
Beyond the Ache: Discovering the Best Pain Management Solutions
February 13, 2026
Twist and Shout No More: How to Sleep with Rotator Cuff Pain
February 18, 2026Chronic Pain Management: Your 2026 Guide to Relief
Why Chronic Pain Management Matters for Your Quality of Life
Chronic pain management is the ongoing process of reducing pain intensity, maximizing daily function, and improving quality of life through a combination of medical treatments, lifestyle changes, and self-care strategies—rather than simply trying to eliminate pain completely.
Quick Answer: What is Chronic Pain Management?
- Goal: Reduce pain and improve function, not necessarily eliminate pain entirely
- Approach: Multidisciplinary team (doctors, physical therapists, psychologists)
- Treatments: Exercise, physical therapy, medications, psychological therapies, lifestyle changes
- Timeline: Ongoing process requiring active participation
- Focus: Maximizing quality of life and daily activities
If you’re one of the 3 out of 10 people in the U.S. living with chronic, persistent pain, you know how deeply it affects your life. Chronic pain can last for weeks, months, or even years—and it’s one of the most common reasons people seek healthcare.
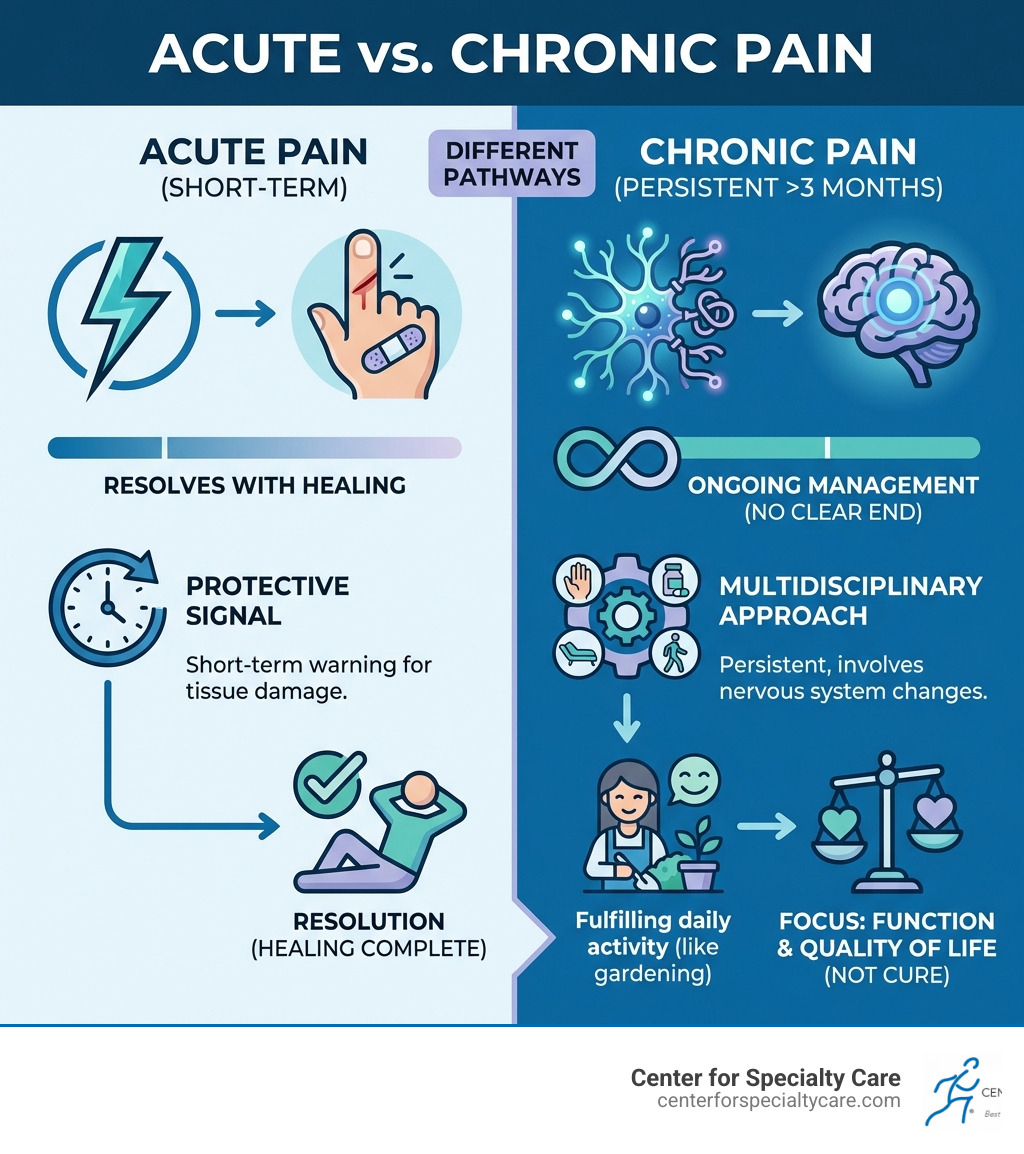
Unlike acute pain that signals tissue damage and resolves as you heal, chronic pain is a distinct condition. It’s a disease process in itself, often involving changes in your nervous system that make pain persist long after an initial injury has healed.
