
Beyond the Ache: Comprehensive Strategies for Rotator Cuff Pain Relief
October 16, 2025
A-Z Guide to Heat for Tendonitis
October 20, 2025Comprehensive Pain Treatment: Your 2025 Ultimate Relief
Why Comprehensive Pain Treatment Changes Lives
Comprehensive pain treatment represents a complete shift from traditional single-approach pain management to addressing every aspect of how pain affects your life. Rather than simply masking symptoms with medication, this integrated approach combines multiple therapies to target the root causes of pain while helping you regain function and improve quality of life.
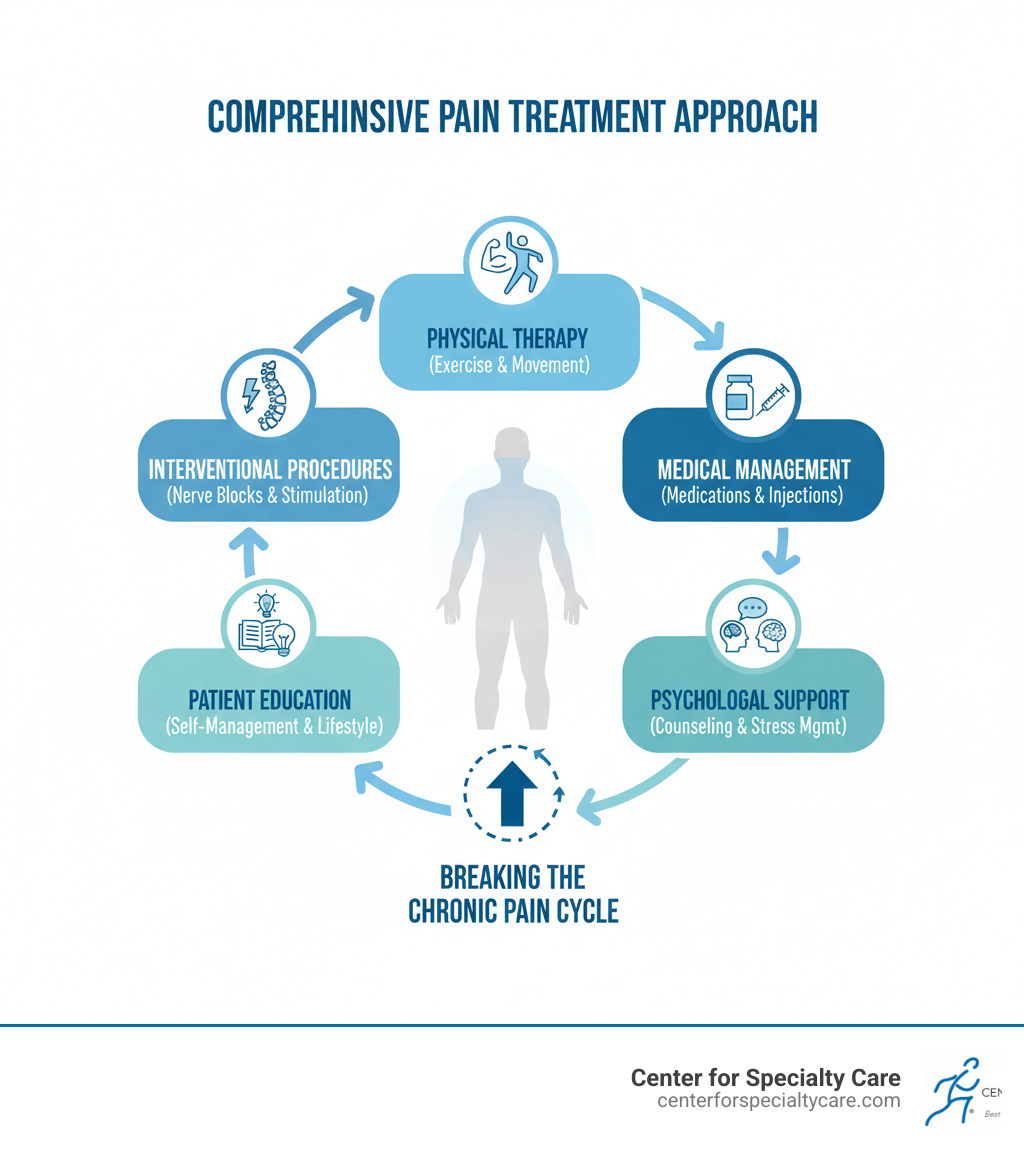
Key Components of Comprehensive Pain Treatment:
- Physical therapies – Exercise, massage, heat/cold therapy
- Medical management – Non-opioid medications, targeted injections
- Psychological support – Cognitive behavioral therapy, mindfulness training
- Interventional procedures – Nerve blocks, spinal cord stimulation
- Patient education – Self-management strategies, lifestyle modifications
The impact of untreated chronic pain extends far beyond physical discomfort. Research shows that 4 billion workdays are lost annually due to pain, highlighting how pain affects not just individuals but entire communities. Chronic pain lasting more than three months becomes a syndrome that changes your nervous system, creating a cycle where pain leads to reduced activity, emotional distress, and heightened pain perception.
