popping or clicking sound at the time of injury, followed by a feeling that the joint is “loose” or “giving way.” This sensation of instability is a hallmark sign. We often hear patients describe their shoulder making clicking and popping sounds, which can indicate a subluxation. If you’re experiencing shoulder clicking and pain, it’s worth getting it checked out.
Other symptoms include a limited range of motion and, in some cases, numbness or tingling if nerves are compressed. While a visible deformity is more common with complete dislocations, a severe subluxation might also cause a subtle change in the joint’s appearance.
Common Types of Subluxations and At-Risk Groups
While any joint can become subluxed, some are more commonly affected than others, and certain populations face a higher risk. Let’s explore some of the most frequent types of subluxations we treat here at the Center for Specialty Care.
Shoulder Subluxation
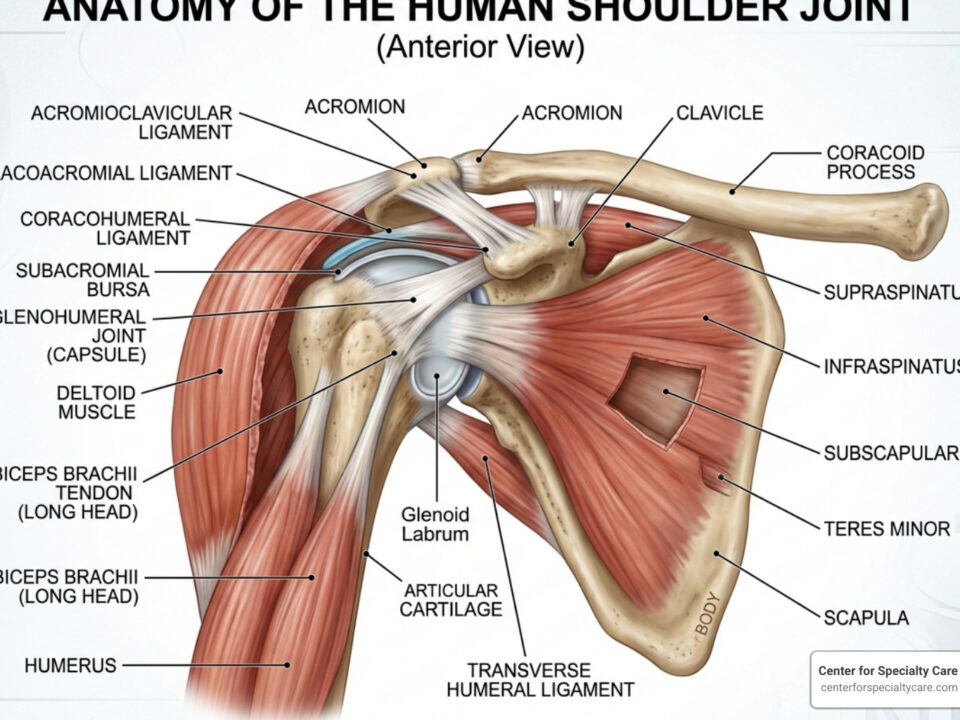
The shoulder is one of the body’s most mobile joints, making it particularly vulnerable to instability and subluxations. A shoulder subluxation occurs when the head of the humerus (upper arm bone) partially slips out of the glenoid (shoulder socket) before returning to its normal position.
This type of injury is incredibly common, especially among athletes. Those involved in sports that require repetitive overhead motions, such as baseball, volleyball, swimming, or tennis, are at a higher risk. The constant stress can stretch the ligaments and joint capsule over time, leading to chronic shoulder instability. For instance, in a study on shoulder subluxations, 45.5% experienced the first subluxation event, while the remaining 54.5% had recurrent shoulder subluxation. This highlights the tendency for these injuries to reoccur once the supporting structures are compromised.