But here’s the important news: effective management is possible. While complete elimination of pain is rarely achievable for any substantial period, reducing pain, maximizing your ability to function, and improving your overall quality of life are realistic goals.
The journey requires a comprehensive approach—one that addresses not just the physical aspects of pain, but also the psychological, social, and lifestyle factors that influence your experience. From supervised exercise programs and cognitive behavioral therapy to careful medication management and stress reduction techniques, today’s chronic pain management offers many paths to relief.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon who has specialized in musculoskeletal pain relief and minimally invasive surgical techniques for over three decades here in Fairmont, Minnesota. Through my work at the Center for Specialty Care, I’ve guided countless patients through comprehensive chronic pain management programs that combine medical expertise with personalized, multidisciplinary care to help them reclaim their quality of life.
Chronic pain management terms you need:
Understanding Your Pain: Diagnosis, Causes, and Goals

When we talk about chronic pain management, we’re referring to pain that lasts for more than three to six months, often extending beyond the expected healing time for an injury or illness. This persistent discomfort can be incredibly frustrating, especially when its origin isn’t immediately clear. It’s a complex condition, involving a mix of physical, psychological, and social factors.
What are the common causes of chronic pain?
Chronic pain can stem from a variety of sources, and sometimes, no single cause can be identified. Here are some of the common culprits we see:
- Underlying diseases: Conditions like rheumatoid arthritis or osteoarthritis are frequent causes of chronic joint pain. Other diseases, such as diabetes, can lead to neuropathic pain.
- Past injuries: While acute pain from an injury typically resolves, sometimes the nervous system continues to send pain signals long after the physical damage has healed. This can happen with issues affecting the back spine, shoulder, knee, or hip.
- Central sensitization: When pain persists, the central nervous system (brain and spinal cord) can become hypersensitive. This means it amplifies pain signals, making it difficult to pinpoint the exact location or cause of discomfort. Think of it like a city that develops multiple highways to handle traffic – the pain pathways become more complex and active.
- Neuropathic changes: Damage to nerves themselves can lead to chronic burning, tingling, or shooting pain, often seen in conditions like sciatica or diabetic neuropathy. We can manage radiating pain with targeted treatments.
- Musculoskeletal issues: Chronic conditions affecting muscles, bones, and joints, such as fibromyalgia or ongoing low back pain, are common sources of persistent discomfort.
- Inflammatory conditions: Chronic inflammation, whether from autoimmune diseases like rheumatoid arthritis or from lifestyle factors, can contribute significantly to ongoing pain.
How is chronic pain diagnosed?
Diagnosing chronic pain is a comprehensive process. Unlike a broken bone that shows up clearly on an X-ray, pain is a subjective experience. There’s no single diagnostic test that definitively measures your pain level. Instead, we rely on a detailed evaluation that considers your unique experience:
- Comprehensive evaluation: This involves a thorough review of your medical history, including any past injuries, surgeries, or underlying conditions. We’ll also discuss your lifestyle, work, and how pain impacts your daily activities.
- Patient history: We’ll ask you to describe your pain in detail: its location, intensity (often on a 0-10 scale), quality (e.g., sharp, dull, burning), frequency, and what makes it better or worse. We might use tools like the PEG scale to assess pain intensity and its interference with enjoyment and general activity. Scientific research on pain assessment emphasizes the importance of these patient-reported measures.
- Physical and neurological exams: Our providers will conduct a physical examination to assess your mobility, strength, reflexes, and sensation. This helps us identify any physical limitations or nerve involvement.
