The Magnificent Four: Unpacking the Rotator Cuff Muscles
January 6, 2026
The Great Debate: When to Use Heat or Ice for Tendonitis
January 8, 2026Basivertebral Nerve Ablation: Ultimate 5-Year Relief
Why Chronic Low Back Pain Deserves a Targeted Solution
Basivertebral nerve ablation is a minimally invasive procedure that uses radiofrequency energy to stop pain signals from damaged vertebral endplates in the spine. Here’s what you need to know:
Quick Overview:
- What it treats: Vertebrogenic pain—chronic low back pain originating from damaged vertebral endplates
- How it works: Heats and ablates the basivertebral nerve to disrupt pain signals
- Ideal candidates: Patients with chronic low back pain lasting 6+ months, Modic changes on MRI, and failed conservative treatments
- Success rates: 65% of patients report at least 50% pain reduction; 32% report complete pain relief
- Recovery: Same-day outpatient procedure with most patients resuming light activities within 2-3 days
Over 30 million Americans live with chronic low back pain, often labeled “non-specific.” However, research now shows that up to 43% of these cases stem from damaged vertebral endplates. When these protective layers between your vertebrae and discs degenerate, they send pain signals through the basivertebral nerve.
While traditional treatments like physical therapy or injections often only mask symptoms, basivertebral nerve ablation targets the pain at its source. This procedure offers long-lasting relief by deactivating the nerve responsible for transmitting pain, all without major surgery.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon at the Center for Specialty Care in Fairmont, Minnesota. With over three decades specializing in minimally invasive spinal procedures, I’ve seen how this procedure has transformed outcomes for patients whose chronic back pain resisted all other treatments.
Basivertebral nerve ablation terms to remember:
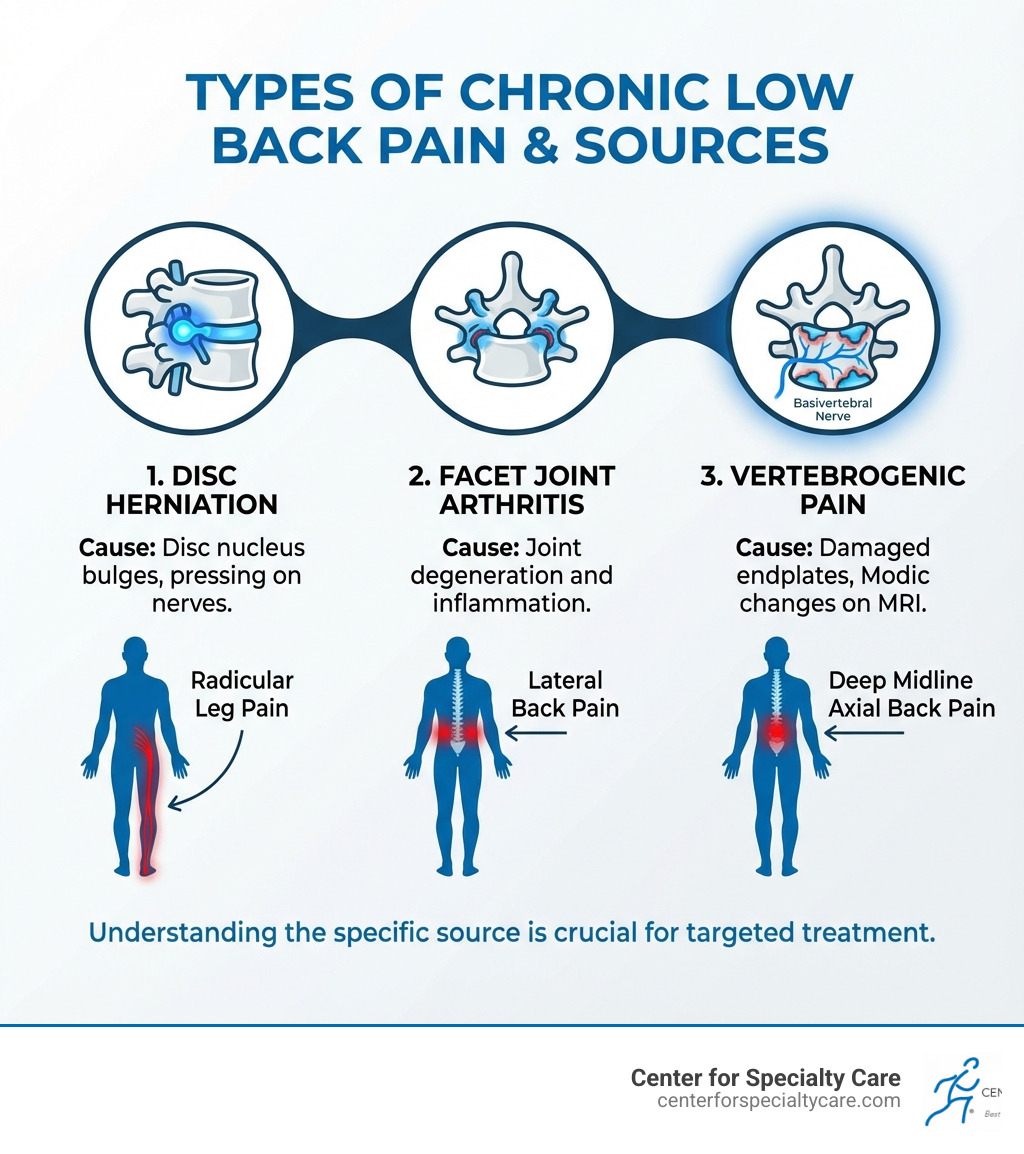
Understanding the True Source: What is Vertebrogenic Pain?
For many, the cause of chronic low back pain remains a mystery. However, a breakthrough has identified a specific source for a subset of patients: vertebrogenic pain. This pain originates from the vertebral endplates—the protective barriers between your vertebral bodies and spinal discs. They are vital for delivering nutrients to the discs and distributing weight throughout the spine.