Unlike acute pain that warns you about injury, chronic pain serves no protective purpose. It becomes a disease itself, requiring comprehensive treatment that addresses the physical, emotional, and social aspects of your condition. Studies consistently show that comprehensive pain programs offer more effective and cost-effective treatment compared to single-modality approaches alone.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon with over three decades of experience treating musculoskeletal conditions in southern Minnesota and northern Iowa. Through my work at the Center for Specialty Care, I’ve witnessed how comprehensive pain treatment transforms lives by combining surgical expertise with multidisciplinary rehabilitation and pain management strategies.
Glossary for comprehensive pain treatment:
Understanding Your Pain: The Difference Between Acute and Chronic
When you stub your toe on the coffee table, you know exactly what that sharp, immediate pain means – and thankfully, it fades quickly. But what happens when pain doesn’t follow the rules? Understanding why some pain heals while other pain lingers is crucial for finding the right path to relief.

Acute pain acts like your body’s built-in warning system. When you touch something hot or twist your ankle, that immediate, sharp sensation tells you “Stop! Something’s wrong!” This type of pain has a clear purpose – it’s your nervous system’s way of protecting you from further harm.
Acute pain typically has clear characteristics: it starts suddenly, feels intense, and most importantly, it goes away as your body heals. Whether it’s a cut on your finger or shoulder pain from a weekend sports injury, acute pain serves its purpose and then fades as the underlying tissue damage repairs itself.
Chronic pain, however, tells a completely different story. This is pain that overstays its welcome – lasting more than three months or persisting long after the original injury should have healed. Unlike acute pain’s helpful warning signal, chronic pain often serves no protective purpose. Instead, it becomes a condition unto itself.
Think of chronic pain as a fire alarm that won’t stop ringing even when there’s no fire. Your nervous system gets stuck in a pain loop, continuing to send distress signals even when the original problem has been resolved. This happens because chronic pain actually changes how your nervous system works.
The Shift from Symptom to Condition
Here’s where things get particularly complex – and why comprehensive pain treatment becomes so important. When pain persists, your nervous system undergoes fundamental changes through a process called central sensitization.
Imagine your pain signals are like volume controls that get stuck on “high.” Your nerves become hypersensitive, overreacting to normal sensations and amplifying pain signals throughout your body. What once felt like a gentle touch might now feel uncomfortable or even painful.
This process literally rewires your brain. Areas responsible for processing pain expand and become more active, while regions that normally help control pain become less effective. It’s not “all in your head” – these are real, measurable changes in your nervous system.
The persistence of pain signals creates a domino effect throughout your life. Depression and anxiety often develop as your brain struggles to cope with constant discomfort. Your sleep becomes disrupted, creating a vicious cycle where poor rest makes pain worse, and worse pain makes sleep even more elusive.
Many people also experience what we call pain avoidance – you naturally start limiting activities that might trigger discomfort. While this seems logical, it often leads to muscle weakness, reduced flexibility, and ironically, more pain over time.
Understanding these complex changes explains why treating chronic pain requires more than just medication or a single therapy. The change from acute to chronic pain affects your whole person – physically, emotionally, and socially. That’s exactly why a multidisciplinary approach addresses not just the pain signals, but all the ways chronic pain has impacted your life.
The Pillars of a Comprehensive Pain Treatment Program
When chronic pain takes over your life, it affects everything – your sleep, your mood, your relationships, and your ability to work or enjoy simple pleasures. That’s why we believe in fighting back with every tool available. At the Center for Specialty Care, our comprehensive pain treatment program brings together a diverse team of healthcare professionals who work as one unified force to help you reclaim your life.