- Diagnostic imaging (MRI, X-ray): While these don’t directly show “pain,” they can reveal structural issues like disc herniations, arthritis, or fractures that might be contributing to your discomfort. Our facility offers MRI, Bone Density, X-Ray, Nerve Conduct services, including open-sided MRI for a more comfortable experience.
- Pain diaries: We might ask you to keep a pain journal to track your symptoms, triggers, and the effectiveness of different coping strategies. This helps us get a clearer picture of your pain patterns over time.
- Assessing functional impairment: Beyond pain intensity, we evaluate how pain affects your ability to perform daily tasks, work, and engage in hobbies. This helps us tailor your chronic pain management plan to improve your quality of life.
The Primary Goals of Chronic Pain Management
It’s important to set realistic expectations. For most chronic pain conditions, the complete elimination of pain is rarely obtainable for any substantial period. Instead, our primary goals for chronic pain management are:
- Pain reduction: Our aim is to significantly decrease your pain to a more tolerable level, making it less disruptive to your life.
- Maximizing daily function: We focus on improving your ability to perform daily activities, return to work, and engage in the things you enjoy, even if some pain persists.
- Improving quality of life: This is paramount. We want to help you live a fulfilling life, reduce the emotional toll of pain, and improve your overall well-being.
- Realistic expectations: We’ll work with you to understand what’s achievable and empower you with tools and strategies to manage your pain long-term.
- Self-management skills: A key goal is to equip you with the knowledge and techniques to actively participate in your own care, giving you more control over your pain journey.
Building Your Team: A Multidisciplinary Approach
Effective chronic pain management is rarely a solo act. For complex cases, we believe in a multidisciplinary, team-based approach. This means bringing together various healthcare professionals to address all facets of your pain – physical, emotional, and social. This holistic care leads to better outcomes and reduces stress on any single provider.
Our team might include:
- Pain specialists: Physicians like those at Center for Specialty Care who specialize in diagnosing and treating chronic pain conditions, often utilizing interventional procedures.
- Physical therapists: Experts in movement and function, helping you regain strength, flexibility, and mobility. We have a dedicated physical therapy department ready to assist you.
- Psychologists or behavioral health specialists: Addressing the mental health aspects of chronic pain, including coping strategies, anxiety, and depression.
- Nutritionists: Guiding you on dietary changes that can reduce inflammation and support overall health.
The Vicious Cycle of Chronic Pain and Mental Health
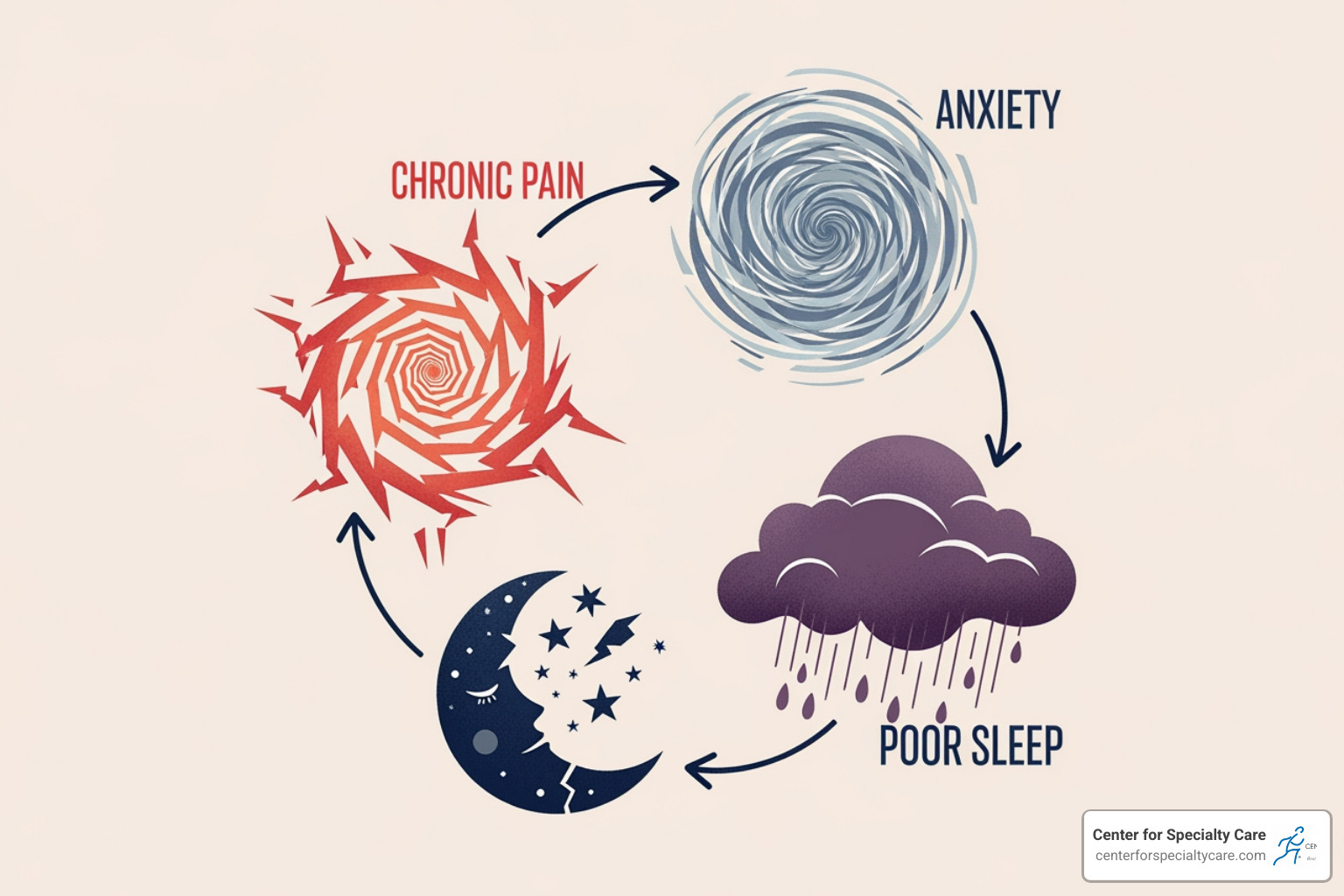
Chronic pain is not just a physical sensation; it deeply impacts your mental and emotional well-being. In fact, chronic pain is linked to anxiety and depression, and it can significantly limit people’s ability to work or do other activities. Research shows well-established associations among chronic pain, substance use disorders (SUDs), and mental disorders like depression, anxiety, and PTSD.
