Your Path to Pain Relief: Discover Intracept Providers Nearby
January 24, 2026
Your Guide to Custom Orthotics and Understanding the Investment
January 28, 2026Tendonitis heat therapy: 2025 Essential Relief
Understanding Tendonitis Pain and Your Recovery Options
Tendonitis heat therapy can be an effective tool for managing chronic tendon pain, but only when used at the right time. Heat works best after the initial inflammation has subsided—typically 48-72 hours post-injury—by increasing blood flow, relaxing tight muscles, and reducing stiffness. For acute injuries with swelling and sharp pain, ice is the better choice.
When to Use Heat for Tendonitis:
- Chronic or ongoing tendon pain (tendinopathy/tendinosis)
- Stiffness and tightness around the affected joint
- Before stretching or exercise to warm up the tissue
- After the first 48-72 hours following injury
When to Use Ice Instead:
- First 48-72 hours after a sudden injury
- Sharp pain and visible swelling
- Acute inflammation or flare-ups
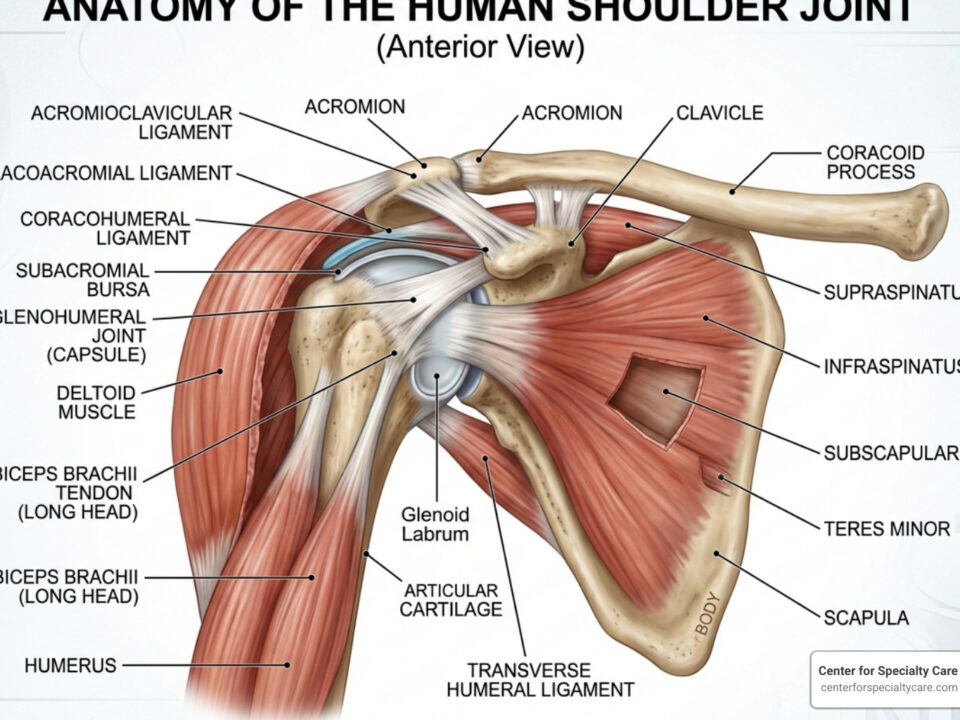
Tendonitis occurs when the tough fibrous cords connecting muscle to bone—your tendons—become irritated or inflamed. This typically happens from repetitive movements, overuse, or sudden increases in activity. Common areas affected include the shoulder (rotator cuff), elbow (tennis elbow), knee (patellar tendonitis), wrist, and Achilles tendon.