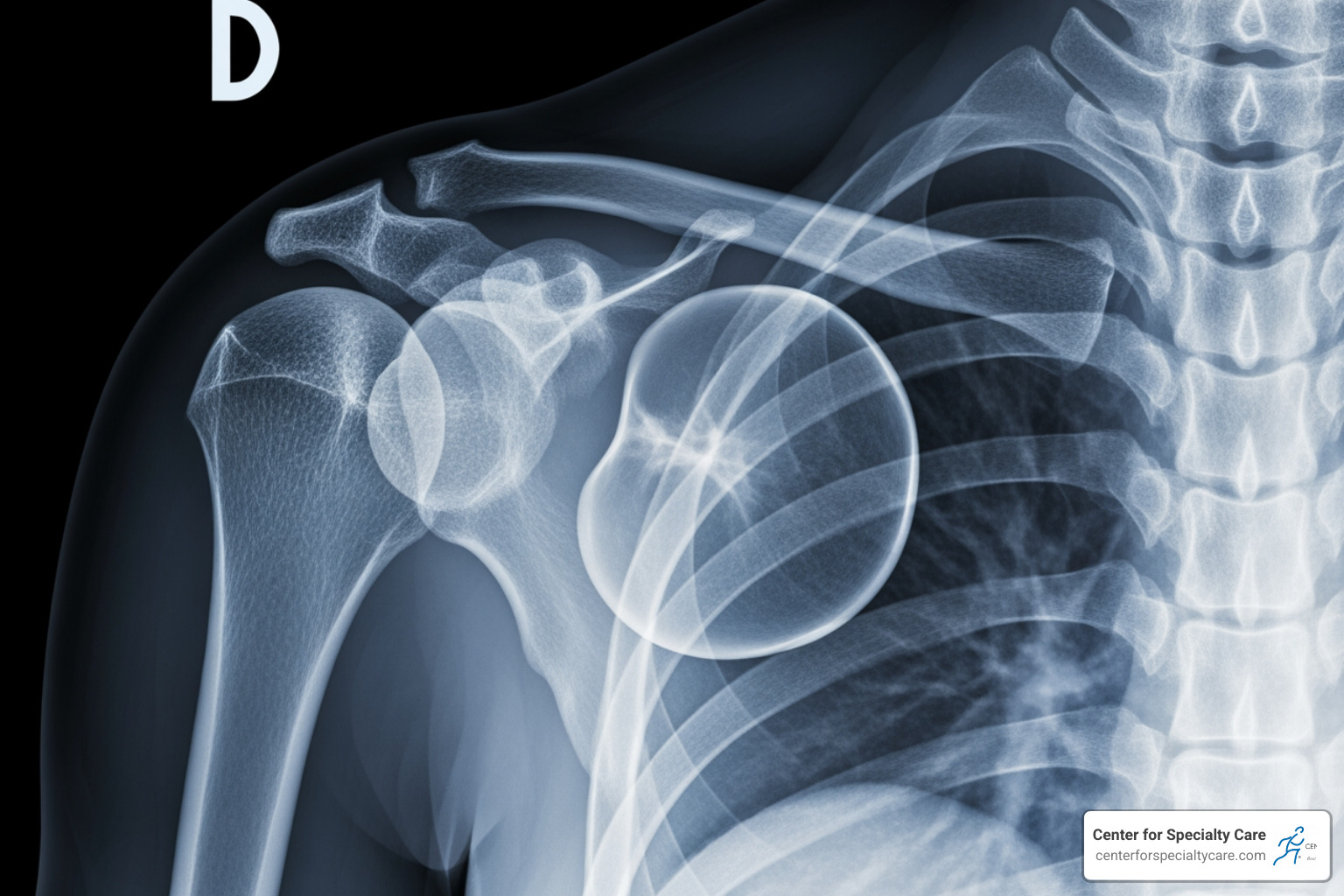
Stroke survivors also frequently experience shoulder subluxations, often due to weakness or paralysis of the muscles supporting the shoulder joint (hemiplegia). The reported incidence in this population varies greatly, from 17% to 81%. This can lead to significant pain and hinder rehabilitation efforts. We offer comprehensive shoulder care and treatment options to help manage and recover from these issues.
The primary causes of shoulder subluxation include:
- Traumatic injury: A fall, direct blow, or sudden twisting motion.
- Rotator cuff weakness: The rotator cuff muscles are crucial for stabilizing the shoulder. If they are weak or injured, the humeral head can become subluxed.
- Ligamentous laxity: Stretched or torn ligaments and a loose joint capsule can allow excessive movement.
- Repetitive microtrauma: Common in athletes, leading to gradual weakening of supporting structures.
Kneecap (Patellar) and Elbow Subluxation
Beyond the shoulder, the kneecap and elbow are other joints that frequently experience subluxations.
