Intracept Explained: Targeting Back Pain at its Source
February 19, 2026
Say Goodbye to Pain: Effective Ingrown Toenail Fixes
February 21, 2026Is ice good for tendonitis: 3-Day Ultimate Relief
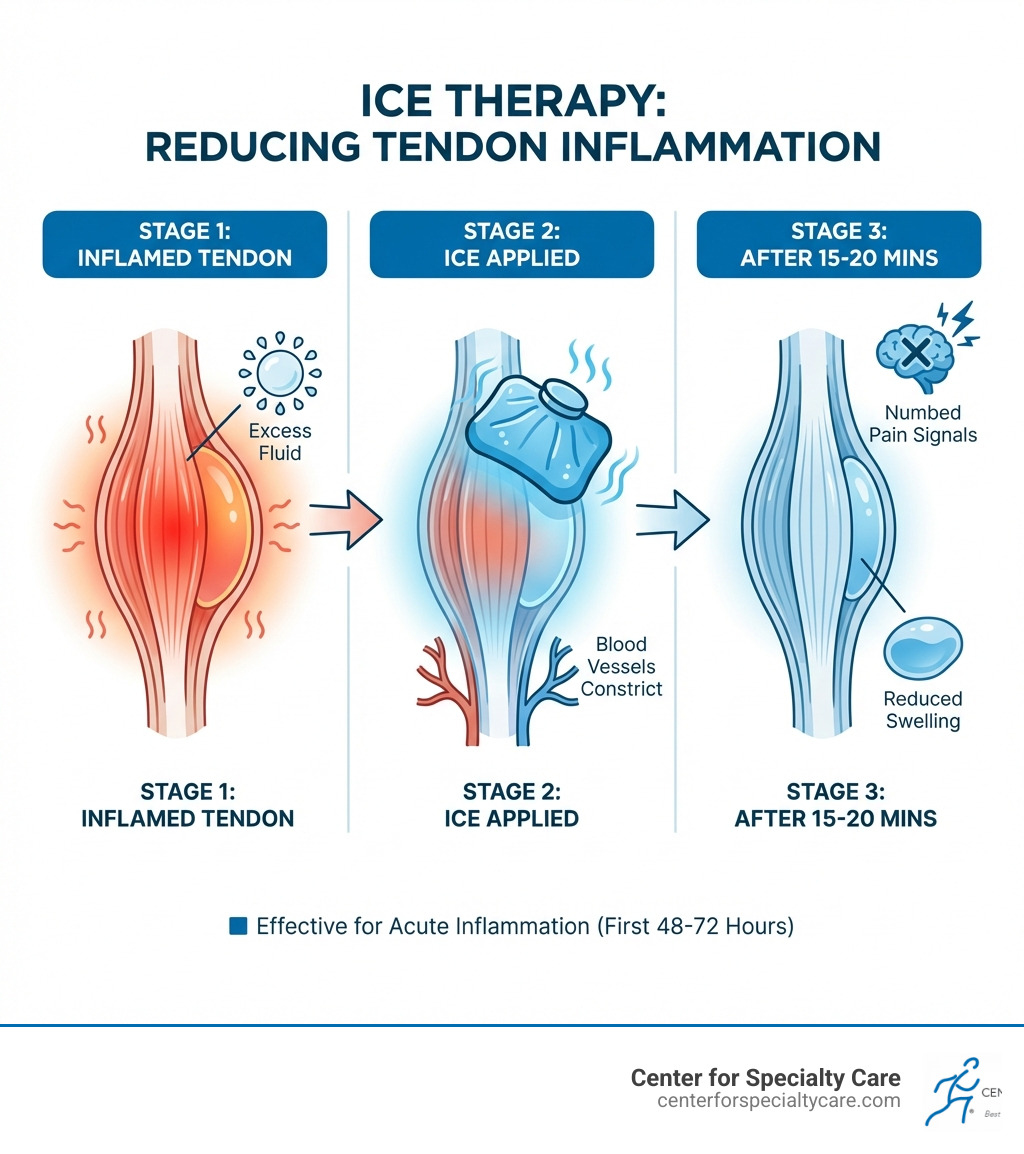
Why Ice Therapy Matters for Tendon Injuries
Is ice good for tendonitis? Yes, ice is highly effective for acute tendonitis—especially during the first 48 to 72 hours after injury or flare-up. Ice therapy (cryotherapy) provides immediate pain relief, reduces swelling, and controls inflammation by constricting blood vessels and numbing nerve endings. However, ice works best for fresh injuries with active inflammation, not for chronic tendon degeneration (tendinosis).