When these endplates are damaged by inflammation, microfractures, or degeneration, they become a source of chronic pain. This is often a deep, central ache in the low back (axial pain) that worsens with activities like prolonged sitting, bending, or lifting, significantly impacting daily life. To learn more about your spinal anatomy, see our guide: Unlocking the secrets of spinal anatomy: a comprehensive guide.
The Role of MRI and Modic Changes in Diagnosis
Accurately diagnosing vertebrogenic pain requires Magnetic Resonance Imaging (MRI). While a physical exam and medical history provide clues, an MRI can reveal “Modic changes,” which are key indicators of pathology in the vertebral endplates and adjacent bone marrow. These changes are classified into types:
- Modic Type 1 Changes: Characterized by bone marrow edema (fluid) and inflammation, these changes are strongly correlated with active, severe low back pain, suggesting a significant inflammatory process.
- Modic Type 2 Changes: In this type, bone marrow is replaced by fat. These changes represent a more chronic stage of degeneration and are also a potential source of pain.
- Modic Type 3 Changes: These involve bone hardening (sclerosis) and are rarely symptomatic or targeted by basivertebral nerve ablation.
The presence of Modic Type 1 or Type 2 changes on your MRI is a key indicator that you might be a candidate for basivertebral nerve ablation, as it confirms the vertebral endplate is the likely origin of your pain. This allows us to move beyond generalized solutions and target the specific anatomical source.
For a deeper dive into the role of the vertebral endplate, you can explore the research: The role of the vertebral end plate in low back pain. To understand how your spinal column protects your nervous system, we recommend: Guardians of the nervous system: how the spinal column protects the cord.
How Basivertebral Nerve Ablation Stops Pain Signals
Once vertebrogenic pain is diagnosed, basivertebral nerve ablation offers a targeted, minimally invasive solution. The procedure works by interrupting pain signals that travel from damaged vertebral endplates through the basivertebral nerve to your brain.
