Twist and Shout No More: How to Sleep with Rotator Cuff Pain
February 18, 2026
Ice Therapy for Tendonitis: Reducing Swelling and Speeding Recovery
February 20, 2026Intracept: Proven 5-Year Pain Relief
Understanding Chronic Low Back Pain and the Intracept Solution
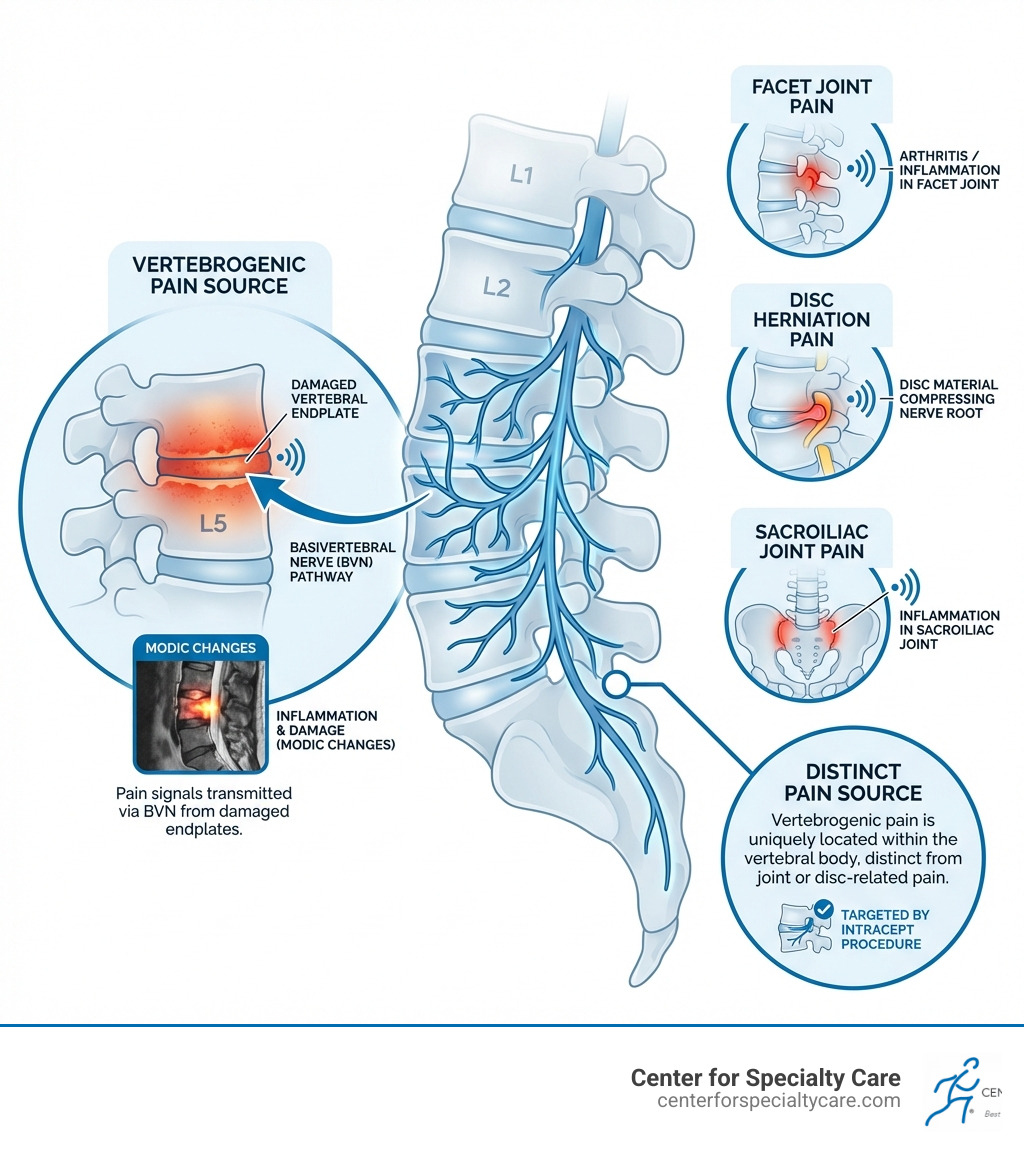
Intracept is a minimally invasive, outpatient procedure designed to treat chronic vertebrogenic low back pain by targeting and ablating the basivertebral nerve—the specific nerve transmitting pain signals from damaged vertebral endplates to your brain.