Quick Answer: When Ice Helps Tendonitis
- ✓ Acute injuries – Sharp pain, visible swelling, recent onset (within 3 days)
- ✓ Post-activity flare-ups – Fresh inflammation after exercise or work
- ✓ Pain relief – Numbs nerve endings almost immediately
- ✓ Swelling reduction – Keeps excess fluid from building up in tissues
- ✓ Inflammation control – Balances healing response without slowing recovery
When Ice May NOT Help
- ✗ Chronic tendinosis – Long-term degeneration without active swelling
- ✗ Stiffness-dominant pain – Heat therapy may be more effective
If you’ve ever pressed a frozen bag of peas against a swollen elbow or wrapped an ice pack around an aching shoulder, you’ve already used one of the most accessible tools for managing tendon pain. But understanding when and how to use ice makes all the difference between effective relief and wasted effort.
The research is clear: ice works best for acute injuries—those fresh, painful flare-ups that happen within the first 48 to 72 hours. When you apply an ice pack correctly, you get several benefits wrapped up in one simple treatment. The pain relief happens almost immediately as cold naturally numbs nerve endings. Reduced swelling is another major win—nobody wants to walk around with a puffy, tender joint. Ice keeps that excess fluid from building up in your tissues, which means less pressure and discomfort.
The decreased inflammation benefit is where ice really shines. While some inflammation is necessary for healing, too much can actually slow down your recovery. Ice helps keep this response balanced—enough to promote healing, but not so much that it causes additional problems.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon with over three decades of experience treating tendon injuries at the Center for Specialty Care in Fairmont, Minnesota. Throughout my career, I’ve helped countless patients answer “is ice good for tendonitis” based on their specific injury, and I’ll guide you through the evidence-based approach to using ice therapy effectively.
Is ice good for tendonitis basics:
Understanding Tendonitis: Is It Inflammation or Degeneration?
Before we dive deeper into ice therapy, it’s crucial to understand what we’re actually treating. The terms “tendonitis” and “tendinosis” are often used interchangeably, but they describe two distinct conditions that require different treatment approaches. Knowing the difference helps us decide whether is ice good for tendonitis in your specific situation, or if another therapy might be more beneficial.
Tendons are tough, fibrous tissues that connect muscles to bones, allowing for movement. They are like strong, flexible ropes that transmit force. When these ropes get irritated or damaged, that’s when tendon pain begins.

For a deeper understanding of these conditions and why this difference matters so much for your recovery, we highly recommend exploring More on Tendinopathy vs Tendinitis.
Tendonitis: The Acute “Itis”
Tendonitis is when a tendon swells and becomes inflamed after an injury. The “itis” suffix signifies inflammation. This is typically an acute, or sudden onset, condition. Think of it as your body’s immediate emergency response to an injury.
What to look for:
- Sharp pain: Often immediate and intense, especially with movement.
- Recent injury: Usually linked to a specific event, like a sudden strain, a new repetitive activity, or an increase in exercise intensity.
- Swelling: The affected area may appear visibly puffy.
- Redness and warmth: The skin around the tendon might be red and feel warm to the touch.
- Overuse: Caused by sudden, sharp movements or repetitive exercise, such as running, jumping, throwing, or repetitive actions at work.
If you’ve ever felt a dull, achy, or throbbing pain coming from your shoulder and arm, or a sharp, stabbing pain when reaching overhead, you may be experiencing tendonitis in your rotator cuff or bicep tendon. This acute inflammation is where ice truly shines.
