Nighttime Rotator Cuff Pain? Here’s How to Finally Get Some Rest
March 14, 2026
Sore Achilles? Here’s How to Choose Between Ice and Heat for Relief
March 17, 2026Getting Zapped: Your Back Ablation Procedure Explained
Why Back Pain Sufferers Are Turning to Nerve Ablation
A back ablation procedure is a minimally invasive treatment that uses heat to destroy specific nerves transmitting pain signals from your spine to your brain. Here’s what you need to know:
Quick Overview:
- What it treats: Chronic lower back pain from arthritis, facet joints, sacroiliac joints, or damaged vertebral endplates
- How it works: Heat from radiofrequency waves (300-500 Hz) creates a lesion on pain-transmitting nerves
- Duration: 60-90 minutes outpatient procedure
- Relief timeline: Pain reduction within 1-6 weeks, lasting 6 months to 5+ years
- Success rate: Roughly two-thirds experience at least 50% pain reduction
If you’ve been dealing with chronic lower back pain that won’t quit—despite months of physical therapy, medications, and injections—you’re probably wondering if there’s a better option than just “living with it” or jumping straight to surgery.
That’s where nerve ablation comes in.
This procedure interrupts the pain signals traveling from damaged joints or vertebrae in your spine. Instead of masking pain with pills or accepting limited mobility, ablation targets the source by disrupting the nerves responsible for sending those pain messages to your brain.
There are two main types: traditional radiofrequency ablation (RFA) targets nerves around facet joints, while basivertebral nerve (BVN) ablation (also called the Intracept procedure) goes deeper to address pain from damaged vertebral endplates. Studies show that 50-70% of patients experience significant relief lasting up to two years or longer.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon with over 30 years of experience treating chronic pain conditions in southern Minnesota and northern Iowa. At Center for Specialty Care, I’ve helped countless patients find relief through back ablation procedures and other minimally invasive techniques that allow them to return home the same day.
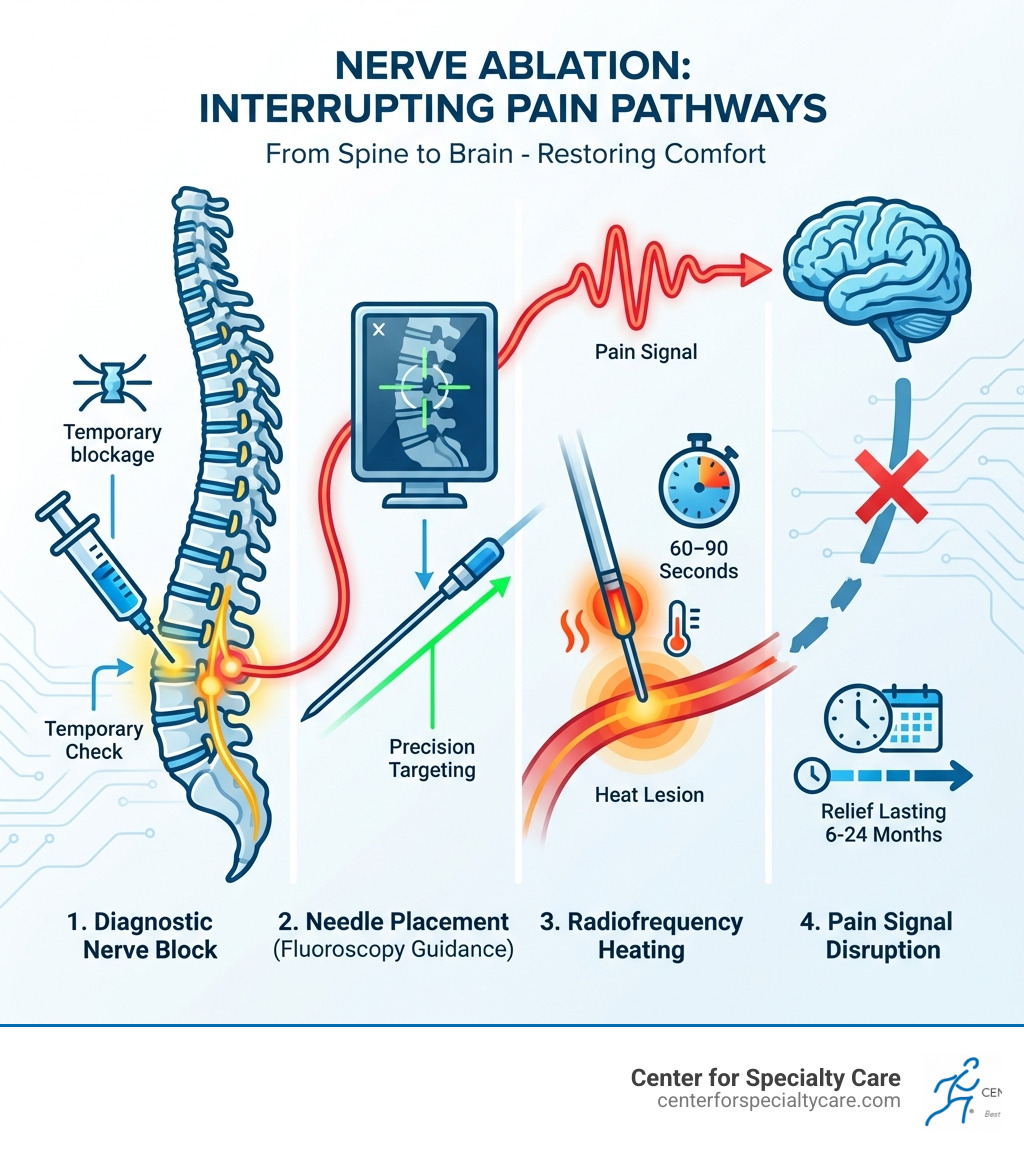
Back ablation procedure vocab explained:
Understanding the Back Ablation Procedure and How It Works