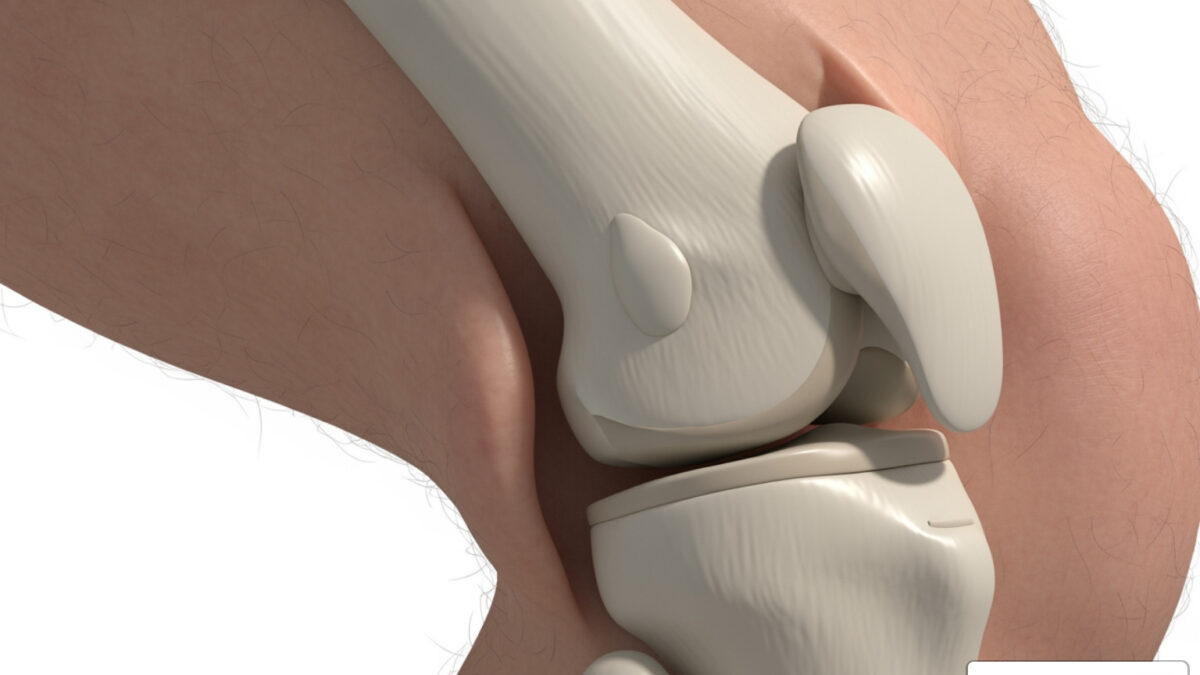
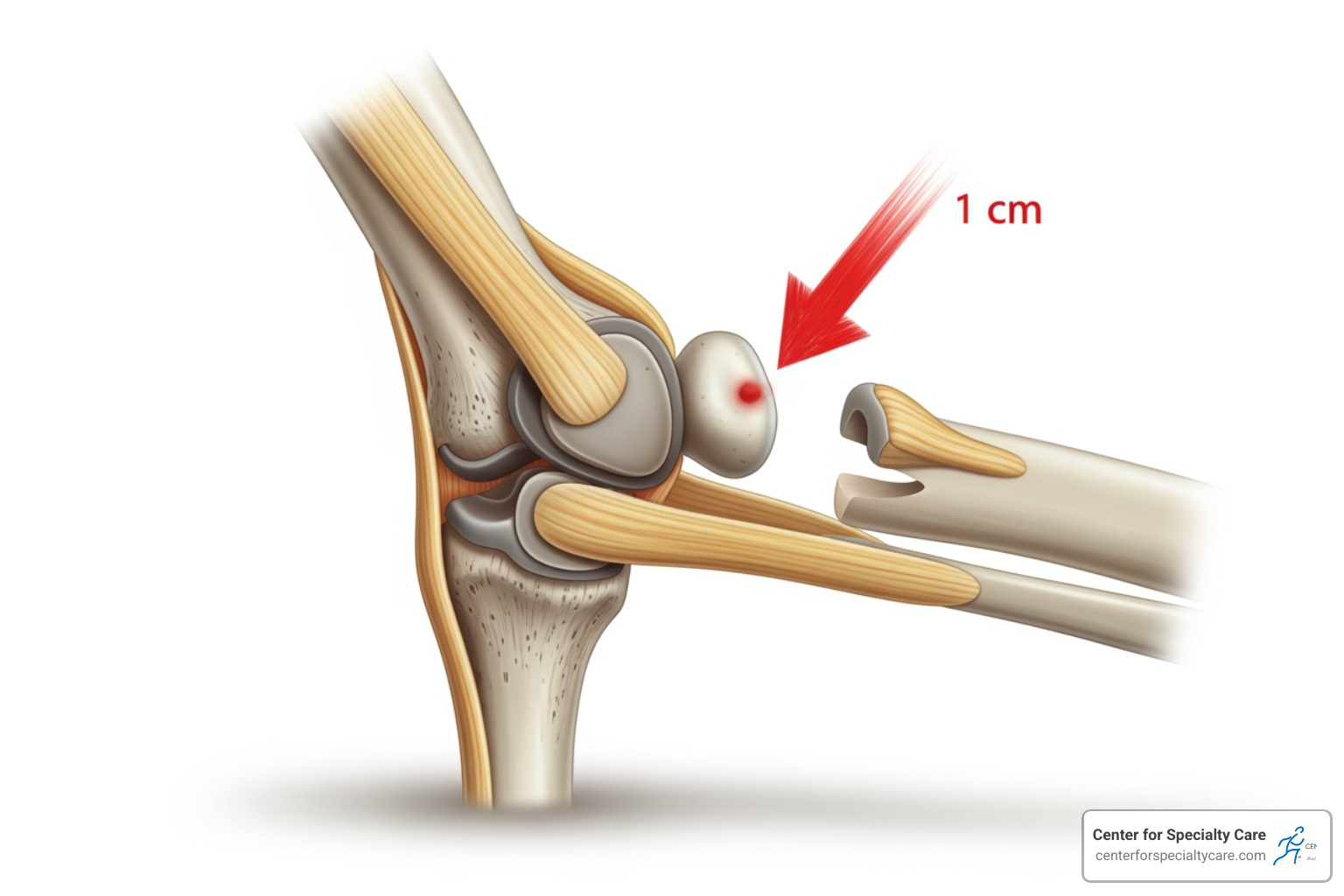
Patellar instability, or a subluxed kneecap, occurs when the patella (kneecap) partially slides out of its groove on the femur (thigh bone). This is particularly common in children and adolescents, especially during growth spurts when muscles and ligaments may not keep pace with bone growth. A direct impact to the knee, a twisting motion, or even certain anatomical factors (like a shallow patellar groove) can cause the kneecap to shift. Fortunately, we provide specialized care for patellar dislocation and instability in children, helping our younger patients regain stability and confidence.
The elbow joint can also be subluxed, with one of the most well-known examples being Nursemaid’s elbow. This common injury in young children (typically under the age of five) occurs when the radial head (the top of the forearm bone) partially slips out of the annular ligament that holds it in place. It often happens when a child’s arm is pulled suddenly, such as by a parent lifting them by the hand or swinging them. The good news is that Nursemaid’s elbow can usually be easily reduced (put back into place) by a medical professional with a simple maneuver.
Other Forms: Spinal
While we primarily focus on orthopedic care, it’s worth noting that the term subluxation can also apply to other areas. However, for our scope, we will concentrate on the spine.
Spinal subluxations refer to a partial misalignment of vertebrae in the spinal column. This can occur due to trauma, degenerative conditions, or inflammatory diseases like rheumatoid arthritis. For example, atlanto-axial subluxation is a condition where the first two vertebrae in the neck (atlas and axis) become partially misaligned. This can be particularly serious because it affects the stability of the upper cervical spine, which houses the spinal cord. Conditions like rheumatoid arthritis can weaken the ligaments in the cervical spine, increasing the risk of such subluxations.
If you’re an athlete and concerned about spinal health or any joint instability, we invite you to learn more about our sports medicine services.
Diagnosis and Treatment: Your Path to Recovery from a Subluxed Joint
Experiencing a subluxed joint can be unsettling, but with proper diagnosis and treatment, most individuals make a full recovery. At Center for Specialty Care, our goal is to get you back to your active life as quickly and safely as possible.