Tendinosis: The Chronic “Osis”
Tendinosis, on the other hand, is a chronic condition characterized by the degeneration of the tendon’s collagen fibers. The “osis” suffix indicates a degenerative process, meaning there’s little to no inflammation present. This condition develops over time, often from repeated overuse where short-term tendonitis goes untreated, leading to the breakdown of the tendon’s structure.
What to look for:
- Dull ache: A persistent, nagging pain rather than a sharp, acute one.
- Long-term pain: Symptoms that have lasted for weeks, months, or even years.
- Stiffness: Especially noticeable in the morning or after periods of inactivity.
- Repetitive strain: Often caused by chronic overuse and microtrauma without adequate healing time.
- No significant swelling: The area might feel thickened or lumpy, but generally won’t show the visible puffiness of acute inflammation.
Well-known conditions like tennis elbow (lateral epicondylosis) and swimmer’s shoulder are sometimes incorrectly labeled as tendonitis—yet these are actually tendinosis. In these cases, the primary issue isn’t inflammation, but rather the deterioration of the tendon itself. This distinction is vital because the treatment approach for tendinosis often differs significantly from that of acute tendonitis, favoring heat and other therapies to encourage blood flow and tissue repair.
So, Is Ice Good for Tendonitis? The Cold, Hard Facts
Now that we understand the difference between tendonitis and tendinosis, we can confidently answer the question: is ice good for tendonitis? For acute tendonitis, absolutely! Ice therapy, or cryotherapy, is a cornerstone of immediate care for these types of injuries. Our Sports Medicine specialists often recommend it as a first-line treatment.
Ice works best for acute injuries—those fresh, painful flare-ups that happen within the first 48 to 72 hours. When you apply an ice pack for tendonitis correctly, you’re getting several benefits wrapped up in one simple treatment.
The Benefits of Using an Ice Pack for Tendonitis
Let’s break down why cold therapy is so effective for acute tendonitis:
- Pain Management: The pain relief happens almost immediately—cold naturally numbs nerve endings, which is why that ice pack feels so good on a fresh injury. This numbing effect reduces your sensitivity to pain, providing much-needed comfort.
- Swelling Control: Reduced swelling is another major win. Nobody wants to walk around with a puffy, tender joint. Ice keeps that excess fluid from building up in your tissues, which means less pressure and discomfort. Cold therapy can significantly reduce swelling that is tied to pain, especially around a joint or tendon.
- Inflammation Reduction: The decreased inflammation benefit is where ice really shines. While some inflammation is necessary for healing, too much can actually slow down your recovery. Ice helps keep this response balanced—enough to promote healing, but not so much that it causes additional problems. By causing vasoconstriction (narrowing of blood vessels), ice reduces blood flow to the injured area, limiting the inflammatory response.
- Slowing Metabolic Rate: Ice also slows the metabolic rate of the injured cells, which can help reduce secondary tissue damage in the hours following an acute injury.
As our colleagues at Hopkins Medicine highlight, cryotherapy lowers skin temperature and reduces nerve activity, both contributing to pain and swelling reduction. Learn more about this approach on their page about Cryotherapy Cold Therapy for Pain Management.
When is ice good for tendonitis?
We recommend reaching for the ice pack when your tendon pain presents with these characteristics:
- Fresh flare-ups: If you’ve just overdone it and your tendon is feeling acutely painful and irritated.
- Post-activity pain: After a workout, a long day at work with repetitive tasks, or any activity that triggers sharp pain and inflammation.
- Visible swelling: If the affected area looks puffy or feels unusually full.
- Sharp, acute pain: When the pain is sudden, intense, and feels like a fresh injury.
- Within 3 days of injury: Ice is most effective in the initial 48-72 hours following an acute injury or the onset of significant symptoms.
Ice is a helpful solution for controlling pain and swelling, but it does not speed up healing directly. Its role is to create a better healing environment by managing the immediate inflammatory response.
The R.I.C.E. Method: How to Apply Ice for Tendonitis Correctly
When it comes to treating acute tendonitis, we always turn to the tried-and-true R.I.C.E. method. This acronym stands for Rest, Ice, Compression, and Elevation, and it’s a widely accepted first-aid treatment for acute soft tissue injuries, including tendonitis. Applying ice correctly is just one part of this comprehensive approach.