Quick Facts: What is the Intracept Procedure?
- What it treats: Vertebrogenic pain caused by damaged vertebral endplates
- How it works: Uses radiofrequency energy to heat and disable the basivertebral nerve
- Procedure type: Minimally invasive, outpatient, implant-free
- Duration: 60-90 minutes
- Recovery: Most people return to normal activities within several days to two weeks
- Pain relief: Typically begins within 2 weeks to 3 months
- Results: Long-lasting relief, proven effective in over 50,000 patients
If you’ve been living with chronic low back pain for six months or longer—pain that gets worse with sitting, bending forward, or physical activity—you’re not alone. Roughly 900,000 new cases of lower back pain are diagnosed in the United States every year. For many people, the source of this pain lies deep within the vertebrae themselves, at the vertebral endplates where wear and tear over time creates inflammation and damage.
For years, patients cycling through physical therapy, medications, and injections without lasting relief had few options beyond major spinal surgery. The Intracept Procedure changed that landscape. It’s the only FDA-cleared treatment specifically designed to address vertebrogenic pain at its source.
As Dr. Corey Welchlin, a board-certified orthopedic surgeon with over three decades of experience, I’ve witnessed how chronic back pain steals quality of life from patients. At the Center for Specialty Care, we now offer the Intracept procedure as a proven option for patients whose pain originates from damaged vertebral endplates confirmed by MRI.
Intracept vocab explained:
What is Vertebrogenic Pain and How is it Diagnosed?
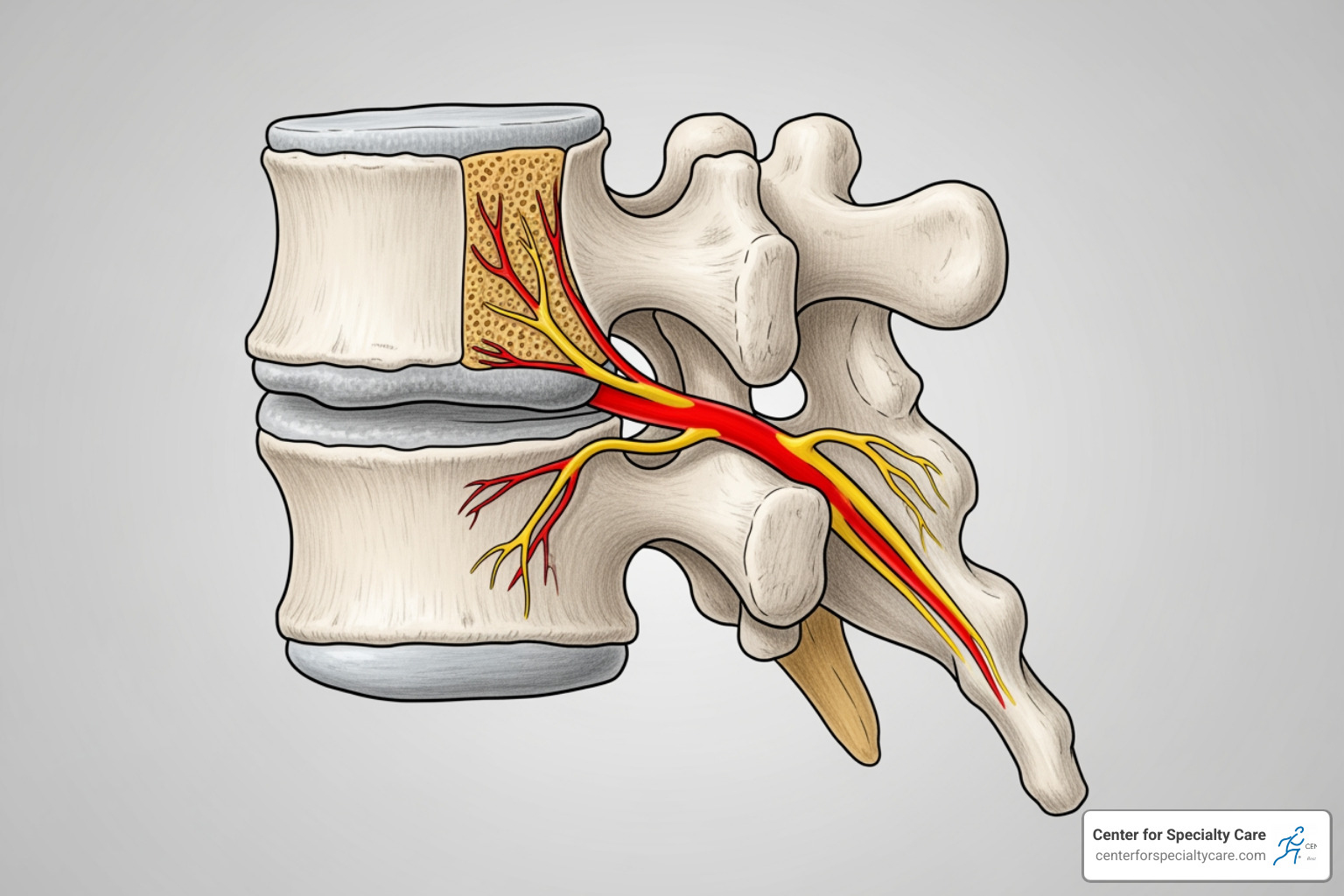