Think of pain treatment like building a house. You wouldn’t rely on just one type of material or one craftsperson to create a strong, lasting home. Similarly, our multidisciplinary team approach combines different specialties to create an integrated care plan focused on your unique needs and patient-centered goals. The goal isn’t just to reduce your pain – it’s to improve your function and help you get back to living the life you want.
Physical and Rehabilitative Therapies
Your body wants to move, heal, and feel strong again. Physical and rehabilitative therapies work with your body’s natural healing abilities to restore movement, build strength, and improve flexibility while reducing inflammation.
Physical therapy forms the backbone of most recovery plans. Our skilled therapists don’t just give you exercises to do – they teach you how to move properly, strengthen weak areas, and protect yourself from future injury. Whether you’re dealing with Achilles Tendonitis or struggling with hip and knee pain, targeted exercises can make a world of difference.
Graded exercise means starting where you are and slowly building up your activity level. We never push you too hard too fast – that just leads to setbacks and frustration.
Massage therapy does more than feel good (though that’s certainly a bonus!). Therapeutic massage increases blood flow to painful areas, releases muscle tension, and triggers your body’s natural painkillers called endorphins.
Heat and cold therapy might seem simple, but these treatments pack a powerful punch. Heat therapy relaxes tight muscles and eases stiffness – especially helpful for conditions like tendonitis. Cold therapy reduces swelling and numbs sharp pain, giving you relief when you need it most.
Pharmacological Management
Medications can be valuable allies in your fight against pain, but we believe in using them wisely. Our approach focuses on non-opioid medications whenever possible, aiming for the lowest effective doses to minimize side effects while maximizing your quality of life.
NSAIDs (like ibuprofen) can reduce both pain and inflammation, though we monitor their use carefully since long-term use can affect your stomach, kidneys, and heart. Antidepressants might surprise you – certain types work well for nerve pain, even if you’re not depressed. Anticonvulsants originally designed for seizures can quiet overactive nerves that cause shooting or burning pain.
We take a cautious approach with opioids because while they can provide relief, they carry significant risks including addiction, tolerance, and dependence. When opioids are necessary, we use them as part of a broader plan focused on improving your function, not just masking pain.
Our medication management goes beyond just prescribing pills. We monitor how you respond, watch for side effects, and adjust your treatment as your body changes. Scientific research on non-pharmacological pain therapies shows that combining medications with other treatments often works better than either approach alone.