Step-by-Step Guide to Icing Your Tendon
To ensure you get the maximum benefit from ice therapy and avoid any potential risks, follow these steps:
- Rest the Affected Area: This is the “R” in R.I.C.E. Stop the activity that caused the pain. Giving your tendon a break prevents further damage and allows the healing process to begin.
- Prepare Your Ice Pack: You can use a commercial gel pack, a bag of frozen peas, or even crushed ice in a plastic bag.
- Use a Barrier: Never apply ice directly to your skin! Always wrap your ice pack in a thin towel, cloth, or pillowcase. This prevents frostbite and skin damage.
- Apply for 15-20 Minute Sessions: Stick to 15-20 minute sessions—long enough to get the benefits, but not so long that you risk skin damage. For targeted relief, an ice massage technique can be very effective. Freeze water in a Styrofoam cup, then tear off the top to expose the ice. Rub the exposed ice directly over the painful tendon for 2 to 4 minutes until the area becomes numb. You’ll typically feel a progression of sensations: cold and painful, then burning, aching, and finally numbness.
- Frequency is Key: For frequency, aim for every 4-6 hours during those crucial first few days. Some sources suggest every 2-3 hours while awake for the first 24-72 hours after injury. Repeated applications of melting ice water through a wet towel for 10-minute periods are most effective.
- Lift the Injured Area: This is the “E” in R.I.C.E. Comfortably set your wrist, foot, or affected area in an liftd position (above heart level) to help reduce swelling.
- Allow for Re-warming: After each session, allow at least 30 minutes for your skin to warm up to the touch before reapplying ice. This is crucial for preventing tissue damage and allowing blood flow to return.
- Consider Compression: The “C” in R.I.C.E. Gently wrap the area with an elastic bandage, tube bandage, or soft brace. Ensure it is snug but not tight—you should still be able to feel your pulse below the bandage and move your fingers or toes easily. Remove compression before going to bed.
Consistency is key. Performing ice massage two to four times a day for three to seven days can lead to noticeable improvement, often 75% or better, in acute tendonitis pain.
What Are the Risks of Using Ice for Tendonitis?
While ice therapy is generally safe and highly beneficial, improper use can lead to risks:
- Frostbite and Skin Damage: The most common risk comes from applying ice directly to the skin or for too long. Always use a barrier and adhere to the 15-20 minute rule. If the area becomes numb, it’s time to remove the ice.
- Nerve Irritation: Prolonged direct contact with ice can potentially irritate superficial nerves, especially in areas close to the skin’s surface.
- Increased Stiffness: Overuse of ice, particularly beyond the acute phase, can sometimes increase stiffness in the joint or tendon, potentially hindering rehabilitation.
- Masking Pain: While pain relief is a benefit, it’s important not to overdo activity just because the pain is numbed. Listen to your body and avoid movements that cause sharp pain.
- Contraindications: If you have certain medical conditions, such as diabetes affecting sensation, peripheral vascular disease, or Raynaud’s phenomenon, consult with one of our healthcare providers in Fairmont, Estherville, Buffalo Center, or St. James before using ice therapy.
Always monitor your skin for any signs of damage, such as excessive redness, blistering, or changes in sensation. If you experience any unusual symptoms, stop icing immediately and contact a medical professional.
The Other Side of the Coin: When to Use Heat and Other Therapies
We’ve established that is ice good for tendonitis when it’s an acute, inflammatory issue. But what about the other side of the coin? When does heat come into play, and what other treatments should we consider for tendon pain? The secret to choosing between ice and heat lies in understanding what your tendon is actually going through. Our Pain Management specialists often help patients steer this choice.