Imagine your spine as a stack of building blocks, with soft, cushioning discs in between. At the top and bottom of each vertebral body (the main part of the block) are specialized layers called vertebral endplates. These endplates are crucial for delivering nutrients to your discs and distributing the weight load across your spine. Over time, due to natural wear and tear, these endplates can become damaged. This damage leads to inflammation, and it’s this inflammation within the bone that triggers a very specific type of pain: vertebrogenic pain.
The pain signals from these damaged endplates are transmitted by tiny nerves called basivertebral nerves (BVN), which run through the bone of each vertebra. When these nerves are irritated, they send constant pain signals to your brain. If you’re experiencing vertebrogenic pain, you might describe it as a dull ache in the middle of your low back, often made worse by physical activity, prolonged sitting, or bending forward. It’s the kind of pain that makes you want to shift constantly, but finding a comfortable position feels impossible.
For more information on various back-related discomforts, you can explore our resources on common spinal conditions.
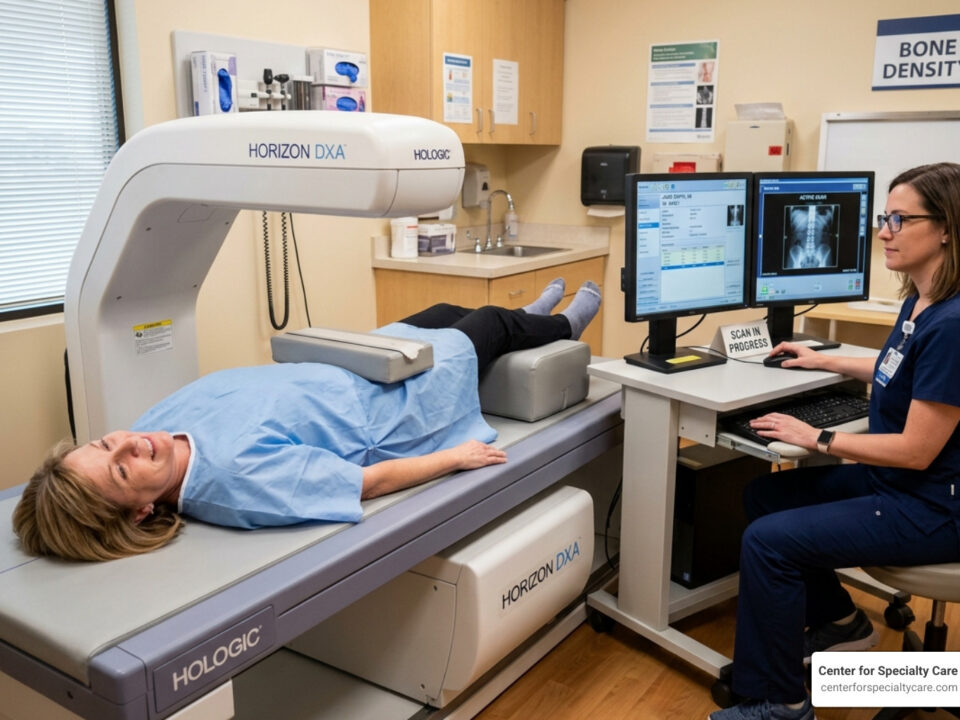
The Role of MRI and Modic Changes
So, how do we pinpoint if your chronic low back pain is actually vertebrogenic? The key diagnostic tool is a Magnetic Resonance Imaging (MRI) scan. An MRI provides detailed images of your spinal structures, allowing us to see changes within the vertebral endplates and bone marrow that are characteristic of vertebrogenic pain.
These specific changes are known as Modic changes, named after the physician who first described them. They appear in different “types” on an MRI, each indicating a different stage of vertebral endplate damage and inflammation:
- Modic Type 1 changes: These indicate acute inflammation and fluid accumulation (edema) within the bone marrow adjacent to the damaged endplate. Think of it like a fresh bruise inside your bone—it’s actively inflamed and often correlates strongly with pain. This is a primary indicator for the Intracept procedure.
