The Full Spectrum: What to Expect from Comprehensive Pain Treatment
October 17, 2025
Intracept: Is It Surgery, and What Does It Entail?
October 21, 2025Heat for Tendonitis: Ultimate Relief 2025
Why Heat for Tendonitis Can Be Your Path to Pain Relief
Heat for tendonitis can be highly effective, but timing is everything. Understanding when to apply heat versus ice can mean the difference between accelerated healing and prolonged pain.
Quick Answer for Heat and Tendonitis:
- Use heat AFTER the first 48-72 hours when swelling has gone down
- Apply for 15-20 minutes at a time with a barrier between skin and heat source
- Best for chronic stiffness and before gentle stretching or exercise
- Avoid heat on acute injuries with visible swelling or inflammation
- Stop immediately if pain increases or skin becomes irritated
Tendonitis pain can be debilitating, affecting millions with sharp shoulder pain or aching elbows from daily activities. A common question is whether to use heat or ice. While ice is known for acute injuries, heat therapy is crucial for tendonitis recovery when used correctly.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon. At the Center for Specialty Care, I’ve seen how educating patients on the proper use of heat for tendonitis and other conservative treatments significantly improves recovery outcomes.
Heat for tendonitis vocabulary:
Understanding Tendonitis: The “Why” Before the “How”
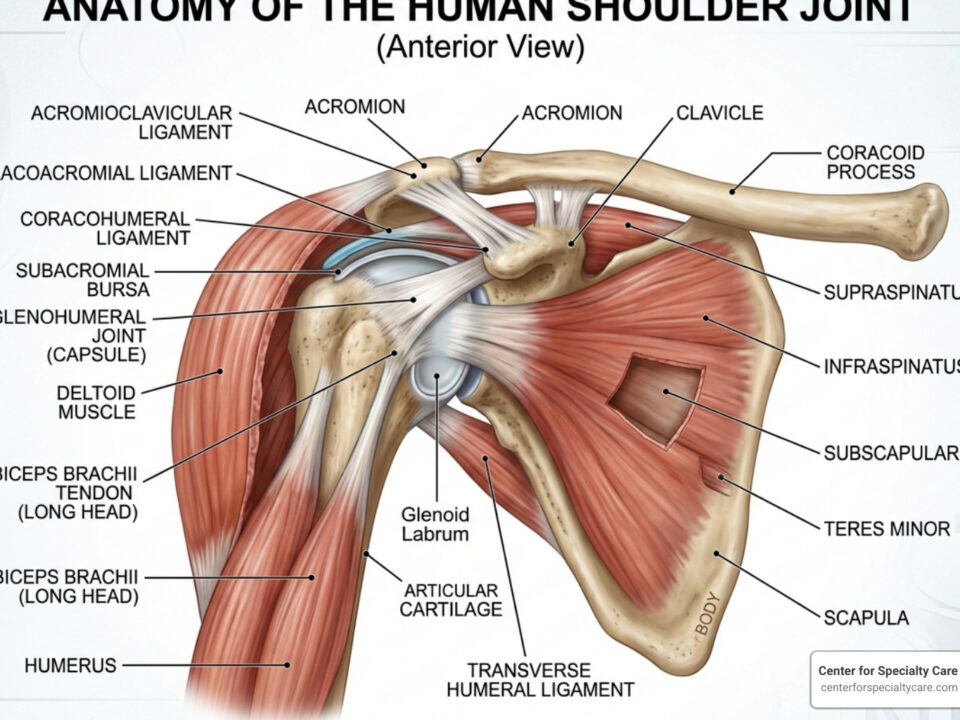
Before exploring when to use heat for tendonitis, it’s important to understand what’s happening in your body. Tendons are the tough, rope-like connectors between muscles and bones. They handle immense stress, and with over 600 in the body, they sometimes need extra care.
When you develop tendonitis, you’re dealing with inflammation or irritation of these tendons. This usually happens from repetitive motions that create overuse injuries, where the tendon can’t keep up with the demands being placed on it.