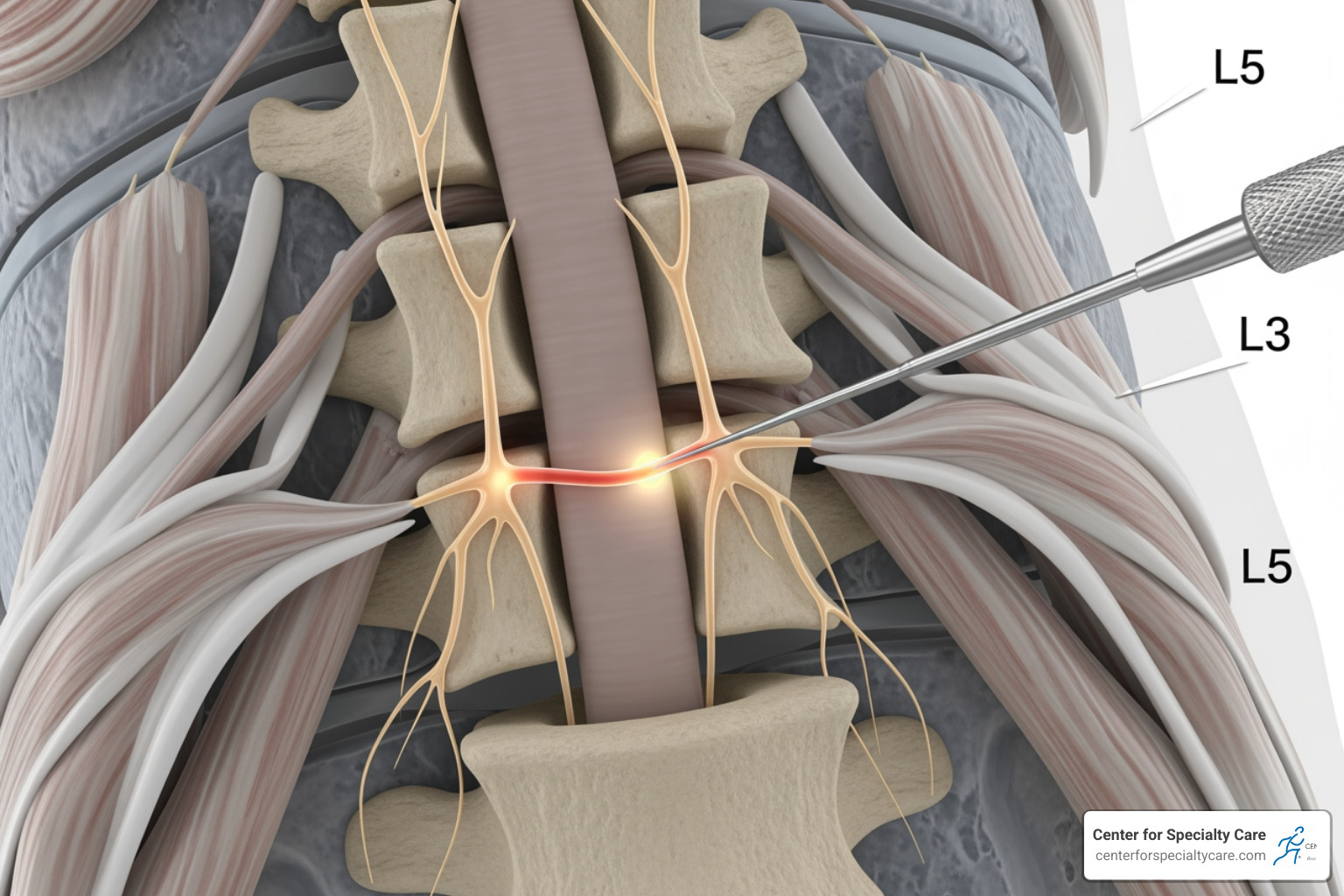
The basivertebral nerve enters each vertebral body and branches out to the endplates. Its fibers are specialized to transmit pain (nociceptive), and they become overactive when the endplates are damaged.
Basivertebral nerve ablation uses radiofrequency energy to create a small heat lesion that deactivates this nerve, effectively turning off the “pain switch” at its source to provide lasting relief. As an outpatient procedure, it allows you to go home the same day. At Center for Specialty Care, we are committed to exploring advanced options to help our patients in Fairmont, Estherville, Buffalo Center, and St. James find relief. For more on our approach, visit: More info about pain management.
The Science of Radiofrequency Ablation
The procedure is based on radiofrequency ablation (RFA), a well-established technique for treating pain. What makes basivertebral nerve ablation unique is its precise focus on the basivertebral nerve.
- Fluoroscopy Guidance: We use real-time X-ray imaging (fluoroscopy) to visualize your spine and precisely guide our instruments for accuracy and safety.
- Transpedicular Approach: To reach the nerve, we insert a thin tube (cannula) through the pedicle, a strong part of the vertebra. This provides safe access to the vertebral body without disturbing the spinal canal.
- Creating a Channel: Through the cannula, we create a small channel leading directly to the basivertebral nerve.