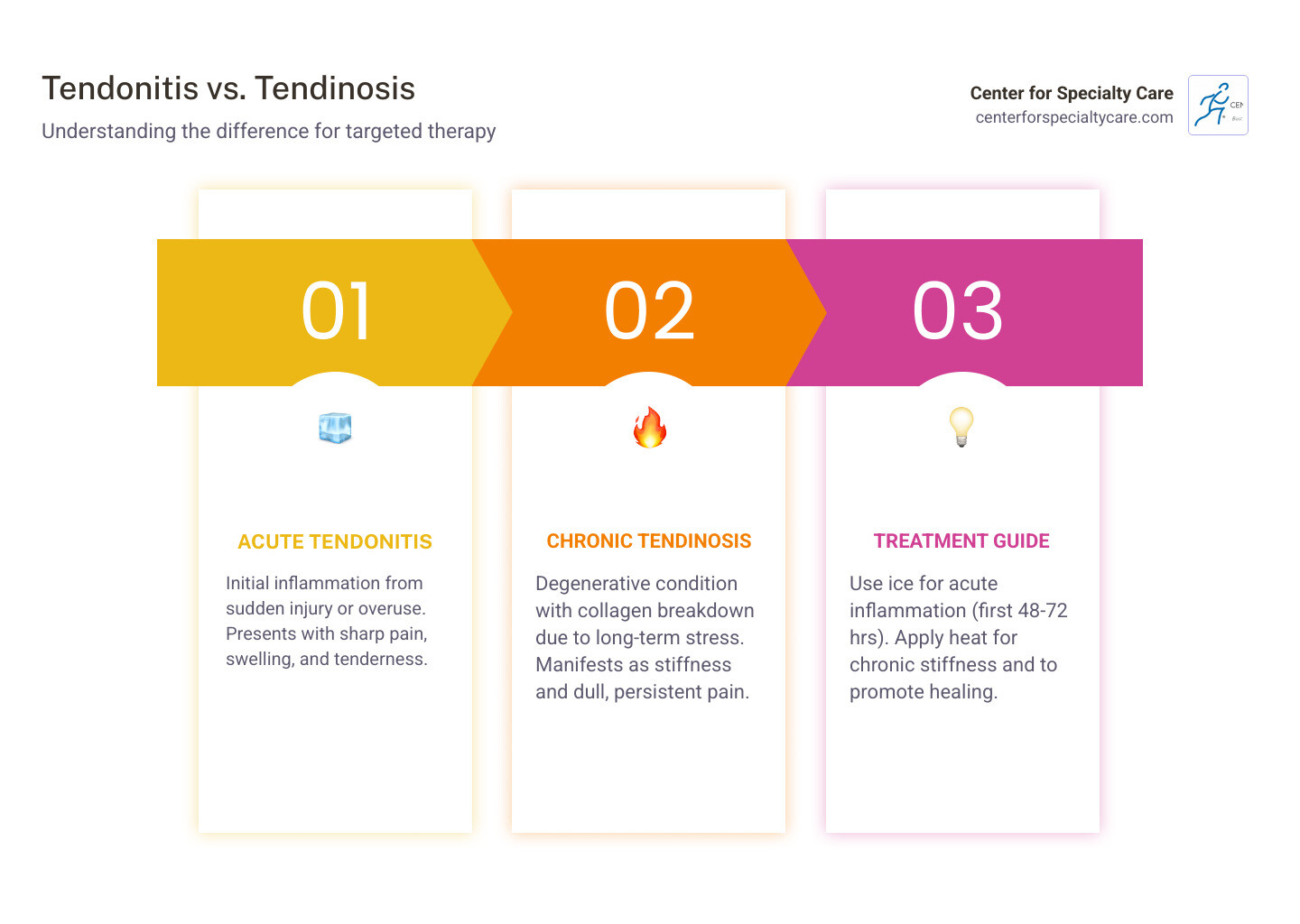
The pain often starts as a dull ache near a joint, accompanied by tenderness, swelling, and reduced range of motion. While acute tendonitis involves inflammation, many chronic cases are actually tendinosis—a degenerative condition where collagen breaks down over time. Understanding this difference is crucial because it determines which therapy works best.
I’m Dr. Corey Welchlin, a board-certified orthopedic surgeon who has spent over 30 years helping patients in southern Minnesota and northern Iowa recover from sports injuries and overuse conditions. Throughout my practice, I’ve guided countless patients through effective tendonitis heat therapy protocols as part of comprehensive treatment plans that get them back to the activities they love.
