
The Intracept Comeback: A Full Guide to Your Recovery Journey
February 3, 2026
Say Goodbye to Foot Pain with Effective Plantar Fasciitis Treatments
February 5, 2026Heat Cold Therapy for Tendonitis: 1 Ultimate Win
Why Heat Cold Therapy for Tendonitis Matters
Heat cold therapy for tendonitis is one of the most accessible and effective ways to manage pain at home. If you’re dealing with tendon pain, here’s what you need to know right now:
Quick Decision Guide:
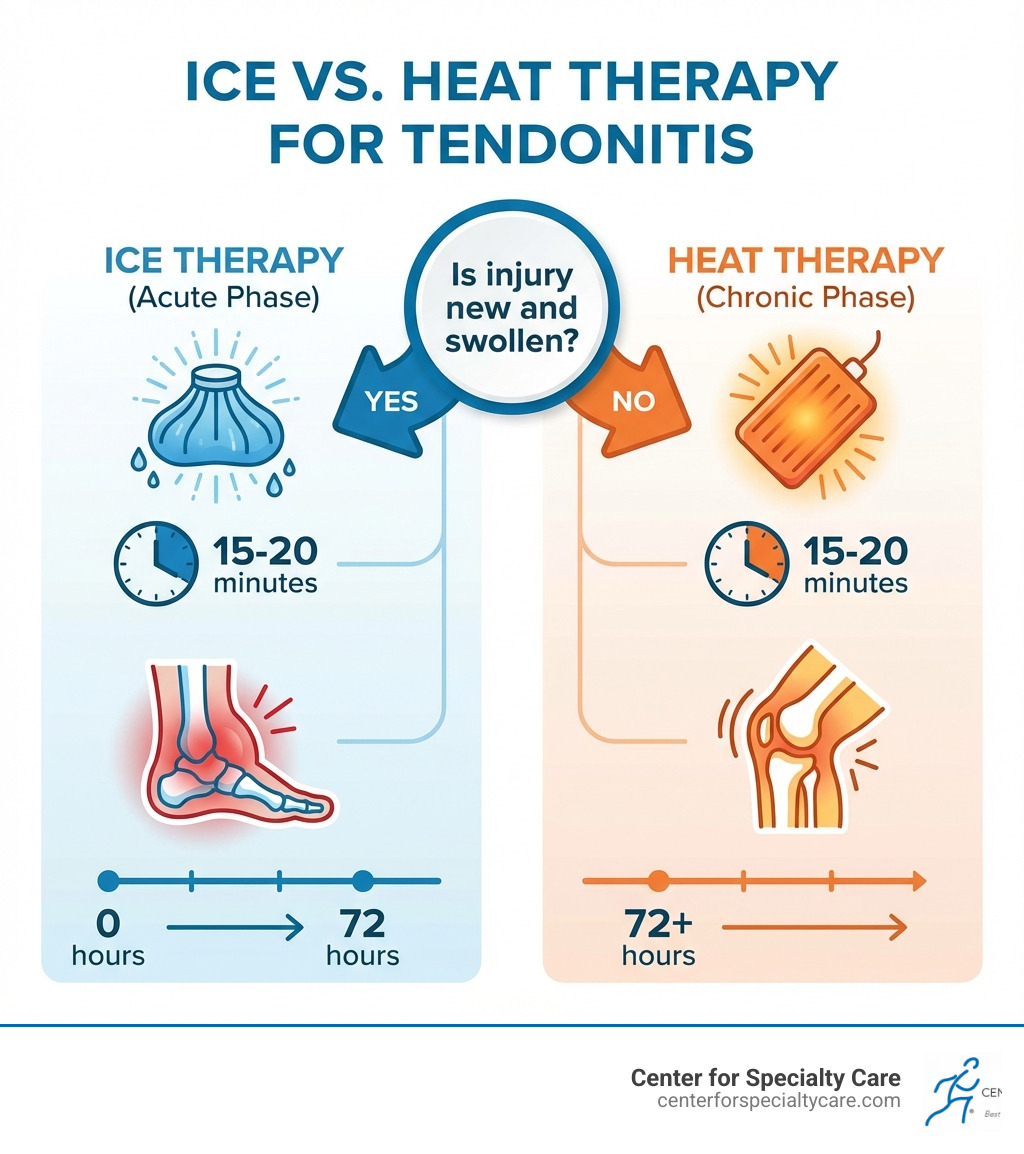
- Use ICE if your injury is new (less than 72 hours), swollen, red, or hot to the touch
- Use HEAT if your pain is chronic (more than 3 days old), stiff, or achy without visible swelling
- Avoid heat on fresh injuries—it can make inflammation worse
- Both therapies work, but timing is everything
Tendonitis affects nearly 7 percent of all injury-related physician visits in the United States, and hundreds of thousands of people deal with this painful condition every year. Whether you’re an athlete with a sore Achilles tendon, an office worker with elbow pain, or someone struggling with a stiff shoulder, understanding when to reach for ice versus heat can dramatically speed your recovery.