- Precise Nerve Targeting: A radiofrequency probe is positioned at the nerve’s terminus. It delivers controlled energy, typically heating to 85°C for about 15 minutes, to create a small lesion that deactivates the nerve and disrupts its ability to transmit pain signals.
This meticulous, image-guided procedure allows us to target the pain source with remarkable precision, offering a sophisticated solution for vertebrogenic pain. For a detailed technical look, medical professionals can refer to guides like: How I do it: basivertebral nerve ablation for vertebrogenic pain.
The Patient Journey: A Step-by-Step Guide
Understanding each step of a medical procedure can help ease your mind. At Center for Specialty Care, we ensure you know what to expect from your initial consultation through recovery from basivertebral nerve ablation.
Who is a Candidate for Basivertebral Nerve Ablation?
Basivertebral nerve ablation is highly effective for a specific group of patients. You are likely a candidate if you meet the following criteria:
- Chronic Low Back Pain: You’ve experienced persistent low back pain for at least six months.
- Failure of Conservative Care: You’ve tried non-surgical treatments like physical therapy, medication, and injections without lasting relief.
- Confirmed Vertebrogenic Pain: Your pain is a deep, midline lumbar ache that often worsens with sitting, bending, or lifting.
- Modic Changes on MRI: Your MRI scans show Modic Type 1 or Type 2 changes in your lumbar spine (L3-S1).
- Significant Functional Impairment: Your pain significantly limits your daily activities or quality of life.
- Absence of Radicular Symptoms: Your primary pain is in your back, without significant pain, numbness, or weakness radiating down your legs.
You are generally not a candidate if your pain stems from other sources (e.g., facet joints, herniated discs) or if you have conditions like pregnancy, active infection, an implanted electronic device, or severe cardiopulmonary compromise. Our team in Fairmont, Estherville, Buffalo Center, and St. James is here to help. Learn more about our services: More info about back & spine services.
The Procedure: Preparation, Treatment, and Recovery
Here’s a step-by-step look at the procedure journey at Center for Specialty Care:
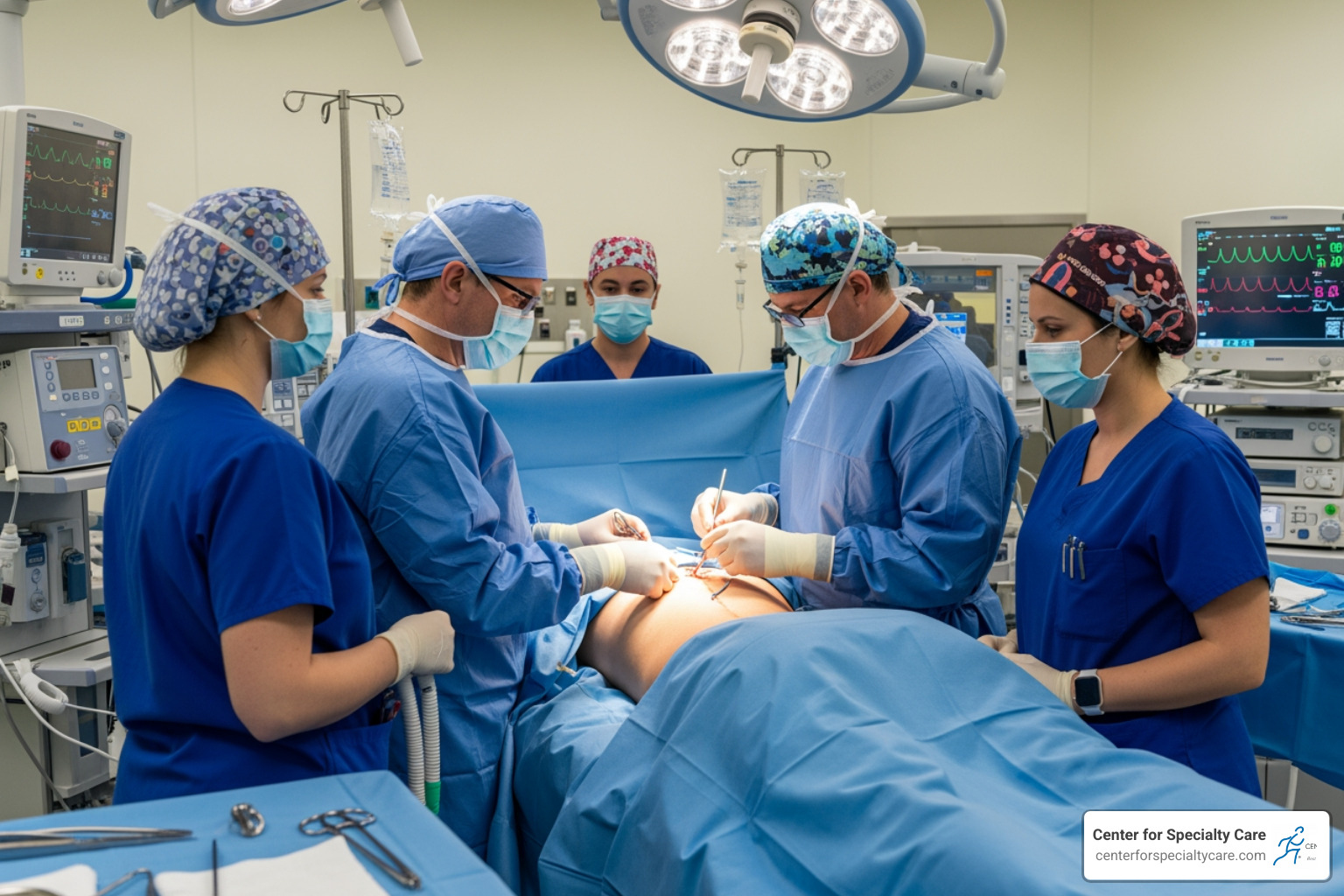
1. Preparation
Before your procedure, we will conduct a full evaluation, review your medications, and provide instructions on fasting. You will need to arrange for a ride home. We often administer IV antibiotics to prevent infection and strongly recommend quitting nicotine to improve healing.
2. The Treatment
The procedure takes about 1 to 1.5 hours as an outpatient. You will receive anesthesia or sedation for comfort and be positioned face-down. Using real-time X-ray guidance, we will numb the area and insert a thin tube through the pedicle to access the basivertebral nerve. A radiofrequency probe then delivers controlled energy for about 15 minutes to ablate the nerve. Finally, the small incision is closed with a dressing.