- Pain-depression link: It’s a cruel cycle. Living with constant pain can lead to feelings of hopelessness, sadness, and withdrawal, often escalating into depression. Conversely, depression can lower your pain threshold, making existing pain feel even worse. Depression and anxiety disorders are four times more likely among patients with chronic pain than pain-free patients.
- Anxiety and stress amplification: Chronic pain often comes with chronic stress and anxiety about the pain itself, its impact on your life, and the uncertainty of the future. This anxiety can heighten your nervous system’s reactivity, amplifying pain signals.
- PTSD: Psychological trauma, such as that experienced by some veterans, is a significant risk factor for chronic pain and for the transition from acute to chronic pain.
- Coping strategies: Untreated psychopathology is associated with poor pain treatment outcomes. This is why addressing mental health is a crucial part of chronic pain management. Our behavioral health services can provide more info about our behavioral health services.
Active Participation in Your Chronic Pain Management Plan
You are the most important member of your healthcare team! Your active participation is key to successful chronic pain management. Here’s how you can take charge:
- Shared decision-making: We believe in empowering you to make informed choices about your care. We’ll present all available options, discuss their benefits and risks, and help you decide on a plan that aligns with your values and goals.
- Tracking symptoms and triggers: Keeping a pain journal (even a simple one on your phone) can help you identify patterns, understand what makes your pain better or worse, and effectively communicate this information to your providers.
- Open communication with providers: Don’t hesitate to share your concerns, progress, and challenges. The more information we have, the better we can tailor your treatment.
- Setting personal, functional goals: Instead of solely focusing on eliminating pain, let’s work together to set goals like “walking to the mailbox without severe pain” or “being able to play with my grandchildren for 30 minutes.” These achievable milestones can significantly improve your quality of life.
- Being your own advocate: Ask questions, seek clarification, and ensure your voice is heard. This is your journey to relief.
Special Considerations for Veterans and High-Risk Groups
We understand that certain populations face unique challenges in chronic pain management.
- Veterans and PTSD: Sadly, nearly all Gulf War Veterans referred to the War Related Illness and Injury Study Center (WRIISC) report chronic pain as one of their top complaints. The link between psychological trauma (like PTSD) and chronic pain is well-established. For these individuals, a sensitive and integrated approach that addresses both physical pain and mental health is paramount. The VA offers valuable resources for Proactive Pain Management for Veterans.