- Modic Type 2 changes: These suggest that fat tissue has started to replace the bone marrow, signifying a more chronic, fatty degeneration. While less acute than Type 1, it still indicates ongoing issues and can be a strong indicator for Intracept candidacy.
- Modic Type 3 changes: These involve bone hardening and thickening (sclerosis), often representing a later, more stable stage of degeneration. While important for understanding spinal health, Type 3 changes are generally not the target for the Intracept procedure.
At Center for Specialty Care, our expert team, including Dr. Corey Welchlin, carefully reviews your MRI results to identify these Modic changes, ensuring we accurately diagnose the source of your pain. Understanding your spinal anatomy is the first step toward effective treatment. You can dig deeper into the intricacies of your spine with our comprehensive guide to spinal anatomy.
The Intracept Procedure: A Minimally Invasive Solution
After years of struggling with persistent low back pain, the idea of another treatment might feel daunting. That’s where the Intracept procedure steps in, offering a unique approach to pain relief. It’s a minimally invasive, implant-free, outpatient procedure that directly targets the basivertebral nerve, the culprit behind vertebrogenic pain. Unlike some other interventions, the Intracept procedure preserves the overall structure of your spine, meaning no fusion, no screws, and no rods are left behind. It’s about addressing the pain at its source without altering your spine’s natural mechanics.
At Center for Specialty Care, we’re proud to offer this advanced treatment as part of our comprehensive suite of orthopedic services, reflecting our commitment to providing innovative solutions for our patients in Fairmont, Estherville, Buffalo Center, and St. James.