3. Recovery
You’ll be monitored in a recovery area until you are stable enough to go home the same day.
- Rest and Activity: Rest for the first day and limit physical activity for 48 hours. Avoid heavy lifting, twisting, bending, and submerging the incision. Avoid driving for 24 hours if you had sedation.
- Incision Care: Keep the site clean and dry, and watch for signs of infection (fever, redness, drainage).
- Pain Management: Temporary soreness is normal and can be managed with over-the-counter pain relievers. A temporary increase in back pain for a week or two is also possible during healing.
- Timeline: Most patients resume light activities in 24-48 hours, with full recovery in one to two weeks. Pain relief may be immediate or take 2-3 months to fully develop.
Evaluating the Outcomes: Success Rates, Benefits, and Risks
When considering basivertebral nerve ablation, it’s important to understand its effectiveness and safety, which are supported by strong clinical evidence.
What are the Benefits and Success Rates?
The primary goal is lasting pain relief and improved quality of life. The clinical evidence is compelling:
- Significant Pain Reduction: Studies show impressive results. 65% of patients report at least a 50% reduction in pain, with a 5-year analysis confirming significant mean pain improvement.
- Improved Function: Patients also experience significant functional improvement. A 5-year analysis showed a mean improvement of 28.0 points on the Oswestry Disability Index, indicating better mobility.
- Long-Term Relief: The results are durable, with many patients experiencing pain reduction for five years or longer. A 5-year analysis found 32.1% of participants reported complete pain relief.
- Reduced Opioid Use: The procedure helps reduce or eliminate the need for opioids. Data shows a 65.2% opioid cessation rate among prior users.
- Return to Prior Activity Levels: Studies indicate that 70% of patients were able to resume their previous activity levels.
- Minimally Invasive: As an outpatient procedure with a small incision, it avoids the long recovery of open surgery, uses no permanent implants, and does not prevent future spinal treatments.
These statistics underscore why we offer this treatment. For more data, review the 5-year pooled analysis from clinical trials.
Understanding the Potential Risks of Basivertebral Nerve Ablation
While safe and effective, basivertebral nerve ablation, like any medical procedure, has potential risks that are important to understand.
Serious complications are rare, with clinical trials reporting a rate below 0.3%. This low rate reflects the procedure’s minimally invasive and precise nature.