- History of Substance Use Disorder (SUD): Managing chronic pain in individuals with a history of SUD, or active addiction, is particularly complex. Research shows well-established associations among chronic pain, SUDs, and mental disorders. The presence of active addiction makes successful treatment of chronic pain improbable. Our approach prioritizes non-opioid treatments and a coordinated care plan with addiction specialists if needed. We use risk assessment tools and careful monitoring to ensure safety and prevent relapse.
Beyond the Pill: Effective Non-Pharmacological Strategies
Medication certainly has its place in chronic pain management, but it’s far from the only tool—and often not the primary one. Many non-pharmacological approaches can provide significant relief, improve function, and improve your quality of life with fewer side effects.
Physical therapy
This is often one of the first and most effective lines of defense against chronic pain. Our physical therapy team in Fairmont and St. James, Minnesota, and Estherville, Iowa, focuses on helping you regain strength, flexibility, and proper movement patterns.
- Supervised exercise programs: We offer supervised group exercise programs to help people aged 16 and over manage chronic primary pain. Low-impact exercises like walking, swimming, or cycling can strengthen muscles, improve circulation, and boost your body’s natural pain-fighting chemicals.
- Manual therapy: Techniques such as massage, mobilization, and manipulation performed by a physical therapist can help reduce muscle tension, improve joint movement, and alleviate pain.
- Improving mobility and strength: The goal isn’t just to reduce pain, but to get you moving better and stronger. This can involve targeted exercises for your shoulder, knee, back, or other affected areas. Many widely used physical therapy interventions, while sometimes lacking definitive evidence for specific modalities, have the advantage of being non-surgical, low-risk, and encouraging patient involvement.
Psychological Therapies for Pain
Your mind plays a powerful role in how you experience and cope with pain. Psychological therapies don’t suggest your pain is “all in your head,” but rather help you change your relationship with pain, reducing its impact on your life.
- Cognitive Behavioral Therapy (CBT): This therapy helps you identify and change negative thought patterns and behaviors related to your pain. It teaches coping skills, such as relaxation techniques and problem-solving, to reduce pain-related distress, disability, depression, and anxiety. We consider CBT for people aged 16 and over with chronic primary pain.
- Acceptance and Commitment Therapy (ACT): ACT focuses on accepting unavoidable pain sensations while committing to actions that align with your values. It helps you live a rich and meaningful life despite the pain, rather than constantly fighting against it. ACT can be considered for people aged 16 and over with chronic primary pain.
- Mindfulness-Based Stress Reduction (MBSR): Mindfulness techniques teach you to be present with your pain without judgment, reducing reactivity and cultivating a sense of calm.
- Biofeedback: This technique helps you gain control over involuntary bodily functions (like heart rate or muscle tension) that can influence pain, allowing you to learn to relax and reduce pain responses.
Complementary and Integrative Approaches
Many people find relief through complementary and alternative medicine (CAM) therapies. Surveys show that 27–60 percent of chronic pain patients use CAM.
- Acupuncture: This ancient practice involves inserting thin needles into specific points on the body. We consider a single course of acupuncture or dry needling for people aged 16 and over to manage chronic primary pain.
- Dry needling: Similar to acupuncture, this technique uses fine needles to target trigger points in muscles, releasing tension and reducing pain.
- Massage therapy: Therapeutic massage can relieve muscle tension, improve circulation, and promote relaxation, which can be beneficial for various types of chronic pain.
- Yoga and Tai Chi: These mind-body practices combine gentle movement, stretching, and breathing exercises. They can improve flexibility, strength, balance, and reduce stress, all of which contribute to better pain management.
Before trying any new complementary therapy, it’s always best to discuss it with your healthcare provider. Here are some questions to ask:
- Is this therapy safe for my specific condition?
- Are there any potential interactions with my current medications?
- What are the expected benefits and risks?
- How many sessions are typically recommended?
- What is the cost, and is it covered by insurance?
The Role of Medication in Chronic Pain Management
Medication is a powerful tool in our chronic pain management toolbox, but it’s important to remember it’s just one tool. It’s rarely a standalone solution, and for chronic pain, medication alone is often not enough. Our approach always involves a regular review with your doctor and strict adherence to prescribing guidelines to ensure safety and effectiveness.
Non-Opioid Medications
For most chronic pain conditions, non-opioid medications are the first line of pharmacological treatment. They offer pain relief with a lower risk profile than opioids.
| Medication Type | Goals | Risks Pears for the management of chronic pain.