To understand how a back ablation procedure works, we first have to talk about how your body processes pain. Think of your nerves as electrical wires. When you have an injury or arthritis in your spine, those “wires” send a constant stream of “ouch!” signals to your brain. Nerve ablation, also known as radiofrequency neurotomy, is essentially like flipping the breaker switch on those specific wires.
Technically speaking, the procedure involves coagulation necrosis. This sounds a bit scary, but it simply means we use high-frequency waves (usually between 300 to 500 Hz) to heat a tiny tip of a needle. When this needle is placed precisely next to a sensory nerve, the heat creates a small lesion, or “zapped” area. This lesion prevents the nerve from being able to transmit nociceptive (pain) signals to your brain.
The beauty of this technology is its precision. We aren’t just heating up your whole back; we are targeting the tiny medial branch nerves that serve the facet joints or the basivertebral nerve inside the bone. Because these are sensory nerves, “zapping” them doesn’t affect your ability to move or walk. It just quiets the noise.
According to Scientific research on ablative nerve blocks, this process is a highly effective alternative to more invasive surgeries for those with chronic, localized pain. For more information on how we apply these techniques to spinal health, you can explore our back spine services.
Common Causes of Chronic Pain Treated by Nerve Ablation
Not all back pain is created equal. We typically see patients in our Fairmont and Estherville clinics who have tried everything—from chiropractic adjustments to “miracle” creams—without success. A back ablation procedure is most effective when the pain comes from specific, identifiable structures in the spine.
- Facet Joint Syndrome (Arthritis of the Spine): Your vertebrae are connected by small joints called facet joints. Like your knees or hips, these can wear down over time, leading to arthritis. This usually feels like a dull, aching pain in the lower back that gets worse when you twist or lean backward.
- Sacroiliac (SI) Joint Pain: This is pain where your spine meets your pelvis. It can cause sharp or dull pain in the buttocks and lower back.
- Vertebrogenic Pain (Endplate Inflammation): This is a relatively “new” findy in pain management. It involves damage to the vertebral endplates (the layers between your discs and the bone). On an MRI, we look for something called “Modic changes,” which indicate inflammation and edema in the bone.