How Doctors Diagnose a Subluxation
When you come to us with a suspected subluxation, our first step is a thorough diagnostic process. This typically begins with a detailed physical examination and taking a comprehensive patient history. We’ll ask about how the injury occurred, your symptoms, and any previous joint issues.
During the physical exam, we will carefully assess the affected joint for tenderness, swelling, range of motion, and stability. For shoulder subluxations, specific tests like the Apprehension test (which checks for a feeling of impending dislocation) and the Load and Shift test (which assesses the amount of translation of the humeral head) are often performed. These tests help us determine the direction and degree of instability.
To confirm the diagnosis and rule out other injuries like fractures, we often rely on imaging studies.
- X-rays provide clear images of bones and can show if there’s any displacement or fracture.
- MRI (Magnetic Resonance Imaging) is excellent for visualizing soft tissues, including ligaments, tendons, cartilage, and the joint capsule, helping us identify any tears or damage.
- CT (Computed Tomography) scans offer detailed cross-sectional images, which can be particularly useful for assessing bone injuries or complex joint anatomy.
By combining your clinical history, physical findings, and advanced imaging, we can accurately diagnose your subluxation and develop the most effective treatment plan. To learn more about how we diagnose and treat various musculoskeletal conditions, please visit our orthopedics services page.
Non-Surgical Treatment and Rehabilitation
For many subluxations, especially initial episodes or less severe cases, non-surgical treatment and rehabilitation are highly effective. Our approach focuses on reducing pain, restoring joint stability, and preventing future occurrences.
The immediate management often involves manual reduction, where a healthcare professional gently maneuvers the bones back into their proper alignment. This should never be attempted at home, as improper technique can cause further damage.
Following reduction, we typically recommend the RICE protocol:
- Rest: Avoid activities that aggravate the joint to allow healing.
- Ice: Apply ice packs to reduce swelling and pain. We advise applying ice for no more than 15-20 minutes several times a day, using a cloth barrier to protect your skin.
- Compression: Use elastic bandages to help control swelling and provide support.
- Elevation: Keep the injured joint liftd above your heart to reduce fluid accumulation.
Immobilization with a splint, brace, or cast may be necessary for a period to protect the joint and allow ligaments and other soft tissues to heal. This helps prevent the joint from becoming subluxed again during the initial recovery phase.
Pain management is also a key component. Over-the-counter NSAIDs (non-steroidal anti-inflammatory drugs) like ibuprofen can help reduce pain and inflammation. In some cases, stronger prescription pain medication may be prescribed.
The cornerstone of long-term recovery from a subluxed joint is physical therapy. Our experienced physical therapists in Fairmont, Estherville, Buffalo Center, and St. James will guide you through a customized rehabilitation program designed to:
- Restore full range of motion.
- Strengthen the muscles surrounding the joint (e.g., rotator cuff muscles for shoulder subluxations).
- Improve motor control and coordination.
- Improve proprioception (your body’s sense of joint position).
- Stabilize the joint, especially through exercises for scapular stabilization in shoulder cases.
This comprehensive approach helps rebuild the strength and stability needed to prevent future subluxations. We are dedicated to providing excellent shoulder treatment with physical therapy for your recovery and pain relief.
When is Surgery Necessary?
While non-surgical methods are often successful, there are situations where surgery becomes the best option to address a subluxed joint and restore long-term stability. We consider surgical intervention when conservative treatments have not yielded the desired results, or when the nature of the injury itself indicates a need for repair.
Common indications for surgery include:
- Recurrent instability: If your joint repeatedly becomes subluxed despite consistent physical therapy and conservative management, surgical stabilization may be necessary.
- Severe ligament or labrum tears: Significant damage to the stabilizing ligaments or the labrum (a rim of cartilage in joints like the shoulder or hip) often requires surgical repair to restore structural integrity.
- Failed conservative treatment: When a prolonged course of non-surgical care doesn’t alleviate symptoms or improve joint function, surgery might be recommended.
Our surgeons use advanced techniques, including both arthroscopic surgery and open repair. Arthroscopy is a minimally invasive procedure where small incisions are made, and a tiny camera (arthroscope) is used to visualize and repair the joint. This often results in less pain and a faster recovery compared to traditional open surgery, which involves a larger incision to access the joint directly. The specific surgical approach will depend on the type of subluxation, the extent of the damage, and your individual needs.