Common, temporary side effects include soreness at the injection site and mild lower back or leg pain, which typically resolve as your body heals. A temporary increase in back pain for a week or two is also a normal part of healing.
Though rare, more serious risks include nerve irritation or damage, bleeding, vertebral fracture (especially with osteoporosis), and infection. We take extensive precautions, including imaging guidance and antibiotics, to minimize these risks. Contact us if you experience signs of infection or severe pain not relieved by medication.
How Does BVNA Compare to Other Back Pain Treatments?
When you’re dealing with chronic low back pain, it’s helpful to understand how basivertebral nerve ablation (BVNA) compares to other common treatments.
| Treatment | Target Area | Invasiveness | Recovery Time | Permanence of Relief | Ideal Candidate |
|---|---|---|---|---|---|
| Basivertebral Nerve Ablation | Basivertebral nerve within the vertebral body, addressing damaged endplates | Minimally invasive (small incision) | Days to 1-2 weeks (light activity) | Long-term (5+ years for many) | Chronic vertebrogenic pain, Modic Type 1 or 2 changes, failed conservative care |
| Epidural Steroid Injections | Nerve roots, spinal canal (to reduce inflammation) | Minimally invasive (needle injection) | Hours to 1-2 days | Temporary (weeks to months) | Disc herniation, nerve compression, inflammation causing radicular pain |
| Spinal Fusion | Entire vertebral segment (to stabilize) | Highly invasive (major surgery) | Months | Permanent (structural change) | Spinal instability, severe deformity, nerve compression unresponsive to less invasive options |
As you can see, each treatment has a unique purpose. Epidural steroid injections are excellent for reducing inflammation around nerve roots but may not address the root cause of vertebrogenic pain. You can learn more about them here: Understanding epidural steroid injections: what you need to know.
Spinal fusion is a major surgical procedure for severe instability or deformity. Other surgeries like laminectomy may also be considered for nerve pressure relief. Learn more here: Unlocking mobility: the role of orthopedic specialists in laminectomy procedures.
Basivertebral nerve ablation fills a crucial gap. It offers a minimally invasive, long-term solution for patients with vertebrogenic pain who haven’t found relief from less invasive options but aren’t candidates for major surgery. It’s a targeted approach that addresses a specific pain generator.
Frequently Asked Questions About the Procedure
Here are answers to some of the most common questions we receive about basivertebral nerve ablation.
Is the procedure painful?
Minimizing discomfort is a top priority. We use anesthesia and sedation to keep you comfortable during the procedure. Afterward, it’s normal to have some manageable soreness at the incision site and in your lower back. Some patients experience a temporary increase in back pain for a week or two as part of the healing process. Our team will provide detailed pain management instructions.
How long does the pain relief last?
The long-term effectiveness of basivertebral nerve ablation is a key benefit. Clinical studies show that many patients experience significant pain reduction lasting five years or longer. While individual results can vary based on your overall health and other factors, the data strongly supports this procedure as a durable, long-term solution for vertebrogenic pain.
Will I need to repeat the procedure?
This procedure is designed for lasting relief and is not typically repeated at the same vertebral level. Research indicates the ablated basivertebral nerve does not regenerate, permanently disrupting pain signals from the treated area. While new issues could develop at different vertebral levels in the future, the goal for the treated segment is durable, sustained relief.
Conclusion: Taking the Next Step Towards a Pain-Free Life
Vertebrogenic pain from damaged vertebral endplates can be a relentless condition. For those who have struggled with treatments that only mask symptoms, basivertebral nerve ablation offers a breakthrough. This targeted, minimally invasive procedure deactivates the basivertebral nerve, interrupting pain signals at their source. With impressive success rates and long-term efficacy, it has the potential to transform lives.
At Center for Specialty Care, we are dedicated to providing personalized, effective solutions for your pain. We make advanced treatments like basivertebral nerve ablation accessible to our communities in Fairmont, Minnesota, Estherville, Iowa, Buffalo Center, Iowa, and St. James, Minnesota.
If you have suffered from chronic low back pain for over six months, haven’t found relief from conservative treatments, and suspect your pain might be vertebrogenic, we encourage you to take the next step. Our expert team can evaluate your condition and determine if this procedure is right for you, guiding you toward a life with less pain and more mobility.
Learn more about the Intracept™ Procedure at Center for Specialty Care