Here’s a quick comparison to guide your decision:
| Feature | Ice Therapy (Cryotherapy) | Heat Therapy (Thermotherapy) |
|---|---|---|
| Primary Goal | Reduce inflammation, swelling, pain | Increase blood flow, relax muscles, reduce stiffness |
| When to Use | Acute injuries (first 48-72 hrs), fresh flare-ups, sharp pain, visible swelling | Chronic pain, stiffness, muscle tension, before activity/stretching |
| Mechanism | Vasoconstriction (narrows blood vessels), numbs nerves | Vasodilation (widens blood vessels), muscle relaxation |
| Application | 15-20 min sessions, with barrier, every 4-6 hrs | 15-20 min sessions, warm (not hot), for chronic issues |
| Avoid If | Chronic stiffness without inflammation, open wounds | Acute inflammation, swelling, fresh injuries (first 72 hrs) |
When and How to Use Heat for Tendonitis
Heat therapy is the gentle, nurturing companion to ice’s sharp, immediate relief. It’s generally recommended for chronic tendon pain or tendinosis, where the primary goal is to increase blood flow, relax stiff muscles, and promote healing rather than to reduce acute inflammation.
When to use heat:
- Chronic Tendinosis: When you experience repeated cases of pain and stiffness from the same tendon, it’s more likely a case of tendinosis. There is no significant swelling to treat, so ice is ineffective. Instead, you should apply heat to encourage blood flow and relieve stiffness.
- Stiffness: If your tendon feels stiff, especially in the morning or after prolonged inactivity.
- Before Activity: Applying heat before gentle stretching or rehabilitative exercises can help warm up the tissues, improve flexibility, and reduce the risk of further injury.
- Muscle Relaxation: Heat can alleviate muscle tension and soothe sore muscles surrounding the affected tendon.
Proper application techniques for heat:
- Warm, Not Hot: Use a gel pack, heating pad, or warm compress. Ensure it’s comfortably warm, not hot enough to cause burns.
- Duration: Apply heat for 15-20 minutes per session.
- Avoid Acute Injuries: Heat therapy should not be used on acute injuries, or within the first 72 hours after an injury, as it can increase inflammation and swelling.
- Moist Heat: Moist heat, like a warm, damp towel, can penetrate deeper than dry heat.
- Watch Your Skin: Just like with ice, be mindful of your skin. Check frequently for any signs of redness or discomfort.
For more detailed guidance on when and how to use heat therapy, including for conditions like chronic tendonitis, check out our article: Does Heat Help Tendonitis? Answers & Tips for Effective Relief.
Contrast Therapy: Some patients find relief by alternating between hot and cold therapy, known as contrast therapy. This can be beneficial for lingering swelling or stiffness after the initial acute phase has passed. The idea is that the alternating temperatures create a “pumping” effect, which can help improve circulation and reduce swelling. Typically, you would apply heat for 3-4 minutes, followed by cold for 1 minute, repeating this cycle 3-5 times and ending with cold.
Beyond Ice and Heat: Other Treatment Options
While ice and heat are excellent tools for managing symptoms, they are rarely the sole solution for tendonitis or tendinosis. A comprehensive approach often includes other therapies to address the root cause and promote long-term healing.
- Stretching: Gentle stretching can help improve flexibility and range of motion in the affected tendon and surrounding muscles.
- Strengthening Exercises: Eccentric strengthening, where the muscle lengthens under tension, is particularly effective for tendinopathies. This type of exercise can help rebuild collagen and strengthen the tendon. Our Physical Therapy team in Fairmont, Estherville, Buffalo Center, and St. James can design a personalized exercise program for you.
- Medication: Over-the-counter pain relievers like acetaminophen, ibuprofen, or naproxen can help manage pain and inflammation. In some cases, your doctor may prescribe stronger anti-inflammatory medications or consider corticosteroid injections for short-term pain relief (though these don’t alter long-term outcomes and aren’t always recommended due to potential tendon weakening).
- Technique Modification: For those whose tendonitis is caused by repetitive motions in sports or work, modifying technique or making ergonomic adjustments can be crucial for preventing recurrence.
- Orthotics and Braces: These can help support, unload, and protect the tendon during activity, especially for conditions like Achilles Tendonitis or patellar tendonitis.
The goal is always to reduce pain, restore function, and prevent future injuries. A combination of therapies, custom to your specific condition, is often the most effective path to recovery.
Prevention and When to Seek Professional Help
An ounce of prevention is worth a pound of cure, especially when it comes to tendonitis. Many cases of tendon pain can be avoided with mindful practices. However, knowing when to stop self-treating and seek professional medical attention is equally vital for your long-term health and recovery.