Glossary for Tendonitis heat therapy:
Heat vs. Ice: Choosing the Right Tool for the Job
When dealing with tendon pain, one of the first questions we often hear is, “Should I use heat or ice?” It’s a common dilemma, and the answer truly depends on the nature and stage of your condition. Think of it like this: are you putting out a fire, or are you warming up a stiff engine?
For sudden injuries to a tendon, where you might experience sharp pain, visible swelling, or acute inflammation, ice is generally our go-to. Ice helps constrict blood vessels, which reduces blood flow to the area. This, in turn, helps to numb the pain, decrease swelling, and blunt the inflammatory response. This is particularly important in the first 48 to 72 hours after an injury or a flare-up.
However, once that initial inflammation has subsided, or if you’re dealing with persistent stiffness and a dull ache from a chronic condition like tendinosis, tendonitis heat therapy steps in as the hero. Heat promotes increased blood flow, which is fantastic for bringing healing nutrients and oxygen to the affected area. It also helps relax tight muscles and connective tissues, easing stiffness and improving flexibility. This is why heat is often more beneficial for ongoing tendon pain, often referred to as tendinopathy or tendinosis.
Medical experts agree: after a sudden injury to a tendon, ice can ease pain and swelling. Heat, on the other hand, is more helpful for ongoing tendon pain (tendinopathy or tendinosis). Heat can boost blood flow, which may help the tendon heal, and can ease pain by relaxing muscles. You can read more about this in the Mayo Clinic resource on tendinitis pain: Should I apply ice or heat?.
Here’s a quick comparison to help you decide:
| Heat Therapy | Ice Therapy | |
|---|---|---|
| When to Use | Chronic pain, stiffness, before activity | Acute injuries, sharp pain, inflammation, swelling |
| Benefits | Increased blood flow, muscle relaxation, reduced stiffness, pain relief | Reduced blood flow, numbing, decreased swelling, reduced inflammation |
| How It Works | Widens blood vessels (vasodilation) | Narrows blood vessels (vasoconstriction) |
The Benefits of Tendonitis Heat Therapy
Once the initial acute phase of your tendonitis has passed, tendonitis heat therapy becomes a powerful ally in your recovery journey. We’ve seen how effectively it can alleviate persistent discomfort and aid healing for our patients throughout our service area. The benefits are numerous and stem from how heat interacts with your body’s physiology:
-
Increased Circulation and Nutrient Delivery: When we apply heat, blood vessels in the treated area dilate (widen). This vasodilation significantly boosts blood flow, carrying more oxygen and essential nutrients to the injured tendon. This increased circulation is vital for tissue repair and regeneration, essentially fueling the healing process. It also helps flush away metabolic waste products that can accumulate and contribute to pain.
-
Muscle Relaxation: Tendonitis often leads to compensatory muscle guarding and spasms around the affected joint. Heat therapy helps these muscles relax, easing tension and reducing the painful spasms that can exacerbate your condition. Relaxed muscles mean less strain on the already compromised tendon.
-
Reduced Stiffness: Stiffness is a hallmark of chronic tendonitis. Heat makes connective tissues, including tendons and ligaments, more pliable and elastic. This means that applying heat before gentle movement or stretching can significantly reduce stiffness, making it easier and less painful to move the affected joint.
-
Pain Relief: Beyond addressing the root causes, heat directly helps with pain management. The warmth stimulates sensory receptors in the skin, which can override pain signals being sent to the brain. This creates a soothing, analgesic effect that can provide much-needed comfort. For more insights into managing persistent pain, explore our resources on pain management.
-
Improved Flexibility and Range of Motion: By relaxing muscles and increasing tissue elasticity, heat therapy prepares your body for movement. This can lead to improved flexibility and a greater range of motion, which is crucial for regaining full function and preventing future injuries.
Tendonitis heat therapy creates a more favorable environment for your body to heal itself, making it an indispensable part of managing chronic tendon pain.