How the Intracept Procedure Works
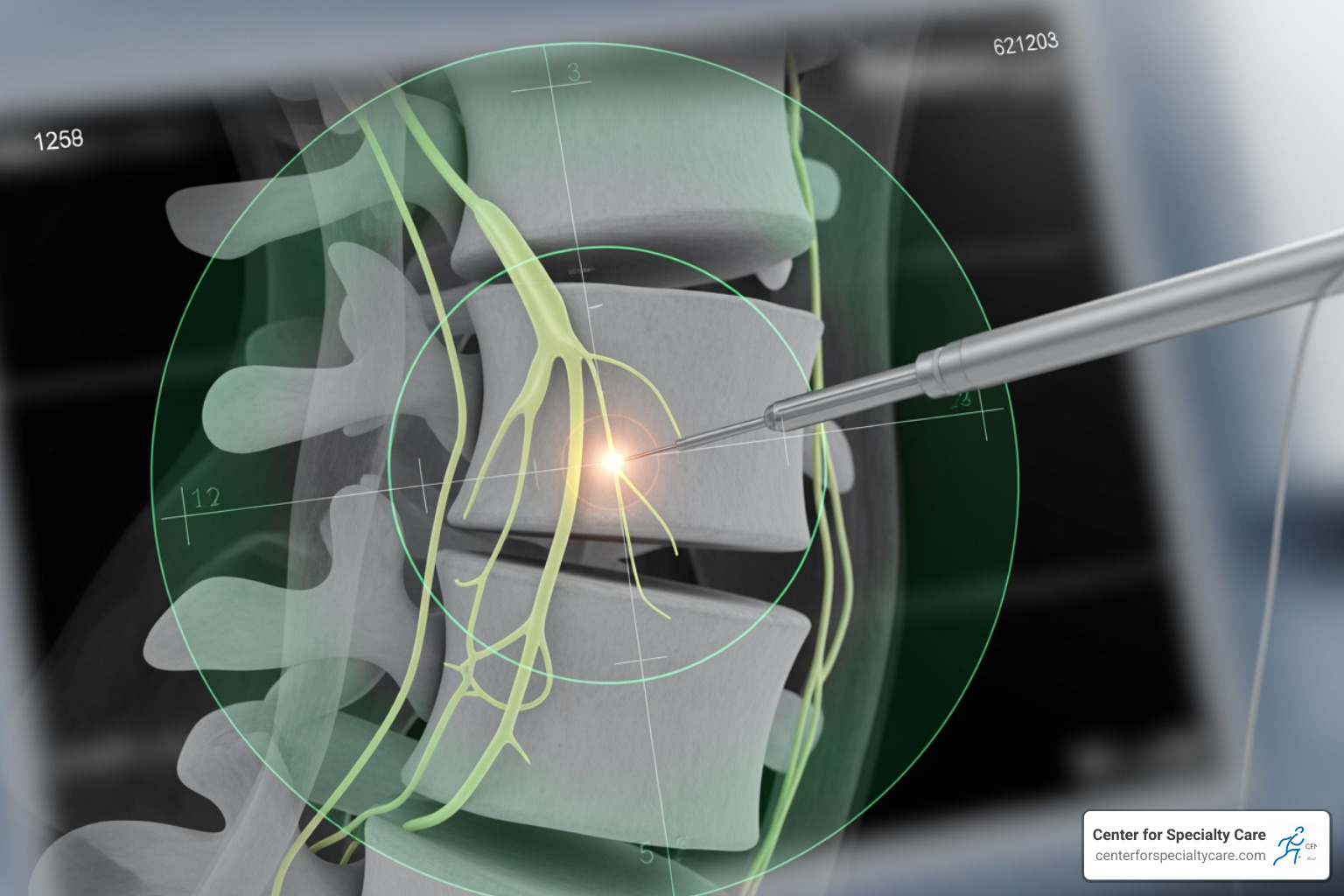
The beauty of the Intracept procedure lies in its precision and direct approach. Here’s a step-by-step look at how we perform it:
- Targeting the Nerve: The procedure begins with you comfortably positioned, typically under general anesthesia, ensuring you experience no discomfort. We use advanced imaging, specifically fluoroscopic guidance (a real-time X-ray), to precisely steer to the affected vertebra. This allows us to visualize the tiny basivertebral nerve within the bone.
- Creating a Channel: Through a small incision, usually no bigger than a pencil eraser, we gently insert a specialized cannula (a thin, hollow tube) into the vertebral body. This cannula acts as a pathway, carefully guided to the exact location of the basivertebral nerve.