The confusion is understandable. One source tells you to ice everything, another swears by heat, and you’re left wondering which approach will actually help. The truth is that both have their place—but using the wrong one at the wrong time can delay healing or even make symptoms worse.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon who has treated tendon injuries for over three decades here in Fairmont, Minnesota. Throughout my career specializing in sports medicine and joint surgery, I’ve guided countless patients through effective heat cold therapy for tendonitis protocols as part of their recovery plans. Let me help you understand exactly when and how to use these simple but powerful tools.
Heat cold therapy for tendonitis glossary:
What is Tendonitis and Why Does It Hurt?
Imagine your body as a complex machine, and your tendons are the strong, fibrous ropes connecting your muscles to your bones. They’re essential for movement, allowing us to walk, lift, throw, and even type. When these crucial connections become inflamed or irritated, that’s what we call tendonitis. This inflammation often leads to pain, swelling, and stiffness, making everyday activities a real challenge.
What causes this irritation? Most often, it’s due to repetitive motions or overloading a joint. Think about a baseball pitcher repeatedly throwing, a construction worker using a jackhammer, or even someone spending hours typing at a keyboard. Over time, these actions can irritate the tendon, leading to injury. Sometimes, factors like aging, certain medications, or even underlying health conditions can increase our risk.
It’s a common issue, too. Tendinopathies, which include tendonitis, account for nearly 7 percent of all injury-related physician office visits in the United States. Hundreds of thousands of employees are affected by these overuse injuries every year, leading to significant lost work time. For example, rotator cuff tendinopathy (shoulder pain) affects one in 50 adults, and issues like lateral epicondylosis (tennis elbow) are seven to ten times more common than their medial counterparts. These statistics highlight just how widespread and impactful tendon pain can be.
What are the common symptoms of tendinitis?
When a tendon decides to throw a party of pain, it usually comes with a predictable set of symptoms. If you’re experiencing tendonitis, you might notice:
- Dull ache near a joint: This is often the primary complaint, a persistent, throbbing pain that can be quite bothersome.
- Pain that worsens with movement: Activities that use the affected tendon will typically increase the discomfort.
- Tenderness to the touch: The area directly over the inflamed tendon will likely feel sore when pressed.
- Mild swelling: You might see some puffiness or feel warmth around the affected joint.
- Stiffness or tightness: The joint connected to the tendon might feel rigid, especially first thing in the morning or after periods of inactivity.
- Grating sensation: Sometimes, you might feel a crackling or grinding when you move the tendon.
These symptoms commonly appear in areas like the shoulder, elbow, wrist, knee, and heel.
Is it tendinitis or tendinosis?
Here’s where things get a little tricky, but understanding the difference is crucial for effective heat cold therapy for tendonitis. Many people use “tendonitis” as a catch-all term for tendon pain, but there’s a significant distinction between tendinitis and tendinosis, and this difference directly affects our treatment choices.
Tendonitis is an acute condition, meaning it has a sudden onset. The “-itis” suffix literally means inflammation. So, tendonitis is when your tendon is inflamed or irritated, often as a result of a sudden injury or a new, aggressive repetitive motion. It’s characterized by inflammation, pain, and sometimes visible swelling. Think of it as a fresh injury, like twisting your ankle.