Common procedures for stabilizing a subluxed joint include:
- Bankart repair: For shoulder subluxations, this involves reattaching the torn labrum and tightening the stretched capsule.
- Capsular shift: A procedure to tighten the joint capsule, often used for generalized joint laxity.
- Ligament reconstruction: Repairing or replacing severely damaged ligaments.
Our team of expert surgeons is committed to providing the highest quality care. You can find more information about our surgery options and how we can help you regain stability and function.
The “Vertebral Subluxation” Controversy: Medical Fact vs. Theory
The term subluxation can cause confusion when discussing spinal health. It’s important to distinguish between the medical definition of a subluxed vertebra and the theoretical concept of “vertebral subluxation” used in some chiropractic philosophies.
The Medical Definition of a Subluxed Vertebra
In medicine, a subluxed vertebra is a partial, structural dislocation of a spinal bone that is visible on imaging like an X-ray or MRI. These are serious conditions, typically caused by significant trauma (like a car accident) or diseases such as rheumatoid arthritis. A medically diagnosed subluxation can compress the spinal cord or nerves, leading to pain, numbness, or weakness. For example, a cervical subluxation is a highly unstable injury that requires prompt medical attention to prevent spinal cord damage, as detailed in scientific research on the condition.
The Chiropractic Theory vs. Scientific Consensus
In contrast, some chiropractic theories use “vertebral subluxation” to describe subtle misalignments believed to interfere with nerve function and overall health. This theoretical condition is generally not a visible or measurable displacement on standard medical imaging.
The mainstream medical and scientific consensus, including the World Health Organization (WHO), defines a subluxation as a significant, structural displacement visible on imaging. The theoretical chiropractic concept lacks this verifiable evidence and is not recognized as a medical diagnosis.
At Center for Specialty Care, our protocols are based on evidence-based medicine, focusing on verifiable conditions with proven treatments.
Frequently Asked Questions about Joint Subluxations
Here, we address some of the most common inquiries we receive from our patients about a subluxed joint.
Can a subluxation heal on its own?
While a joint might slip back into place on its own (spontaneous reduction), the underlying injury to the ligaments and joint capsule remains. Without proper healing, these tissues can stay weakened, leading to chronic instability and a high risk of future subluxations or dislocations. It is crucial to seek a medical evaluation even if the joint feels better, to assess the damage and create a rehabilitation plan to prevent long-term problems.
What does a subluxed joint feel like?
A subluxed joint often causes a distinct popping or shifting sensation at the moment of injury, followed by sudden pain. Patients frequently describe a persistent feeling of looseness or instability, as if the joint is “out of place” or might “give way.” Depending on the severity, you might also experience swelling, temporary numbness, tingling, or weakness in the limb.
How long does it take to recover from a subluxation?
Recovery time varies widely based on the joint, injury severity, and treatment plan. A minor subluxation may heal in a few weeks with rest and physical therapy. However, more severe cases, especially those with significant ligament damage or requiring surgery, can take several months to fully recover. Our team provides a personalized recovery timeline to guide you through each stage of rehabilitation for the best possible outcome.
Conclusion: Prevention and Expert Care for Joint Instability
Dealing with a subluxed joint is challenging, but it doesn’t have to be a permanent setback. With the right care, recovery and long-term joint health are achievable. Prevention is key, and strategies like targeted strengthening exercises, using proper body mechanics, and managing underlying conditions can significantly reduce your risk.
The prognosis for most subluxations is good, especially with an accurate diagnosis and timely treatment. Early intervention is the best way to prevent chronic instability and recurring injuries.
At Center for Specialty Care, our expert team uses advanced diagnostics to pinpoint the exact nature of your subluxation. We then create a personalized treatment plan, ranging from conservative care like physical therapy to surgical intervention when necessary.
We offer comprehensive orthopedic and pain management care for patients across Fairmont MN, Estherville IA, Buffalo Center IA, and St James MN. Our commitment to patient satisfaction, personalized care, and quick appointments makes us your trusted partner in health. Don’t let joint instability hold you back. If you suspect you have a subluxed joint, seek our specialized care to regain mobility and live a pain-free life.