The reality is that medication tolerance can develop over time, meaning you might need higher doses for the same relief. That’s why we emphasize building a comprehensive treatment plan that doesn’t rely solely on medications.
Interventional Procedures
Sometimes conservative treatments need backup. When physical therapy, medications, and other approaches aren’t providing enough relief, interventional procedures can target the source of your pain directly and interrupt those persistent pain signals.
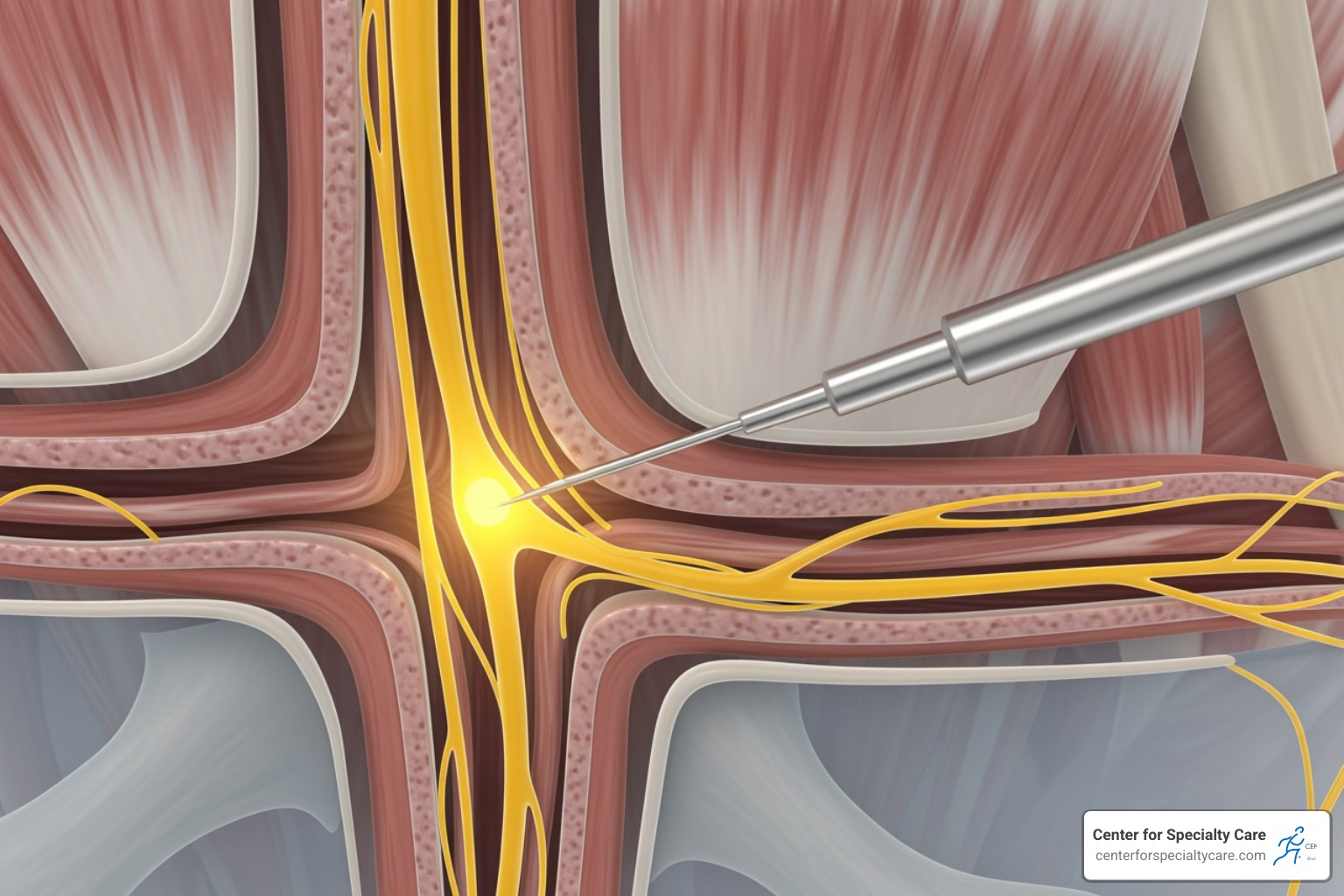
Nerve blocks deliver medication directly to specific nerves that are sending pain signals. Think of it like turning off a circuit breaker for pain – the nerve can’t send pain messages to your brain. These work especially well for localized pain, such as radiating pain or issues with a pinched nerve.
Epidural steroid injections target inflammation around your spinal nerves, providing relief for back and leg pain. If you’re curious about this treatment, we have detailed information on Understanding Epidural Steroid Injections to help you make informed decisions.
Radiofrequency ablation uses controlled heat to disable nerve fibers that carry pain signals. It sounds more intimidating than it is – patients often experience significant relief for months or even years after this procedure.
For severe, persistent pain that hasn’t responded to other treatments, spinal cord stimulators offer hope. These small devices send gentle electrical pulses to your spinal cord, essentially scrambling pain signals before they reach your brain. Many patients find this life-changing technology gives them back activities they thought they’d lost forever.
Psychological and Behavioral Support
Pain doesn’t just hurt your body – it affects your thoughts, emotions, and relationships. That’s why addressing the mind-body connection is crucial for lasting relief. Psychological and behavioral support helps you develop powerful coping strategies and stress management techniques.
Cognitive-Behavioral Therapy (CBT) teaches you to recognize and change thought patterns that make pain worse. When you learn to challenge catastrophic thinking and develop realistic expectations, you often find that your pain becomes more manageable.
Mindfulness practices help you observe pain without being overwhelmed by it. Through meditation and breathing exercises, you can learn to change your relationship with pain, reducing the anxiety and stress that often amplify physical discomfort.
Biofeedback training uses technology to help you see how your body responds to stress and pain. Once you can see your heart rate, muscle tension, or skin temperature on a monitor, you can learn to control these responses consciously.
These approaches work by literally changing pain perception in your brain. When you learn new ways to think about and respond to pain, you’re rewiring neural pathways and taking back control of your experience.