Tendinosis, on the other hand, is a chronic condition that develops over time. It doesn’t involve significant inflammation. Instead, it’s characterized by the degeneration of the tendon’s collagen, the structural protein that gives tendons their strength and flexibility. This breakdown typically occurs due to repetitive actions over a long period, especially if short-term tendonitis goes untreated. Conditions often mislabeled as tendonitis, like tennis elbow (lateral epicondylosis) or swimmer’s shoulder, are actually more commonly tendinosis. Since there’s no inflammation to treat with tendinosis, ice is usually ineffective. Instead, we focus on treatments that encourage blood flow and relieve stiffness.
For a deeper dive into this distinction, you can explore resources like The difference between tendinitis and tendinosis. Recognizing whether you’re dealing with acute inflammation (tendonitis) or chronic degeneration (tendinosis) is the first step toward choosing the right therapeutic approach.
The Great Debate: A Guide to Heat Cold Therapy for Tendonitis
So, you’ve got tendon pain. The big question is: do you reach for the ice pack or the heating pad? This is the core of heat cold therapy for tendonitis, and getting it right can make all the difference in your recovery journey. Both methods offer unique benefits, and neither is inherently “better”—it’s all about timing and what your body needs at that moment.
To help you make the best choice, we’ve put together a quick comparison table:
| Therapy Type | When to Use | Primary Benefit | How it Works | Best For |
|---|---|---|---|---|
| Ice Therapy | Acute injuries (first 24-72 hours), sudden pain, swelling, redness, heat | Reduces inflammation, numbs pain | Constricts blood vessels, decreases blood flow, slows nerve impulses | New sprains, strains, post-activity flare-ups, immediate injury response |
| Heat Therapy | Chronic pain (after 72 hours), stiffness, dull ache, muscle tension | Increases blood flow, relaxes muscles, improves flexibility | Dilates blood vessels, increases circulation, soothes tight tissues | Morning stiffness, chronic tendonosis, before stretching/exercise, muscle soreness |
When should I use ice for tendonitis?
Ice therapy, also known as cryotherapy, is your go-to friend for fresh injuries. If you’ve just experienced a sudden injury to a tendon, or if your tendonitis has flared up with sharp pain, visible swelling, redness, or warmth to the touch, ice is the answer.
Here’s why ice works wonders in these situations:
- Acute Phase Relief: Ice is most effective in the first 24 to 72 hours after an injury or during a flare-up. It helps manage the immediate inflammatory response.
- Sudden, Sharp Pain: If the pain is sharp and intense, ice can help numb the area, providing much-needed relief.
- Visible Swelling and Redness: Ice therapy causes vasoconstriction, meaning it narrows the blood vessels. This reduces blood flow to the injured area, which in turn minimizes swelling and inflammation. Less swelling means less pressure on nerve endings, leading to less pain.
- After an Activity that Causes a Flare-up: If you know a certain activity aggravates your tendonitis, applying ice afterward can help prevent excessive inflammation.
Think of ice as the fire extinguisher for inflammation. It calms things down, reduces the “heat” of the injury, and helps control the initial pain and swelling.
When should I use heat for tendonitis?
While ice is for acute situations, heat therapy (thermotherapy) steps in for the long haul, particularly for chronic tendon pain or tendinosis. If your pain has been lingering for more than 72 hours, or if you’re experiencing persistent stiffness, a dull ache without visible swelling, or muscle tension around the tendon, heat is likely your best bet.
The benefits of heat therapy for these chronic conditions are quite different:
- Chronic Phase Relief: Heat is generally recommended after the initial inflammatory phase has passed. Using heat too early on a fresh injury can actually increase swelling and make things worse!
- Persistent Stiffness and Soreness: Heat promotes vasodilation, which means it widens blood vessels. This increased blood flow delivers more oxygen and nutrients to the area, which can help stimulate healing in chronically damaged tendons. It also helps to relax tight muscles surrounding the tendon, easing stiffness.
- Dull, Aching Pain without Swelling: For that nagging, deep ache where there’s no obvious swelling, heat can be incredibly soothing. It helps to ease muscle spasms and can improve overall comfort.