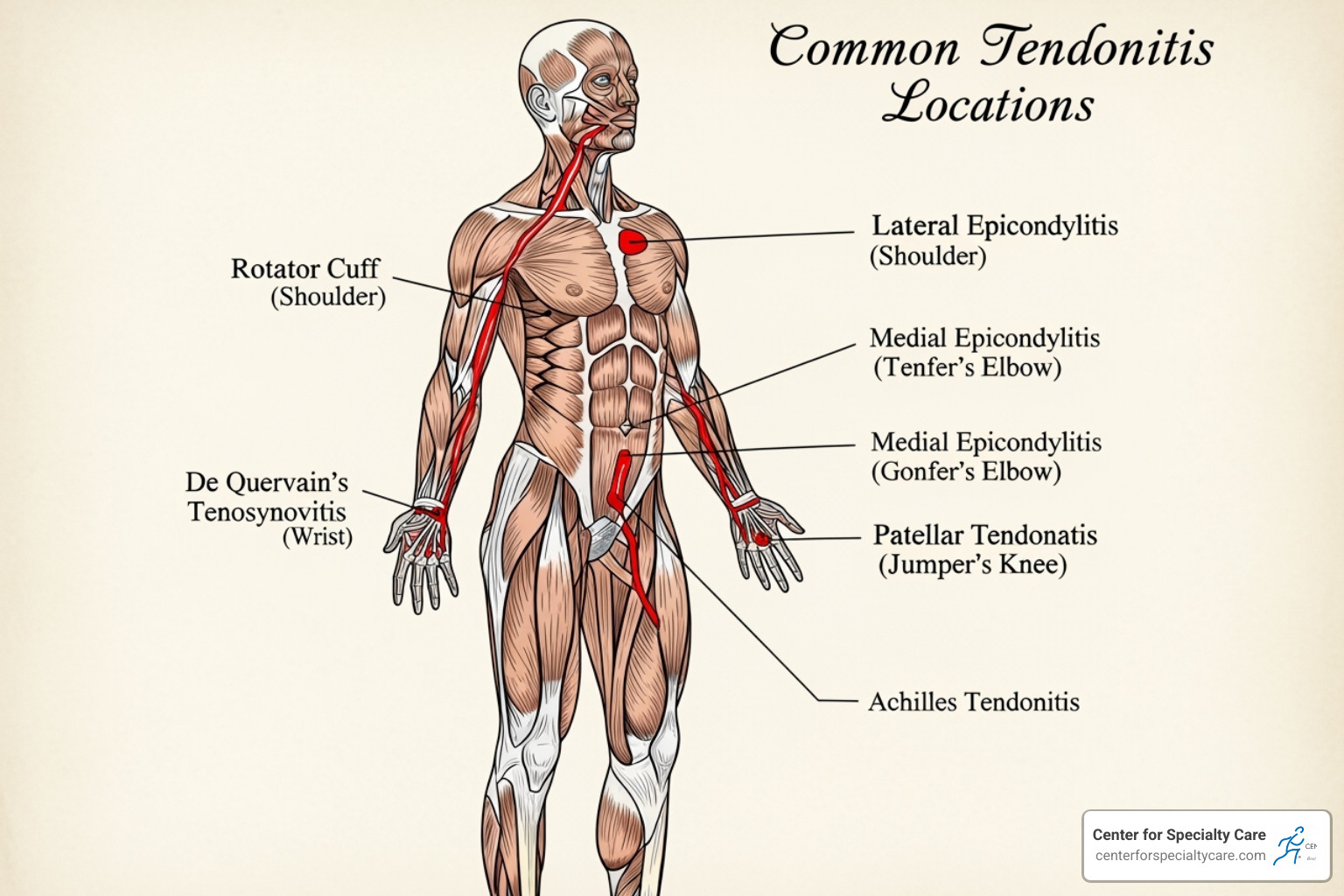
What is Tendonitis and What Are the Symptoms?
Tendonitis is the swelling and irritation of a tendon after injury or overuse, causing joint pain and stiffness. While it can affect any tendon, it’s most common in the shoulders (rotator cuff), elbows (tennis elbow), wrists, knees (jumper’s knee), and heels (Achilles tendonitis).
Common symptoms include:
- A dull, persistent ache around the joint.
- Tenderness to touch on the affected area.
- Mild swelling around the tendon.
- A grating or crackling sensation with movement.
- Stiffness, especially in the morning or after periods of inactivity.
- Pain with specific movements that engage the tendon.
These symptoms can make simple tasks challenging, but understanding them is the first step toward relief.
Key Causes and Risk Factors
Tendonitis is often caused by a combination of factors. Repetitive motion from activities like typing, throwing, or running is the most common culprit. A sudden injury or trauma can also trigger acute tendonitis.
Other significant risk factors include:
- Poor posture and technique during work or exercise, which puts uneven stress on tendons.
- Aging, as tendons naturally become less flexible and more prone to injury over time.
- High-risk activities, as seen in athletes. Tendon injuries account for 50% of all sports injuries, with runners often facing Achilles tendonitis and basketball players dealing with patellar tendonitis.
- Medical conditions like diabetes, arthritis, and thyroid disease.
- Certain medications, such as fluoroquinolone antibiotics.