Why an Integrated Approach Beats a Single Treatment
Think about trying to solve a jigsaw puzzle with only one piece at a time. You might make some progress, but you’ll never see the complete picture. Comprehensive pain treatment works the same way – chronic pain is far too complex for any single therapy to handle on its own.
When you rely on just one treatment approach, you’re essentially putting a band-aid on a much larger problem. Take medication alone, for example. While pills might dial down your pain signals, they won’t strengthen your weakened muscles or help you sleep better at night. Physical therapy might get you moving again, but it won’t address the anxiety that makes you afraid to exercise or the depression that saps your motivation.
Single-modality limitations become crystal clear when you consider how chronic pain affects your entire life. Your pain doesn’t just hurt – it changes how you move, how you think, how you feel, and how you connect with others. A truly effective treatment needs to address all these interconnected pieces.
Comprehensive pain treatment recognizes that your pain experience involves physical factors like inflammation and muscle weakness, psychological factors such as stress and fear of movement, and social factors including how pain impacts your work and relationships. When we treat all these aspects together, something remarkable happens.
You start seeing improved function in ways that surprise you. Tasks that seemed impossible become manageable again. We can often reduce your medication reliance, especially those risky opioids that come with so many unwanted side effects. Most importantly, you develop long-term success strategies that stick with you for life.
The research backs this up too. Studies consistently show that comprehensive pain treatment programs are not only more effective than single treatments but also more cost-effective in the long run. You get better results while often spending less money overall.
The Benefits of a Multidisciplinary Team
At the Center for Specialty Care, we’ve built something special – a team where every healthcare professional works together like pieces of a well-oiled machine. Our orthopedic surgeons, pain management specialists, physical therapists, and other experts don’t just work in the same building; they truly collaborate on your care.
This collaborative care plan means each specialist brings their unique perspective to understand your pain completely. Your physical therapist might notice movement patterns that help your doctor understand why certain treatments aren’t working. Your pain specialist might adjust medications based on insights from your therapy sessions.
Consistent communication between team members ensures you never get conflicting advice or feel lost between different treatments. We regularly discuss your progress, share observations, and adjust your plan as needed. You benefit from our collective expertise rather than getting fragmented care from isolated providers.
This approach becomes especially powerful when treating complex pain conditions like rheumatoid arthritis. Our Rheumatology team works seamlessly with our Physical Therapy specialists to address both the inflammatory aspects and functional limitations of these challenging conditions.
The results speak for themselves. Patients consistently experience better functional outcomes because we’re not just reducing pain – we’re helping you reclaim your life. The higher patient satisfaction we see comes from people feeling truly understood and supported by a team that genuinely cares about their complete well-being, not just their symptoms.
Your Journey to Comprehensive Pain Treatment
Taking the first step toward comprehensive pain treatment can feel overwhelming when you’re dealing with chronic pain. At the Center for Specialty Care, we understand that you’re not just looking for another doctor’s appointment – you’re searching for hope, answers, and a path back to the life you want to live.
Your journey begins with recognizing that you deserve to be an active participant in your recovery, not just a passive recipient of treatment. We believe in empowering our patients because, frankly, you know your body better than anyone else. When you walk through our doors, you’re not just another case number – you’re a person with unique goals, concerns, and dreams for your future.
The Importance of Patient-Centered Care in comprehensive pain treatment
At our clinic, patient-centered care isn’t just a buzzword – it’s how we’ve built our practice around achieving 100% patient satisfaction. This approach means your voice matters in every decision we make together.
Personalized treatment plans form the foundation of everything we do. Your chronic pain story is uniquely yours, whether it stems from common spinal conditions or something more complex. We take time to understand not just what hurts, but how that pain affects your work, your family time, and the activities that bring you joy.
Shared decision-making means we explain your options in plain English, discuss what each treatment involves, and work together to choose the path that feels right for you. Some patients want to try every conservative option before considering procedures, while others are ready for more aggressive intervention. There’s no wrong choice – only what’s right for your situation.
We recognize that your unique needs extend beyond medical symptoms. Maybe you’re a farmer who needs to get back to physical work, or perhaps you’re a grandparent who just wants to play with grandchildren without wincing. These personal goals shape how we design your comprehensive pain treatment plan.