- Delivering Radiofrequency Energy: Once the cannula is in place, a radiofrequency probe is advanced through it. This probe delivers controlled radiofrequency energy (a form of heat) to the nerve. This carefully applied heat ablates (disables) the basivertebral nerve, effectively stopping it from sending pain signals to your brain. The nerve ablation process can take between 7 and 15 minutes for each treated level of your spine.
- Disrupting Pain Signals: By ablating the basivertebral nerve, we disrupt the pain pathway, providing relief from the chronic ache originating from the damaged vertebral endplates. The basivertebral nerve has not shown an ability to grow back after treatment, suggesting long-lasting relief.
- Closing the Incision: After the nerve ablation is complete, the probe and cannula are removed, and the small incision is closed with a bandage. There are no implants left inside, and the entire procedure typically takes between 60 to 90 minutes. You’ll be surprised at how quickly such a targeted treatment can be completed!
This innovative approach is a testament to how far spinal treatments have come, offering a less invasive alternative to traditional surgery. For those interested in learning more about surgical interventions, our surgery options page provides additional details.
Are You a Candidate for the Intracept Procedure?
Deciding if the Intracept procedure is right for you involves a careful and personalized clinical review. We understand that living with chronic low back pain is a journey, often marked by trying various treatments. The Intracept procedure is specifically designed for a particular subset of patients who haven’t found adequate relief from more conservative care options. Our goal at Center for Specialty Care is always to provide solutions that genuinely address the root cause of your discomfort, and sometimes that means exploring advanced, targeted therapies.
We believe in empowering our patients with knowledge and ensuring they receive the most appropriate care for their unique situation. This is why a thorough discussion with one of our pain management specialists is crucial. We encourage you to learn more about our comprehensive approach to pain management.
Key Candidacy Criteria for the Intracept Procedure
The Intracept procedure is not a one-size-fits-all solution, but it can be a life-changing option for the right candidate. Here are the specific indications that we look for:
- Chronic Low Back Pain for at Least Six Months: You must have experienced persistent low back pain for a minimum of six months. This ensures we’re addressing truly chronic pain, not acute episodes that might resolve on their own.
- Tried Conservative Care for at Least Six Months: Before considering Intracept, you should have undergone at least six months of conservative treatments. This typically includes physical therapy, medications (over-the-counter or prescription), and sometimes injections. We want to ensure that less invasive options have been exhausted before proceeding.
- MRI Confirmation of Modic Changes: As discussed earlier, your MRI must show features consistent with Modic changes (specifically Type 1 or Type 2) in the vertebral endplates. These changes are the definitive visual evidence that your pain is vertebrogenic, originating from inflammation and damage within the bone.
These criteria are essential for identifying patients who are most likely to benefit significantly from the Intracept procedure. We want to make sure we’re targeting the problem effectively!
Who Should Not Consider This Procedure?
While incredibly beneficial for many, the Intracept procedure isn’t suitable for everyone. We prioritize your safety and well-being above all else. During your clinical review, we will carefully assess for any contraindications that would make the procedure unsafe or ineffective for you.
Here’s a list of conditions that would typically exclude a patient from receiving the Intracept procedure:
- Pregnancy: The procedure is not recommended for pregnant individuals.
- Active Implanted Electronic Devices: If you have an active implanted electronic medical device, such as a spinal cord stimulator or certain nerve stimulators, the Intracept procedure might be contraindicated due to potential interference.
- Pacemakers: Patients with pacemakers or other implantable cardiac devices are generally not candidates.
- Systemic or Local Infection: Any active systemic infection (e.g., a widespread infection throughout the body) or a local infection at the proposed treatment site must be resolved before considering the procedure.
- Anatomy that Could Be Damaged Unintentionally: If your specific spinal anatomy presents an unusual risk of unintentional damage during the ablation process, we would not proceed.
- Skeletally Immature Patients: The procedure is not indicated for individuals who are skeletally immature, generally those under 18 years of age.
- Severe Cardiac or Pulmonary Issues: Patients with weakened cardiac or pulmonary function may not be suitable candidates due to the nature of the procedure and anesthesia.