- Before Stretching or Activity: Applying heat before gentle stretching or physical therapy exercises can warm up the tissues, making them more pliable and flexible. This can improve the effectiveness of your exercises and reduce the risk of further injury.
So, if ice is the fire extinguisher, heat is the warm, comforting blanket that promotes circulation and relaxation. It’s about encouraging healing and easing stiffness rather than quelling acute inflammation.
How to Use Cold Therapy (Cryotherapy) for Tendonitis
When it comes to heat cold therapy for tendonitis, applying ice correctly is just as important as knowing when to use it. Our goal is to reduce inflammation and pain without causing further harm.

Common methods for cold therapy include:
- Ice packs: These are readily available and convenient. You can use gel packs from the freezer or even a bag of frozen vegetables (peas or corn conform well to body parts!).
- Ice massage: For smaller, more localized areas, gently rubbing an ice cube (or an ice cup) in small circles over the affected tendon can be very effective.
- PRICE method: This is a classic acronym for managing acute injuries: Protect, Rest, Ice, Compress, Elevate. Incorporating these steps can significantly aid initial recovery by reducing inflammation and providing pain relief. For example, elevating the injured area, such as comfortably setting your wrist or foot in an liftd position, helps to reduce swelling.
What are the best practices for applying ice?
To get the most out of your ice therapy and keep yourself safe, follow these best practices:
- Wrap in a towel: Never, ever apply ice directly to your skin. Always place a thin towel or cloth between the ice pack and your skin. This protects against ice burns and skin damage.
- Apply for 15-20 minutes: This is the sweet spot for effective icing. Longer than this can actually cause a rebound effect where blood flow increases, or even lead to frostbite.
- Wait 4-6 hours between applications: Give your skin and tissues time to return to normal temperature. You can reapply ice as many times as necessary throughout the day, but allow at least 30 minutes between icing sessions.
- Move the ice around: If you’re using an ice cube for massage, keep it moving. If you’re using a pack, ensure it’s not sitting too long in one spot to prevent frostbite.
- Lift the injured area: Whenever possible, lift the injured area above your heart. This uses gravity to help reduce swelling.
For more detailed guidance on safe icing techniques, you can refer to resources like More on safe icing techniques.
Are there risks with using ice?
While ice therapy is generally safe, it’s not without its risks if misused or applied to individuals with certain conditions:
- Frostbite and skin damage: Applying ice directly to the skin or for too long can cause frostbite, leading to blisters and tissue damage. Always use a barrier!
- Nerve damage: Prolonged application in one spot, especially over superficial nerves, can potentially cause temporary or even permanent nerve damage.
- Not for people with circulatory issues: If you have conditions like poor circulation, peripheral vascular disease, or Raynaud’s syndrome, cold therapy can be detrimental. It constricts blood vessels, which can be dangerous for those whose circulation is already compromised.
- Decreased skin sensation: Individuals with conditions that cause decreased skin sensation (e.g., diabetes) need to be extra cautious, as they may not feel when the ice is causing harm.
Always listen to your body. If you experience unusual pain, numbness, or skin discoloration, remove the ice immediately.
How to Use Heat Therapy (Thermotherapy) for Tendonitis
Once the initial inflammation has subsided, or if you’re dealing with chronic stiffness and pain, heat therapy becomes a valuable tool in your heat cold therapy for tendonitis arsenal. The goal here is to increase blood flow, relax muscles, and improve flexibility.

There are several effective ways to apply heat:
- Moist heat packs: These are excellent because moisture increases heat penetration, allowing the warmth to reach deeper tissues. They’re ideal for larger joints like shoulders, knees, and elbows.
- Warm towels or compresses: Dampen a towel with warm (not scalding) water and apply it to the affected area.
- Hot water bottles: A classic, simple way to apply localized heat. Just make sure it’s not too hot and always use a cover.
- Warm bath or shower: For more widespread stiffness or muscle tension, a warm bath or shower can be incredibly relaxing and help prepare your body for stretching or activity.
Heat therapy works by causing vasodilation, which widens blood vessels. This influx of blood brings healing nutrients to the area and helps flush away waste products. It also helps to relax tight muscles and connective tissues, making them more pliable and less painful.