Tendonitis vs. Tendinosis: An Important Distinction
It’s vital to distinguish between “tendonitis” and “tendinosis,” as they require different treatments. This distinction is crucial when considering heat for tendonitis.
Tendonitis is the acute phase, characterized by inflammation, swelling, and pain from a fresh injury. The body’s inflammatory response is in full effect.
Tendinosis is the chronic phase, involving collagen degeneration from long-term overuse or improperly treated tendonitis. In this stage, there is often little to no inflammation or swelling.
This difference is key: ice is best for reducing inflammation in acute tendonitis, while it’s less helpful for chronic tendinosis. For tendinosis, treatments that promote blood flow and repair, like heat, are far more beneficial. An accurate diagnosis is essential for choosing the right treatment and speeding up recovery.
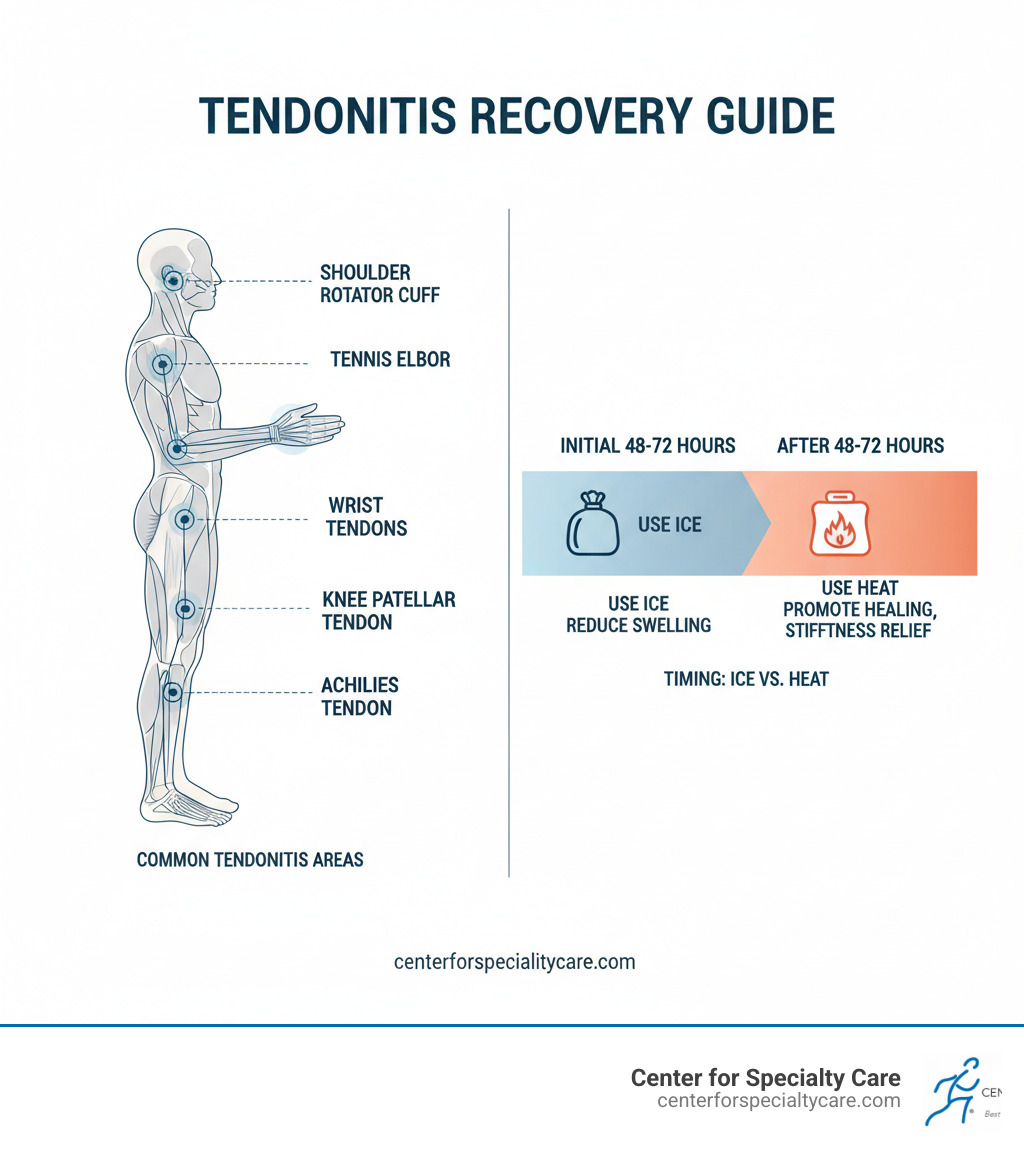
The Great Debate: When to Use Heat vs. Ice
Deciding between heat and ice for tendon pain is a common dilemma. Both are effective, but timing is critical. Using the wrong one can slow healing or increase pain. At Center for Specialty Care, our Sports Medicine team helps patients steer this choice daily.