It’s vital to have an open and honest discussion with our team about your complete medical history and any conditions you may have. We’re here to guide you to the safest and most effective treatment path.
The Patient Journey: What to Expect During and After Intracept
When you decide to proceed with the Intracept procedure at Center for Specialty Care, we ensure you’re fully prepared and comfortable every step of the way. Our personalized care means we’ll walk you through everything, from pre-procedure instructions to post-recovery guidance.
Procedure Preparation: Before your appointment, we’ll provide detailed instructions. Since the procedure is performed under general anesthesia, you’ll need to arrange for a trusted friend or family member to drive you home. We’ll also review all medications and supplements you’re currently taking, as some may need to be temporarily stopped beforehand.
During the Procedure: On the day of your procedure, our warm and caring team in Fairmont, Estherville, Buffalo Center, or St. James will welcome you. Once you’re comfortable and under general anesthesia, the procedure itself typically takes between 60 and 90 minutes. It’s an outpatient procedure, meaning you won’t need an overnight hospital stay. Our specialists, utilizing fluoroscopic guidance, will perform the precise basivertebral nerve ablation as described earlier.
After the Procedure: Following the procedure, you’ll be monitored in our recovery area for a short period, typically up to an hour, to ensure you’re waking up comfortably from the anesthesia. Most people are able to go home the very same day. We’re proud to offer quick appointment availability, making your journey to relief as smooth as possible. For more information on how we care for your spine, check out our resources on back and spine care.
Recovery and Onset of Pain Relief
One of the significant advantages of the Intracept procedure is its relatively quick recovery time. Most people can go back to normal activities after a short rest and within several days. For some, particularly those with physically demanding jobs, it might take one to two weeks to fully resume all activities.
It’s normal to experience some slight soreness, bruising, or minor swelling at the incision site for a few days after the procedure. This discomfort is usually manageable with over-the-counter pain relievers like acetaminophen or ibuprofen. Our team will provide you with specific post-treatment instructions to ensure a smooth recovery. We always recommend you rest as much as possible and avoid strenuous exercise for about 48 hours immediately following the procedure.
The onset of pain relief can vary. Some people start to feel pain relief within two weeks, which is fantastic! Many others continue to improve gradually over three months. It’s a journey, not a sprint, but the relief can be profound and lasting. It’s important to remember that improvements can be progressive. If you’re experiencing pain that radiates, you might find our article on managing radiating pain helpful.
Proven Benefits and Long-Term Outcomes
The Intracept procedure isn’t just another treatment; it’s a breakthrough for chronic vertebrogenic low back pain. It is FDA-cleared, a testament to its safety and effectiveness. We’re also encouraged by the real-world results: it has been trusted by over 50,000 patients and counting. This significant number speaks volumes about its acceptance and success in providing relief.
Patients who undergo the Intracept procedure often experience not just a reduction in pain scores but also a significant improvement in their overall function and activity levels. Imagine being able to enjoy hobbies you once loved, or simply walking without that nagging ache. The procedure has been proven to reduce pain and improve activity in most people with vertebrogenic back pain.
But what about long-term? This is where Intracept truly shines. A prospective randomized double-blind sham-controlled multi-center study, with a 5-year treatment arm, demonstrated durable relief. The results were impressive:
- Roughly two-thirds of patients reported at least a 50% reduction in pain five years after a single Intracept procedure.
- Approximately one-third of patients were 100% pain-free at the five-year mark.
- A remarkable 70% of patients resumed their pre-pain activity levels, indicating a significant return to a fuller, more active life.
These statistics underscore the potential for long-lasting, meaningful pain relief, truly allowing our patients to “get back what pain has stolen.” You can dig into the full findings of this study here: Long-term outcomes following intraosseous basivertebral nerve ablation for the treatment of chronic low back pain: 5-year treatment arm results from a prospective randomized double-blind sham-controlled multi-center study.