What are the best practices for applying heat?
Just like with ice, proper application of heat is key for safety and effectiveness:
- Use warm, not hot, temperatures: The heat should feel comfortable and soothing, never painful or scalding. Temperatures above 113°F can be painful, and anything above 122°F can burn the skin. Aim for a maximum of 40-45°C (104°F).
- Protect skin with a barrier: Even with comfortable temperatures, always place a towel or cloth between the heat source and your skin to prevent burns, especially if using an electric heating pad or hot water bottle.
- Apply for 15-20 minutes: For localized application, this duration is usually sufficient to achieve the desired effects. For a warm bath, you might enjoy longer sessions for general relaxation.
- Do not use on a fresh, swollen injury: This is critical! If there’s any sign of acute inflammation (swelling, redness, heat), heat will make it worse. Wait at least 72 hours after an acute injury before introducing heat.
- Consider longer sessions for severe stiffness: For chronic conditions, longer sessions in a warm bath might be beneficial.
- Apply before activity: Using heat before stretching or exercises can help warm up the muscles and tendons, making them more flexible.
For more insights into when and how to apply heat effectively, check out our article: Does Heat Help Tendonitis? Answers & Tips for Effective Relief.
What are the risks of using heat?
While heat therapy can be wonderfully soothing, be aware of the potential risks:
- Burns: The most obvious risk is burning your skin. Always check the temperature, use a barrier, and never apply heat that feels uncomfortably hot.
- Increased inflammation if used too soon: Applying heat to a fresh injury (within the first 72 hours) or an area that is already swollen, red, or hot will increase blood flow and can significantly worsen the inflammation and swelling.
- Not for areas with poor sensation: Similar to ice, if you have conditions that reduce skin sensation (like neuropathy or diabetes), you might not feel when the heat is too intense, leading to burns.
- Do not fall asleep with a heating pad: This is a common mistake that can lead to severe burns. If you’re feeling sleepy, turn off the heating pad before drifting off.
- Contraindications: Avoid heat if you have bleeding, are using topical menthol or medicated ointments, have burned or radiated skin, vascular diseases, or deep vein thrombosis (DVT).
Always err on the side of caution. If heat causes increased pain, swelling, or any discomfort, remove it immediately.
Beyond the Basics: Advanced and Complementary Treatments
While ice and heat are fantastic tools for self-care, they are often just one part of a comprehensive recovery plan for heat cold therapy for tendonitis. For many, combining these therapies with other treatments and getting professional guidance is the fastest path to lasting relief. Our sports medicine team at Center for Specialty Care specializes in helping individuals in Minnesota and Iowa recover from these types of injuries. Visit our Sports Medicine page to learn more about our approach.
Can you combine heat and ice (contrast therapy)?
Yes, you absolutely can! This is known as contrast therapy, and it can be a highly effective approach, especially for subacute or chronic tendon issues where there’s some lingering stiffness or minor swelling.
Contrast therapy involves alternating between hot and cold applications. The theory is that this creates a “pumping action” in the blood vessels: heat causes them to dilate (widen), and cold causes them to constrict (narrow). This rapid change in blood flow is thought to help improve circulation, reduce stiffness, and flush out metabolic waste products, potentially promoting healing.
Here’s how to generally approach it:
- Start with heat: Apply heat for 3-5 minutes.
- Switch to cold: Apply cold for 1 minute.
- Repeat: Cycle through this sequence 3-5 times.
- End with cold: If there’s any residual swelling or if you’re dealing with an injury that still has an inflammatory component, always finish with a cold application.
Contrast baths, where you immerse the affected body part alternately in warm and cold water, are a common method for this. This can be particularly beneficial if you experience minor swelling but find that heat provides comfort.
What are the best practices for heat cold therapy for tendonitis in specific areas?
The principles of heat cold therapy for tendonitis remain consistent, but some specific areas benefit from custom application:
- Shoulder (Rotator Cuff): Rotator cuff tendinopathy is very common, affecting one in 50 adults. For acute flare-ups or after aggravating activity, ice is best to reduce inflammation. For chronic stiffness or before exercises to improve range of motion, heat can be very beneficial. Our team can help you develop a targeted plan. To learn more about recovery, visit our Shoulder Treatment: Physical Therapy Tips for Fast Recovery.