How Can Tendinitis Be Prevented?
Incorporating these habits into your daily routine can significantly reduce your risk of developing tendonitis:
- Stretching Routines: Regular stretching, especially before and after physical activity, helps maintain flexibility in your tendons and muscles. Warm up before exercising and gently stretch afterward.
- Strengthening Supporting Muscles: Strong muscles surrounding a tendon help distribute stress and protect the tendon from overload. Focus on balanced strength training. For example, for shoulder tendonitis, strengthening your abdominals, upper back postural muscles, and rotator cuff muscles is key.
- Avoiding Overuse and Taking Breaks: Repetitive motions are a common culprit for tendonitis. Take regular breaks during repetitive tasks, whether at work or during sports. Avoid overexerting tired muscles.
- Proper Technique and Posture: Whether you’re playing a sport, lifting objects, or sitting at a desk, using proper technique and maintaining good posture is critical. Poor mechanics can place undue stress on tendons. For example, improving posture habits (head up and shoulders back) can prevent shoulder and arm tendonitis.
- Gradual Progression: Don’t suddenly increase the intensity, duration, or frequency of an activity. Gradually build up your tolerance to allow your tendons to adapt.
- Supportive Footwear/Gear: Wear appropriate and supportive shoes or gear for your activities.
- Hydration: Staying well-hydrated is important for overall tissue health.
- Smoking Cessation: Smoking can impair blood flow and slow down the healing process of tendon injuries.
When is it time to seek professional help for tendonitis?
While home remedies like ice therapy are effective for many mild cases of tendonitis, there are times when it’s crucial to consult a medical professional. As orthopedic specialists in Minnesota and Iowa, we emphasize personalized care and quick appointment availability, so don’t hesitate to reach out if you experience any concerning symptoms.
You should contact your healthcare provider or seek medical attention if:
- Pain Worsens or Doesn’t Improve: If your pain intensifies, or if you don’t see any improvement after 2-3 weeks of consistent home treatment with ice, rest, and over-the-counter pain relievers.
- Popping or Snapping Sound: If you heard a sudden popping or snapping sound at the time of injury, especially if accompanied by immediate pain and weakness. This could indicate a more severe injury, such as a tendon rupture.
- Inability to Move the Joint: If you cannot move the affected joint or limb, or if it feels unstable.
- Severe Swelling, Redness, and Warmth: While some inflammation is normal, excessive swelling, redness spreading beyond the immediate injury site, or warmth that doesn’t subside could indicate a more serious infection or condition.
- Deformity: If the joint appears deformed.
- Fever: If your tendon pain is accompanied by a fever.
- Numbness or Tingling: If you experience numbness, tingling, or weakness in the limb.
Early diagnosis and appropriate treatment can prevent acute tendonitis from progressing into chronic tendinosis or other more severe complications. We are here to provide comprehensive care and guide you through your recovery journey.
Take Control of Your Tendonitis Recovery
Understanding whether is ice good for tendonitis is a powerful first step in managing your pain and facilitating recovery. For acute tendonitis, characterized by sharp pain, swelling, and inflammation, ice therapy is your best friend. It provides immediate pain relief, reduces swelling, and helps control the inflammatory response, creating an optimal environment for healing.
However, we’ve also learned that not all tendon pain is created equal. For chronic stiffness and degeneration (tendinosis), heat therapy often proves more beneficial by promoting blood flow and muscle relaxation. The key is a correct diagnosis and understanding what your body is trying to tell you.
Always listen to your body. Pay attention to whether your pain is acute and inflammatory or chronic and stiff. Use ice for the former, and heat for the latter. And remember that these therapies are often just one part of a broader treatment plan that may include rest, physical therapy, medication, and lifestyle adjustments.
At Center for Specialty Care, we are committed to providing personalized care and helping you get back to living life without the constant worry of tendon pain. For a comprehensive evaluation and personalized treatment plan that goes beyond ice and heat therapy, explore our Orthopedics services. Our dedicated team in Fairmont, Estherville, Buffalo Center, and St. James is ready to help you take control of your tendonitis recovery.