When to Use Ice Instead
While tendonitis heat therapy is excellent for chronic conditions, there are specific situations where ice, or cryotherapy, is the undisputed champion. It’s all about timing and what your body needs at that moment.
We recommend reaching for the ice pack when:
- You’ve sustained a sudden injury: If you twisted your ankle, over-extended your wrist, or felt a sudden pop or sharp pain during an activity, ice should be your immediate response.
- You experience sharp, acute pain: This type of pain often indicates ongoing tissue damage or an inflammatory response. Ice helps to calm this down.
- There’s visible swelling: Swelling is a clear sign of inflammation and fluid accumulation. Ice helps to reduce this by constricting blood vessels, slowing blood flow, and limiting the amount of fluid that leaks into the surrounding tissues.
- It’s within the first 48-72 hours post-injury: This is the critical acute phase where inflammation is at its peak. Applying ice during this window helps to control the initial inflammatory cascade.
- You need a numbing effect: Ice provides a powerful analgesic effect by slowing nerve conduction, effectively numbing the painful area. This can offer immediate relief from acute discomfort.
- There’s active inflammation or a flare-up: Even if your tendonitis is generally chronic, a sudden increase in pain, redness, or warmth indicates an acute inflammatory flare-up. In these cases, revert to ice until the acute symptoms subside.
Using heat on an acute injury with active inflammation can actually worsen swelling and pain. So, always assess the situation: if it’s new, hot, swollen, or sharply painful, grab the ice!
How to Safely Apply Tendonitis Heat Therapy at Home
Applying tendonitis heat therapy effectively and safely at home is key to maximizing its benefits without causing further harm. We guide our patients through these methods regularly, ensuring they feel confident in their self-care routines.

Here are some of the best methods for applying heat:
- Moist Heating Pads: These are fantastic because moist heat penetrates deeper into tissues than dry heat. They’re excellent for larger joints like shoulders, knees, and elbows, where you might experience conditions like Extensor Tendonitis. Many electric heating pads offer a moist heat setting, or you can place a damp towel between a dry heating pad and your skin.
- Warm Compresses or Towels: A simple, effective, and readily available method. Dampen a clean towel with warm (not hot!) water, wring out the excess, and apply.
- Warm Baths or Showers: For more generalized stiffness or pain in areas like the back, shoulder, or hip, a warm bath or shower can provide comforting, all-encompassing heat. This is especially good before gentle stretching.
- Heated Gel Packs or Heat Wraps: These are convenient, portable options that can be heated in the microwave or are air-activated. They conform well to body contours and are great for targeted relief.
Step-by-Step Application Guide
To ensure you get the most out of your tendonitis heat therapy and keep yourself safe, follow these steps:
- Prepare the Area: Ensure the skin on the affected area is clean and free of any lotions or oils that might interfere with heat absorption or cause irritation.
- Choose Your Method: Select one of the methods listed above that best suits the area of your body and your convenience.
- Apply for 15-20 Minutes: This is the optimal duration for heat therapy. It’s long enough to allow the warmth to penetrate and stimulate blood flow and muscle relaxation, but not so long as to risk skin irritation or burns.
- Use a Barrier: Always place a thin towel or cloth between the heat source (especially electric heating pads or very warm gel packs) and your bare skin. This prevents direct contact, which can lead to burns.
- Wait Between Sessions: If you need to reapply heat, allow at least an hour for your skin to return to its normal temperature. This gives your skin a break and reduces the risk of overheating. You can typically apply heat 2-3 times daily, once inflammation has resolved.
- Combine with Stretching: Heat therapy is particularly beneficial before gentle stretching or rehabilitative exercises. The warmth increases tissue elasticity, making stretches more effective and less painful.
Safety Precautions for Tendonitis Heat Therapy
While tendonitis heat therapy is generally safe and beneficial, certain precautions are crucial to prevent injury. We always emphasize these points to our patients:
- Avoid Direct Skin Contact: As mentioned, always use a barrier like a towel. This is non-negotiable, especially with electric heating pads or very warm compresses.