- Elbow (Tennis/Golfer’s Elbow): These conditions, often involving lateral epicondylosis (tennis elbow), are frequently cases of tendinosis rather than true tendonitis. Since they involve tendon degeneration and stiffness more than acute inflammation, heat is often preferred. Applying heat before gentle stretches and strengthening exercises can significantly improve flexibility and reduce stiffness.
- Achilles Tendon: Achilles tendinopathy is common among adult runners. If you’re a runner experiencing pain after a workout, ice is excellent for reducing any post-activity inflammation. For morning stiffness, a warm compress or warm shower on the Achilles can help loosen things up before you start your day. For more information, read our guide on Achilles Tendonitis 101.
Can you combine treatments with heat cold therapy for tendonitis?
Absolutely! Heat cold therapy for tendonitis is rarely a standalone solution for long-term recovery. It’s often most effective when integrated into a broader treatment strategy. Here are some complementary treatments we often recommend:
- Rest and activity modification: This is foundational. Resting the injured tendon and modifying activities that aggravate it are crucial to allow healing. Sometimes, this means taking a break from sports or adjusting your work ergonomics.
- Stretching and strengthening exercises: Once the acute pain subsides, a progressive exercise program, often focusing on eccentric (lengthening) exercises, is vital for rebuilding tendon strength and flexibility. Our physical therapists are experts in this area. You can find out more about our services here: Physical Therapy.
- Anti-inflammatory medications: Over-the-counter NSAIDs (nonsteroidal anti-inflammatory drugs) can help manage pain and inflammation in the short term. Always consult with a healthcare provider before starting any new medication.
- Braces or orthotics: For certain types of tendonitis, supportive braces or custom orthotics can help unload the tendon and provide stability, aiding in recovery.
- Physical Therapy: A structured physical therapy program is often recommended to strengthen surrounding muscles, improve flexibility, and correct biomechanical imbalances that may have contributed to the tendonitis.
- Massage Therapy: Can help reduce muscle tension and improve blood flow to the affected area.
- Cortisone injections: In some cases, a corticosteroid injection might be considered for short-term pain relief, but these are typically used cautiously due to potential long-term effects on tendon health.
By combining the targeted effects of heat and cold with these other approaches, you create a powerful healing environment for your tendons.
When to See a Doctor for Tendonitis Pain
While heat cold therapy for tendonitis and other home remedies can be incredibly effective, there are times when professional medical advice is essential. We encourage you to listen to your body and recognize when it’s time to seek a specialist’s opinion.
You should consider seeing a doctor if:
- Pain doesn’t improve after a week of self-care: If you’ve been diligently applying ice or heat and resting the area, but your symptoms persist or worsen after about a week, it’s time for a professional evaluation.
- Pain that disrupts daily activities or sleep: If your tendon pain is significantly impacting your quality of life, making it hard to work, exercise, or get a good night’s rest, a doctor can help diagnose the underlying issue and develop a more comprehensive treatment plan.
- Inability to move the joint: If you experience a sudden loss of range of motion or can’t move the affected joint at all, this could indicate a more serious injury, such as a tendon tear.
- A sudden, severe injury: Any sudden, sharp pain accompanied by a “pop” or immediate weakness should prompt a visit to a medical professional right away.
- Signs of infection: If you notice fever, increasing redness, warmth, or pus around the injured area, seek immediate medical attention, as this could indicate an infection.
At Center for Specialty Care in Fairmont, Minnesota, and our other locations in Estherville, Iowa, Buffalo Center, Iowa, and St. James, Minnesota, we pride ourselves on 100% patient satisfaction, personalized care, and quick appointment availability. We understand that pain can’t wait. Our dedicated team of specialists is here to provide accurate diagnoses and custom treatment plans, whether it’s through Pain Management techniques or more advanced orthopedic interventions.
For a comprehensive evaluation of your joint pain, don’t hesitate to contact our orthopedics team. We’re here to help you get back to living your life to the fullest.