- Degenerative Disc Disease: While ablation doesn’t “fix” the disc, it can stop the nerves in the surrounding bone from sending pain signals caused by the disc’s wear and tear.
- Whiplash-Associated Pain: While often associated with the neck, the mechanical stress of whiplash can affect the joints of the upper and lower back as well.
If you are curious about what might be causing your specific symptoms, check out our guide on common spinal conditions. Understanding the source of your pain is the first step toward “zapping” it for good.
Types of Ablation: Traditional RFA vs. Basivertebral Nerve (BVN) Ablation
When we talk about a back ablation procedure, we are usually referring to one of two primary methods. Choosing the right one depends entirely on where your pain is coming from.
| Feature | Traditional Radiofrequency Ablation (RFA) | Basivertebral Nerve (BVN) Ablation |
|---|---|---|
| Primary Target | Medial branch nerves (outside the bone) | Basivertebral nerve (inside the bone) |
| Source of Pain | Facet joints (arthritis/inflammation) | Vertebral endplates (vertebrogenic pain) |
| Procedure Name | Rhizotomy or RFA | Intracept Procedure |
| Imaging Evidence | Physical exam & diagnostic blocks | MRI showing Modic Type 1 or 2 changes |
| Relief Duration | 6 to 24 months | 5+ years (potentially permanent) |
| Device Used | Standard RF needle/electrode | Specialized Intracept cannula & probe |
Traditional RFA is the “old reliable.” It’s been used since the 1970s to treat facet joint pain. We target the nerves that live on the outside of the joints. Because these nerves can eventually grow back, the relief is often temporary (though 6-24 months is a long time for someone in chronic pain!).
On the other hand, the Intracept procedure (BVN ablation) is a game-changer for people with vertebrogenic pain. Instead of targeting nerves on the outside, we go into the vertebral body itself to stop the pain signals at the source. Research shows that Basivertebral Nerve Ablation is incredibly durable, with many patients remaining pain-free five years later.
We are proud to offer the Intracept procedure at our Center for Specialty Care locations for those who qualify based on their MRI results.
Step-by-Step: Navigating Your Back Ablation Procedure
Walking into a procedure room can be nerve-wracking, but knowing exactly what is going to happen can take the “spicy” out of the experience. A back ablation procedure is an outpatient affair, meaning you’ll be back in your own recliner in Fairmont or St. James by the afternoon.
Preparing for Your Back Ablation Procedure
Before we ever pick up a radiofrequency probe, we have to make sure we’re targeting the right “wire.” This is done through a diagnostic nerve block. We inject a small amount of anesthetic (like Novocain) onto the suspected nerves. If your pain disappears for a few hours, we know we’ve found the culprit!
On the day of the procedure:
- Fasting: You’ll likely be asked not to eat or drink for about 8 hours prior if you are receiving IV sedation.
- Medications: We will review your meds, especially blood thinners, which usually need to be paused.
- Transportation: Because we use sedation to keep you comfortable, you must have a responsible adult to drive you home. No Ubering or hitching a ride on a tractor!
For more on how we prepare our patients, visit our pain management page.
The Back Ablation Procedure Process
Once you’re in the procedure suite, here is the play-by-play:
- Positioning: You will lie face down on a specialized X-ray table. We’ll make sure you’re comfortable with pillows and cushions.
- Numbing: We use a local anesthetic to numb the skin and deeper tissues. You might feel a little sting and burn, but that’s the last of the discomfort.
- Guidance: Using a “C-arm” (a mobile X-ray called fluoroscopy), we guide the ablation needle exactly to the target nerve. This is like using GPS for your spine.
- Testing: This is the most important part. We use a tiny bit of electrical current to stimulate the nerve. You might feel a dull throb or a twitch. This confirms we are on the sensory nerve and safely away from the motor nerves that move your legs.
- The Zap: Once we are sure of the placement, the radiofrequency energy is turned on. It heats the nerve for 60-90 seconds. Most patients just feel a sensation of warmth.