- Do Not Use on Fresh Injuries: This is perhaps the most important rule. If you have a new injury, or if there’s active swelling, redness, or warmth, use ice, not heat. Heat will only exacerbate inflammation and swelling in these acute phases.
- Check Skin Frequently: Periodically lift the heat source and check your skin for excessive redness, blistering, or any signs of irritation. If the skin feels uncomfortably hot or looks irritated, remove the heat immediately.
- Avoid Sleeping with a Heating Pad: Never fall asleep with an electric heating pad turned on. This significantly increases the risk of severe burns, as your body’s ability to sense discomfort is diminished during sleep.
- Caution with Diabetes or Neuropathy: If you have conditions that impair sensation, such as diabetes or peripheral neuropathy, exercise extreme caution. You may not be able to accurately gauge the temperature, increasing your risk of burns. Consult with your healthcare provider before using heat therapy if you have these conditions.
- Do Not Apply to Open Wounds or Damaged Skin: Heat should only be applied to intact skin.
- Avoid Overheating: The heat should feel comfortably warm, not painfully hot. If it’s uncomfortable, it’s too hot.
By following these safety guidelines, you can harness the therapeutic power of heat to aid your tendonitis recovery effectively and without incident.
Maximizing Your Recovery Beyond Heat Therapy
While tendonitis heat therapy is a valuable component of managing chronic tendon pain, it’s most effective when integrated into a broader, comprehensive recovery plan. At Center for Specialty Care, we believe in personalized treatment plans that address all aspects of your health and well-being.

Here are some complementary treatments that work well with heat therapy:
- Gentle Stretching: As we’ve discussed, heat therapy makes tissues more pliable. Following a heat session with gentle, controlled stretches can significantly improve flexibility and range of motion. For example, if you have shoulder tendonitis, gentle pendulum stretches or cross-body reaches can be beneficial. For wrist tendonitis, careful wrist flexor and extensor stretches can help. Always stretch within a comfortable range and stop if you feel any sharp pain.
- Strengthening Exercises: Once your pain has subsided and flexibility improves, targeted strengthening exercises are crucial for rebuilding tendon resilience and preventing recurrence. Eccentric strength training, where the muscle lengthens under tension, is particularly effective for many tendinopathies. A physical therapist at our clinic can design a program custom to your specific condition and body part.
- Activity Modification: This involves identifying and adjusting the activities that aggravate your tendonitis. It might mean changing your grip on a tool, modifying your sports technique, or taking more frequent breaks. Small changes can make a big difference in reducing strain on the tendon.
- Ergonomic Adjustments: For work-related tendonitis (e.g., wrist or elbow pain from computer use), optimizing your workspace ergonomics can be transformative. Proper chair height, keyboard and mouse placement, and monitor position can all reduce repetitive strain.
- Physical Therapy: A physical therapist is an invaluable partner in tendonitis recovery. They can assess your condition, provide hands-on treatment, guide you through therapeutic exercises, and teach you strategies to prevent future issues. Our team offers comprehensive physical therapy services to help you regain strength and mobility.
- Medications: Over-the-counter pain relievers like ibuprofen or naproxen can help manage pain and inflammation. In some cases, your doctor might prescribe stronger anti-inflammatory medications.
- Injections: For persistent cases, your doctor might consider treatments such as corticosteroid injections or platelet-rich plasma (PRP) therapy, when appropriate. These options are carefully evaluated and discussed with you as part of your personalized care plan.
The goal is not just to alleviate pain but to promote true healing and restore full function. A multi-faceted approach, guided by healthcare professionals, is often the most successful path to recovery.
When to See a Doctor for Tendonitis
While home remedies like tendonitis heat therapy and ice can provide significant relief, it’s crucial to know when to seek professional medical help. Your body has a remarkable ability to heal, but sometimes it needs a little expert guidance.
We strongly recommend consulting with a doctor at Center for Specialty Care if:
- Your pain persists for more than two weeks: If your symptoms aren’t improving with consistent home care (rest, ice/heat, OTC pain relievers) after a couple of weeks, it’s time for an evaluation.
- You experience severe pain or swelling: Intense pain that limits your daily activities, or significant swelling that doesn’t subside, warrants a medical opinion.