Think of it this way: ice hits the brakes on inflammation, while heat presses the gas on healing. The key is knowing when to brake and when to accelerate.
| Feature | Ice Therapy (Cold) | Heat Therapy (Warm) |
|---|---|---|
| When to Use | Acute injuries (first 48-72 hours), sudden pain, visible swelling, after activity that causes inflammation | Chronic pain, stiffness, muscle tightness, before stretching/exercise, after 72 hours (no swelling) |
| Benefits | Reduces pain, decreases swelling, numbs the area, constricts blood vessels, reduces inflammation | Increases blood flow, relaxes muscles, reduces stiffness, promotes healing, improves flexibility |
| Duration | 15-20 minutes, every 2-3 hours (initial phase), 4-6 hours (later) | 15-20 minutes, 2-3 times daily (once inflammation subsides) |
| Mechanism | Vasoconstriction, slows metabolic activity | Vasodilation, increases tissue extensibility, speeds metabolic activity |
| Goal | Control inflammation, pain, and swelling | Promote healing, reduce stiffness, prepare for movement |
When Ice is Your Best Friend (The First 48-72 Hours)
For a new injury with swelling, heat, and throbbing pain, ice is the best choice. During the first 48 to 72 hours after a flare-up, your body’s inflammatory response is high. While this is a natural part of healing, too much inflammation can increase pain and slow recovery.
Ice works by numbing the area to dull pain signals and causing vasoconstriction (shrinking of blood vessels) to reduce blood flow. This helps limit swelling and internal bleeding in the acute phase.
The classic RICE method (Rest, Ice, Compression, Elevation) is the standard for acute care. Apply an ice pack wrapped in a thin towel for 15-20 minutes every 2-3 hours during the first few days. Never apply ice directly to the skin. Ice helps control the initial chaos, giving your tendon time to begin repairing itself.
When to Turn Up the Heat (Chronic Pain and Stiffness)
After 48-72 hours, when sharp pain subsides and stiffness sets in, it’s time to switch to heat. This is when heat for tendonitis becomes your best ally, especially for chronic pain without significant swelling.
Heat therapy causes vasodilation, widening blood vessels to increase the flow of oxygen and nutrients to the injured tendon. This improved circulation also helps flush out waste products that contribute to pain and stiffness.
Heat for tendonitis is particularly effective for the muscle tightness that often accompanies tendon injuries. It helps relax tense muscles, breaking the cycle of pain and restriction. Applying heat for 15-20 minutes before gentle stretching or exercise can improve flexibility and make movements more effective. It’s especially beneficial for morning stiffness, helping to loosen collagen fibers and improve range of motion.
A Guide to Applying Heat for Tendonitis
Applying heat for tendonitis correctly is key to its effectiveness. Heat therapy promotes muscle relaxation, improves circulation by dilating blood vessels, provides soothing pain relief, and increases the flexibility of collagen fibers in your tendons. This is especially helpful for morning stiffness or reduced range of motion.

Best Methods for Applying Heat for Tendonitis
You have several options for applying heat for tendonitis, depending on your preference and the affected area.
- Moist heating pads are highly effective, as the moisture helps heat penetrate deeper into tissues. They are great for larger areas like shoulders and knees.
- Warm compresses or towels are a simple, targeted option. Soak a towel in warm water, wring it out, and apply.
- Warm baths or showers provide comprehensive relief, helping to loosen tight joints and muscles throughout the body.
- Heated gel packs or heat wraps offer convenient and portable warmth that conforms to your body’s contours, ideal for use during daily activities.
With any method, the heat should feel comfortably warm, never hot or scalding.
Safety Precautions for Effective Heat for Tendonitis
Using heat safely is essential to avoid injury. Follow these precautions to ensure your heat therapy is both helpful and harmless.
- Protect your skin. Always use a thin towel or cloth as a barrier between the heat source and your skin to prevent burns.
- Monitor the temperature. The heat should be pleasantly warm. If it feels too hot, reduce the temperature or add another layer of protection.
- Limit your sessions. Stick to 15-20 minute sessions. Longer exposure increases the risk of skin damage without adding benefits.
- Never sleep with a heating device. Most serious burns occur during sleep when your protective reflexes are inactive.