How to Access a comprehensive pain treatment Program
Getting started with our comprehensive pain treatment program is designed to be straightforward, not another source of stress in your life. We’ve streamlined our process because we know that when you’re in pain, waiting weeks for answers isn’t acceptable.
Initial consultation is where your healing journey truly begins. During this visit, we conduct a thorough review of your medical history and perform a comprehensive physical exam. We want to understand not just your pain, but your complete health picture. This isn’t a rushed appointment – we take the time needed to really listen to your story.
Diagnostic evaluation may follow, depending on what we find during your consultation. Sometimes we need imaging studies like X-rays or MRI scans, or specialized tests to pinpoint exactly what’s causing your pain. Think of this as detective work – we’re gathering clues to solve your pain puzzle.
The referral process varies depending on your insurance and specific situation. Many patients can schedule directly with us, while others may need a referral from their primary care physician. Our staff is happy to help steer these requirements and work with your existing healthcare team to ensure smooth communication.
Creating your custom plan happens once our multidisciplinary team has all the information we need. This is where our collaborative approach really shines – our specialists work together to design a treatment strategy that addresses your specific condition, lifestyle, and goals. We’re proud of our quick appointment availability, often seeing new patients within one week of their initial call, because we believe prompt care leads to better outcomes.
For additional support and resources, you might find helpful information through Government of Canada’s resources for Canadians living with pain, which provides valuable guidance for those navigating chronic pain management.
The Future of Pain Management: Technology and Innovation
The world of pain management is experiencing an exciting change. New technologies and innovative treatments are changing how we understand and treat chronic pain, offering hope for people who haven’t found relief through traditional methods. At the Center for Specialty Care, we’re committed to bringing you the most advanced comprehensive pain treatment options available.
| Therapy Type | Traditional Pain Therapies | Emerging Therapies |
|---|---|---|
| Mechanism | NSAIDs reduce inflammation; Physical therapy strengthens muscles and improves mobility | VR distracts the brain from pain signals; Regenerative medicine repairs damaged tissues |
| Application | Widely used for most pain conditions; Well-established protocols | Targeted for specific conditions; Personalized based on individual needs |
| Accessibility | Readily available in most clinics; Insurance coverage common | Limited availability; Evolving insurance coverage |
The contrast between traditional and emerging therapies is fascinating. While NSAIDs and physical therapy work through well-understood mechanisms – reducing inflammation and strengthening muscles – newer approaches like virtual reality therapy actually change how your brain processes pain signals. Regenerative medicine goes even further, potentially repairing the damaged tissues that cause pain in the first place.
What makes these emerging treatments particularly exciting is their potential for personalization. Traditional therapies often follow a one-size-fits-all approach, but new technologies allow us to tailor treatments to your specific pain patterns, genetics, and lifestyle.
Emerging Therapies on the Horizon
Virtual Reality (VR) for pain distraction represents one of the most promising developments in comprehensive pain treatment. By immersing you in engaging virtual environments, VR can literally redirect your brain’s attention away from pain signals. Studies show this technology can reduce pain intensity by up to 50% during procedures and rehabilitation sessions.
Wearable health monitors are revolutionizing how we track and manage pain. These devices continuously monitor your activity levels, sleep patterns, heart rate, and even stress indicators. This real-time data helps us understand your pain triggers and adjust your treatment plan accordingly.
Telehealth consultations have become game-changers, especially for people in rural areas like those we serve in Fairmont, MN and surrounding communities. You can now receive expert pain management guidance from the comfort of your home, making comprehensive pain treatment more accessible than ever.
Regenerative medicine offers perhaps the most exciting long-term potential. Treatments like stem cell therapy and advanced platelet-rich plasma (PRP) procedures work to actually repair damaged tissues rather than just managing symptoms. While still evolving, these therapies show remarkable promise for conditions that previously had limited treatment options.
Personalized neuromodulation represents the cutting edge of pain technology. Advanced spinal cord stimulators now use artificial intelligence to learn your unique pain patterns and automatically adjust stimulation parameters throughout the day. This means more effective pain relief with fewer side effects.
The future of pain management isn’t just about new gadgets and procedures – it’s about understanding pain as a complex, individual experience that requires personalized solutions. At the Center for Specialty Care, we’re excited to integrate these innovations into our comprehensive pain treatment programs as they become available and proven effective.