How Intracept Compares to Other Treatments
When considering treatment for chronic low back pain, it’s helpful to see how Intracept stacks up against other common options. We believe in providing you with all the information to make an informed decision.
| Feature | Conservative Care (PT, Medications, Injections) | Spinal Fusion Surgery | Intracept Procedure |
|---|---|---|---|
| Invasiveness | Non-invasive to minimally invasive (injections) | Highly invasive (major surgery) | Minimally invasive |
| Recovery Time | Ongoing, variable | Weeks to months, often extensive rehabilitation | Days to 2 weeks for full activity |
| Implant Use | None | Permanent implants (screws, rods) | None (implant-free) |
| Spine Structure | Preserved | Altered (fusion of vertebrae) | Preserved (no alteration of spine mechanics) |
| Pain Relief | Temporary or partial for vertebrogenic pain | Can be significant, but major surgery risks/recovery | Durable, long-term relief for vertebrogenic pain |
| Future Treatments | Does not preclude other options | May limit future options in fused segments | Does not preclude future spinal treatments if needed |
| Target | General pain relief, muscle strengthening | Stabilizes unstable segments, addresses disc issues | Specific basivertebral nerve for vertebrogenic pain |
As you can see, Intracept offers a compelling middle ground: it’s more definitive than conservative care for specific vertebrogenic pain, but far less invasive than major surgery, with a quicker recovery and preservation of your natural spinal structure.
Frequently Asked Questions about the Intracept Procedure
It’s natural to have questions about any medical procedure, especially one designed to address chronic pain. We’ve compiled some of the most common inquiries our patients have about the Intracept procedure.
Is the Intracept procedure painful?
The Intracept procedure is performed under general anesthesia, so you will not feel any pain during the actual procedure. Afterward, it’s common to experience some temporary soreness, bruising, or mild swelling at the small incision site. This discomfort is typically manageable with over-the-counter pain relievers and usually subsides within a few days to a week. While some patients might experience a temporary increase in back pain for a week or two post-procedure, this is generally part of the healing process and resolves as relief sets in. We’ll ensure you have appropriate pain management strategies for your comfort during recovery.
How long do the results of the Intracept procedure last?
The results of the Intracept procedure are designed to be long-lasting. Clinical studies, including a significant 5-year follow-up, have demonstrated durable pain relief for many patients. The reason for this sustained relief is that the procedure ablates (disables) the basivertebral nerve, and current research indicates that this nerve does not typically regrow after treatment. This means the pain signals from the damaged vertebral endplates are permanently interrupted, providing continuous relief for years. For many, it’s a one-time procedure that offers significant, long-term benefits.
Will my insurance cover the Intracept procedure?
Many insurance plans, including Medicare, do provide coverage for the Intracept procedure, especially given its FDA clearance and proven efficacy for specific types of chronic low back pain. However, coverage can vary depending on your specific insurance provider and plan. Our dedicated team at Center for Specialty Care will work with you to understand your benefits and steer any necessary prior authorization processes. We’ll help you explore your options and provide clarity on coverage so you can focus on your journey to relief.
Take the Next Step Towards Relief
Chronic low back pain doesn’t just hurt; it can steal your joy, limit your activities, and diminish your quality of life. At Center for Specialty Care, we understand this deeply, and we’re dedicated to helping you reclaim your life from pain. The Intracept procedure offers a powerful, minimally invasive, and long-lasting solution for those suffering from vertebrogenic low back pain, providing hope where other treatments may have fallen short.
We pride ourselves on 100% patient satisfaction, offering personalized care custom to your unique needs, and ensuring quick appointment availability so you can start your journey to relief without unnecessary delays. Our expert team in Fairmont, Estherville, Buffalo Center, and St. James is here to provide an accurate diagnosis and guide you through every step of the process.
If you’ve been living with chronic low back pain for at least six months, have tried conservative treatments without success, and your MRI shows Modic changes, the Intracept procedure could be the answer you’ve been searching for.
Don’t let back pain define your life any longer. We invite you to explore a future with less pain and more possibility.
Contact us today to schedule a consultation for the Intracept Procedure and find if this innovative treatment is right for you.