- Know when to avoid heat. Do not use heat on a fresh injury with visible swelling or inflammation. If you have diabetes, poor circulation, or reduced sensation, consult a doctor before using heat therapy.
- Check your skin after use. Slight pinkness that fades quickly is normal. Persistent redness, blistering, or pain are signs of a burn.
- Allow recovery time. Wait at least an hour between heat applications to let your skin temperature return to normal.
Beyond Heat: Complementary Treatments and Professional Care
While heat for tendonitis is a powerful tool, it’s most effective as part of a comprehensive recovery plan that addresses the root cause of your pain.
A holistic approach gives your tendon the best environment to heal properly. This includes strategic rest and activity modification—not stopping all activity, but avoiding movements that aggravate the tendon. Gentle stretching, especially after applying heat, can significantly improve flexibility. Simple ergonomic adjustments at your desk or during exercise can also prevent future flare-ups.

Complementary Therapies for Tendon Pain
Several other therapies work well alongside heat treatment.
- Anti-inflammatory approaches, such as over-the-counter medications like ibuprofen or naproxen, can help manage pain and any residual inflammation.
- Massage therapy can relax tight muscles around the tendon, improve circulation, and break down restrictive scar tissue.
- Gradual return to activity is crucial for rebuilding tendon strength. Rushing back to your normal routine is a common cause of re-injury. A personalized exercise program is the safest way to progress.
At Center for Specialty Care, our Physical Therapy team develops custom programs that start with gentle movements and gradually increase in intensity, custom to your specific condition and goals.
When to See a Doctor for Tendonitis
Self-care is effective, but some symptoms require professional medical attention. It’s time to see a doctor if you experience any of the following:
- Pain that persists for more than two weeks despite consistent self-treatment.
- Severe, sudden pain, especially if it occurs during an activity.
- A “pop” or “snap” sound at the time of injury, which could indicate a tendon rupture.
- Inability to move the joint normally.
- Symptoms that worsen despite rest and heat therapy.
At Center for Specialty Care, we understand that persistent pain is frustrating. We focus on personalized care and quick appointment availability in Fairmont, MN, and surrounding areas. Our goal is 100% patient satisfaction, achieved by listening to your concerns and creating a treatment plan that works for you. Whether you need an orthopedic specialist or other treatment options, we’re here to help you get back to the activities you love.
Frequently Asked Questions about Heat and Tendonitis
Here are answers to common questions about using heat for tendonitis to ensure you’re using it safely and effectively.
Can heat make tendonitis worse?
Yes, heat can worsen tendonitis if used at the wrong time. Applying heat to a fresh, inflamed injury (typically within the first 48-72 hours) increases blood flow, which can intensify swelling and pain. Heat is beneficial only after the initial inflammatory phase has passed and swelling has subsided.
How long should I use heat for tendonitis?
Apply heat for 15-20 minutes per session. This duration is sufficient to achieve the benefits of increased blood flow and muscle relaxation without risking skin irritation. Allow your skin to return to a normal temperature for at least an hour between sessions. You can safely apply heat two to three times a day, especially before gentle stretching.
Is it okay to alternate heat and ice for tendonitis?
Yes, alternating heat and ice, known as contrast therapy, can be very effective after the acute inflammatory phase (the first 48-72 hours). The cycle of dilating blood vessels with heat and constricting them with cold creates a pumping action that can improve circulation and reduce stiffness. A common method is to apply heat for 10-15 minutes, then switch to ice for 10-15 minutes. This should not be used on fresh injuries where only ice is recommended.
Your Next Steps for Tendonitis Relief
Understanding when to use heat for tendonitis is a key part of your recovery. Remember the crucial timing: ice for the first 48-72 hours to control inflammation, and heat for the chronic phase to reduce stiffness and promote healing.
Heat therapy supports your body’s natural healing by increasing blood flow and relaxing tight muscles. However, every case of tendonitis is unique, so listen to your body. Stop any therapy that increases your pain.
An effective recovery plan often combines heat for tendonitis with gentle stretching, strategic rest, and a gradual return to activity. This holistic approach addresses both the symptoms and their underlying causes.
If self-care isn’t enough, professional guidance can make all the difference. At Center for Specialty Care, we reject one-size-fits-all solutions. Our team takes the time to understand your specific condition, lifestyle, and goals to create a personalized care plan.
Whether you need conservative treatments like physical therapy or more advanced interventions, we are committed to helping you find relief. Our focus on 100% patient satisfaction means we’re dedicated to helping you feel better.
Ready to take the next step? Learn more about our comprehensive Orthopedics services and find how our personalized approach can support your journey back to comfort and mobility.