The Power of Lifestyle: How Daily Habits Impact Pain
Our daily habits significantly influence our overall health, and this is especially true for those living with chronic pain. Embracing a healthy lifestyle can reduce inflammation, improve mood, and boost your body’s natural ability to cope with pain.
Anti-inflammatory Diet
The food we eat can either fuel or fight inflammation in our bodies. An anti-inflammatory diet focuses on whole, unprocessed foods and can be a powerful ally in chronic pain management.
- Include: Plenty of fruits and vegetables, lean proteins (especially fatty fish rich in omega-3s), whole grains, and healthy fats like olive oil.
- Limit: Processed foods, excessive sugar, unhealthy trans fats, and refined carbohydrates, which can contribute to inflammation.
Sleep Hygiene
Good quality sleep is crucial for pain management. Sleep complaints occur in 67–88% of individuals with chronic pain, and poor sleep can exacerbate pain perception and interfere with healing.
- Establish a routine: Go to bed and wake up at the same time each day, even on weekends.
- Create a comfortable sleep environment: Ensure your bedroom is dark, quiet, and cool.
- Avoid stimulants: Limit caffeine and alcohol, especially close to bedtime.
- Use your bed for sleep and intimacy only: Avoid working or watching TV in bed to help your brain associate the space with rest.
Stress Management Techniques
Stress is a known amplifier of pain. Learning to manage stress effectively can significantly improve your pain experience.
- Mindfulness and meditation: Practicing mindfulness, focusing on the present moment without judgment, can reduce stress and alter your perception of pain.
- Deep breathing exercises: Simple breathing techniques can calm your nervous system and reduce muscle tension.
- Engage in hobbies: Sometimes, taking your mind off the symptoms by engaging in a favorite hobby or social interaction can help reduce stress and improve pain management.
- Regular physical activity: Even gentle exercise can be a great stress reliever.
Quitting Smoking
Smoking restricts blood flow, which prevents healing and can worsen chronic pain. If you smoke, quitting is one of the most impactful steps you can take for your overall health and pain management. The VA offers valuable information on quitting smoking and resources to help you on your journey.
Emerging and Advanced Treatments
The field of chronic pain management is constantly evolving, with new research and technologies offering hope for those whose pain has been resistant to traditional treatments.
- Neuroplasticity concepts: This involves understanding how the brain can rewire itself in response to pain. Therapies based on neuroplasticity aim to “retrain” the brain to reduce pain signals and improve function.
- Repetitive Transcranial Magnetic Stimulation (rTMS): This non-invasive procedure uses magnetic fields to stimulate nerve cells in the brain. VA researchers at the VA Palo Alto Health Care System are studying whether symptoms of chronic pain can be improved using rTMS. This could be a promising avenue for many. You can learn more about VA research on emerging pain treatments.
- Spinal cord stimulators (SCS): For certain types of chronic pain, particularly neuropathic pain or failed back surgery syndrome, SCS devices can be implanted. These devices deliver mild electrical pulses to the spinal cord, which interfere with pain signals traveling to the brain, replacing pain with a tingling sensation or, with newer technology, no sensation at all. Our pain specialists offer spinal cord stimulation as a treatment option.
- The future of pain research: We are continually following the latest scientific advancements to bring the most effective and innovative treatments to our patients.
Conclusion: Taking the First Step Toward Relief
Navigating the complexities of chronic pain can feel overwhelming, but we hope this guide has illuminated the many pathways to relief. Effective chronic pain management is not about a quick fix; it’s an active, ongoing process that requires patience, persistence, and a willingness to explore various strategies.
We’ve seen that by understanding your pain, building a supportive multidisciplinary team, exploring non-pharmacological therapies, carefully managing medications, and embracing healthy lifestyle habits, you can significantly reduce your pain, maximize your function, and dramatically improve your quality of life.
You are not alone in this journey. Millions of Americans live with chronic pain, and specialized care is available. Empowerment comes from knowledge and active participation in your treatment plan.
For a personalized and comprehensive treatment plan, the team at Center for Specialty Care in Fairmont, Minnesota, Estherville, Iowa, Buffalo Center, Iowa, and St. James, Minnesota, is ready to help. Our commitment to 100% patient satisfaction, personalized care, and quick appointment availability means you can start your journey to relief sooner. We’re here to guide you every step of the way. Learn more info about our pain management services and schedule your consultation today.