- Completion: We may treat multiple levels (like L3, L4, and L5) during the same session. Once finished, the needles are removed, and a small bandage is applied.
Research on sacroiliac joint targeting shows that this level of precision is what makes the procedure so much more effective than general injections.
Candidacy, Benefits, and Risks
Who is the “perfect” candidate for a back ablation procedure? Generally, we look for patients who meet these criteria:
- Chronic lower back pain lasting at least six months.
- Pain that hasn’t responded to conservative care (PT, meds, chiropractic).
- A positive response to a diagnostic nerve block (at least 50-80% relief).
- For BVN ablation, an MRI showing Modic changes.
The Benefits: The most obvious benefit is the reduction in pain. Roughly two-thirds of patients see their pain cut in half, and many see 100% resolution. Beyond the numbers, it’s about quality of life. 70% of Intracept patients resume the activities they loved before the pain started—whether that’s golfing, gardening, or just playing with the grandkids. It also helps many people reduce or eliminate their reliance on opioid pain medications.
The Risks: No procedure is 100% risk-free, but nerve ablation is remarkably safe. The serious complication rate is less than 0.3%. The most common “side effect” is temporary soreness at the injection site or a “sunburn” sensation that lasts a few days. Rare risks include infection, bleeding, or temporary nerve irritation.
At Center for Specialty Care, our goal is always 100% patient satisfaction through expert orthopedic care. We take every precaution to ensure your safety and comfort.
Recovery and Long-Term Effectiveness
Recovery from a back ablation procedure is relatively quick, but you do have to give your body a minute to catch up.
The First 24-48 Hours:
- Rest: Take it easy. No heavy lifting or marathons.
- Ice: Use an ice pack on the site (20 minutes on, 20 minutes off) to reduce soreness.
- Shower: You can usually shower the next day, but avoid baths or hot tubs for 48 hours.
The Timeline of Relief: Don’t be discouraged if you aren’t pain-free the second you stand up. In fact, some patients feel a little more sore for the first week—this is just the nerves reacting to being “zapped.” Most people start feeling the real benefit within 2 to 4 weeks, with maximum relief peaking around the 3-month mark.
How Long Does It Last?
- Traditional RFA: Typically 6 to 24 months. If the nerve regrows and the pain returns, the procedure can be repeated.
- BVN Ablation (Intracept): Studies show improvements lasting up to 5 years for many patients.
According to research on long-term BVN outcomes, 50% to 70% of patients maintain their improvements for at least two years. That is a lot of pain-free living!
Frequently Asked Questions about Back Ablation
Who is a good candidate for nerve ablation?
A good candidate is someone with chronic axial (middle of the back) pain that has lasted more than 6 months and hasn’t improved with physical therapy. You must have skeletal maturity (no growing kids!) and a successful diagnostic block. If you’re looking for an expert opinion locally, check out our guide on finding a pain management doctor.
How does BVN ablation differ from traditional RFA?
Traditional RFA targets the medial branch nerves outside the vertebrae to treat facet joint arthritis. BVN ablation (Intracept) targets the basivertebral nerve inside the vertebral bone to treat vertebrogenic pain caused by endplate damage (Modic changes). One treats the “joints,” the other treats the “bone.”
How long does the pain relief last?
For traditional RFA, expect 6 to 24 months. For BVN ablation, the relief is much more durable, often lasting 5 years or more. Because nerves can regenerate over time in RFA, the procedure is repeatable.
Conclusion
Chronic back pain doesn’t have to be your “new normal.” Whether you’re in Fairmont, MN, or Estherville, IA, the team at Center for Specialty Care is dedicated to helping you find the right path to relief. We pride ourselves on personalized care and quick appointment availability—because when you’re in pain, every day counts.
A back ablation procedure offers a scientifically proven, minimally invasive way to stop pain at the source without the long recovery times of traditional surgery. If you’re ready to stop the “ouch” and start living again, we invite you to schedule your Intracept procedure consultation today. Let’s get you zapped and back to the life you love!