- You have an inability to move the affected joint: If you can’t move your shoulder, elbow, knee, or other joint through its normal range of motion due to pain or stiffness, it could indicate a more serious issue.
- Your symptoms worsen despite home care: If your pain or other symptoms are getting worse, rather than better, despite your best efforts, please don’t delay seeking help.
- You heard a “popping” sound at the time of injury: A sudden pop, especially accompanied by immediate pain and weakness, could signal a tendon rupture, which requires prompt medical attention.
- You develop fever, redness, or warmth around the tendon: These symptoms, particularly a fever above 100°F (38°C), could indicate an infection, which is a medical emergency.
- Tendonitis interferes significantly with your daily activities or sleep: If your quality of life is being severely impacted, we can help find solutions.
Our team, specializing in sports medicine and orthopedics, can accurately diagnose your condition, differentiate between tendonitis and tendinosis, and develop a custom treatment plan. This might include further diagnostic imaging, physical therapy, medication, or other interventions to get you back on track. Early intervention can often prevent chronic problems and more complex treatments down the road.
Frequently Asked Questions about Heat for Tendonitis
We often encounter common questions about using heat for tendonitis. Here are some of the most frequent ones, along with our expert answers:
Can heat make tendonitis worse?
Yes, if used improperly, heat can absolutely make tendonitis worse. The key is timing. If you apply heat to a fresh injury or an area with active inflammation (characterized by swelling, redness, and warmth), you will likely increase blood flow to an already inflamed area. This can exacerbate swelling and intensify pain, delaying the healing process. Tendonitis heat therapy is best reserved for chronic stiffness, muscle tightness, and dull aches after the initial acute inflammatory phase (typically 48-72 hours post-injury) has passed.
How long should I apply heat for tendonitis?
For most effective and safe application of tendonitis heat therapy, we recommend applying heat for 15-20 minutes at a time. This duration allows the warmth to penetrate the tissues, promote blood flow, and relax muscles without risking burns or excessive skin irritation. You can repeat these sessions up to 2-3 times daily, but it’s crucial to allow at least an hour between applications for your skin to return to its normal temperature. Always check your skin periodically during and after application.
Can I alternate heat and ice for tendonitis?
Yes, alternating heat and ice, often referred to as contrast therapy, can be a beneficial approach for managing tendonitis, especially in subacute or chronic phases where there might still be some lingering inflammation alongside stiffness. The theory behind contrast therapy is that the alternating temperatures cause blood vessels to constrict (with cold) and then dilate (with heat), creating a “pumping” action that can help improve circulation, reduce swelling, and alleviate pain. A common approach involves applying heat for a few minutes (e.g., 3-5 minutes) followed by cold for a shorter period (e.g., 1 minute), repeating this cycle several times. It’s often recommended to start and end with cold in acute or subacute phases to minimize residual swelling. However, for active acute injuries with significant swelling, it’s best to stick to ice initially.
Your Next Step Towards Tendonitis Relief
We’ve covered a lot about tendonitis heat therapy, from understanding when and why to use it to the best methods and crucial safety precautions. We’ve also highlighted how heat therapy fits into a broader strategy that includes ice, stretching, strengthening, and professional medical guidance.
The goal is to ease your pain, reduce stiffness, and promote healing so you can return to the activities you love without discomfort. While home therapies are excellent tools, understanding the nuances of your specific condition is paramount. Whether you’re dealing with a nagging ache or a more persistent issue, our team at Center for Specialty Care is here to help.
We are dedicated to providing personalized treatment plans and quick appointment availability for our patients across Fairmont MN, Estherville IA, Buffalo Center IA, and St James MN. We’re committed to 100% patient satisfaction, ensuring you receive the comprehensive, compassionate care you deserve.
Don’t let tendonitis hold you back. If you’re struggling with persistent tendon pain or if home remedies aren’t providing sufficient relief, we encourage you to reach out. Our expert orthopedic team is ready to assess your condition and guide you toward lasting relief.
Find expert orthopedic care with us today.